Abstract
Purpose
Metformin induces GLUT-4 mRNA expression in insulin target tissues in PCOS. It is unclear how long this impact is sustained after withdrawal of metformin. We aimed to compare the effect of metformin withdrawal on GLUT-4 mRNA expression in subcutaneous adipose tissue after prior short (ST, 1 year, N = 11) and long term (LT, at least 3 years, N = 13) treatment in obese PCOS women.
Methods
At baseline and 6 months after withdrawal, biopsy of subcutaneous adipose tissue followed by quantitative PCR analysis was performed to determine GLUT-4 mRNA expression.
Results
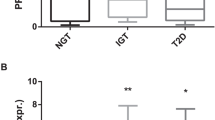
We found no time/effect differences in GLUT-4 mRNA expression in ST (2-dCt at baseline 0.42 (0.16–0.48) vs 2-dCt after 6 months 0.31 (0.22–0.56), p = 0.594) and no time/effect difference in LT group (2-dCt at baseline 0.24 (0.14–0.39) vs 2-dCt after 6 months 0.25 (0.20–0.38), p = 0.382). There was also no difference in GLUT-4 mRNA expression between both groups at baseline and after 6 months.
Conclusions
In summary, 6 months after metformin withdrawal, GLUT-4 mRNA expression in subcutaneous adipose tissue remained stable, regardless of the prior treatment duration.

Similar content being viewed by others
Availability of data and material
The datasets used and/or analyzed during the current study are available from the corresponding author upon reasonable request.
References
Y.H. Chen, S. Heneidi, J.M. Lee, L.C. Layman, D.W. Stepp, G.M. Gamboa, B.S. Chen, G. Chazenbalk, R. Azziz, Mirna-93 Inhibits Glut4 and is overexpressed in adipose tissue of polycystic ovary syndrome patients and women with insulin resistance. Diabetes 62(7), 2278–2286 (2013). https://doi.org/10.2337/db12-0963
A. Dunaif, Insulin resistance and the polycystic ovary syndrome: mechanism and implications for pathogenesis. Endocr. Rev. 18(6), 774–800 (1997). https://doi.org/10.1210/edrv.18.6.0318
C.M. DeUgarte, A.A. Bartolucci, R. Azziz, Prevalence of insulin resistance in the polycystic ovary syndrome using the homeostasis model assessment. Fertil. Steril. 83(5), 1454–1460 (2005). https://doi.org/10.1016/j.fertnstert.2004.11.070
R.S. Legro, V.D. Castracane, R.P. Kauffman, Detecting insulin resistance in polycystic ovary syndrome: purposes and pitfalls. Obstet. Gynecol. Surv. 59(2), 141–154 (2004). https://doi.org/10.1097/01.OGX.0000109523.25076.E2
A. Corbould, Chronic testosterone treatment induces selective insulin resistance in subcutaneous adipocytes of women. J. Endocrinol 192(3), 585–594 (2007). https://doi.org/10.1677/joe.1.07070
U. Ezeh, I.Y.D. Chen, Y.H. Chen, R. Azziz, Adipocyte expression of glucose transporter 1 and 4 in PCOS: relationship to insulin-mediated and non–insulin-mediated whole-body glucose uptake. Clin. Endocrinol. (Oxf). 90(4), 542–552 (2019). https://doi.org/10.1111/cen.13931
T.P. Ciaraldi, V. Aroda, S. Mudaliar, R.J. Chang, R.R. Henry, Polycystic ovary syndrome is associated with tissue-specific differences in insulin resistance. J. Clin. Endocrinol. Metab. 94(1), 157–163 (2009). https://doi.org/10.1210/jc.2008-1492
L.J. Shaw, C.N. Bairey Merz, R. Azziz, F.Z. Stanczyk, G. Sopko, G.D. Braunstein, S.F. Kelsey, K.E. Kip, R.M. Cooper-Dehoff, B.D. Johnson et al. Postmenopausal women with a history of irregular menses and elevated androgen measurements at high risk for worsening cardiovascular event-free survival: results from the National Institutes of Health–National heart, lung, and blood institute sponsored. J. Clin. Endocrinol. Metab. 93(4), 1276–1284 (2008). https://doi.org/10.1210/jc.2007-0425
D. Rosenbaum, R.S. Haber, A. Dunaif, Insulin resistance in polycystic ovary syndrome: decreased expression of GLUT-4 glucose transporters in adipocytes. Am. J. Physiol. - Endocrinol. Metab., 1993, 264 (2 27-2). https://doi.org/10.1152/ajpendo.1993.264.2.e197.
P.J. Marsden, A.P. Murdoch, R. Taylor, Tissue insulin sensitivity and body weight in polycystic ovary syndrome. Clin. Endocrinol. (Oxf) 55(2), 191–199 (2001). https://doi.org/10.1046/j.1365-2265.2001.01303.x
A. Biyasheva, R.S. Legro, A. Dunaif, M. Urbanek, Evidence for association between polycystic ovary syndrome (PCOS) and TCF7L2 and glucose intolerance in women with PCOS and TCF7L2. J. Clin. Endocrinol. Metab. 94(7), 2617–2625 (2009). https://doi.org/10.1210/jc.2008-1664
J. Lord, R. Thomas, B. Fox, U. Acharya, T. Wilkin, The effect of metformin on fat distribution and the metabolic syndrome in women with polycystic ovary syndrome–a randomised, double-blind, placebo-controlled trial. BJOG 113(7), 817–824 (2006). https://doi.org/10.1111/j.1471-0528.2006.00966.x
P.R. Shepherd, B.B. Kahn, Glucose transporters and insulin action–implications for insulin resistance and diabetes mellitus. N. Engl. J. Med. 341(4), 248–257 (1999). https://doi.org/10.1056/NEJM199907223410406
M.J. Thomson, M.G. Williams, S.C. Frost, Development of insulin resistance in 3T3-L1 adipocytes. J. Biol. Chem. 272(12), 7759–7764 (1997). https://doi.org/10.1074/jbc.272.12.7759
R. Fornes, P. Ormazabal, C. Rosas, F. Gabler, D. Vantman, C. Romero, M. Vega, Changes in the expression of insulin signaling pathway molecules in endometria from polycystic ovary syndrome women with or without hyperinsulinemia. Mol. Med. 16(3–4), 129–136 (2010). https://doi.org/10.2119/molmed.2009.00118
H.J. Teede, M.L. Misso, M.F. Costello, A. Dokras, J. Laven, L. Moran, T. Piltonen, R.J. Norman, M. Andersen, R. Azziz, et al. Recommendations from the International evidence-based guideline for the assessment and management of polycystic ovary syndrome. Hum. Reprod. (2018). https://doi.org/10.1093/humrep/dey256.
R.S. Legro, S.A. Arslanian, D.A. Ehrmann, K.M. Hoeger, M.H. Murad, R. Pasquali, C.K. Welt, Diagnosis and treatment of polycystic ovary syndrome: an endocrine society clinical practice guideline. J. Clin. Endocrinol. Metab. 98(12), 4565–4592 (2013). https://doi.org/10.1210/jc.2013-2350
M. Jensterle, A. Janez, B. Mlinar, J. Marc, J. Prezelj, M. Pfeifer, Impact of metformin and rosiglitazone treatment on glucose transporter 4 MRNA expression in women with polycystic ovary syndrome. Eur. J. Endocrinol. 158(6), 793–801 (2008). https://doi.org/10.1530/EJE-07-0857
J.O. Lee, S.K. Lee, J.H. Kim, N. Kim, G.Y. You, J.W. Moon, S.J. Kim, S.H. Park, H.S. Kim, Metformin regulates glucose transporter 4 (GLUT4) translocation through AMP-activated protein kinase (AMPK)-mediated Cbl/CAP signaling in 3T3-L1 preadipocyte cells. J. Biol. Chem. 287(53), 44121–44129 (2012). https://doi.org/10.1074/jbc.M112.361386
group, T. R. E. P. consensus workshop, Revised 2003 consensus on diagnostic criteria and long‐term health risks related to polycystic ovary syndrome (PCOS). Hum. Reprod. 19(1), 41–47 (2004). https://doi.org/10.1093/humrep/deh098
M. Ryo, K. Maeda, T. Onda, M. Katashima, A. Okumiya, M. Nishida, T. Yamaguchi, T. Funahashi, Y. Matsuzawa, T. Nakamura et al. A new simple method for the measurement of visceral fat accumulation by bioelectrical impedance. Diabetes Care 28(2), 451–453 (2005). https://doi.org/10.2337/diacare.28.2.451
B. Hedblad, P. Nilsson, L. Janzon, G. Berglund, Relation between insulin resistance and carotid intima-media thickness and stenosis in non-diabetic subjects. results from a cross-sectional study in Malmö, Sweden. Diabet. Med. 17(4), 299–307 (2000). https://doi.org/10.1046/j.1464-5491.2000.00280.x
D.R. Matthews, J.P. Hosker, A.S. Rudenski, B.A. Naylor, D.F. Treacher, R.C. Turner, Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia 28(7), 412–419 (1985). https://doi.org/10.1007/BF00280883
S. Zheng, H. Zhou, T. Han, Y. Li, Y. Zhang, W. Liu, Y. Hu, Clinical characteristics and beta cell function in Chinese patients with newly diagnosed type 2 diabetes mellitus with different levels of serum triglyceride. BMC Endocr. Disord. 15, 21 (2015). https://doi.org/10.1186/s12902-015-0018-1
M. Jensterle, N.A. Kravos, S. Ferjan, K. Goricar, V. Dolzan, A. Janez, Long-term efficacy of metformin in overweight-obese PCOS: longitudinal follow-up of retrospective cohort. Endocr. Connect 9(1), 44–54 (2020). https://doi.org/10.1530/EC-19-0449
T. Nagai, M. Imamura, M. Mori, Metformin use in an obese diabetic patient from weeks 1 to 21 of pregnancy. J. Med. 34(1–6), 163–168 (2003)
J. Grisouard, K. Timper, T.M. Radimerski, D.M. Frey, R. Peterli, B. Kola, M. Korbonits, P. Herrmann, S. Krähenbühl, H. Zulewski et al. Mechanisms of metformin action on glucose transport and metabolism in human adipocytes. Biochem. Pharmacol. 80(11), 1736–1745 (2010). https://doi.org/10.1016/j.bcp.2010.08.021
T.E. Lamoia, G.I. Shulman, Cellular and molecular mechanisms of metformin action. Endocr. Rev. 42(1), 77–96 (2021). https://doi.org/10.1210/endrev/bnaa023
B. Viollet, B. Guigas, N. Sanz Garcia, J. Leclerc, M. Foretz, F. Andreelli, Cellular and molecular mechanisms of metformin: an overview. Clin. Sci. 122(6), 253–270 (2012). https://doi.org/10.1042/CS20110386
Y. Naghiaee, R. Didehdar, F. Pourrajab, M. Rahmanian, N. Heiranizadeh, A. Mohiti, J. Mohiti-Ardakani, Metformin downregulates MiR223 expression in insulin-resistant 3T3L1 cells and human diabetic adipose tissue. Endocrine 70(3), 498–508 (2020). https://doi.org/10.1007/s12020-020-02459-2
S.C. Bridgeman, G.C. Ellison, P.E. Melton, P. Newsholme, C.D.S. Mamotte, Epigenetic effects of metformin: from molecular mechanisms to clinical implications. Diabetes, Obes. Metab. 20(7), 1553–1562 (2018). https://doi.org/10.1111/dom.13262
N. Alimoradi, N. Firouzabadi, R. Fatehi, Metformin and insulin-resistant related diseases: emphasis on the role of microRNAs. Biomed. Pharmacother. 139, 111662 (2021). https://doi.org/10.1016/j.biopha.2021.111662
P.B. Udesen, D. Glintborg, A.E. Sørensen, R. Svendsen, N.L.S. Nielsen, M.L.M. Wissing, M.S. Andersen, A.L.M. Englund, L.T. Dalgaard, Metformin decreases MiR-122, MiR-223 and MiR-29a in women with polycystic ovary syndrome. Endocr. Connect 9(11), 1075–1084 (2020). https://doi.org/10.1530/EC-20-0195
Y.-H. Chen, S. Heneidi, J.-M. Lee, L.C. Layman, D.W. Stepp, G.M. Gamboa, B.-S. Chen, G. Chazenbalk, R. Azziz, MiRNA-93 inhibits GLUT4 and is overexpressed in adipose tissue of polycystic ovary syndrome patients and women with insulin resistance. Diabetes 62(7), 2278–2286 (2013). https://doi.org/10.2337/db12-0963
G.D. Ferreira, A. Germeyer, A. De Barros Machado, T.L. Do Nascimento, T. Strowitzki, I.S. Brum, H. Von Eye Corleta, E. Capp, Metformin Modulates PI3K and GLUT4 expression and Akt/PKB phosphorylation in human endometrial stromal cells after stimulation with androgen and insulin. Eur. J. Obstet. Gynecol. Reprod. Biol. 175(1), 157–162 (2014). https://doi.org/10.1016/j.ejogrb.2014.01.009
M.F. Heber, S.R. Ferreira, G.A. Abruzzese, R. Trinidad, O.P. Pignataro, M. Vega, A.B. Motta, Metformin improves ovarian insulin signaling alterations caused by fetal programming. J. Endocrinol. 240(3), 431–443 (2019). https://doi.org/10.1530/JOE-18-0520
F. Wang, S. Wang, Z. Zhang, Q. Lin, Y. Liu, Y. Xiao, K. Xiao, Z. Wang, Defective insulin signaling and the protective effects of dimethyldiguanide during follicular development in the ovaries of polycystic ovary syndrome. Mol. Med. Rep. 16(6), 8164–8170 (2017). https://doi.org/10.3892/mmr.2017.7678
L. Hu, B. Wang, Y. Tao, Mitigating effect of metformin on polycystic ovarian syndrome and insulin resistance in rats, and the mechanisms involved. Trop. J. Pharm. Res. 19(9), 1941–1946 (2020). https://doi.org/10.4314/tjpr.v19i9.20
J.E. Gunton, P.J.D. Delhanty, S.I. Takahashi, R.C. Baxter, Metformin rapidly increases insulin receptor activation in human liver and signals preferentially through insulin-receptor substrate-2. J. Clin. Endocrinol. Metab. 88(3), 1323–1332 (2003). https://doi.org/10.1210/jc.2002-021394
X. Li, P. Cui, H.Y. Jiang, Y.R. Guo, B. Pishdari, M. Hu, Y. Feng, H. Billig, R. Shao, Reversing the reduced level of endometrial GLUT4 expression in polycystic ovary syndrome: a mechanistic study of metformin action. Am. J. Transl. Res. 7(3), 574–586 (2015)
J. Zhai, C.X. Liu, Z.R. Tian, Q.H. Jiang, Y.P. Sun, Effects of metformin on the expression of GLUT4 in endometrium of obese women with polycystic ovary syndrome. Biol. Reprod. 87(2), 1–5 (2012). https://doi.org/10.1095/biolreprod.112.099788
D. Ujvari, M. Hulchiy, A. Calaby, A. Nybacka, B. Byström, A.L. Hirschberg, Lifestyle intervention up-regulates gene and protein levels of molecules involved in insulin signaling in the endometrium of overweight/obese women with polycystic ovary syndrome. Hum. Reprod. 29(7), 1526–1535 (2014). https://doi.org/10.1093/humrep/deu114
Z. Polianskyte-Prause, T.A. Tolvanen, S. Lindfors, V. Dumont, M. Van, H. Wang, S.N. Dash, M. Berg, J.B. Naams, L.C. Hautala et al. Metformin increases glucose uptake and acts renoprotectively by reducing SHIP2 activity. FASEB J. 33(2), 2858–2869 (2019). https://doi.org/10.1096/fj.201800529RR
S. Rice, L.J. Pellatt, S.J. Bryan, S.A. Whitehead, H.D. Mason, Action of metformin on the insulin-signaling pathway and on glucose transport in human granulosa cells. J. Clin. Endocrinol. Metab 96(3), 427–435 (2011). https://doi.org/10.1210/jc.2010-2060
B. Sonntag, M. Götte, P. Wülfing, A.N. Schüring, L. Kiesel, R.R. Greb, Metformin alters insulin signaling and viability of human granulosa cells. Fertil. Steril. 84(SUPPL. 2), 1173–1179 (2005). https://doi.org/10.1016/j.fertnstert.2005.04.043
T.P. Ciaraldi, A.P.S. Kong, N.V. Chu, D.D. Kim, S. Baxi, M. Loviscach, R. Plodkowski, R. Reitz, M. Caulfield, S. Mudaliar et al. Regulation of glucose transport and insulin signaling by troglitazone or metformin in adipose tissue of type 2 diabetic subjects. Diabetes 51(1), 30–36 (2002). https://doi.org/10.2337/diabetes.51.1.30
S. Matthaei, J.P. Reibold, A. Hamann, H. Benecke, H.U. Häring, H. Greten, H.H. Klein, In vivo metformin treatment ameliorates insulin resistance: evidence for potentiation of insulin-induced translocation and increased functional activity of glucose transporters in obese (Fa/Fa) zucker rat adipocytes. Endocrinology 133(1), 304–311 (1993). https://doi.org/10.1210/endo.133.1.8391425
I.J. Kozka, G.D. Holman, Metformin blocks downregulation of cell surface GLUT4 caused by chronic insulin treatment of rat adipocytes. Diabetes 42(8), 1159–1165 (1993). https://doi.org/10.2337/diabetes.42.8.1159
G.N. Kraniou, D. Cameron-Smith, M. Hargreaves, Effect of short-term training on GLUT-4 MRNA and protein expression in human skeletal muscle. Exp. Physiol. 89(5), 559–563 (2004). https://doi.org/10.1113/expphysiol.2004.027409
S. Matthaei, A. Hamann, H.H. Klein, H. Benecke, G. Kreymann, J.S. Flier, H. Greten, Association of metformin’s effect to increase insulin-stimulated glucose transport with potentiation of insulin-induced translocation of glucose transporters from intracellular pool to plasma membrane in rat adipocytes. Diabetes 40(7), 850–857 (1991). https://doi.org/10.2337/diab.40.7.850
M. Ahmed, M.J. Neville, M.J. Edelmann, B.M. Kessler, F. Karpe, Proteomic analysis of human adipose tissue after rosiglitazone treatment shows coordinated changes to promote glucose uptake. Obesity 18(1), 27–34 (2010). https://doi.org/10.1038/oby.2009.208
J. Purintrapiban, S. Ratanachaiyavong, H. Mcshane, The effects of insulin and metformin on glucose uptake in L8 myotubes. ScienceAsia 29(4), 341 (2003). https://doi.org/10.2306/scienceasia1513-1874.2003.29.341
T.P. Ciaraldi, A. el-Roeiy, Z. Madar, D. Reichart, J.M. Olefsky, S.S. Yen, Cellular mechanisms of insulin resistance in polycystic ovarian syndrome. J. Clin. Endocrinol. Metab. 75(2), 577–583 (1992). https://doi.org/10.1210/jcem.75.2.1322430
D.A. Dumesic, J.D. Phan, K.L. Leung, T.R. Grogan, X. Ding, X. Li, L.R. Hoyos, D.H. Abbott, G.D. Chazenbalk, Adipose insulin resistance in normal-weight women with polycystic ovary syndrome. J. Clin. Endocrinol. Metab. 104(6), 2171–2183 (2019). https://doi.org/10.1210/jc.2018-02086
W. Chang, M.O. Goodarzi, H. Williams, D.A. Magoffin, M. Pall, R. Azziz, Adipocytes from women with polycystic ovary syndrome demonstrate altered phosphorylation and activity of glycogen synthase kinase 3. Fertil. Steril. 90(6), 2291–2297 (2008). https://doi.org/10.1016/j.fertnstert.2007.10.025
G. Chazenbalk, P. Singh, D. Irge, A. Shah, D.H. Abbott, D.A. Dumesic, Androgens inhibit adipogenesis during human adipose stem cell commitment to preadipocyte formation. Steroids 78(9), 920–926 (2013). https://doi.org/10.1016/j.steroids.2013.05.001
S.C. Fisch, A.F. Nikou, E.A. Wright, J.D. Phan, K.L. Leung, T.R. Grogan, D.H. Abbott, G.D. Chazenbalk, D.A. Dumesic, Precocious subcutaneous abdominal stem cell development to adipocytes in normal-weight women with polycystic ovary syndrome. Fertil. Steril. 110(7), 1367–1376 (2018). https://doi.org/10.1016/j.fertnstert.2018.08.042
S. Virtue, A. Vidal-Puig, It’s not how fat you are, it’s what you do with it that counts. PLoS Biol. 6(9), e237 (2008). https://doi.org/10.1371/journal.pbio.0060237
R.H. Unger, G.O. Clark, P.E. Scherer, L. Orci, Lipid homeostasis, lipotoxicity and the metabolic syndrome. Biochim. Biophys. Acta 1801(3), 209–214 (2010). https://doi.org/10.1016/j.bbalip.2009.10.006
G.I. Shulman, Ectopic fat in insulin resistance, dyslipidemia, and cardiometabolic disease. N. Engl. J. Med. 371(12), 1131–1141 (2014). https://doi.org/10.1056/NEJMra1011035
Y. Cao, N. Gathaiya, Q. Han, B.J. Kemp, M.D. Jensen, Subcutaneous adipose tissue free fatty acid uptake measured using positron emission tomography and adipose biopsies in humans. Am. J. Physiol. Endocrinol. Metab. 317(2), E194–E199 (2019). https://doi.org/10.1152/ajpendo.00030.2019
A.H. Ali, C. Koutsari, M. Mundi, M.D. Stegall, J.K. Heimbach, S.J. Taler, J. Nygren, A. Thorell, L.D. Bogachus, L.P. Turcotte et al. Free fatty acid storage in human visceral and subcutaneous adipose tissue: role of adipocyte proteins. Diabetes 60(9), 2300–2307 (2011). https://doi.org/10.2337/db11-0219
N. Al-Sari, T. Suvitaival, I. Mattila, A. Ali, L. Ahonen, K. Trost, T.F. Henriksen, F. Pociot, L.O. Dragsted, C. Legido-Quigley, Lipidomics of human adipose tissue reveals diversity between body areas. PLoS One 15(6), e0228521 (2020)
J.G. Boyle, P.J. Logan, G.C. Jones, M. Small, N. Sattar, J.M.C. Connell, S.J. Cleland, I.P. Salt, AMP-activated protein kinase is activated in adipose tissue of individuals with type 2 diabetes treated with metformin: a randomised glycaemia-controlled crossover study. Diabetologia 54(7), 1799–1809 (2011). https://doi.org/10.1007/s00125-011-2126-4
Acknowledgements
We thank the study participants. We appreciate the assistance of Mirela Ozura, Elizabeta Stepanovic and Melita Dolenc, RNs. We wish to acknowledge Mrs. Savica Soldat, B.S., for her expert technical assistance with RNA isolation and assist. Tanja Blagus, B.S. for gene expression analyses.
Funding
This research was funded by Slovenian Research Agency, grant numbers #P3-0298 and P1-0170.
Author information
Authors and Affiliations
Contributions
Conceptualization: A.J. and M.J.; methodology: K.G., M.J., V.D.; formal analysis: K.G., M.J., N.A.K.; writing—original draft preparation: M.J., N.A.K., R.H.; writing—review and editing: A.J., M.R., V.D. All authors have read and agreed to the published version of the paper.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that the current research was conducted independently. Mojca Jensterle has given lectures, received honoraria and participated in conferences, advisory boards sponsored by pharmaceutical companies including Amgen, Pfeizer, Novo Nordisk, Novartis. Andrej Janez has given lectures, received honoraria and research support, and participated on Speakers Bureaus, advisory boards and clinical trials sponsored by pharmaceutical companies including AstraZeneca, Boehringer Ingelheim, Eli Lilly, Merck Sharp & Dohme, Novo Nordisk, Medtronic and Sanofi. Manfredi Rizzo is a full-time Professor of Internal Medicine at the University of Palermo, Italy, and currently Medical Director in Novo Nordisk Eastern Europe; he has given lectures, received honoraria and research support, and participated in conferences, advisory boards and clinical trials sponsored by many pharmaceutical companies including Amgen, AstraZeneca, Boehringer Ingelheim, Kowa, Eli Lilly, Meda, Mylan, Merck Sharp & Dohme, Novo Nordisk, Novartis, Roche Diagnostics, Sanofi and Servier. None of the above had any role in this article, which has been written independently, without any financial or professional help, and reflects only the opinion of the authors, without any role of the industry.
Consent to participate and for publication
All subjects were informed of the study aims and provided written consent to participate in a study and have their data published in a journal article.
Ethical approval
The study was conducted according to the guidelines of the Declaration of Helsinki and its later amendment and was approved by the National Ethical Committee (protocol code 0120101/2018/18).
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Jensterle, M., Kravos, N.A., Dolžan, V. et al. Glucose transporter 4 mRNA expression in subcutaneous adipose tissue of women with PCOS remains unchanged despite metformin withdrawal: is there a cellular metabolic treatment legacy effect?. Endocrine 75, 804–813 (2022). https://doi.org/10.1007/s12020-021-02934-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-021-02934-4