Abstract
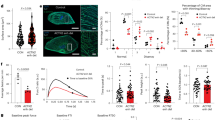
Yohimbine is a highly selective and potent α2-adrenoceptor antagonist, which is usually treated as an adjunction for impotence, as well for weight loss and natural bodybuilding aids. However, it was recently reported that Yohimbine causes myocardial injury and controversial results were reported in the setting of cardiac diseases. Here, we used human-induced pluripotent stem cell-derived cardiomyocytes (hiPSC-CMs) as a model system to explore electrophysiologic characterization after exposure to Yohimbine. HiPSC-CMs were differentiated by employment of inhibitory Wnt compounds. For analysis of electrophysiological properties, conventional whole-cell patch-clamp recording was used. Specifically, spontaneous action potentials, pacemaker currents (If), sodium (Na+) channel (INa), and calcium (Ca++) channel currents (ICa) were assessed in hiPSC-CMs after exposure to Yohimbine. HiPSC-CMs expressed sarcomeric-α-actinin and MLC2V proteins, as well as exhibited ventricular-like spontaneous action potential waveform. Yohimbine inhibited frequency of hiPSC-CMs spontaneous action potentials and significantly prolonged action potential duration in a dose-dependent manner. In addition, rest potential, threshold potential, amplitude, and maximal diastolic potential were decreased, whereas APD50/APD90 was prolonged. Yohimbine inhibited the amplitude of INa in low doses (IC50 = 14.2 μM, n = 5) and inhibited ICa in high doses (IC50 = 139.7 μM, n = 5). Whereas Yohimbine did not affect the activation curves, treatment resulted in left shifts in inactivation curves of both Na+ and Ca++ channels. Here, we show that Yohimbine induces direct cardiotoxic effects on spontaneous action potentials of INa and ICa in hiPSC-CMs. Importantly, these effects were not mediated by α2-adrenoceptor signaling. Our results strongly suggest that Yohimbine directly and negatively affects electrophysiological properties of human cardiomyocytes. These findings are highly relevant for potential application of Yohimbine in patients with atrioventricular conduction disorder.





Similar content being viewed by others
Availability of Data and Materials
The data generated from this study are available from the corresponding author upon reasonable request.
References
Anversa, P., Kajstura, J., Rota, M., et al. (2013). Regenerating new heart with stem cells. The Journal of Clinical Investigation, 123, 62–70.
Joggerst, S. J., & Hatzopoulos, A. K. (2009). Stem cell therapy for cardiac repair: benefits and barriers. Expert Reviews in Molecular Medicine, 11, e20.
Magdy, T., Schuldt, A. J. T., Wu, J. C., et al. (2018). Human induced pluripotent stem cell (hiPSC)-derived cells to assess drug cardiotoxicity: Opportunities and problems. Annual Review of Pharmacology and Toxicology, 58, 83–103.
Burridge, P. W., Li, Y. F., Matsa, E., et al. (2016). Human induced pluripotent stem cell–derived cardiomyocytes recapitulate the predilection of breast cancer patients to doxorubicin-induced cardiotoxicity. Nature Medicine, 22, 547–556.
Sharma, A., Burridge, P. W., McKeithan, W. L., et al. (2017). High-throughput screening of tyrosine kinase inhibitor cardiotoxicity with human induced pluripotent stem cells. Science Translational Medicine. https://doi.org/10.1126/scitranslmed.aaf2584
Sharma, A., McKeithan, W. L., Serrano, R., et al. (2018). Use of human induced pluripotent stem cell-derived cardiomyocytes to assess drug cardiotoxicity. Nature Protocols, 13, 3018–3041.
McKeithan, W. L., Feyen, D. A. M., Bruyneel, A. A. N., et al. (2020). Reengineering an antiarrhythmic drug using patient hiPSC cardiomyocytes to improve therapeutic potential and reduce toxicity. Cell Stem Cell, 27, 813–21.e6.
Yang, L., Gong, Y., Tan, Y., et al. (2021). Dexmedetomidine exhibits antiarrhythmic effects on human-induced pluripotent stem cell-derived cardiomyocytes through a Na/Ca channel-mediated mechanism. Ann Transl Med, 9, 399.
Stoelzle, S., Haythornthwaite, A., Kettenhofen, R., et al. (2011). Automated patch clamp on mESC-derived cardiomyocytes for cardiotoxicity prediction. Journal of Biomolecular Screening, 16, 910–916.
Scheel, O., Frech, S., Amuzescu, B., et al. (2014). Action potential characterization of human induced pluripotent stem cell-derived cardiomyocytes using automated patch-clamp technology. ASSAY and Drug Development Technologies, 12, 457–469.
Richardson, E. S., & Xiao, Y.-F., et al. (2010). Electrophysiology of single cardiomyocytes: Patch clamp and other recording Methods. In D. C. Sigg, P. A. Iaizzo, & Y.-F. Xiao (Eds.), Cardiac Electrophysiology methods and models (pp. 329–348). Springer, US.
Liu, J., Laksman, Z., & Backx, P. H. (2016). The electrophysiological development of cardiomyocytes. Advanced Drug Delivery Reviews, 96, 253–273.
Goldberg, M. R., & Robertson, D. (1983). Yohimbine: A pharmacological probe for study of the alpha 2-adrenoreceptor. Pharmacological Reviews, 35, 143–180.
Ho, C. C. K., & Tan, H. M. (2011). Rise of herbal and traditional medicine in erectile dysfunction management. Current Urology Reports, 12, 470–478.
Tam, S. W., Worcel, M., & Wyllie, M. (2001). Yohimbine: A clinical review. Pharmacology & Therapeutics, 91, 215–243.
McCarty, M. F. (2002). Pre-exercise administration of Yohimbine may enhance the efficacy of exercise training as a fat loss strategy by boosting lipolysis. Medical Hypotheses, 58, 491–495.
Ostojic, S. M. (2006). Yohimbine: The effects on body composition and exercise performance in soccer players. Research in Sports Medicine, 14, 289–299.
Peskind, E. R., Wingerson, D., Murray, S., et al. (1995). Effects of Alzheimer’s disease and normal aging on cerebrospinal fluid norepinephrine responses to Yohimbine and Clonidine. Archives of General Psychiatry, 52, 774–782.
Petrie, E. C., Peskind, E. R., Dobie, D. J., et al. (2000). Increased plasma norepinephrine response to Yohimbine in elderly men. The Journals of Gerontology: Series A, 55, M155–M159.
Friesen, K., Palatnick, W., & Tenenbein, M. (1993). Benign course after massive ingestion of yohimbine. The Journal of Emergency Medicine, 11, 287–288.
Linden, C. H., Vellman, W. P., & Rumack, B. (1985). Yohimbine: A new street drug. Annals of Emergency Medicine, 14, 1002–1004.
Song, J., & Sharman, T. (2019). Yohimbine induced type II myocardial injury: An underrecognized and dangerous adverse effect. American Journal of Medical Case Reports, 7, 271–273.
Giampreti, A., Lonati, D., Locatelli, C., et al. (2009). Acute neurotoxicity after yohimbine ingestion by a body builder. Clinical Toxicology, 47, 827–829.
Drevin, G., Palayer, M., Compagnon, P., et al. (2020). A fatal case report of acute yohimbine intoxication. Forensic Toxicology, 38, 287–291.
Gu, H., Huang, X., Xu, J., et al. (2018). Optimizing the method for generation of integration-free induced pluripotent stem cells from human peripheral blood. Stem Cell Research & Therapy, 9, 163.
Lian, X., Zhang, J., Azarin, S. M., et al. (2013). Directed cardiomyocyte differentiation from human pluripotent stem cells by modulating Wnt/β-catenin signaling under fully defined conditions. Nature Protocols, 8, 162–175.
Burridge, P. W., Matsa, E., Shukla, P., et al. (2014). Chemically defined generation of human cardiomyocytes. Nature Methods, 11, 855–860.
Yang, X., Pabon, L., & Murry, C. E. (2014). Engineering adolescence. Circulation Research, 114, 511–523.
Denning, C., Borgdorff, V., Crutchley, J., et al. (2016). Cardiomyocytes from human pluripotent stem cells: From laboratory curiosity to industrial biomedical platform. Biochimica et Biophysica Acta (BBA)—Molecular Cell Research, 1863, 1728–48.
Bedada, F. B., Wheelwright, M., & Metzger, J. M. (2016). Maturation status of sarcomere structure and function in human iPSC-derived cardiac myocytes. Biochimica et Biophysica Acta (BBA)—Molecular Cell Research, 1863, 1829–38.
Gong, Y., Chen, Z., Yang, L., et al. (2020). Intrinsic color sensing system allows for real-time observable functional changes on human induced pluripotent stem cell-derived cardiomyocytes. ACS Nano, 14, 8232–8246.
Zhao, Z., Lan, H., El-Battrawy, I., et al. (2018). Ion channel expression and characterization in human induced pluripotent stem cell-derived cardiomyocytes. Stem Cells International, 2018, 6067096.
Paci, M., Hyttinen, J., Rodriguez, B., et al. (2015). Human induced pluripotent stem cell-derived versus adult cardiomyocytes: An in silico electrophysiological study on effects of ionic current block. British Journal of Pharmacology, 172, 5147–5160.
Liang, P., Lan, F., Lee, A. S., et al. (2013). Drug screening using a library of human induced pluripotent stem cell-derived cardiomyocytes reveals disease-specific patterns of cardiotoxicity. Circulation, 127, 1677–1691.
Colatsky, T., Fermini, B., Gintant, G., et al. (2016). The comprehensive in vitro Proarrhythmia Assay (CiPA) initiative—Update on progress. Journal of Pharmacological and Toxicological Methods, 81, 15–20.
Xiao, R.-P., Zhu, W., Zheng, M., et al. (2006). Subtype-specific α1- and β-adrenoceptor signaling in the heart. Trends in Pharmacological Sciences, 27, 330–337.
Northover, B. J. (1983). A comparison of the electrophysiological actions of phentolamine with those of some other antiarrhythmic drugs on tissues isolated from the rat heart. British Journal of Pharmacology, 80, 85–93.
Azuma, J., Vogel, S., Josephson, I., et al. (1978). Yohimbine blockade of ionic channels in myocardial cells. European Journal of Pharmacology, 51, 109–119.
Hasegawa, J., Hirai, S., Saitoh, M., et al. (1988). Antiarrhythmic effects of alpha-adrenoceptor antagonists in guinea pig ventricular myocardium. Journal of the American College of Cardiology, 12, 1590–1598.
Satin, J., Kehat, I., Caspi, O., et al. (2004). Mechanism of spontaneous excitability in human embryonic stem cell derived cardiomyocytes. The Journal of Physiology, 559, 479–496.
Poulet, C., Wettwer, E., Grunnet, M., et al. (2015). Late sodium current in human atrial cardiomyocytes from patients in sinus rhythm and atrial fibrillation. PLoS ONE, 10, e0131432.
Morad, M., & Zhang, X.-H. (2017). Mechanisms of spontaneous pacing: sinoatrial nodal cells, neonatal cardiomyocytes, and human stem cell derived cardiomyocytes. Canadian Journal of Physiology and Pharmacology, 95, 1100–7.
Acknowledgements
All authors appreciate Professor Li Yanxin (Shanghai Children's Medical Center, Shanghai, China) for providing cell resources.
Funding
This study was supported by General Program of National Natural Science Foundation of China (82070430), Shanghai Pujiang Program (18PJD031), Shanghai Collaborative Innovation Center for Translational Medicine (TM201821), Shanghai Natural Science Foundation (20ZR1434500), Science and Technology Development Foundation of Shanghai Pudong (PKJ2020-Y06), the Biomedical Engineering fund of Shanghai Jiao Tong University (YG2021GD04), National Key R&D Program of China (2019YFA0110400), Health Commission of Minhang District, Shanghai (2018MW02).
Author information
Authors and Affiliations
Contributions
(I) Conception and design: WW, WF, JJZ; (II) administrative support: none; (III) provision of study materials or patients: none; (IV) collection and assembly of data: YQG, LY, YT; (V) data analysis and interpretation: YQG, LY; (VI) manuscript writing: all authors; (VII) final approval of manuscript: all authors.
Corresponding authors
Ethics declarations
Conflict of interest
All authors have no conflicts of interest to declare.
Ethical Approval
Not applicable.
Consent to Participate
Not applicable.
Consent for Publication
All authors have read the final manuscript and approved submission.
Informed Consent
Not applicable.
Research Involving Human Participants and/or Animals
Not applicable.
Additional information
Handling Editor: Michael Tranter.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Gong, Y., Yang, L., Tang, J. et al. Yohimbine Directly Induces Cardiotoxicity on Human-Induced Pluripotent Stem Cell-Derived Cardiomyocytes. Cardiovasc Toxicol 22, 141–151 (2022). https://doi.org/10.1007/s12012-021-09709-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12012-021-09709-3