Abstract
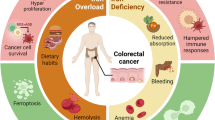
Colon cancer is a widespread life-threatening malignancy with complex and multifactorial etiology. Both epidemiological cohort studies and basic research support the substantial role of iron metabolism in colon cancer. Thus, understanding the mechanisms of how essential iron metabolic proteins are dysregulated may provide new treatment strategies for colon cancer. Ferritin is the main iron storage protein that occupies a vital position in iron metabolism. Studies reported that ferritin is differentially highly expressed in tissues from multiple malignancies. However, the source and function of highly expressed ferritin in colon cancer have not been explored. In this study, we found that the protein level but not RNA level of ferritin heavy chain (FTH1) was upregulated in colon cancer using paired clinical samples. Co-culture system was used to mimic the in vivo circumstance and study the cell–cell communication of macrophages and colon cancer cells. Results showed that M2 macrophages could substantially increase the FTH1 levels in colon cancer cells. This effect could be blocked by the exosome biogenesis/ secretion inhibitor GW4869, implying the vital role of exosomes in this biological process. Besides, we found that purified exosomes from M2 macrophages could deliver FTH1 into colon cancer cells and promote cell proliferation. Furtherly, EdU assay and live cell imaging system were performed in FTH1-OE (overexpression) colon cancer cell lines and confirmed the cell proliferation promoting effect of FTH1. Our results unveil the source and function of highly expressed FTH1 in colon cancer and provide a new potential therapeutic target for the treatment of colon cancer.






Similar content being viewed by others
Abbreviations
- FTH1:
-
Ferritin heavy chain 1
- OE:
-
Overexpression
- DMT1:
-
Divalent metal transporter1
- FTL:
-
Ferritin light chain
- TME:
-
Tumor microenvironment
- TAMs:
-
Tumor-associated macrophages
- COAD:
-
Colonic adenocarcinoma
- IHC:
-
Immunohistochemistry
- RT-qPCR:
-
Reverse transcription-quantitative polymerase chain reaction
- GAPDH:
-
Glyceraldehyde 3-phosphate dehydrogenase
- GEPIA:
-
Gene Expression Profiling Interactive Analysis
- TCGA:
-
The Cancer Genome Atlas
- GTEx:
-
Genotype-Tissue Expression
- FBS:
-
Fetal bovine serum
- PMA:
-
Phorbol-12-myristate-13-acetate
- CM:
-
Conditioned medium
- HRP:
-
Horseradish Peroxidase
- NTA:
-
Nanoparticle Tracking Analysis
- DAPI:
-
4′,6-Diamidino-2-phenylindole
- TPM:
-
Transcripts per million
- iNOS:
-
Induced nitrogen monoxide synthase
- ARG1:
-
Arginase-1
- LIP:
-
Labile iron pools
References
Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, Bray F (2021) Global Cancer Statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 71(3):209–249. https://doi.org/10.3322/caac.21660
Loomans-Kropp HA, Umar A (2019) Increasing incidence of colorectal cancer in young adults. J Cancer Epidemiol 2019:9841295. https://doi.org/10.1155/2019/9841295
Juloski JT, Rakic A, Cuk VV, Cuk VM, Stefanovic S, Nikolic D, Jankovic S, Trbovich AM, De Luka SR (2020) Colorectal cancer and trace elements alteration. J Trace Elem Med Biol 59:126451. https://doi.org/10.1016/j.jtemb.2020.126451
Feyzi A, Delkhosh A, Nasrabadi HT, Cheraghi O, Khakpour M, Barekati-Mowahed M, Soltani S, Mohammadi SM, Kazemi M, Hassanpour M, Rezabakhsh A, Maleki-Dizaji N, Rahbarghazi R, Namdarian R (2017) Copper sulfate pentahydrate reduced epithelial cytotoxicity induced by lipopolysaccharide from enterogenic bacteria. Biomed Pharmacother 89:454–461. https://doi.org/10.1016/j.biopha.2017.02.060
Cross AJ, Leitzmann MF, Gail MH, Hollenbeck AR, Schatzkin A, Sinha R (2007) A prospective study of red and processed meat intake in relation to cancer risk. PLoS Med 4(12):e325. https://doi.org/10.1371/journal.pmed.0040325
Cross AJ, Ferrucci LM, Risch A, Graubard BI, Ward MH, Park Y, Hollenbeck AR, Schatzkin A, Sinha R (2010) A large prospective study of meat consumption and colorectal cancer risk: an investigation of potential mechanisms underlying this association. Cancer Res 70(6):2406–2414. https://doi.org/10.1158/0008-5472.CAN-09-3929
Zhu CS, Pinsky PF, Kramer BS, Prorok PC, Purdue MP, Berg CD, Gohagan JK (2013) The prostate, lung, colorectal, and ovarian cancer screening trial and its associated research resource. J Natl Cancer Inst 105(22):1684–1693. https://doi.org/10.1093/jnci/djt281
Abbaspour N, Hurrell R, Kelishadi R (2014) Review on iron and its importance for human health. J Res Med Sci 19(2):164–174
Torti SV, Manz DH, Paul BT, Blanchette-Farra N, Torti FM (2018) Iron and cancer. Annu Rev Nutr 38:97–125. https://doi.org/10.1146/annurev-nutr-082117-051732
Xue X, Ramakrishnan SK, Weisz K, Triner D, Xie L, Attili D, Pant A, Gyorffy B, Zhan M, Carter-Su C, Hardiman KM, Wang TD, Dame MK, Varani J, Brenner D, Fearon ER, Shah YM (2016) Iron uptake via DMT1 integrates cell cycle with JAK-STAT3 signaling to promote colorectal tumorigenesis. Cell Metab 24(3):447–461. https://doi.org/10.1016/j.cmet.2016.07.015
Ren Y, Walczyk T (2014) Quantification of ferritin bound iron in human serum using species-specific isotope dilution mass spectrometry. Metallomics 6(9):1709–1717. https://doi.org/10.1039/c4mt00127c
Levi, S., A. Luzzago, G. Cesareni, A. Cozzi, F. Franceschinelli, A. Albertini and P. Arosio (1988) Mechanism of ferritin iron uptake: activity of the H-chain and deletion mapping of the ferro-oxidase site. A study of iron uptake and ferro-oxidase activity of human liver, recombinant H-chain ferritins, and of two H-chain deletion mutants. J Biol Chem 263(34): 18086–18092
Muhammad JS, Bajbouj K, Shafarin J, Hamad M (2020) Estrogen-induced epigenetic silencing of FTH1 and TFRC genes reduces liver cancer cell growth and survival. Epigenetics 15(12):1302–1318. https://doi.org/10.1080/15592294.2020.1770917
Alkhateeb AA, Connor JR (2013) The significance of ferritin in cancer: anti-oxidation, inflammation and tumorigenesis. Biochim Biophys Acta 1836(2):245–254. https://doi.org/10.1016/j.bbcan.2013.07.002
Alkhateeb AA, Han B, Connor JR (2013) Ferritin stimulates breast cancer cells through an iron-independent mechanism and is localized within tumor-associated macrophages. Breast Cancer Res Treat 137(3):733–744. https://doi.org/10.1007/s10549-012-2405-x
Buranrat B, Connor JR (2015) Cytoprotective effects of ferritin on doxorubicin-induced breast cancer cell death. Oncol Rep 34(5):2790–2796. https://doi.org/10.3892/or.2015.4250
Vaughn CB, Weinstein R, Bond B, Rice R, Vaughn RW, McKendrick A, Ayad G, Rockwell MA, Rocchio R (1987) Ferritin content in human cancerous and noncancerous colonic tissue. Cancer Invest 5(1):7–10. https://doi.org/10.3109/07357908709020300
van Niel G, D’Angelo G, Raposo G (2018) Shedding light on the cell biology of extracellular vesicles. Nat Rev Mol Cell Biol 19(4):213–228. https://doi.org/10.1038/nrm.2017.125
An T, Qin S, Xu Y, Tang Y, Huang Y, Situ B, Inal JM, Zheng L (2015) Exosomes serve as tumour markers for personalized diagnostics owing to their important role in cancer metastasis. J Extracell Vesicles 4:27522. https://doi.org/10.3402/jev.v4.27522
Milane L, Singh A, Mattheolabakis G, Suresh M, Amiji MM (2015) Exosome mediated communication within the tumor microenvironment. J Control Release 219:278–294. https://doi.org/10.1016/j.jconrel.2015.06.029
Mostafazadeh M, Kahroba H, Haiaty S, TazeKand AP, Samadi N, Rahbarghazi R, Nouri M (2022) In vitro exosomal transfer of Nrf2 led to the oxaliplatin resistance in human colorectal cancer LS174T cells. Cell Biochem Funct 40(4):391–402. https://doi.org/10.1002/cbf.3703
Arneth, B. (2019) Tumor microenvironment. Medicina (Kaunas) 56(1). https://doi.org/10.3390/medicina56010015
Jung M, Mertens C, Brune B (2015) Macrophage iron homeostasis and polarization in the context of cancer. Immunobiology 220(2):295–304. https://doi.org/10.1016/j.imbio.2014.09.011
Badawi MA, Abouelfadl DM, El-Sharkawy SL, El-Aal WE, Abbas NF (2015) Tumor-associated macrophage (TAM) and angiogenesis in human colon carcinoma. Open Access Maced J Med Sci 3(2):209–214. https://doi.org/10.3889/oamjms.2015.044
Lan J, Sun L, Xu F, Liu L, Hu F, Song D, Hou Z, Wu W, Luo X, Wang J, Yuan X, Hu J, Wang G (2019) M2 macrophage-derived exosomes promote cell migration and invasion in colon cancer. Cancer Res 79(1):146–158. https://doi.org/10.1158/0008-5472.CAN-18-0014
Ma YS, Wu TM, Ling CC, Yu F, Zhang J, Cao PS, Gu LP, Wang HM, Xu H, Li L, Wu ZJ, Wang GR, Li W, Lin QL, Liu JB, Fu D (2021) M2 macrophage-derived exosomal microRNA-155-5p promotes the immune escape of colon cancer by downregulating ZC3H12B. Mol Ther Oncolytics 20:484–498. https://doi.org/10.1016/j.omto.2021.02.005
Pinto ML, Rios E, Duraes C, Ribeiro R, Machado JC, Mantovani A, Barbosa MA, Carneiro F, Oliveira MJ (2019) The two faces of tumor-associated macrophages and their clinical significance in colorectal cancer. Front Immunol 10:1875. https://doi.org/10.3389/fimmu.2019.01875
Tang Z, Kang B, Li C, Chen T, Zhang Z (2019) GEPIA2: an enhanced web server for large-scale expression profiling and interactive analysis. Nucleic Acids Res 47(W1):W556-w560. https://doi.org/10.1093/nar/gkz430
Chanput W, Mes JJ, Wichers HJ (2014) THP-1 cell line: an in vitro cell model for immune modulation approach. Int Immunopharmacol 23(1):37–45. https://doi.org/10.1016/j.intimp.2014.08.002
Locati M, Curtale G, Mantovani A (2020) Diversity, mechanisms, and significance of macrophage plasticity. Annu Rev Pathol 15:123–147. https://doi.org/10.1146/annurev-pathmechdis-012418-012718
Genin M, Clement F, Fattaccioli A, Raes M, Michiels C (2015) M1 and M2 macrophages derived from THP-1 cells differentially modulate the response of cancer cells to etoposide. BMC Cancer 15:577. https://doi.org/10.1186/s12885-015-1546-9
Xu J, Wan Z, Zhou B (2019) Drosophila ZIP13 is posttranslationally regulated by iron-mediated stabilization. Biochim Biophys Acta Mol Cell Res 1866(9):1487–1497. https://doi.org/10.1016/j.bbamcr.2019.06.009
Catalano M, O’Driscoll L (2020) Inhibiting extracellular vesicles formation and release: a review of EV inhibitors. J Extracell Vesicles 9(1):1703244. https://doi.org/10.1080/20013078.2019.1703244
Wang H, An P, Xie E, Wu Q, Fang X, Gao H, Zhang Z, Li Y, Wang X, Zhang J, Li G, Yang L, Liu W, Min J, Wang F (2017) Characterization of ferroptosis in murine models of hemochromatosis. Hepatology 66(2):449–465. https://doi.org/10.1002/hep.29117
Wan Z, Xu J, Huang Y, Zhai Y, Ma Z, Zhou B, Cao Z (2020) Elevating bioavailable iron levels in mitochondria suppresses the defective phenotypes caused by PINK1 loss-of-function in Drosophila melanogaster. Biochem Biophys Res Commun 532(2):285–291. https://doi.org/10.1016/j.bbrc.2020.08.002
Xu J, Liu S, Cui Z, Wang X, Ning T, Wang T, Zhang N, Xie S, Min L, Zhang S, Liang C, Zhu S (2021) Ferrostatin-1 alleviated TNBS induced colitis via the inhibition of ferroptosis. Biochem Biophys Res Commun 573:48–54. https://doi.org/10.1016/j.bbrc.2021.08.018
Jung M, Mertens C, Tomat E, Brune B (2019) Iron as a central player and promising target in cancer progression. Int J Mol Sci 20(2). https://doi.org/10.3390/ijms20020273
Thevenod F (2018) Iron and its role in cancer defense: a double-edged sword. Met Ions Life Sci 18. https://doi.org/10.1515/9783110470734-021
Hou W, Xie Y, Song X, Sun X, Lotze MT, Zeh HJ 3rd, Kang R, Tang D (2016) Autophagy promotes ferroptosis by degradation of ferritin. Autophagy 12(8):1425–1428. https://doi.org/10.1080/15548627.2016.1187366
Kakhlon O, Gruenbaum Y, Cabantchik ZI (2002) Ferritin expression modulates cell cycle dynamics and cell responsiveness to H-ras-induced growth via expansion of the labile iron pool. Biochem J 363(Pt 3):431–436. https://doi.org/10.1042/0264-6021:3630431
Hu W, Zhou C, Jing Q, Li Y, Yang J, Yang C, Wang L, Hu J, Li H, Wang H, Yuan C, Zhou Y, Ren X, Tong X, Du J, Wang Y (2021) FTH promotes the proliferation and renders the HCC cells specifically resist to ferroptosis by maintaining iron homeostasis. Cancer Cell Int 21(1):709. https://doi.org/10.1186/s12935-021-02420-x
Li JY, Paragas N, Ned RM, Qiu A, Viltard M, Leete T, Drexler IR, Chen X, Sanna-Cherchi S, Mohammed F, Williams D, Lin CS, Schmidt-Ott KM, Andrews NC, Barasch J (2009) Scara5 is a ferritin receptor mediating non-transferrin iron delivery. Dev Cell 16(1):35–46. https://doi.org/10.1016/j.devcel.2008.12.002
Zhao M, Zhou B (2020) A distinctive sequence motif in the fourth transmembrane domain confers ZIP13 iron function in Drosophila melanogaster. Biochim Biophys Acta Mol Cell Res 1867(2):118607. https://doi.org/10.1016/j.bbamcr.2019.118607
Min L, Zhu S, Chen L, Liu X, Wei R, Zhao L, Yang Y, Zhang Z, Kong G, Li P, Zhang S (2019) Evaluation of circulating small extracellular vesicles derived miRNAs as biomarkers of early colon cancer: a comparison with plasma total miRNAs. J Extracell Vesicles 8(1):1643670. https://doi.org/10.1080/20013078.2019.1643670
Guo J, Wang X, Guo Q, Zhu S, Li P, Zhang S, Min L (2022) M2 Macrophage derived extracellular vesicle-mediated transfer of MiR-186-5p promotes colon cancer progression by targeting DLC1. Int J Biol Sci 18(4):1663–1676. https://doi.org/10.7150/ijbs.69405
Wang W, Knovich MA, Coffman LG, Torti FM, Torti SV (2010) Serum ferritin: past, present and future. Biochim Biophys Acta 1800(8):760–769. https://doi.org/10.1016/j.bbagen.2010.03.011
Ramirez-Carmona, W., B. Diaz-Fabregat, A. Yuri Yoshigae, A. Musa de Aquino, W. R. Scarano, A. C. de Souza Castilho, J. Avansini Marsicano, R. Leal do Prado, J. P. Pessan and L. de Oliveira Mendes (2021) Are serum ferritin levels a reliable cancer biomarker? A systematic review and meta-analysis. Nutr Cancer 1–10https://doi.org/10.1080/01635581.2021.1982996
Feng Z, Chen JW, Feng JH, Shen F, Cai WS, Cao J, Xu B (2015) The association between serum ferritin with colorectal cancer. Int J Clin Exp Med 8(12):22293–22299
Tappin JA, George WD, Bellingham AJ (1979) Effect of surgery on serum ferritin concentration in patients with breast cancer. Br J Cancer 40(4):658–660. https://doi.org/10.1038/bjc.1979.232
Acknowledgements
Figures 3a and 6 in this article were created by biorender.com (https://biorender.com/).
Funding
This work was supported by the Digestive Medical Coordinated Development Center of Beijing Hospitals Authority (XXZ015 to Jing Wu), the Special Scientific Research Fund for Tutor (YYDSZX201901 to Jing Wu), the Beijing Science and Technology Program (Z211100002921028 to Jing Wu), the Capital’s Funds for Health Improvement and Research (CFH2022-2–2025 to Jing Wu), and the Natural Science Foundation of Capital Medical University (PYZ21048 to Junxuan Xu).
Author information
Authors and Affiliations
Contributions
Zilu Cui designed and performed the experiments, analyzed data, and wrote the original manuscript. Wenkun Li, Yadan Wang, Kuiliang Liu, Yi Yang, Shuo Teng, and Nan Zhang helped with some of the experiments and analyzed data. Mengran Zhao helped with manuscript editing and provided key advice. Li Min, Peng Li, and Shutian Zhang provided key reagents and advice. Junxuan Xu conceived and supervised the study, analyzed data, and wrote and edited the original manuscript. Jing Wu conceived and supervised the study, analyzed data, and reviewed and edited the manuscript.
Corresponding authors
Ethics declarations
Ethics Approval and Consent to Participate
All patients enrolled in this study have signed the informed consents and this study was approved by the Ethics Committee of the Beijing Shijitan Hospital, Capital Medical University (Approval number: 2020–11).
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
12011_2022_3488_MOESM1_ESM.doc
Supplementary file1 Figure S1. The protein levels of FTH1 in colon cancer cells and macrophages. a Western Blot assay was used to detect the protein levels of FTH1 in Caco-2, SW480, M1, and M2 macrophages. (DOC 66 KB)
12011_2022_3488_MOESM2_ESM.doc
Supplementary file2 Figure S2. The overexpression of FTH1 does not promote the cell migration ability of colon cancer cells. a The cell migration was assessed by wound healing assay in Caco-2 and SW480 cells transfected with FTH1 overexpression plasmids or empty vectors. b Quantitative results of wound healing assay. All data were presented as the mean ± SEM of 3 independent assays. *p < 0.05, **p < 0.01, ***p < 0.001. ****p < 0.0001 vs Vector group. (DOC 824 KB)
12011_2022_3488_MOESM3_ESM.doc
Supplementary file3 Figure S3. M2 macrophage-derived exosomes promote colon cancer cell proliferation, but the effect was significantly attenuated by GW4869 (inhibitors of exosome). a After co-culture with supernatant medium from macrophage, EdU assay was used to detect the proliferation ability of Caco-2 and SW480 cells. b Quantitative results of EdU assay. All data were presented as the mean ± SEM of 3 independent assays. *p < 0.05, **p < 0.01, ***p < 0.001. ****p < 0.0001 vs Vector group. (DOC 972 KB)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Cui, Z., Li, W., Wang, Y. et al. M2 Macrophage-Derived Exosomal Ferritin Heavy Chain Promotes Colon Cancer Cell Proliferation. Biol Trace Elem Res 201, 3717–3728 (2023). https://doi.org/10.1007/s12011-022-03488-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12011-022-03488-w