Abstract
Purpose
Primary hyperparathyroidism (PHPT) is associated with increased risk of cardiovascular morbidity and mortality. We aim to determine whether parathyroidectomy (PTX) can change cardiometabolic risk factors including serum lipids, glycemic parameters, systolic and diastolic blood pressure, C reactive protein (CRP), and body mass index (BMI).
Methods
MEDLINE, Web of Science, Scopus, and Google Scholar were searched for relevant articles published till June 2020. Fixed-effect or random-effects models were used to estimate the weighted mean difference (WMD) and 95% CI for outcomes where applicable.
Results
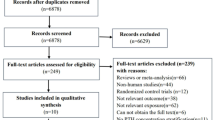
In total, 34 studies were eligible to be included in the current meta-analysis. Our results indicated no favorable change in serum triglyceride (n = 13, WMD = −0.06, 95% CI: −0.15, 0.03 mmol/L), total cholesterol (n = 15, WMD = 0.01, 95% CI: −0.14, 0.16 mmol/L), LDL-C (n = 10, WMD = −0.01, 95% CI: −0.17, 0.19 mmol/L), HDL-C (n = 10, WMD = 0.03, 95% CI: −0.001, 0.06 mmol/L), and CRP (n = 5, WMD = 0.82, 95% CI: −0.01, 1.64 mg/L) after PTX in PHPT patients. However, glucose (n = 24, WMD = −0.16, 95% CI: −0.26, −0.06 mmol/L), serum insulin (n = 12, WMD = −1.11, 95% CI: −1.73, −0.49 µIU/mL), systolic (n = 17, WMD = −10.14, 95% CI: −12.27, −8.01 mmHg), and diastolic (n = 16, WMD = −5.21, 95% CI: −7.0, −3.43 mmHg) blood pressures were decreased after PTX, whilst a significant increase was observed in BMI (n = 13, WMD = 0.35, 95% CI: 0.19, 0.51 kg/m2).
Conclusions
PTX could improve glycemic parameters and blood pressure, without any significant change in serum lipoproteins and CRP.





Similar content being viewed by others
Data availability
Data will be available on request.
References
S. Minisola, J. Pepe, S. Piemonte, C. Cipriani, The diagnosis and management of hypercalcaemia. BMJ 350, h2723 (2015). https://doi.org/10.1136/bmj.h2723
B.L. Clarke, Epidemiology of primary hyperparathyroidism. J. Clin. Densitom. 16, 8–13 (2013). https://doi.org/10.1016/j.jocd.2012.11.009
D.M. Press, A.E. Siperstein, E. Berber et al. The prevalence of undiagnosed and unrecognized primary hyperparathyroidism: a population-based analysis from the electronic medical record. Surgery 154, 1232–1238 (2013). https://doi.org/10.1016/j.surg.2013.06.051
S. Minisola, Primary hyperparathyroidism is one of the three most frequent endocrine disorders, typically diagnosed in the years following menopause and with advancing age. J. Endocrinol. Invest. 35(7 Suppl), 1 (2012)
J.P. Bilezikian, Primary hyperparathyroidism. J. Clin. Endocrinol. Metab. 103, 3993–4004 (2018). https://doi.org/10.1210/jc.2018-01225
A.A. Khan, J.P. Bilezikian, J.T. Potts Jr, Hyperparathyroidism GEftTIWoAP. The diagnosis and management of asymptomatic primary hyperparathyroidism revisited. (2009). https://doi.org/10.1210/jc.2008-1757
M. Procopio, G. Magro, F. Cesario et al. The oral glucose tolerance test reveals a high frequency of both impaired glucose tolerance and undiagnosed Type 2 diabetes mellitus in primary hyperparathyroidism. Diabet. Med. 19, 958–61 (2002). https://doi.org/10.1046/j.1464-5491.2002.00809.x
M.J. Bolland, A.B. Grey, G.D. Gamble, I.R. Reid, Association between primary hyperparathyroidism and increased body weight: a meta-analysis. J. Clin. Endocrinol. Metab. 90, 1525–1530 (2005). https://doi.org/10.1210/jc.2004-1891
S. Ljunghall, H. Lithell, B. Vessby, L. Wide, Glucose and lipoprotein metabolism in primary hyperparathyroidism. Effects of parathyroidectomy. Acta Endocrinol. 89, 580–589 (1978). https://doi.org/10.1530/acta.0.0890580
S. Ljunghall, M. Palmér, G. Akerström, L. Wide, Diabetes mellitus, glucose tolerance and insulin response to glucose in patients with primary hyperparathyroidism before and after parathyroidectomy. Eur. J. Clin. Investig. 13, 373–377 (1983). https://doi.org/10.1111/j.1365-2362.1983.tb00116.x
P. Farahnak, G. Lärfars, M. Sten-Linder, I.L. Nilsson, Mild primary hyperparathyroidism: vitamin D deficiency and cardiovascular risk markers. J. Clin. Endocrinol. Metab. 96, 2112–2118 (2011). https://doi.org/10.1210/jc.2011-0238
E. Hagström, E. Lundgren, H. Lithell et al. Normalized dyslipidaemia after parathyroidectomy in mild primary hyperparathyroidism: population-based study over five years. Clin. Endocrinol. 56, 253–260 (2002). https://doi.org/10.1046/j.0300-0664.2001.01468.x
S.J. Silverberg, B.L. Clarke, M. Peacock et al. Current issues in the presentation of asymptomatic primary hyperparathyroidism: proceedings of the Fourth International Workshop. J. Clin. Endocrinol. Metab. 99, 3580–3594 (2014). https://doi.org/10.1210/jc.2014-1415
F. Tassone, M. Maccario, L. Gianotti et al. Insulin sensitivity in normocalcaemic primary hyperparathyroidism. Endocrine 44, 812–814 (2013). https://doi.org/10.1007/s12020-013-0059-z
J. Sancho, J. Rouco, R. Riera-Vidal, A. Sitges-Serra, Long-term effects of parathyroidectomy for primary hyperparathyroidism on arterial hypertension. World J. Surg. 16, 732–735 (1992). https://doi.org/10.1007/BF02067371
D. Jones, J. Jones, H. Lloyd, P. Lucas, W. Wilkins, D. Walker, Changes in blood pressure and renal function after parathyroidectomy in primary hyperparathyroidism. Postgrad. Med. J. 59, 350–353 (1983). https://doi.org/10.1136/pgmj.59.692.350
J. Bollerslev, T. Rosen, C.L. Mollerup et al. Effect of surgery on cardiovascular risk factors in mild primary hyperparathyroidism. J. Clin. Endocrinol. Metab. 94, 2255–61 (2009). https://doi.org/10.1210/jc.2008-2742
K. Godang, K. Lundstam, C. Mollerup et al. The effect of surgery on fat mass, lipid and glucose metabolism in mild primary hyperparathyroidism. Endocr. Connect. 7, 941–948 (2018). https://doi.org/10.1530/EC-18-0259
E. Rydberg, M. Birgander, A.-G. Bondeson, L. Bondeson, R. Willenheimer, Effect of successful parathyroidectomy on 24-hour ambulatory blood pressure in patients with primary hyperparathyroidism. Int. J. Cardiol. 142, 15–21 (2010). https://doi.org/10.1016/j.ijcard.2008.12.027
A. Liberati, D.G. Altman, J. Tetzlaff et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. J. Clin. Epidemiol. 62, e1–e34 (2009). https://doi.org/10.1016/j.jclinepi.2009.06.006
J.P. Higgins, S.G. Thompson, Quantifying heterogeneity in a meta‐analysis. Stat. Med. 21, 1539–58 (2002). https://doi.org/10.1002/sim.1186
R. DerSimonian, N. Laird, Meta-analysis in clinical trials. Control Clin. Trials 7, 177–88 (1986). https://doi.org/10.1016/0197-2456(86)90046-2
M. Egger, G.D. Smith, M. Schneider, C. Minder, Bias in meta-analysis detected by a simple, graphical test. BMJ 315, 629–34 (1997). https://doi.org/10.1136/bmj.315.7109.629
M. Egger, G. Davey-Smith, D. Altman. Systematic Reviews in Health Care: Meta-analysis in Context (John Wiley & Sons, UK, 2008)
I.L. Nilsson, J. Aberg, J. Rastad, L. Lind, Left ventricular systolic and diastolic function and exercise testing in primary hyperparathyroidism-effects of parathyroidectomy. Surgery 128, 895–902 (2000). https://doi.org/10.1067/msy.2000.110240
M. Kızılgül, M. Çalışkan, S. Beysel, M. Özbek, E. Çakal, Effect of parathyroidectomy on epicardial fat thickness as a cardiovascular risk factor in patients with primary hyperparathyroidism. Turk. J. Med. Sci. 49, 1165–1169 (2019). https://doi.org/10.3906/sag-1902-40
H. Ejlsmark-Svensson, L. Rolighed, L. Rejnmark, Effect of parathyroidectomy on cardiovascular risk factors in primary hyperparathyroidism: a randomized clinical trial. J. Clin. Endocrinol. Metab. 104, 3223–32 (2019). https://doi.org/10.1210/jc.2018-02456
S. Beysel, M. Caliskan, M. Kizilgul et al. Parathyroidectomy improves cardiovascular risk factors in normocalcemic and hypercalcemic primary hyperparathyroidism. BMC Cardiovasc. Disord. 19, 106 (2019). https://doi.org/10.1186/s12872-019-1093-4
S. Storvall, E.M. Ryhänen, I. Heiskanen, H. Sintonen, R.P. Roine, C. Schalin-Jäntti, Surgery significantly improves neurocognition, sleep, and blood pressure in primary hyperparathyroidism: a 3-year prospective follow-up study. Horm. Metab. Res. 49, 772–777 (2017). https://doi.org/10.1055/s-0043-118347
M. Karakose, M. Caliskan, M.S. Arslan, T. Demirci, S. Karakose, E. Cakal, The impact of parathyroidectomy on serum ADAMTS1, ADAMTS4 levels, insulin resistance, and subclinical cardiovascular disease in primary hyperparathyroidism. Endocrine 55, 283–288 (2017). https://doi.org/10.1007/s12020-016-1175-3
R. Putnam, D.P. Dhibar, S. Varshney et al. Effect of curative parathyroidectomy on insulin resistance. Indian J. Endocrinol. Metab. 20, 784–789 (2016). https://doi.org/10.4103/2230-8210.192916
I.L. Nilsson, S. Norenstedt, F. Granath, J. Zedenius, Y. Pernow, T.E. Larsson, FGF23, metabolic risk factors, and blood pressure in patients with primary hyperparathyroidism undergoing parathyroid adenomectomy. Surgery 159, 211–217 (2016). https://doi.org/10.1016/j.surg.2015.06.057
G.B. Cansu, N. Yılmaz, S. Özdem et al. Parathyroidectomy in asymptomatic primary hyperparathyroidism reduces carotid intima-media thickness and arterial stiffness. Clin. Endocrinol. 84, 39–47 (2016). https://doi.org/10.1111/cen.12952
G. Cvijovic, D. Micic, A. Kendereski et al. The effect of parathyroidectomy on insulin sensitivity in patients with primary hyperparathyroidism—an never ending story? Exp. Clin. Endocrinol. Diabetes 123, 336–41 (2015). https://doi.org/10.1055/s-0035-1549906
M.D. Walker, T. Rundek, S. Homma et al. Effect of parathyroidectomy on subclinical cardiovascular disease in mild primary hyperparathyroidism. Eur. J. Endocrinol. 167, 277–85 (2012). https://doi.org/10.1530/EJE-12-0124
P. Luigi, F.M. Chiara, Z. Laura et al. Arterial hypertension, metabolic syndrome and subclinical cardiovascular organ damage in patients with asymptomatic primary hyperparathyroidism before and after parathyroidectomy: preliminary results. Int. J. Endocrinol. 2012, 408295 (2012). https://doi.org/10.1155/2012/408295
E.G. Almqvist, A.G. Bondeson, L. Bondeson, D. Mellström, J. Svensson, Factors influencing insulin sensitivity in patients with mild primary hyperparathyroidism before and after parathyroidectomy. Scand. J. Clin. Lab. Investig. 72, 92–99 (2012). https://doi.org/10.3109/00365513.2011.634432
A. Ishay, P. Herer, R. Luboshitzky, Effects of successful parathyroidectomy on metabolic cardiovascular risk factors in patients with severe primary hyperparathyroidism. Endocr. Pract. 17, 584–90 (2011). https://doi.org/10.4158/EP10321.OR
P.D. Broulik, A. Brouliková, S. Adámek et al. Improvement of hypertension after parathyroidectomy of patients suffering from primary hyperparathyroidism. Int. J. Endocrinol. 2011, 309068 (2011). https://doi.org/10.1155/2011/309068
S.K. Bhadada, A. Bhansali, V.N. Shah, D.S. Rao, Changes in serum leptin and adiponectin concentrations and insulin resistance after curative parathyroidectomy in moderate to severe primary hyperparathyroidism. Singap Med. J. 52, 890–893 (2011)
A. Heyliger, V. Tangpricha, C. Weber, J. Sharma, Parathyroidectomy decreases systolic and diastolic blood pressure in hypertensive patients with primary hyperparathyroidism. Surgery 146, 1042–1047 (2009). https://doi.org/10.1016/j.surg.2009.09.024
A.A. Khaleeli, J.N. Johnson, W.H. Taylor, Prevalence of glucose intolerance in primary hyperparathyroidism and the benefit of parathyroidectomy. Diabetes Metab. Res. Rev. 23, 43–48 (2007). https://doi.org/10.1002/dmrr.637
S. Valdemarsson, P. Lindblom, A. Bergenfelz, Metabolic abnormalities related to cardiovascular risk in primary hyperparathyroidism: effects of surgical treatment. J. Intern. Med. 244, 241–249 (1998). https://doi.org/10.1046/j.1365-2796.1998.00366.x
A. Kautzky-Willer, G. Pacini, B. Niederle, G. Schernthaner, R. Prager, Insulin secretion, insulin sensitivity and hepatic insulin extraction in primary hyperparathyroidism before and after surgery. Clin. Endocrinol. 37, 147–55 (1992). https://doi.org/10.1111/j.1365-2265.1992.tb02299.x
R. Prager, G. Schernthaner, B. Niederle, R. Roka, Evaluation of glucose tolerance, insulin secretion, and insulin action in patients with primary hyperparathyroidism before and after surgery. Calcif. Tissue Int. 46, 1–4 (1990). https://doi.org/10.1007/BF02555816
K. Brismar, S. Werner, E. Bucht, L. Wetterberg, Melatonin, cortisol, prolactin, and calcitonin secretion in primary hyperparathyroidism before and after surgery. J. Pineal Res. 4, 277–85 (1987). https://doi.org/10.1111/j.1600-079x.1987.tb00865.x
P.D. Broulik, K. Horký, V. Pacovský, Blood pressure in patients with primary hyperparathyroidism before and after parathyroidectomy. Exp. Clin. Endocrinol. 86, 346–52 (1985). https://doi.org/10.1055/s-0029-1210507
J.D. Ringe, Reversible hypertension in primary hyperparathyroidism-pre- and posteroperative blood pressure in 75 cases. Klin. Wochenschr. 62, 465–469 (1984). https://doi.org/10.1007/BF01726908
N.D. Vaziri, L. Wellikson, G. Gwinup, C. Byrne, Lipid fractions in primary hyperparathyroidism before and after surgical cure. Acta Endocrinol. 102, 539–42 (1983). https://doi.org/10.1530/acta.0.1020539
T. Christensson, K. Einarsson, Serum lipids before and after parathyroidectomy in patients with primary hyperparathyroidism. Clin. Chim. Acta 78, 411–415 (1977). https://doi.org/10.1016/0009-8981(77)90074-2
T. Madhavan, B. Frame, M.A. Block, Influence of surgical correction of primary hyperparathyroidism on associated hypertension. Arch. Surg. 100, 212–214 (1970). https://doi.org/10.1001/archsurg.1970.01340200100022
A. Rudman, E.R. Pearson, D. Smith, R. Srivastava, M.J. Murphy, G.P. Leese, Insulin resistance before and after parathyroidectomy in patients with primary hyperparathyroidism—a pilot study. Endocr. Res. 35, 85–93 (2010). https://doi.org/10.3109/07435801003724503
M.D. Walker, S.J. Silverberg, Cardiovascular aspects of primary hyperparathyroidism. J. Endocrinol. Investig. 31, 925–31 (2008). https://doi.org/10.1007/BF03346443
N. Garcia de la Torre, J.A. Wass, H.E. Turner, Parathyroid adenomas and cardiovascular risk. Endocr. Relat. Cancer 10, 309–22 (2003). https://doi.org/10.1677/erc.0.0100309
P. Andersson, E. Rydberg, R. Willenheimer, Primary hyperparathyroidism and heart disease—a review. Eur. Heart J. 25, 1776–87 (2004). https://doi.org/10.1016/j.ehj.2004.07.010
T. Ahlström, E. Hagström, A. Larsson, C. Rudberg, L. Lind, P. Hellman, Correlation between plasma calcium, parathyroid hormone (PTH) and the metabolic syndrome (MetS) in a community-based cohort of men and women. Clin. Endocrinol. 71, 673–678 (2009). https://doi.org/10.1111/j.1365-2265.2009.03558.x
E. Hagström, K. Michaëlsson, H. Melhus et al. Plasma-parathyroid hormone is associated with subclinical and clinical atherosclerotic disease in 2 community-based cohorts. Arterioscler. Thromb. Vasc. Biol. 34, 1567–73 (2014). https://doi.org/10.1161/ATVBAHA.113.303062
R. Jorde, K.H. Bonaa, J. Sundsfjord, Population based study on serum ionised calcium, serum parathyroid hormone, and blood pressure. The Tromsø study. Eur. J. Endocrinol. 141, 350–357 (1999). https://doi.org/10.1530/eje.0.1410350
L. Lind, S. Jacobsson, M. Palmér, H. Lithell, B. Wengle, S. Ljunghall, Cardiovascular risk factors in primary hyperparathyroidism: a 15-year follow-up of operated and unoperated cases. J. Intern. Med. 230, 29–35 (1991). https://doi.org/10.1111/j.1365-2796.1991.tb00403.x
A. Bergenfelz, A. Bladström, M. Their, E. Nordenström, S. Valdemarsson, J. Westerdahl, Serum levels of uric acid and diabetes mellitus influence survival after surgery for primary hyperparathyroidism: a prospective cohort study. World J. Surg. 31, 1393–1400 (2007). https://doi.org/10.1007/s00268-007-9091-6
S. Kumar, A.O. Olukoga, C. Gordon et al. Impaired glucose tolerance and insulin insensitivity in primary hyperparathyroidism. Clin. Endocrinol. 40, 47–53 (1994). https://doi.org/10.1111/j.1365-2265.1994.tb02442.x
H. Kim, R.K. Kalkhoff, N.V. Costrini, J.M. Cerletty, M. Jacobson, Plasma insulin disturbances in primary hyperparathyroidism. J. Clin. Investig. 50, 2596–605 (1971). https://doi.org/10.1172/JCI106760
S.N. Karras, T. Koufakis, X. Tsekmekidou, V. Antonopoulou, P. Zebekakis, K. Kotsa, Increased parathyroid hormone is associated with higher fasting glucose in individuals with normocalcemic primary hyperparathyroidism and prediabetes: a pilot study. Diabetes Res. Clin. Pract. 160, 107985 (2020). https://doi.org/10.1016/j.diabres.2019.107985
A. Tomaschitz, E. Ritz, B. Pieske et al. Aldosterone and parathyroid hormone interactions as mediators of metabolic and cardiovascular disease. Metabolism 63, 20–31 (2014). https://doi.org/10.1016/j.metabol.2013.08.016
E. Kamycheva, J. Sundsfjord, R. Jorde, Serum parathyroid hormone levels predict coronary heart disease: the Tromsø study. Eur. J. Cardiovasc. Prev. Rehabilit. 11, 69–74 (2004). https://doi.org/10.1097/01.hjr.0000114706.27531.01
E.G. Almqvist, A.G. Bondeson, L. Bondeson, J. Svensson, Increased markers of inflammation and endothelial dysfunction in patients with mild primary hyperparathyroidism. Scand. J. Clin. Lab. Investig. 71, 139–44 (2011). https://doi.org/10.3109/00365513.2010.543694
E. Osto, F. Fallo, M.R. Pelizzo et al. Coronary microvascular dysfunction induced by primary hyperparathyroidism is restored after parathyroidectomy. Circulation 126, 1031–1039 (2012). https://doi.org/10.1161/CIRCULATIONAHA.111.081307
S. Iwata, M.D. Walker, M.R. Di Tullio et al. Aortic valve calcification in mild primary hyperparathyroidism. J. Clin. Endocrinol. Metab. 97, 132–137 (2012). https://doi.org/10.1210/jc.2011-2107
S.S. Thomas, W.E. Mitch, Parathyroid hormone stimulates adipose tissue browning: a pathway to muscle wasting. Curr. Opin. Clin. Nutr. Metab. Care 20(3), 153–157 (2017). https://doi.org/10.1097/MCO.0000000000000357
M.H. Christensen, S.N. Dankel, Y. Nordbø et al. Primary hyperparathyroidism influences the expression of inflammatory and metabolic genes in adipose tissue. PLoS ONE 6(6), e20481 (2011). https://doi.org/10.1371/journal.pone.0020481
C.C. Solorzano, W. Mendez, J.I. Lew et al. Long-term outcome of patients with elevated parathyroid hormone levels after successful parathyroidectomy for sporadic primary hyperparathyroidism. Arch. Surg. 143(7), 659–663 (2008). https://doi.org/10.1001/archsurg.143.7.659
Acknowledgements
We thank Isfahan University of Medical Sciences, Isfahan, Iran to support this work.
Funding
This work was supported by grants from Isfahan University of Medical Sciences, Isfahan, Iran (No: 299066).
Author information
Authors and Affiliations
Contributions
M.Y. and H.R. contributed to the concept. M.Y., F.H., and A.G. searched databases, screened articles, and extracted data. A.F. contributed to data synthesis and analysis. M.Y., F.H., and A.G. contributed to paper drafting. All steps were performed under the supervision of H.R. All authors read the final version of paper and approved it.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Yavari, M., Feizi, A., Haghighatdoost, F. et al. The influence of parathyroidectomy on cardiometabolic risk factors in patients with primary hyperparathyroidism: a systematic review and meta-analysis. Endocrine 72, 72–85 (2021). https://doi.org/10.1007/s12020-020-02519-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-020-02519-7