Abstract
Purpose
We investigated the impact of different cut-offs on the prevalence of 25-hydroxyvitamin D [25-(OH)D] deficiency.
Methods
We used baseline data of 4149 participants (45–75 years, 50% women) of the population-based Heinz Nixdorf Recall study. Serum 25-(OH)D was measured with the Roche Cobas assay. Quartiles (p25, p50, and p75) were calculated. Data were stratified by months, sex, and age. According to the recommendations of ‘Dachverband Osteologie’, Endocrine Society and National Institute of Health we used 25-(OH)D thresholds of 12, 20, and 30 ng/ml to estimate vitamin D deficiency.
Results
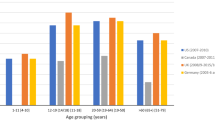
Overall the median of 25-(OH)D was 19.8 ng/ml (p25 = 14.4 ng/ml, p75 = 26.6 ng/ml), with highest concentrations in July (p50 = 23.8 ng/ml, p25 = 18.2 ng/ml, and p75 = 31.2 ng/ml) and lowest in March (p50 = 15.8 ng/ml, p25 = 11.5 ng/ml, and p75 = 20.6 ng/ml). Prevalence of vitamin D deficiency rose from 16, 51 up to 83% using the cut-offs of <12, <20 ng/ml, and <30 ng/ml, respectively. With respect to seasonal variance, prevalence of vitamin D deficiency rose to 92% in February/March using the cut-off <30 ng/ml (<12: 28%, <20 ng/ml: 71%) whereas in June/July prevalence of vitamin D deficiency decreased to 71% (<12: 6%, <20 ng/ml: 30%). The chance to attest the diagnosis of vitamin D deficiency for cut-off 12 ng/ml in March is 6.4-fold higher than in June, for cut-off 20 ng/ml, 5.5-fold higher and for cut-off 30 ng/ml, 3.1-fold higher.
Conclusions
Guidelines to define vitamin D deficiency revealed extremely different prevalence rates ranging between 6 and 92%. Accounting for collection time and antecedent sun exposure are important to reduce bias in research studies and improve decision-making in clinical care. Vitamin D thresholds have to be rethought.

Similar content being viewed by others
References
M.C. Chapuy, P. Preziosi, M. Maamer et al., Prevalence of vitamin D insufficiency in an adult normal population. Osteoporos. Int. 7, 439–443 (1997)
M.F. Holick, High prevalence of vitamin D inadequacy and implications for health. Mayo Clin. Proc. 81, 353–373 (2006)
Bundesinstitut für Risikobewertung: http://www.bfr.bund.de/de/ausgewaehlte_fragen_und_antworten_zu_vitamin_d-131898.html (2012). Accessed 22 Oct 2016
T. Kulie, A. Groff, J. Redmer, J. Hounshell, S. Schrager, Vitamin D: an evidence-based review. J. Am. Board Fam. Med. 22, 698–706 (2009)
J.S. Adams, M. Hewison, Update in vitamin D. J. Clin. Endocrinol. Metab. 95, 471–478 (2010)
S.S. Sherman, B.W. Hollis, J.D. Tobin, Vitamin D status and related parameters in a healthy population: the effects of age, sex, and season. J. Clin. Endocrinol. Metab. 71, 405–413 (1990)
H.A. Bischoff-Ferrari, D.P. Kiel, B. Dawson-Hughes et al., Dietary calcium and serum 25-hydroxyvitamin D status in relation to BMD among U.S. adults. J. Bone Miner. Res. 24, 935–942 (2009)
J.A. Cauley, A.Z. Lacroix, L. Wu et al., Serum 25-hydroxyvitamin D concentrations and risk for hip fractures. Ann. Intern. Med. 149, 242–250 (2008)
H. Dobnig, S. Pilz, H. Scharnagl et al., Independent association of low serum 25-hydroxyvitamin d and 1,25-dihydroxyvitamin d levels with all-cause and cardiovascular mortality. Arch. Intern. Med. 168, 1340–1349 (2008)
D.M. Lee, M.K. Rutter, T.W. O’Neill et al., Vitamin D, parathyroid hormone and the metabolic syndrome in middle-aged and older European men. Eur. J. Endocrinol. 161, 947–954 (2009)
S.K. Kunutsor, T.A. Apekey, M. Steur, Vitamin D and risk of future hypertension: meta-analysis of 283,537 participants. Eur. J. Epidemiol. 28, 205–221 (2013)
R.L. Prince, N. Austin, A. Devine, I.M. Dick, D. Bruce, K. Zhu, Effects of ergocalciferol added to calcium on the risk of falls in elderly high-risk women. Arch. Intern. Med. 168, 103–108 (2008)
H. van der Rhee, J.W. Coebergh, E. de Vries, Is prevention of cancer by sun exposure more than just the effect of vitamin D? A systematic review of epidemiological studies. Eur. J. Cancer 49, 1422–1436 (2013)
B. Pozuelo-Moyano, J. Benito-Leon, A.J. Mitchell, J. Hernandez-Gallego, A. Systematic, Review of randomized, double-blind, placebo-controlled trials examining the clinical efficacy of vitamin D in multiple sclerosis. Neuroepidemiology 40, 147–153 (2012)
C. Mathieu, C. Gysemans, A. Giulietti, R. Bouillon, Vitamin D and diabetes. Diabetologia 48, 1247–1257 (2005)
C. Balion, L.E. Griffith, L. Strifler et al., Vitamin D, cognition, and dementia: a systematic review and meta-analysis. Neurology. 79, 1397–1405 (2012)
S. Straube, S. Derry, R.A. Moore, H.J. McQuay, Vitamin D for the treatment of chronic painful conditions in adults. Cochrane. Database. Syst. Rev. 1, CD007771 (2010)
X. Guillot, L. Semerano, N. Saidenberg-Kermanac’h, G. Falgarone, M.C. Boissier, Vitamin D and inflammation. Joint Bone Spine 77, 552–557 (2010)
G. Bjelakovic, L. Gluud, D. Nikolova et al., Vitamin D supplementation for prevention of mortality in adults. Cochrane Database Syst. Rev. 7, CD007470 (2011)
K.C. Norris, S.F. Williams, Race/ethnicity, serum 25-hydroxyvitamin D, and heart disease. JAMA 310, 153–155 (2013)
M.C. Robertson, L.D. Gillespie, Fall prevention in community-dwelling older adults. JAMA 309, 1406–1407 (2013)
DVO-LEITLINIE: http://www.dv-osteologie.org/dvo_leitlinien/osteoporose-leitlinie-2014 (2014). Accessed 22 Oct 2016
National Institutes of Health: http://ods.od.nih.gov/factsheets/Vitamin-D-HealthProfessional/#h5 (2014). Accessed 22 Oct 2016
Endocrine society: http://www.hormone.org/patient-guides/2011/vitamin-D-deficiency (2014). Accessed 22 Oct 2016
A. Schmermund, S. Möhlenkamp, A. Stang et al., Assessment of clinically silent atherosclerotic disease and established and novel risk factors for predicting myocardial infarction and cardiac death in healthy middle-aged subjects: rationale and design of the Heinz Nixdorf RECALL Study. Risk factors, evaluation of coronary calcium and lifestyle. Am. Heart J. 144, 212–218 (2002)
A. Stang, S. Moebus, N. Dragano et al., Baseline recruitment and analyses of nonresponse of the Heinz Nixdorf recall study: identifiability of phone numbers as the major determinant of response. Eur. J. Epidemiol. 20, 489–496 (2005)
C. Agborsangaya, A.T. Toriola, K. Grankvist et al., The effects of storage time and sampling season on the stability of serum 25-hydroxy vitamin D and androstenedione. Nutr. Cancer 62, 51–57 (2010)
E. Klingberg, G. Oleröd, J. Konar et al., Seasonal variations in serum 25-hydroxy vitamin D levels in a Swedish cohort. Endocrine 49, 800–808 (2015)
M.J. Bolland, A.B. Grey, R.W. Ames et al., The effects of seasonal variation of 25-hydroxyvitamin D and fat mass on a diagnosis of vitamin D sufficiency. Am. J. Clin. Nutr. 86, 959–964 (2007)
R. Jorde, M. Sneve, M. Hutchinson, N. Emaus, Y. Figenschau, G. Grimnes, Tracking of serum 25-hydroxyvitamin D levels during 14 years in a population-based study and during 12 months in an intervention study. Am. J. Epidemiol. 171, 903–908 (2010)
T.C. Stamp, J.M. Round, Seasonal changes in human plasma levels of 25-hydroxyvitamin D. Nature 247, 563–565 (1974)
A.B. Shoben, B. Kestenbaum, G. Levin et al., Seasonal variation in 25-hydroxyvitamin D concentrations in the cardiovascular health study. Am. J. Epidemiol. 174, 1363–1372 (2011)
P. Vuistiner, V. Rousson, H. Henry, A. Population-Based, Model to consider the effect of seasonal variation on serum 25(OH)D and Vitamin D status. Biomed. Res. Int 2015, 168189 (2015)
E. Lester, R.K. Skinner, M.R. Wills, Seasonal variation in serum-25-hydroxyvitamin-D in the elderly in Britain. Lancet 1, 979–980 (1977)
M.F. Holick, L.Y. Matsuoka, J. Wortsman, Age, vitamin D, and solar ultraviolet. Lancet 2, 1104–1105 (1989)
A.G. Need, H.A. Morris, M. Horowitz, C. Nordin, Effects of skin thickness, age, body fat, and sunlight on serum 25-hydroxyvitamin D. Am. J. Clin. Nutr. 58, 882–885 (1993)
D. Corless, S.P. Gupta, D.A. Sattar, S. Switala, B.J. Boucher, Vitamin D status of residents of an old people’s home and long-stay patients. Gerontology 25, 350–355 (1979)
K. Guggenheim, M. Kravitz, R. Tal, N.A. Kaufmann, Biochemical parameters of vitamin D nutriture in old people in Jerusalem. Nutr. Metab. 23, 172–178 (1979)
G. Toss, S. Almqvist, L. Larsson, H. Zetterqvist, Vitamin D deficiency in welfare institutions for the aged. Acta Med. Scand 208, 87–89 (1980)
V. Carnevale, S. Modoni, M. Pileri et al., Longitudinal evaluation of vitamin D status in healthy subjects from southern Italy: seasonal and gender differences. Osteoporos. Int. 12, 1026–1030 (2001)
M.J. Bolland, A. Grey, G.D. Gamble, I.R. Reid, The effect of vitamin D supplementation on skeletal, vascular, or cancer outcomes: a trial sequential meta-analysis. Lancet Diabetes Endocrinol 2, 307–320 (2014)
A. Cranney, T. Horsley, S. O’Donnell, H.A. Weiler et al., Effectiveness and safety of vitamin D in Relation to bone health. Evidence report/technology assessment No. 158 (Prepared by the University of Ottawa evidence-based practice center (UO-EPC) under contract no. 290-02-0021. AHRQ Publication No. 07-E013. Rockville, MD: Agency for Healthcare Research and Quality (2007)
R.D. Jackson, A.Z. LaCroix, M. Gass et al., Calcium plus vitamin D supplementation and the risk of fractures. N. Engl. J. Med. 354, 669–683 (2006)
S.D. Anker, S. von Haehling, Vitamin D in chronic kidney disease: more questions than answers. JAMA 307, 722–723 (2012)
S.C. Palmer, D.O. McGregor, P. Macaskill et al., Meta-analysis: vitamin D compounds in chronic kidney disease. Ann. Intern. Med. 147, 840–853 (2007)
G.D. Carter, R. Carter, J. Jones, J. Berry, How accurate are assays for 25-hydroxyvitamin D? Data from the international vitamin D external quality assessment scheme. Clin. Chem. 50, 2195–2197 (2004)
Gel-H. Fuleihan, R. Bouillon, B. Clarke et al., Serum 25-Hydroxyvitamin D levels: variability, knowledge gaps, and the concept of a desirable range. J. Bone Miner. Res. 30, 1119–33 (2015)
Vitamin D External Quality Assessment Scheme (DEQAS) http://www.deqas.org/. Accessed 12 Dec 2016
G. Snellman, H. Melhus, R. Gedeborg et al., Determining vitamin D status: a comparison between commercially available assays. PLoS. One 5(7), e11555 (2010)
Acknowledgments
We are indebted to all the study participants and to the dedicated personnel of both the study center of the HNR study and the EBT-scanner facilities Prof. D. Grönemeyer, Bochum and Dr. R. Seibel, Mülheim as well as to the investigative group, in particular to U. Roggenbuck, U. Slomiany, E.M. Beck, A. Öffner, S. Münkel, M. Bauer, S. Schrader, R. Peter, and H. Hirche. We acknowledge the support of the SarstedtAG&Co. (Nümbrecht, Germany) concerning laboratory equipment. We thank Prof. K. Lauterbach (Adjunct Prof., Harvard School of Public Health, Boston, USA) for his valuable contributions in an earlier phase of the study. We thank the Heinz Nixdorf Foundation [Chairman: Martin Nixdorf; Past Chairman: Dr Jur Gerhard Schmidt (deceased)], for their generous support of this study. This study is also supported by the German Federal Ministry of Education and Research (BMBF) that transferred the monitoring of the study Deutsches Zentrum für Luft- und Raumfahrt (DLR), Bonn, Germany. An international advisory board and quality control as well as event committee were established, but had no role concerning the study design, data collection, analysis, interpretation, or writing the report. The Deutsche Forschungsgemeinschaft (DFG) supported the study (DFG project: ER 155/6-1 and ER 155/6-2). This study is also supported by the Kulturstiftung Essen.
Author Contributions
S.H.S.: analysis and interpretation of data, drafting the manuscript. K.H.J. and R.E.: study concept and design. H.L., K.H.J., R.E., D.F., S.M.: assisted with drafting the manuscript for intellectual content. All authors read and approved the final manuscript.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
The study was approved by the institutional ethics committee.
Informed consent
All participants provided written informed consent.
Rights and permissions
About this article
Cite this article
Schramm, S., Lahner, H., Jöckel, KH. et al. Impact of season and different vitamin D thresholds on prevalence of vitamin D deficiency in epidemiological cohorts—a note of caution. Endocrine 56, 658–666 (2017). https://doi.org/10.1007/s12020-017-1292-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-017-1292-7