Abstract
Dental mesenchymal stem cells (MSCs) are characterized by unlimited self-renewal ability and high multidirectional differentiation potential. Since dental MSCs can be easily isolated and exhibit a high capability to differentiate into odontogenic cells, they are considered as attractive therapeutic agents in regenerative dentistry. Recently, MSC-derived extracellular vesicles (MSC-EVs) have attracted widespread attention as carriers for cell-free therapy due to their potential functions. Many studies have shown that MSC-EVs can mediate microenvironment at tissue damage site, and coordinate the regeneration process. Additionally, MSC-EVs can mediate intercellular communication, thus affecting the phenotypes and functions of recipient cells. In this review, we mainly summarized the types of MSCs that could be potentially applied in regenerative dentistry, the possible molecular cargos of MSC-EVs, and the major effects of MSC-EVs on the therapeutic induction of osteogenic differentiation.
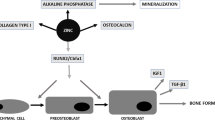
Graphical abstract


Similar content being viewed by others
Data availability
Not applicable.
References
Tatullo, M., Marrelli, M., & Paduano, F. (2015). The regenerative medicine in oral and maxillofacial surgery: The most important innovations in the clinical application of mesenchymal stem cells. International Journal of Medical Sciences, 12(1), 72–77.
Mao, A. S., & Mooney, D. J. (2015). Regenerative medicine: Current therapies and future directions. Proc Natl Acad Sci U S A, 112(47), 14452–14459.
Wu, V., et al. (2019). Bone Tissue Regeneration in the Oral and Maxillofacial Region: A Review on the Application of Stem Cells and New Strategies to Improve Vascularization. Stem Cells Int, 2019, 6279721.
Amrollahi, P., et al. (2016). Recent advancements in regenerative dentistry: A review. Materials Science & Engineering, C: Materials for Biological Applications, 69, 1383–1390.
Oldershaw, R. A. (2012). Cell sources for the regeneration of articular cartilage: The past, the horizon and the future. International Journal of Experimental Pathology, 93(6), 389–400.
Weatherholt, A.M., R.K. Fuchs, and S.J. Warden, Specialized connective tissue: bone, the structural framework of the upper extremity. J Hand Ther, 2012. 25(2): p. 123–31; quiz 132.
Chamberlain, G., et al. (2007). Concise review: Mesenchymal stem cells: Their phenotype, differentiation capacity, immunological features, and potential for homing. Stem Cells, 25(11), 2739–2749.
Chang, J., et al. (2009). Inhibition of osteoblastic bone formation by nuclear factor-kappaB. Nature Medicine, 15(6), 682–689.
Moerman, E. J., et al. (2004). Aging activates adipogenic and suppresses osteogenic programs in mesenchymal marrow stroma/stem cells: The role of PPAR-gamma2 transcription factor and TGF-beta/BMP signaling pathways. Aging Cell, 3(6), 379–389.
Yuan, Z., et al. (2016). PPARgamma and Wnt Signaling in Adipogenic and Osteogenic Differentiation of Mesenchymal Stem Cells. Current Stem Cell Research & Therapy, 11(3), 216–225.
Liu, S., et al. (2015). MSC Transplantation Improves Osteopenia via Epigenetic Regulation of Notch Signaling in Lupus. Cell Metabolism, 22(4), 606–618.
Wu, Q., et al. (2018). Therapeutic antibody directed osteogenic differentiation of induced pluripotent stem cell derived MSCs. Acta Biomaterialia, 74, 222–235.
Um, S., Lee, J. H., & Seo, B. M. (2018). TGF-beta2 downregulates osteogenesis under inflammatory conditions in dental follicle stem cells. International Journal of Oral Science, 10(3), 29.
Wang, S., et al. (2012). Insulin-like growth factor 1 can promote the osteogenic differentiation and osteogenesis of stem cells from apical papilla. Stem Cell Res, 8(3), 346–356.
Li, B., et al. (2012). Basic fibroblast growth factor inhibits osteogenic differentiation of stem cells from human exfoliated deciduous teeth through ERK signaling. Oral Diseases, 18(3), 285–292.
Kinane, D. F., Stathopoulou, P. G., & Papapanou, P. N. (2017). Periodontal diseases. Nat Rev Dis Primers, 3, 17038.
Liu, Y., et al. (2011). MiR-17 modulates osteogenic differentiation through a coherent feed-forward loop in mesenchymal stem cells isolated from periodontal ligaments of patients with periodontitis. Stem Cells, 29(11), 1804–1816.
Li, H., et al. (2019). Immunomodulatory Functions of Mesenchymal Stem Cells in Tissue Engineering. Stem Cells Int, 2019, 9671206.
Andrukhov, O., et al. (2019). Immunomodulatory properties of dental tissue-derived mesenchymal stem cells: Implication in disease and tissue regeneration. World J Stem Cells, 11(9), 604–617.
Toh, W. S., et al. (2014). Advances in mesenchymal stem cell-based strategies for cartilage repair and regeneration. Stem Cell Rev Rep, 10(5), 686–696.
Bagno, L., et al. (2018). Mesenchymal Stem Cell-Based Therapy for Cardiovascular Disease: Progress and Challenges. Molecular Therapy, 26(7), 1610–1623.
Han, C., et al. (2016). Exosomes and Their Therapeutic Potentials of Stem Cells. Stem Cells Int, 2016, 7653489.
Huang, C. C., et al. (2020). Evaluating the Endocytosis and Lineage-Specification Properties of Mesenchymal Stem Cell Derived Extracellular Vesicles for Targeted Therapeutic Applications. Frontiers in Pharmacology, 11, 163.
Lai, R. C., et al. (2010). Exosome secreted by MSC reduces myocardial ischemia/reperfusion injury. Stem Cell Res, 4(3), 214–222.
Valadi, H., et al. (2007). Exosome-mediated transfer of mRNAs and microRNAs is a novel mechanism of genetic exchange between cells. Nature Cell Biology, 9(6), 654–659.
Konala, V. B., et al. (2016). The current landscape of the mesenchymal stromal cell secretome: A new paradigm for cell-free regeneration. Cytotherapy, 18(1), 13–24.
Pomatto, M., et al., Differential Therapeutic Effect of Extracellular Vesicles Derived by Bone Marrow and Adipose Mesenchymal Stem Cells on Wound Healing of Diabetic Ulcers and Correlation to Their Cargoes. Int J Mol Sci, 2021. 22(8).
Tuz, H. H., et al. (2019). Reconstruction and Implant-Supported Rehabilitation of an Iatrogenically Caused Maxillary Alveolar Defect. Implant Dentistry, 28(5), 510–513.
Dimitriou, R., et al. (2011). Bone regeneration: Current concepts and future directions. BMC Medicine, 9, 66.
Stern, A., & Barzani, G. (2015). Autogenous bone harvest for implant reconstruction. Dental Clinics of North America, 59(2), 409–420.
Khojasteh, A., et al. (2017). Guided Bone Regeneration for the Reconstruction of Alveolar Bone Defects. Ann Maxillofac Surg, 7(2), 263–277.
Stegen, S., van Gastel, N., & Carmeliet, G. (2015). Bringing new life to damaged bone: The importance of angiogenesis in bone repair and regeneration. Bone, 70, 19–27.
Hughes, F. J., et al. (2000). Effects of growth factors and cytokines on osteoblast differentiation. Periodontology, 2006(41), 48–72.
Panetta, N. J., Gupta, D. M., & Longaker, M. T. (2010). Bone regeneration and repair. Current Stem Cell Research & Therapy, 5(2), 122–128.
Del Fattore, A., et al. (2014). An experimental therapy to improve skeletal growth and prevent bone loss in a mouse model overexpressing IL-6. Osteoporosis International, 25(2), 681–692.
Rao, S. S., et al. (2018). Omentin-1 prevents inflammation-induced osteoporosis by downregulating the pro-inflammatory cytokines. Bone Res, 6, 9.
Fliefel, R., et al. (2016). Mesenchymal stem cell proliferation and mineralization but not osteogenic differentiation are strongly affected by extracellular pH. Journal of Cranio-Maxillo-Facial Surgery, 44(6), 715–724.
Hu, L., et al., Mesenchymal Stem Cells: Cell Fate Decision to Osteoblast or Adipocyte and Application in Osteoporosis Treatment. Int J Mol Sci, 2018. 19(2).
Botelho, J., et al. (2017). Dental stem cells: Recent progresses in tissue engineering and regenerative medicine. Annals of Medicine, 49(8), 644–651.
Kumar, A., et al. (2017). Secretome Cues Modulate the Neurogenic Potential of Bone Marrow and Dental Stem Cells. Molecular Neurobiology, 54(6), 4672–4682.
Fujii, Y., et al. (2018). Bone regeneration by human dental pulp stem cells using a helioxanthin derivative and cell-sheet technology. Stem Cell Research & Therapy, 9(1), 24.
Bakopoulou, A., & About, I. (2016). Stem Cells of Dental Origin: Current Research Trends and Key Milestones towards Clinical Application. Stem Cells Int, 2016, 4209891.
Chalisserry, E. P., et al. (2017). Therapeutic potential of dental stem cells. J Tissue Eng, 8, 2041731417702531.
Huang, G.T., S. Gronthos, and S. Shi, (2009). Mesenchymal stem cells derived from dental tissues vs. those from other sources: their biology and role in regenerative medicine. J Dent Res, 88(9):792–806.
Peng, L., Ye, L., & Zhou, X. D. (2009). Mesenchymal stem cells and tooth engineering. International Journal of Oral Science, 1(1), 6–12.
Hu, L., Liu, Y., & Wang, S. (2018). Stem cell-based tooth and periodontal regeneration. Oral Diseases, 24(5), 696–705.
Aydin, S., & Sahin, F. (2019). Stem Cells Derived from Dental Tissues. Advances in Experimental Medicine and Biology, 1144, 123–132.
Gronthos, S., et al. (2000). Postnatal human dental pulp stem cells (DPSCs) in vitro and in vivo. Proc Natl Acad Sci U S A, 97(25), 13625–13630.
Gronthos, S., et al. (2002). Stem cell properties of human dental pulp stem cells. Journal of Dental Research, 81(8), 531–535.
Pisciotta, A., et al. (2015). Human dental pulp stem cells (hDPSCs): Isolation, enrichment and comparative differentiation of two sub-populations. BMC Developmental Biology, 15, 14.
Gopinath, V. K., Soumya, S., & Jayakumar, M. N. (2020). Osteogenic and odontogenic differentiation potential of dental pulp stem cells isolated from inflamed dental pulp tissues (I-DPSCs) by two different methods. Acta Odontologica Scandinavica, 78(4), 281–289.
Hossein-Khannazer, N., et al. (2019). Study of the immunomodulatory effects of osteogenic differentiated human dental pulp stem cells. Life Sciences, 216, 111–118.
Tomasello, L., et al. (2017). Mesenchymal stem cells derived from inflamed dental pulpal and gingival tissue: A potential application for bone formation. Stem Cell Research & Therapy, 8(1), 179.
Qin, Z., et al. (2015). High dose of TNF-alpha suppressed osteogenic differentiation of human dental pulp stem cells by activating the Wnt/beta-catenin signaling. Journal of Molecular Histology, 46(4–5), 409–420.
Feng, G., et al. (2016). SIRT1 was involved in TNF-alpha-promoted osteogenic differentiation of human DPSCs through Wnt/beta-catenin signal. In Vitro Cellular and Developmental Biology. Animal, 52(10), 1001–1011.
Cui, Y. M., et al. (2017). TNF-alpha was involved in calcium hydroxide-promoted osteogenic differentiation of human DPSCs through NF-kappaB/p38MAPK/Wnt pathway. Die Pharmazie, 72(6), 329–333.
Chen, L., et al. (2016). Calcium Hydroxide-induced Proliferation, Migration, Osteogenic Differentiation, and Mineralization via the Mitogen-activated Protein Kinase Pathway in Human Dental Pulp Stem Cells. Journal of Endodontia, 42(9), 1355–1361.
Winning, L., El Karim, I. A., & Lundy, F. T. (2019). A Comparative Analysis of the Osteogenic Potential of Dental Mesenchymal Stem Cells. Stem Cells Dev, 28(15), 1050–1058.
Wang, H., et al. (2018). Comparative characterization of SHED and DPSCs during extended cultivation in vitro. Molecular Medicine Reports, 17(5), 6551–6559.
Jin, Q., et al. (2019). Comparative characterization of mesenchymal stem cells from human dental pulp and adipose tissue for bone regeneration potential. Artif Cells Nanomed Biotechnol, 47(1), 1577–1584.
Jarmalaviciute, A., et al. (2015). Exosomes from dental pulp stem cells rescue human dopaminergic neurons from 6-hydroxy-dopamine-induced apoptosis. Cytotherapy, 17(7), 932–939.
Shen, Z., et al. (2020). Chitosan hydrogel incorporated with dental pulp stem cell-derived exosomes alleviates periodontitis in mice via a macrophage-dependent mechanism. Bioact Mater, 5(4), 1113–1126.
Ji, L., et al. (2019). Comparison of immunomodulatory properties of exosomes derived from bone marrow mesenchymal stem cells and dental pulp stem cells. Immunologic Research, 67(4–5), 432–442.
Miura, M., et al. (2003). SHED: Stem cells from human exfoliated deciduous teeth. Proc Natl Acad Sci U S A, 100(10), 5807–5812.
Kashyap, R., SHED - Basic Structure for Stem Cell Research. J Clin Diagn Res, 2015. 9(3): p. ZE07–9.
Brar, G. S., & Toor, R. S. (2012). Dental stem cells: Dentinogenic, osteogenic, and neurogenic differentiation and its clinical cell based therapies. Indian Journal of Dental Research, 23(3), 393–397.
Zhang, N., et al. (2016). Isolation, characterization and multi-lineage differentiation of stem cells from human exfoliated deciduous teeth. Molecular Medicine Reports, 14(1), 95–102.
Yamaza, T., et al. (2010). Immunomodulatory properties of stem cells from human exfoliated deciduous teeth. Stem Cell Research & Therapy, 1(1), 5.
Junior, A. L., et al. (2020). Mesenchymal Stem Cells from Human Exfoliated Deciduous Teeth and the Orbicularis Oris Muscle: How Do They Behave When Exposed to a Proinflammatory Stimulus? Stem Cells Int, 2020, 3670412.
Zhai, Y., et al. (2019). Activation and Biological Properties of Human beta Defensin 4 in Stem Cells Derived From Human Exfoliated Deciduous Teeth. Frontiers in Physiology, 10, 1304.
Sebastian, A. A., et al. (2018). Interleukin-17A promotes osteogenic differentiation by increasing OPG/RANKL ratio in stem cells from human exfoliated deciduous teeth (SHED). Journal of Tissue Engineering and Regenerative Medicine, 12(8), 1856–1866.
Novais, A., et al. (2019). Priming Dental Pulp Stem Cells from Human Exfoliated Deciduous Teeth with Fibroblast Growth Factor-2 Enhances Mineralization Within Tissue-Engineered Constructs Implanted in Craniofacial Bone Defects. Stem Cells Translational Medicine, 8(8), 844–857.
Ishiy, F. A. A., et al. (2018). CD105 is regulated by hsa-miR-1287 and its expression is inversely correlated with osteopotential in SHED. Bone, 106, 112–120.
Sonoyama, W., et al. (2008). Characterization of the apical papilla and its residing stem cells from human immature permanent teeth: A pilot study. Journal of Endodontia, 34(2), 166–171.
Li, W., et al. (2018). Depletion of HOXA5 inhibits the osteogenic differentiation and proliferation potential of stem cells from the apical papilla. Cell Biology International, 42(1), 45–52.
Gao, R. T., et al. (2015). Homeobox B7 promotes the osteogenic differentiation potential of mesenchymal stem cells by activating RUNX2 and transcript of BSP. International Journal of Clinical and Experimental Medicine, 8(7), 10459–10470.
Li, G., et al. (2018). Homeobox C10 inhibits the osteogenic differentiation potential of mesenchymal stem cells. Connective Tissue Research, 59(3), 201–211.
Zhou, M., et al. (2017). Blockade of LGR4 inhibits proliferation and odonto/osteogenic differentiation of stem cells from apical papillae. Journal of Molecular Histology, 48(5–6), 389–401.
He, W., et al. (2014). Regulatory interplay between NFIC and TGF-beta1 in apical papilla-derived stem cells. Journal of Dental Research, 93(5), 496–501.
Liu, C., et al. (2016). Long-term exposure to pro-inflammatory cytokines inhibits the osteogenic/dentinogenic differentiation of stem cells from the apical papilla. International Endodontic Journal, 49(10), 950–959.
Seo, B. M., et al. (2004). Investigation of multipotent postnatal stem cells from human periodontal ligament. Lancet, 364(9429), 149–155.
Abedian, Z., et al. (2020). A comparative study on immunophenotypic characterization and osteogenic differentiation of human mesenchymal stromal cells derived from periodontal ligament and gingiva. Journal of Periodontology, 91(9), 1194–1202.
Ai, T., et al. (2018). DNA methylation profile is associated with the osteogenic potential of three distinct human odontogenic stem cells. Signal Transduction and Targeted Therapy, 3, 1.
Xia, Y., et al. (2016). Cell Responses to Conditioned Media Produced by Patient-Matched Stem Cells Derived From Healthy and Inflamed Periodontal Ligament Tissues. Journal of Periodontology, 87(5), e53-63.
Tang, H. N., et al. (2016). Stem cells derived from “inflamed” and healthy periodontal ligament tissues and their sheet functionalities: A patient-matched comparison. Journal of Clinical Periodontology, 43(1), 72–84.
Kato, H., et al. (2014). Porphyromonas gingivalis LPS inhibits osteoblastic differentiation and promotes pro-inflammatory cytokine production in human periodontal ligament stem cells. Archives of Oral Biology, 59(2), 167–175.
Li, C., et al. (2014). Lipopolysaccharide differentially affects the osteogenic differentiation of periodontal ligament stem cells and bone marrow mesenchymal stem cells through Toll-like receptor 4 mediated nuclear factor kappaB pathway. Stem Cell Research & Therapy, 5(3), 67.
Albiero, M.L., et al., Osteogenic potential of periodontal ligament stem cells are unaffected after exposure to lipopolysaccharides. Braz Oral Res, 2017. 31: p. e17.
Liu, H., et al., Exendin-4 regulates Wnt and NF-kappaB signaling in lipopolysaccharide-induced human periodontal ligament stem cells to promote osteogenic differentiation. Int Immunopharmacol, 2019. 75: p. 105801.
Mao, C.Y., et al., Double-edged-sword effect of IL-1beta on the osteogenesis of periodontal ligament stem cells via crosstalk between the NF-kappaB, MAPK and BMP/Smad signaling pathways. Cell Death Dis, 2016. 7: p. e2296.
Zhang, K., et al. (2019). Autophagy preserves the osteogenic ability of periodontal ligament stem cells under high glucose conditions in rats. Archives of Oral Biology, 101, 172–179.
Kato, H., et al. (2016). High Glucose Concentrations Suppress the Proliferation of Human Periodontal Ligament Stem Cells and Their Differentiation Into Osteoblasts. Journal of Periodontology, 87(4), e44-51.
Di Vito, A., et al. (2019). In Vitro Long-Term Expansion and High Osteogenic Potential of Periodontal Ligament Stem Cells: More Than a Mirage. Cell Transplantation, 28(1), 129–139.
Yang, S., et al. (2018). Nitric oxide balances osteoblast and adipocyte lineage differentiation via the JNK/MAPK signaling pathway in periodontal ligament stem cells. Stem Cell Research & Therapy, 9(1), 118.
Li, M., et al. (2017). Effect of cryopreservation on proliferation and differentiation of periodontal ligament stem cell sheets. Stem Cell Research & Therapy, 8(1), 77.
Zhang, J., et al. (2019). Dental Follicle Stem Cells: Tissue Engineering and Immunomodulation. Stem Cells Dev, 28(15), 986–994.
Shoi, K., et al. (2014). Characterization of pulp and follicle stem cells from impacted supernumerary maxillary incisors. Pediatric Dentistry, 36(3), 79–84.
Mori, G., et al. (2012). Osteogenic differentiation of dental follicle stem cells. International Journal of Medical Sciences, 9(6), 480–487.
Yao, S., et al. (2013). Expression of bone morphogenetic protein-6 in dental follicle stem cells and its effect on osteogenic differentiation. Cells, Tissues, Organs, 198(6), 438–447.
Rezai Rad, M., et al. (2015). The role of dentin matrix protein 1 (DMP1) in regulation of osteogenic differentiation of rat dental follicle stem cells (DFSCs). Archives of Oral Biology, 60(4), 546–556.
Yao, S., et al. (2017). Expression of odontogenic ameloblast-associated protein in the dental follicle and its role in osteogenic differentiation of dental follicle stem cells. Archives of Oral Biology, 78, 6–12.
Chen, C., et al. (2018). Nkd2 promotes the differentiation of dental follicle stem/progenitor cells into osteoblasts. International Journal of Molecular Medicine, 42(5), 2403–2414.
Rezai-Rad, M., et al. (2015). Evaluation of bone regeneration potential of dental follicle stem cells for treatment of craniofacial defects. Cytotherapy, 17(11), 1572–1581.
Rezai Rad, M., et al. (2013). Activation of proliferation and differentiation of dental follicle stem cells (DFSCs) by heat stress. Cell Proliferation, 46(1), 58–66.
Raposo, G., & Stoorvogel, W. (2013). Extracellular vesicles: Exosomes, microvesicles, and friends. Journal of Cell Biology, 200(4), 373–383.
Harding, C., Heuser, J., & Stahl, P. (1983). Receptor-mediated endocytosis of transferrin and recycling of the transferrin receptor in rat reticulocytes. Journal of Cell Biology, 97(2), 329–339.
Johnstone, R.M., et al. (1987). Vesicle formation during reticulocyte maturation. Association of plasma membrane activities with released vesicles (exosomes). J Biol Chem, 262(19): 9412–9420.
Thery, C., et al. (2018). Minimal information for studies of extracellular vesicles 2018 (MISEV2018): A position statement of the International Society for Extracellular Vesicles and update of the MISEV2014 guidelines. J Extracell Vesicles, 7(1), 1535750.
Stoorvogel, W., et al. (2002). The biogenesis and functions of exosomes. Traffic, 3(5), 321–330.
Thery, C., Zitvogel, L., & Amigorena, S. (2002). Exosomes: Composition, biogenesis and function. Nature Reviews Immunology, 2(8), 569–579.
Ludwig, A. K., & Giebel, B. (2012). Exosomes: Small vesicles participating in intercellular communication. International Journal of Biochemistry & Cell Biology, 44(1), 11–15.
Simons, M., & Raposo, G. (2009). Exosomes–vesicular carriers for intercellular communication. Current Opinion in Cell Biology, 21(4), 575–581.
Greening, D. W., et al. (2015). A protocol for exosome isolation and characterization: Evaluation of ultracentrifugation, density-gradient separation, and immunoaffinity capture methods. Methods in Molecular Biology, 1295, 179–209.
Flaherty, S. E., 3rd., et al. (2019). A lipase-independent pathway of lipid release and immune modulation by adipocytes. Science, 363(6430), 989–993.
Hannafon, B. N., et al. (2019). Metastasis-associated protein 1 (MTA1) is transferred by exosomes and contributes to the regulation of hypoxia and estrogen signaling in breast cancer cells. Cell Communication and Signaling: CCS, 17(1), 13.
Cabral, J., et al. (2018). Extracellular vesicles as modulators of wound healing. Advanced Drug Delivery Reviews, 129, 394–406.
Riazifar, M., et al. (2019). Stem Cell-Derived Exosomes as Nanotherapeutics for Autoimmune and Neurodegenerative Disorders. ACS Nano, 13(6), 6670–6688.
Chen, B., et al. (2017). Stem Cell-Derived Extracellular Vesicles as a Novel Potential Therapeutic Tool for Tissue Repair. Stem Cells Translational Medicine, 6(9), 1753–1758.
Kaushik, S., & Cuervo, A. M. (2015). Proteostasis and aging. Nature Medicine, 21(12), 1406–1415.
Sato-Kuwabara, Y., et al. (2015). The fusion of two worlds: Non-coding RNAs and extracellular vesicles–diagnostic and therapeutic implications (Review). International Journal of Oncology, 46(1), 17–27.
Narayanan, K., et al. (2018). Lineage-specific exosomes could override extracellular matrix mediated human mesenchymal stem cell differentiation. Biomaterials, 182, 312–322.
Ma, H., et al. (2018). Analysis of differentially expressed microRNA of TNF-alpha-stimulated mesenchymal stem cells and exosomes from their culture supernatant. Archives of Medical Science, 14(5), 1102–1111.
Kharmate, G., et al., Epidermal Growth Factor Receptor in Prostate Cancer Derived Exosomes. PLoS One, 2016. 11(5): p. e0154967.
Han, Y., et al. (2019). Exosomes from hypoxia-treated human adipose-derived mesenchymal stem cells enhance angiogenesis through VEGF/VEGF-R. International Journal of Biochemistry & Cell Biology, 109, 59–68.
Sundaram, K., et al. (2019) Plant-Derived Exosomal Nanoparticles Inhibit Pathogenicity of Porphyromonas gingivalis. iScience, 21: p. 308–327.
Gnecchi, M., et al. (2016). Paracrine Mechanisms of Mesenchymal Stem Cells in Tissue Repair. Methods in Molecular Biology, 1416, 123–146.
Furuta, T., et al. (2016). Mesenchymal Stem Cell-Derived Exosomes Promote Fracture Healing in a Mouse Model. Stem Cells Translational Medicine, 5(12), 1620–1630.
Narayanan, R., Huang, C. C., & Ravindran, S. (2016). Hijacking the Cellular Mail: Exosome Mediated Differentiation of Mesenchymal Stem Cells. Stem Cells Int, 2016, 3808674.
Wang, X., et al. (2018). Mesenchymal stem cell-derived exosomes have altered microRNA profiles and induce osteogenic differentiation depending on the stage of differentiation. PLoS One, 13(2), e0193059.
Chen, S., et al. (2015). Co-culture with periodontal ligament stem cells enhanced osteoblastic differentiation of MC3T3-E1 cells and osteoclastic differentiation of RAW264.7 cells. Int J Clin Exp Pathol, 8(11), 14596–607.
Wang, M., et al. (2020). SHED-derived conditioned exosomes enhance the osteogenic differentiation of PDLSCs via Wnt and BMP signaling in vitro. Differentiation, 111, 1–11.
Ekstrom, K., et al., Monocyte exosomes stimulate the osteogenic gene expression of mesenchymal stem cells. PLoS One, 2013. 8(9): p. e75227.
Zheng, Y., et al. (2019). Exosomal microRNA-155-5p from PDLSCs regulated Th17/Treg balance by targeting sirtuin-1 in chronic periodontitis. Journal of Cellular Physiology, 234(11), 20662–20674.
Thind, A., & Wilson, C. (2016). Exosomal miRNAs as cancer biomarkers and therapeutic targets. J Extracell Vesicles, 5, 31292.
Lai, R. C., Chen, T. S., & Lim, S. K. (2011). Mesenchymal stem cell exosome: A novel stem cell-based therapy for cardiovascular disease. Regenerative Medicine, 6(4), 481–492.
Vishnoi, A., & Rani, S. (2017). MiRNA Biogenesis and Regulation of Diseases: An Overview. Methods in Molecular Biology, 1509, 1–10.
Deng, Y., et al. (2013). Effects of a miR-31, Runx2, and Satb2 regulatory loop on the osteogenic differentiation of bone mesenchymal stem cells. Stem Cells Dev, 22(16), 2278–2286.
Fang, S., et al. (2015). MicroRNAs regulate bone development and regeneration. International Journal of Molecular Sciences, 16(4), 8227–8253.
Xu, J. F., et al. (2014). Altered microRNA expression profile in exosomes during osteogenic differentiation of human bone marrow-derived mesenchymal stem cells. PLoS One, 9(12), e114627.
Gallo, A., et al. (2012). The majority of microRNAs detectable in serum and saliva is concentrated in exosomes. PLoS One, 7(3), e30679.
Lee, M. J., Park, D. H., & Kang, J. H. (2016). Exosomes as the source of biomarkers of metabolic diseases. Ann Pediatr Endocrinol Metab, 21(3), 119–125.
Huang, Y., et al. (2021). miR-19b enhances osteogenic differentiation of mesenchymal stem cells and promotes fracture healing through the WWP1/Smurf2-mediated KLF5/beta-catenin signaling pathway. Experimental & Molecular Medicine, 53(5), 973–985.
Jiang, Y., et al. (2020). Bone Marrow Mesenchymal Stem Cell-Derived Exosomal miR-25 Regulates the Ubiquitination and Degradation of Runx2 by SMURF1 to Promote Fracture Healing in Mice. Front Med (Lausanne), 7, 577578.
Zuo, R., et al. (2019). Exosomes derived from human CD34(+) stem cells transfected with miR-26a prevent glucocorticoid-induced osteonecrosis of the femoral head by promoting angiogenesis and osteogenesis. Stem Cell Research & Therapy, 10(1), 321.
Chen, C., et al. (2017). Mesenchymal stem cell transplantation in tight-skin mice identifies miR-151-5p as a therapeutic target for systemic sclerosis. Cell Research, 27(4), 559–577.
Lv, P. Y., et al. (2020). Osteocyte-derived exosomes induced by mechanical strain promote human periodontal ligament stem cell proliferation and osteogenic differentiation via the miR-181b-5p/PTEN/AKT signaling pathway. Stem Cell Research & Therapy, 11(1), 295.
Du, W., et al. (2019). Exosomes derived from preadipocytes improve osteogenic differentiation, potentially via reduced miR223 expression. Molecular Medicine Reports, 19(2), 951–958.
Chen, S., et al. (2019). Exosomes derived from miR-375-overexpressing human adipose mesenchymal stem cells promote bone regeneration. Cell Prolif, 52(5), e12669.
Hashimoto, K., et al. (2018). Cancer-secreted hsa-miR-940 induces an osteoblastic phenotype in the bone metastatic microenvironment via targeting ARHGAP1 and FAM134A. Proc Natl Acad Sci U S A, 115(9), 2204–2209.
Jiang, L. B., Tian, L., & Zhang, C. G. (2018). Bone marrow stem cells-derived exosomes extracted from osteoporosis patients inhibit osteogenesis via microRNA-21/SMAD7. European Review for Medical and Pharmacological Sciences, 22(19), 6221–6229.
Yang, J. X., et al. (2020). Osteoclast-derived miR-23a-5p-containing exosomes inhibit osteogenic differentiation by regulating Runx2. Cell Signal, 70, 109504.
Zhuang, X.M. and B. Zhou, Exosome secreted by human gingival fibroblasts in radiation therapy inhibits osteogenic differentiation of bone mesenchymal stem cells by transferring miR-23a. Biomed Pharmacother, 2020. 131: p. 110672.
Xu, R., et al. (2018). MicroRNA-31a-5p from aging BMSCs links bone formation and resorption in the aged bone marrow microenvironment. Aging Cell, 17(4), e12794.
Xu, T., et al. (2020). Exosomal miRNA-128-3p from mesenchymal stem cells of aged rats regulates osteogenesis and bone fracture healing by targeting Smad5. J Nanobiotechnology, 18(1), 47.
Yang, S., et al. (2020). Exosomal miR-130a-3p regulates osteogenic differentiation of Human Adipose-Derived stem cells through mediating SIRT7/Wnt/beta-catenin axis. Cell Prolif, 53(10), e12890.
Davis, C., et al. (2017). MicroRNA-183-5p Increases with Age in Bone-Derived Extracellular Vesicles, Suppresses Bone Marrow Stromal (Stem) Cell Proliferation, and Induces Stem Cell Senescence. Tissue Engineering Part A, 23(21–22), 1231–1240.
Cao, F., et al. (2017). miR-214 promotes periodontal ligament stem cell osteoblastic differentiation by modulating Wnt/betacatenin signaling. Molecular Medicine Reports, 16(6), 9301–9308.
Li, K. C., et al. (2017). Baculovirus-Mediated miR-214 Knockdown Shifts Osteoporotic ASCs Differentiation and Improves Osteoporotic Bone Defects Repair. Science and Reports, 7(1), 16225.
Sun, Q., et al. (2013). Expression and significance of miRNA-21 and BTG2 in lung cancer. Tumour Biology, 34(6), 4017–4026.
Funding
This work was supported by Guangdong Basic and Applied Basic Research Foundation (General Program: 2020A1515010237); Shenzhen Key Medical Discipline Construction Fund (No.SZXK039); and Special Fund for Science and Technology Development of Longgang District, Shenzhen (LGKCYLWS2021000031).
Author information
Authors and Affiliations
Contributions
Haiying Kong and Peiqi Liu finished the writing-original draft; Hongwen Li, Xiantao Zeng, Peiwu Xu, Xinhui Yao and Senqing Liu were involved in investigation and validation; Chak Kwong Cheng did conceptualization and editing; Jian Xu performed supervision and funding acquisition.
Corresponding authors
Ethics declarations
Ethical Approval
Not applicable.
Consent to Participate
Not applicable.
Consent to Publish
The authors are alone responsible for the content and writing of the paper. All authors reviewed and approved the final version of the manuscript.
Competing Interests
The authors declare that they have no conflict interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kong, H., Liu, P., Li, H. et al. Mesenchymal Stem Cell-Derived Extracellular Vesicles: The Novel Therapeutic Option for Regenerative Dentistry. Stem Cell Rev and Rep 19, 46–58 (2023). https://doi.org/10.1007/s12015-022-10342-y
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12015-022-10342-y