Abstract
Background
The atherogenic index of plasma (AIP) is considered a powerful biomarker of dyslipidemia and atherosclerosis (AS). However, limited evidence is available regarding the relationship between the AIP and carotid artery plaques (CAPs) in patients with coronary heart disease (CHD).
Methods
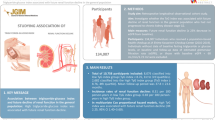
This retrospective study included 9281 patients with CHD who underwent carotid ultrasound. Participants were divided according to the AIP tertiles: T1, AIP < 1.02; T2, 1.02 ≤ AIP < 1.25; and T3, AIP ≥ 1.25. The presence or absence of CAPs was assessed using carotid ultrasound. Logistic regression was used to analyze the relationship between the AIP and CAPs in patients with CHD. The relationship between the AIP and CAPs was assessed according to sex, age, and glucose metabolic status.
Results
The baseline characteristics revealed significant differences in related parameters among patients with CHD after stratification into the three groups according to the AIP tertiles. Compared with T1, the odds ratio (OR) of T3 in patients with CHD was 1.53 (95% confidence interval [CI]:1.35–1.74). The association between AIP and CAPs was higher in females (OR: 1.63; 95% CI: 1.38–1.92) than in males (OR: 1.38; 95% CI: 1.12–1.70). The OR for patients aged ≤60 years (OR: 1.40; 95% CI: 1.14–1.71) was lower than that for patients aged >60 years (OR: 1.49; 95% CI: 1.26–1.76). AIP was significantly associated with the risk of CAPs formation in different glucose metabolic states, with diabetes having the highest OR value (OR: 1.31; 95% CI: 1.19–1.43).
Conclusion
The AIP and CAPs were significantly associated in patients with CHD, and the association was higher in female than in male patients. The association was lower in patients aged ≤60 years than in patients aged >60 years. Under different glucose metabolism statuses, the association between the AIP and the CAPs among patients with CHD was highest in patients with diabetes.
Graphical Abstract


Similar content being viewed by others
Data availability
The datasets used and/or analyzed in this study are available from the corresponding author upon reasonable request.
Abbreviations
- AIP:
-
The atherogenic index of plasma
- AS:
-
Atherosclerosis
- CAD:
-
Coronary atherosclerotic disease
- CAP:
-
Carotid artery plaque
- CHD:
-
Coronary heart disease
- DBP:
-
Diastolic blood pressure
- DM:
-
Diabetes mellitus
- FPG:
-
Fasting plasma glucose
- HbA1c:
-
Glycosylated hemoglobin
- HDL-C:
-
High-density lipoprotein cholesterol
- IQR:
-
Interquartile range
- LDL-C:
-
Low-density lipoprotein cholesterol
- OR:
-
Odds ratio
- pre-DM:
-
pre-diabetes mellitus
- SBP:
-
Systolic blood pressure
- T2DM:
-
Type 2 diabetes mellitus
- TC:
-
Total cholesterol
- TG:
-
Triglyceride
References
C.W. Tsao, A.W. Aday, Z.I. Almarzooq, C.A.M. Anderson, P. Arora, C.L. Avery, C.M. Baker-Smith, A.Z. Beaton, A.K. Boehme, A.E. Buxton, Y. Commodore-Mensah, M.S.V. Elkind, K.R. Evenson, C. Eze-Nliam, S. Fugar, G. Generoso, D.G. Heard, S. Hiremath, J.E. Ho, R. Kalani, D.S. Kazi, D. Ko, D.A. Levine, J. Liu, J. Ma, J.W. Magnani, E.D. Michos, M.E. Mussolino, S.D. Navaneethan, N.I. Parikh, R. Poudel, M. Rezk-Hanna, G.A. Roth, N.S. Shah, M.P. St-Onge, E.L. Thacker, S.S. Virani, J.H. Voeks, N.Y. Wang, N.D. Wong, S.S. Wong, K. Yaffe, S.S. Martin; American Heart Association Council on Epidemiology and Prevention Statistics Committee and Stroke Statistics Subcommittee, Heart disease and stroke statistics-2023 update: a report from the American Heart Association. Circulation 147(8), e93–e621 (2023). https://doi.org/10.1161/CIR.0000000000001123
B.Q. Yin, Y.H. Guo, Y. Liu, Y.Y. Zhao, S.M. Huang, X.W. Wei, H.S. Wang, R.Y. Liu, Y. Liu, Y.P. Tang, Molecular mechanism of Chuanxiong Rhizoma in treating coronary artery diseases. Chin. Herb. Med. 13(3), 396–402 (2021). https://doi.org/10.1016/j.chmed.2021.03.001
D.M. Xing, M.J. Zhu, C.X. Liu, H. Wang, Outcome measures in clinical trials of traditional Chinese medicine for stable angina pectoris. Acupunct. Herb. Med. 1(2), 99–106 (2021). https://doi.org/10.1097/HM9.0000000000000014
J.P. Duggan, A.S. Peters, G.D. Trachiotis, J.L. Antevil, Epidemiology of coronary artery disease. Surg. Clin. North Am. 102(3), 499–516 (2022). https://doi.org/10.1016/j.suc.2022.01.007
Z. Li, Q. Cheng, Y. Liu, X. Cheng, S. Wang, Y. He, X. Wang, M. Huang, Y. Li, X. Xue, Y. Xu, L. Li, Y. Zheng, R. Yang, S. Gao, C. Yu, Low-/high-density lipoprotein cholesterol ratio and carotid plaques in patients with coronary heart disease: a Chinese cohort study. Lipids Health Dis. 20(1), 144 (2021). https://doi.org/10.1186/s12944-021-01575-w
T. Hirata, Y. Arai, M. Takayama, Y. Abe, K. Ohkuma, T. Takebayashi, Carotid plaque score and risk of cardiovascular mortality in the oldest old: results from the TOOTH study. J. Atheroscler. Thromb. 25(1), 55–64 (2018). https://doi.org/10.5551/jat.37911
North American Symptomatic Carotid Endarterectomy Trial, Methods, patient characteristics, and progress. Stroke 22(6), 711–720 (1991). https://doi.org/10.1161/01.str.22.6.711
D.H.K. van Dam-Nolen, A.C. van Dijk, G.A.J.C. Crombag, C. Lucci, M.E. Kooi, J. Hendrikse, P.J. Nederkoorn, M.J.A.P. Daemen, A.F.W. van der Steen, P.J. Koudstaal, F. Kronenberg, J.E. Roeters van Lennep, M.T. Mulder, A. van der Lugt, Lipoprotein(a) levels and atherosclerotic plaque characteristics in the carotid artery: The Plaque at RISK (PARISK) study. Atherosclerosis 329, 22–29 (2021). https://doi.org/10.1016/j.atherosclerosis.2021.06.004
X. He, G. Kuang, Y. Wu, C. Ou, Emerging roles of exosomal miRNAs in diabetes mellitus. Clin. Transl. Med. 11(6), e468 (2021). https://doi.org/10.1002/ctm2.468
J. Alegre-Díaz, W. Herrington, M. López-Cervantes, L. Gnatiuc, R. Ramirez, M. Hill, C. Baigent, M.I. McCarthy, S. Lewington, R. Collins, G. Whitlock, R. Tapia-Conyer, R. Peto, P. Kuri-Morales, J.R. Emberson, Diabetes and cause-specific mortality in Mexico city. N. Engl. J. Med. 375(20), 1961–1971 (2016). https://doi.org/10.1056/NEJMoa1605368
B. Murphy-Chutorian, G. Han, S.R. Cohen, Dermatologic manifestations of diabetes mellitus: a review. Endocrinol. Metab. Clin. North Am. 42(4), 869–898 (2013). https://doi.org/10.1016/j.ecl.2013.07.004
X. He, C. Ou, Y. Xiao, Q. Han, H. Li, S. Zhou, LncRNAs: key players and novel insights into diabetes mellitus. Oncotarget 8(41), 71325–71341 (2017). https://doi.org/10.18632/oncotarget.19921
J.L. Jin, Y.X. Cao, H.H. Liu, H.W. Zhang, Y.L. Guo, N.Q. Wu, C.G. Zhu, R.X. Xu, Y. Gao, J. Sun, Q. Dong, J.J. Li, Impact of free fatty acids on prognosis in coronary artery disease patients under different glucose metabolism status. Cardiovasc Diabetol. 18(1), 134 (2019). https://doi.org/10.1186/s12933-019-0936-8
H.H. Liu, Y.X. Cao, S. Li, Y.L. Guo, C.G. Zhu, N.Q. Wu, Y. Gao, Q.T. Dong, X. Zhao, Y. Zhang, D. Sun, J.J. Li, Impacts of prediabetes mellitus alone or plus hypertension on the coronary severity and cardiovascular outcomes. Hypertension 71(6), 1039–1046 (2018). https://doi.org/10.1161/HYPERTENSIONAHA.118.11063
J.L. Jin, Y.X. Cao, H.W. Zhang, D. Sun, Q. Hua, Y.F. Li, Y.L. Guo, N.Q. Wu, C.G. Zhu, Y. Gao, Q.T. Dong, H.H. Liu, Q. Dong, J.J. Li, Lipoprotein(a) and cardiovascular outcomes in patients with coronary artery disease and prediabetes or diabetes. Diabetes Care 42(7), 1312–1318 (2019). https://doi.org/10.2337/dc19-0274
S. Niroumand, M. Khajedaluee, M. Khadem-Rezaiyan, M. Abrishami, M. Juya, G. Khodaee, M. Dadgarmoghaddam, Atherogenic Index of Plasma (AIP): a marker of cardiovascular disease. Med. J. Islam Repub. Iran 29, 240 (2015).
J.C. Fernández-Macías, A.C. Ochoa-Martínez, J.A. Varela-Silva, I.N. Pérez-Maldonado, Atherogenic index of plasma: novel predictive biomarker for cardiovascular illnesses. Arch. Med. Res. 50(5), 285–294 (2019). https://doi.org/10.1016/j.arcmed.2019.08.009
G. Cai, W. Liu, S. Lv, X. Wang, Y. Guo, Z. Yan, Y. Du, Y. Zhou, Gender-specific associations between atherogenic index of plasma and the presence and severity of acute coronary syndrome in very young adults: a hospital-based observational study. Lipids Health Dis. 18(1), 99 (2019). https://doi.org/10.1186/s12944-019-1043-2
X. Zhang, X. Zhang, X. Li, J. Feng, X. Chen, Association of metabolic syndrome with atherogenic index of plasma in an urban Chinese population: a 15-year prospective study. Nutr. Metab. Cardiovasc Dis. 29(11), 1214–1219 (2019). https://doi.org/10.1016/j.numecd.2019.07.006
B. Joob, V. Wiwanitkit, Atherogenic index of plasma for the assessment of cardiovascular risk factors. Ann. Afr. Med. 16(3), 148 (2017). https://doi.org/10.4103/aam.aam_332_16
J.M. Flack, B. Adekola, Blood pressure and the new ACC/AHA hypertension guidelines. Trends Cardiovasc Med. 30(3), 160–164 (2020). https://doi.org/10.1016/j.tcm.2019.05.003
Joint Committee for Developing Chinese guidelines on Prevention and Treatment of Dyslipidemia in Adults, Chinese guidelines on prevention and treatment of dyslipidemia in adults. Zhonghua Xin Xue Guan Bing. Za Zhi 35(5), 390–419 (2007).
L. Yang, Z. Li, Y. Song, Y. Liu, H. Zhao, Y. Liu, T. Zhang, Y. Yuan, X. Cai, S. Wang, P. Wang, S. Gao, L. Li, Y. Li, C. Yu, Study on urine metabolic profiling and pathogenesis of hyperlipidemia. Clin. Chim. Acta 495, 365–373 (2019). https://doi.org/10.1016/j.cca.2019.05.001
Y. Liu, Y. Zhu, W. Jia, D. Sun, L. Zhao, C. Zhang, C. Wang, G. Chen, S. Fu, Y. Bo, Y. Xing, Association between lipid profiles and presence of carotid plaque. Sci. Rep. 9(1), 18011 (2019). https://doi.org/10.1038/s41598-019-54285-w
R.S. Barua, N.A. Rigotti, N.L. Benowitz, K.M. Cummings, M.A. Jazayeri, P.B. Morris, E.V. Ratchford, L. Sarna, E.C. Stecker, B.S. Wiggins, 2018 ACC expert consensus decision pathway on tobacco cessation treatment: a report of the American College of cardiology task force on clinical expert consensus documents. J. Am. Coll. Cardiol. 72(25), 3332–3365 (2018). https://doi.org/10.1016/j.jacc.2018.10.027
A.Z. Fan, W.J. Ruan, S.P. Chou, Re-examining the relationship between alcohol consumption and coronary heart disease with a new lens. Prev. Med. 118, 336–343 (2019). https://doi.org/10.1016/j.ypmed.2018.11.022
H. Huang, X. Yu, L. Li, G. Shi, F. Li, J. Xiao, Z. Yun, G. Cai, Atherogenic index of plasma is related to coronary atherosclerotic disease in elderly individuals: a cross-sectional study. Lipids Health Dis. 20(1), 68 (2021). https://doi.org/10.1186/s12944-021-01496-8
G. Zhu, J. Hom, Y. Li, B. Jiang, F. Rodriguez, D. Fleischmann, D. Saloner, M. Porcu, Y. Zhang, L. Saba, M. Wintermark, Carotid plaque imaging and the risk of atherosclerotic cardiovascular disease. Cardiovasc Diagn. Ther. 10(4), 1048–1067 (2020). https://doi.org/10.21037/cdt.2020.03.10
Y. Li, G. Zhu, V. Ding, Y. Huang, B. Jiang, R.L. Ball, F. Rodriguez, D. Fleischmann, M. Desai, D. Saloner, L. Saba, J. Hom, M. Wintermark, Assessing the relationship between atherosclerotic cardiovascular disease risk score and carotid artery imaging findings. J. Neuroimag. 29(1), 119–125 (2019). https://doi.org/10.1111/jon.12573
M. Dobiášová, Atherogenic impact of lecithin-cholesterol acyltransferase and its relation to cholesterol esterification rate in HDL (FER(HDL)) and AIP [log(TG/HDL-C)] biomarkers: the butterfly effect? Physiol. Res. 66(2), 193–203 (2017). https://doi.org/10.33549/physiolres.933621.
J. Wu, Q. Zhou, Z. Wei, J. Wei, M. Cui, Atherogenic index of plasma and coronary artery disease in the adult population: a meta-analysis. Front. Cardiovasc. Med. 8, 817441 (2021). https://doi.org/10.3389/fcvm.2021.817441
N. Puig, E. Jiménez-Xarrié, P. Camps-Renom, S. Benitez, Search for reliable circulating biomarkers to predict carotid plaque vulnerability. Int J. Mol. Sci. 21(21), 8236 (2020). https://doi.org/10.3390/ijms21218236
O. Karayiğit, A. K. Dolu, M. C. Çelik, C. Özkan, B. Demirtaş, Relationship between the atherogenic index of plasma and non-dipping circadian pattern in hypertensive patients. Med. Princ. Pract. (2022). https://doi.org/10.1159/000527662
G. Yildiz, E. Hür, A. Özçiçek, F. Candan, M. Kayatas, The mean platelet volume and atherogenic index of plasma in nondipper normotensive individuals compared to dippers. Clin. Exp. Hypertens. 35(1), 35–39 (2013). https://doi.org/10.3109/10641963.2012.689043
T. Kubozono, M. Miyata, S. Kawasoe, S. Ojima, S. Yoshifuku, H. Miyahara, S. Maenohara, M. Ohishi, High pulse wave velocity has a strong impact on early carotid atherosclerosis in a Japanese general male population. Circ. J. 81(3), 310–315 (2017). https://doi.org/10.1253/circj.CJ-16-0687
J.D. Humphrey, D.G. Harrison, C.A. Figueroa, P. Lacolley, S. Laurent, Central artery stiffness in hypertension and aging: a problem with cause and consequence. Circ. Res. 118(3), 379–381 (2016). https://doi.org/10.1161/CIRCRESAHA.115.307722
H. Chen, Y. Chen, W. Wu, Z. Cai, Z. Chen, X. Yan, S. Wu, Total cholesterol, arterial stiffness, and systolic blood pressure: a mediation analysis. Sci. Rep. 11(1), 1330 (2021). https://doi.org/10.1038/s41598-020-79368-x
X. Ma, Y. Sun, Y. Cheng, H. Shen, F. Gao, J. Qi, L. Yang, Z. Wang, D. Shi, Y. Liu, X. Liu, Y. Zhou, Prognostic impact of the atherogenic index of plasma in type 2 diabetes mellitus patients with acute coronary syndrome undergoing percutaneous coronary intervention. Lipids Health Dis. 19(1), 240 (2020). https://doi.org/10.1186/s12944-020-01418-0
L. Fu, Y. Zhou, J. Sun, Z. Zhu, Z. Xing, S. Zhou, Y. Wang, S. Tai, Atherogenic index of plasma is associated with major adverse cardiovascular events in patients with type 2 diabetes mellitus. Cardiovasc Diabetol. 20(1), 201 (2021). https://doi.org/10.1186/s12933-021-01393-5
M. Murguía-Romero, J.R. Jiménez-Flores, S.C. Sigrist-Flores, M.A. Espinoza-Camacho, M. Jiménez-Morales, E. Piña, A.R. Méndez-Cruz, R. Villalobos-Molina, G.M. Reaven, Plasma triglyceride/HDL-cholesterol ratio, insulin resistance, and cardiometabolic risk in young adults. J. Lipid Res. 54(10), 2795–2799 (2013). https://doi.org/10.1194/jlr.M040584
M.R. Salazar, H.A. Carbajal, W.G. Espeche, M. Aizpurúa, P.M. Maciel, G.M. Reaven, Identification of cardiometabolic risk: visceral adiposity index versus triglyceride/HDL cholesterol ratio. Am. J. Med. 127(2), 152–157 (2014). https://doi.org/10.1016/j.amjmed.2013.10.012
J.A. Beckman, M.A. Creager, P. Libby, Diabetes and atherosclerosis: epidemiology, pathophysiology, and management. JAMA 287(19), 2570–2581 (2002). https://doi.org/10.1001/jama.287.19.2570
S.J. Nicholls, E.M. Tuzcu, S. Kalidindi, K. Wolski, K.W. Moon, I. Sipahi, P. Schoenhagen, S.E. Nissen, Effect of diabetes on progression of coronary atherosclerosis and arterial remodeling: a pooled analysis of 5 intravascular ultrasound trials. J. Am. Coll. Cardiol. 52(4), 255–262 (2008). https://doi.org/10.1016/j.jacc.2008.03.051
B. Tramunt, S. Smati, N. Grandgeorge, F. Lenfant, J.F. Arnal, A. Montagner, P. Gourdy, Sex differences in metabolic regulation and diabetes susceptibility. Diabetologia 63(3), 453–461 (2020). https://doi.org/10.1007/s00125-019-05040-3
F. Bragg, M.V. Holmes, A. Iona, Y. Guo, H. Du, Y. Chen, Z. Bian, L. Yang, W. Herrington, D. Bennett, I. Turnbull, Y. Liu, S. Feng, J. Chen, R. Clarke, R. Collins, R. Peto, L. Li, Z. Chen; China Kadoorie Biobank Collaborative Group, Association between diabetes and cause-specific mortality in rural and urban areas of China. JAMA 317(3), 280–289 (2017). https://doi.org/10.1001/jama.2016.19720
R. de Ritter, S.J.S. Sep, C.J.H. van der Kallen, M.T. Schram, A. Koster, A.A. Kroon, M.M.J. van Greevenbroek, S.J.P.M. Eussen, P.C. Dagnelie, M. de Jong, R.C. Vos, M. Woodward, M.L. Bots, S.A.E. Peters, C.D.A. Stehouwer, Adverse differences in cardiometabolic risk factor levels between individuals with pre-diabetes and normal glucose metabolism are more pronounced in women than in men: the Maastricht study. BMJ Open Diabetes Res Care 7(1), e000787 (2019). https://doi.org/10.1136/bmjdrc-2019-000787
M.N. Christiansen, L. Køber, P. Weeke, R.S. Vasan, J.L. Jeppesen, J.G. Smith, G.H. Gislason, C. Torp-Pedersen, C. Andersson, Age-specific trends in incidence, mortality, and comorbidities of heart failure in Denmark, 1995 to 2012. Circulation 135(13), 1214–1223 (2017). https://doi.org/10.1161/CIRCULATIONAHA.116.025941
J. Tromp, S.M.A. Paniagua, E.S. Lau, N.B. Allen, M.J. Blaha, R.T. Gansevoort, H.L. Hillege, D.E. Lee, D. Levy, R.S. Vasan, P. van der Harst, W.H. van Gilst, M.G. Larson, S.J. Shah, R.A. de Boer, C.S.P. Lam, J.E. Ho, Age dependent associations of risk factors with heart failure: pooled population based cohort study. BMJ 372, n461 (2021). https://doi.org/10.1136/bmj.n461
Acknowledgements
We thank all the participants in the study, the members of the survey teams, and the groups for providing financial support.
Funding
This study was supported by the National Basic Research Program of China (973 project, grant number2014CB542902) and the National Natural Science Fund project (approval number82074140).
Author information
Authors and Affiliations
Contributions
C.Q.Y., S.G., X.L.W., and Y.Y.H. participated in the study design and statistical analysis; Y.Y.H. and Z.L. analyzed the data and drafted the manuscript; and L.Y., Y.J.L., L.L., and R.R.Y. participated in data collection. All the authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Ethics approval and consent to participate
This study was approved by the ethics committee of Tianjin University of Traditional Chinese Medicine (TJUTCM-EC20190008) and was registered in the Chinese Clinical Trial Registry (ChiCTR-1900024535) and Clinical Trials.gov (NCT04026724).
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
He, Y., Li, Z., Yu, L. et al. Association between the atherogenic index of plasma and carotid artery plaques in patients with coronary heart disease in different glucose metabolism states: an RCSCD-TCM study in Tianjin, China. Endocrine 81, 252–261 (2023). https://doi.org/10.1007/s12020-023-03389-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-023-03389-5