Abstract
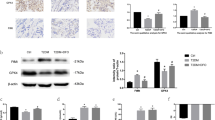
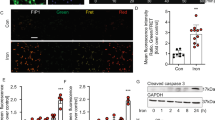
Iron overload has been found very common in diseases such as hereditary hemochromatosis, thalassemia, and sickle cell disease and in healthy postmenopausal women. Recent studies have shown that iron overload is considered an independent risk factor for osteoporosis. Studies have demonstrated that iron overload could induce apoptosis and inhibit viability in osteoblasts. However, the underlying mechanism still remains poorly understood. The purpose of the present study is to investigate possible mechanism of iron overload–induced apoptosis, and the roles autophagy and reactive oxygen species (ROS) played under iron overload conditions. Ferric ammonium citrate (FAC) (100–1600 μM) was utilized as iron donor to induce iron overload conditions. Intracellular iron concentration was measured using Iron Assay Kit. The viability was assessed by CCK-8 assay. Cell apoptosis was examined using Annexin V-FITC/PI staining with a flow cytometry, and levels of Bax, Bcl-2, cleaved caspase-3, and cleaved PARP were evaluated with Western blot. Cell autophagy was detected by evaluating LC3 with immunofluorescence and Western blot. The expressions of Beclin-1 and P62 were also assessed with Western blot. The intracellular ROS level was evaluated using a DCFH-DA probe with a flow cytometry, and NADPH oxidase 4 (Nox4) expressions were assessed with Western blot. Our results showed that FAC increased intracellular iron concentration and significantly inhibited cell viability. Furthermore, iron overload induced apoptosis and autophagy in osteoblast cells. What’s more, pretreatment with autophagy inhibitor chloroquine (CQ) enhanced iron overload–induced osteoblast apoptosis via the activation of caspases. Moreover, iron overload increased ROS production and Nox4 expression. Inhibition of autophagy increased ROS production, and scavenging of ROS by antioxidant N-Acetyl-L-cysteine (NAC) inhibited caspases activity and rescued iron overload–induced apoptosis. These results suggested that autophagy exerted cytoprotective effect, and scavenging excessive intracellular ROS could be a novel approach for the treatment of iron overload–induced osteoporosis.







Similar content being viewed by others
Data Availability
All data generated or analyzed during this study are included in this published article.
References
Bogdan AR, Miyazawa M, Hashimoto K, Tsuji Y (2016) Regulators of Iron homeostasis: new players in metabolism, cell death, and disease. Trends Biochem Sci 41(3):274–286. https://doi.org/10.1016/j.tibs.2015.11.012
Verbon EH, Trapet PL, Stringlis IA, Kruijs S, Bakker P, Pieterse CMJ (2017) Iron and immunity. Annu Rev Phytopathol 55:355–375. https://doi.org/10.1146/annurev-phyto-080516-035537
Franca M, Marti-Bonmati L, Porto G, Silva S, Guimaraes S, Alberich-Bayarri A, Vizcaino JR, Pessegueiro Miranda H (2018) Tissue iron quantification in chronic liver diseases using MRI shows a relationship between iron accumulation in liver, spleen, and bone marrow. Clin Radiol 73(2):215 e211–215 e219. https://doi.org/10.1016/j.crad.2017.07.022
Mehta KJ, Farnaud SJ, Sharp PA (2019) Iron and liver fibrosis: mechanistic and clinical aspects. World J Gastroenterol 25(5):521–538. https://doi.org/10.3748/wjg.v25.i5.521
Kew MC (2014) Hepatic iron overload and hepatocellular carcinoma. Liver Cancer 3(1):31–40. https://doi.org/10.1159/000343856
Gordan R, Wongjaikam S, Gwathmey JK, Chattipakorn N, Chattipakorn SC, Xie LH (2018) Involvement of cytosolic and mitochondrial iron in iron overload cardiomyopathy: an update. Heart Fail Rev 23(5):801–816. https://doi.org/10.1007/s10741-018-9700-5
Zhang H, Zhabyeyev P, Wang S, Oudit GY (2019) Role of iron metabolism in heart failure: from iron deficiency to iron overload. Biochim Biophys Acta Mol basis Dis 1865(7):1925–1937. https://doi.org/10.1016/j.bbadis.2018.08.030
Simcox JA, McClain DA (2013) Iron and diabetes risk. Cell Metab 17(3):329–341. https://doi.org/10.1016/j.cmet.2013.02.007
Yan N, Zhang J (2019) Iron metabolism, ferroptosis, and the links with Alzheimer’s disease. Front Neurosci 13:1443. https://doi.org/10.3389/fnins.2019.01443
Cotts KG, Cifu AS (2018) Treatment of osteoporosis. Jama 319(10):1040–1041. https://doi.org/10.1001/jama.2017.21995
Tella SH, Gallagher JC (2014) Prevention and treatment of postmenopausal osteoporosis. J Steroid Biochem Mol Biol 142:155–170. https://doi.org/10.1016/j.jsbmb.2013.09.008
Schnitzler CM, Schnaid E, MacPhail AP, Mesquita JM, Robson HJ (2005) Ascorbic acid deficiency, iron overload and alcohol abuse underlie the severe osteoporosis in black African patients with hip fractures--a bone histomorphometric study. Calcif Tissue Int 76(2):79–89. https://doi.org/10.1007/s00223-004-0053-9
Weinberg ED (2006) Iron loading: a risk factor for osteoporosis. Biometals 19(6):633–635. https://doi.org/10.1007/s10534-006-9000-8
Jeney V (2017) Clinical impact and cellular mechanisms of iron overload-associated bone loss. Front Pharmacol 8:77. https://doi.org/10.3389/fphar.2017.00077
Black DM, Rosen CJ (2016) Clinical practice. Postmenopausal osteoporosis. N Engl J Med 374(3):254–262. https://doi.org/10.1056/NEJMcp1513724
Thaung Zaw JJ, Howe PRC, Wong RHX (2018) Postmenopausal health interventions: time to move on from the Women’s Health Initiative? Ageing Res Rev 48:79–86. https://doi.org/10.1016/j.arr.2018.10.005
Cheng Q, Zhang X, Jiang J, Zhao G, Wang Y, Xu Y, Xu X, Ma H (2017) Postmenopausal iron overload exacerbated bone loss by promoting the degradation of type I collagen. Biomed Res Int 2017:1345193–1345199. https://doi.org/10.1155/2017/1345193
Zhang P, Wang S, Wang L, Shan BC, Zhang H, Yang F, Zhou ZQ, Wang X, Yuan Y, Xu YJ (2018) Hepcidin is an endogenous protective factor for osteoporosis by reducing iron levels. J Mol Endocrinol 60(4):297–306. https://doi.org/10.1530/JME-17-0301
Masse PG, Dosy J, Cole DE, Evroski J, Allard J, D'Astous M (2004) Is serum ferritin an additional cardiovascular risk factor for all postmenopausal women? Ann Nutr Metab 48(6):381–389. https://doi.org/10.1159/000082366
Kim BJ, Ahn SH, Bae SJ, Kim EH, Lee SH, Kim HK, Choe JW, Koh JM, Kim GS (2012) Iron overload accelerates bone loss in healthy postmenopausal women and middle-aged men: a 3-year retrospective longitudinal study. J Bone Miner Res 27(11):2279–2290. https://doi.org/10.1002/jbmr.1692
Kim BJ, Lee SH, Koh JM, Kim GS (2013) The association between higher serum ferritin level and lower bone mineral density is prominent in women >/=45 years of age (KNHANES 2008-2010). Osteoporos Int 24(10):2627–2637. https://doi.org/10.1007/s00198-013-2363-0
Siddiqui JA, Partridge NC (2016) Physiological bone remodeling: systemic regulation and growth factor involvement. Physiology (Bethesda) 31(3):233–245. https://doi.org/10.1152/physiol.00061.2014
Xia D, Wu J, Xing M, Wang Y, Zhang H, Xia Y, Zhou P, Xu S (2019) Iron overload threatens the growth of osteoblast cells via inhibiting the PI3K/AKT/FOXO3a/DUSP14 signaling pathway. J Cell Physiol 234:15668–15677. https://doi.org/10.1002/jcp.28217
Tower J (2015) Programmed cell death in aging. Ageing Res Rev 23(Pt A):90–100. https://doi.org/10.1016/j.arr.2015.04.002
Sendoel A, Hengartner MO (2014) Apoptotic cell death under hypoxia. Physiology (Bethesda) 29(3):168–176. https://doi.org/10.1152/physiol.00016.2013
Fuchs Y, Steller H (2011) Programmed cell death in animal development and disease. Cell 147(4):742–758. https://doi.org/10.1016/j.cell.2011.10.033
Tsay J, Yang Z, Ross FP, Cunningham-Rundles S, Lin H, Coleman R, Mayer-Kuckuk P, Doty SB, Grady RW, Giardina PJ, Boskey AL, Vogiatzi MG (2010) Bone loss caused by iron overload in a murine model: importance of oxidative stress. Blood 116(14):2582–2589. https://doi.org/10.1182/blood-2009-12-260083
Green DR, Llambi F (2015) Cell death signaling. Cold Spring Harb Perspect Biol 7(12). https://doi.org/10.1101/cshperspect.a006080
Kim KH, Lee MS (2014) Autophagy--a key player in cellular and body metabolism. Nat Rev Endocrinol 10(6):322–337. https://doi.org/10.1038/nrendo.2014.35
Parzych KR, Klionsky DJ (2014) An overview of autophagy: morphology, mechanism, and regulation. Antioxid Redox Signal 20(3):460–473. https://doi.org/10.1089/ars.2013.5371
Cen WJ, Feng Y, Li SS, Huang LW, Zhang T, Zhang W, Kong WD, Jiang JW (2018) Iron overload induces G1 phase arrest and autophagy in murine preosteoblast cells. J Cell Physiol 233(9):6779–6789. https://doi.org/10.1002/jcp.26405
Dixon SJ, Stockwell BR (2014) The role of iron and reactive oxygen species in cell death. Nat Chem Biol 10(1):9–17. https://doi.org/10.1038/nchembio.1416
Zheng QQ, Zhao YS, Guo J, Zhao SD, Song LX, Fei CM, Zhang Z, Li X, Chang CK (2017) Iron overload promotes erythroid apoptosis through regulating HIF-1a/ROS signaling pathway in patients with myelodysplastic syndrome. Leuk Res 58:55–62. https://doi.org/10.1016/j.leukres.2017.04.005
Doyard M, Fatih N, Monnier A, Island ML, Aubry M, Leroyer P, Bouvet R, Chales G, Mosser J, Loreal O, Guggenbuhl P (2012) Iron excess limits HHIPL-2 gene expression and decreases osteoblastic activity in human MG-63 cells. Osteoporos Int 23(10):2435–2445. https://doi.org/10.1007/s00198-011-1871-z
Chen B, Yan YL, Liu C, Bo L, Li GF, Wang H, Xu YJ (2014) Therapeutic effect of deferoxamine on iron overload-induced inhibition of osteogenesis in a zebrafish model. Calcif Tissue Int 94(3):353–360. https://doi.org/10.1007/s00223-013-9817-4
Kaminskyy VO, Zhivotovsky B (2014) Free radicals in cross talk between autophagy and apoptosis. Antioxid Redox Signal 21(1):86–102. https://doi.org/10.1089/ars.2013.5746
Mazure NM, Pouyssegur J (2010) Hypoxia-induced autophagy: cell death or cell survival? Curr Opin Cell Biol 22(2):177–180. https://doi.org/10.1016/j.ceb.2009.11.015
Radi E, Formichi P, Battisti C, Federico A (2014) Apoptosis and oxidative stress in neurodegenerative diseases. J Alzheimers Dis 42(Suppl 3):S125–S152. https://doi.org/10.3233/JAD-132738
Simao M, Camacho A, Ostertag A, Cohen-Solal M, Pinto IJ, Porto G, Hang Korng E, Cancela ML (2018) Iron-enriched diet contributes to early onset of osteoporotic phenotype in a mouse model of hereditary hemochromatosis. PLoS One 13(11):e0207441. https://doi.org/10.1371/journal.pone.0207441
Bordbar M, Haghpanah S, Zekavat OR, Saki F, Bazrafshan A, Bozorgi H (2019) Effect of different iron chelation regimens on bone mass in transfusion-dependent thalassemia patients. Expert Rev Hematol 12:1–7. https://doi.org/10.1080/17474086.2019.1662721
Chen X, Wang Z, Duan N, Zhu G, Schwarz EM, Xie C (2018) Osteoblast-osteoclast interactions. Connect Tissue Res 59(2):99–107. https://doi.org/10.1080/03008207.2017.1290085
Wang X, Chen B, Sun J, Jiang Y, Zhang H, Zhang P, Fei B, Xu Y (2018) Iron-induced oxidative stress stimulates osteoclast differentiation via NF-kappaB signaling pathway in mouse model. Metabolism 83:167–176. https://doi.org/10.1016/j.metabol.2018.01.005
Zhang J, Hu W, Ding C, Yao G, Zhao H, Wu S (2019) Deferoxamine inhibits iron-uptake stimulated osteoclast differentiation by suppressing electron transport chain and MAPKs signaling. Toxicol Lett 313:50–59. https://doi.org/10.1016/j.toxlet.2019.06.007
Galluzzi L, Green DR (2019) Autophagy-independent functions of the autophagy machinery. Cell 177(7):1682–1699. https://doi.org/10.1016/j.cell.2019.05.026
Cao L, Walker MP, Vaidya NK, Fu M, Kumar S, Kumar A (2016) Cocaine-mediated autophagy in astrocytes involves sigma 1 receptor, PI3K, mTOR, Atg5/7, Beclin-1 and induces type II programed cell death. Mol Neurobiol 53(7):4417–4430. https://doi.org/10.1007/s12035-015-9377-x
Xie D, Zhou P, Liu L, Jiang W, Xie H, Zhang L, Xie D (2019) Protective effect of Astragaloside IV on hepatic injury induced by iron overload. Biomed Res Int 2019:3103946–3103949. https://doi.org/10.1155/2019/3103946
Zheng Q, Zhao Y, Guo J, Zhao S, Fei C, Xiao C, Wu D, Wu L, Li X, Chang C (2018) Iron overload promotes mitochondrial fragmentation in mesenchymal stromal cells from myelodysplastic syndrome patients through activation of the AMPK/MFF/Drp1 pathway. Cell Death Dis 9(5):515. https://doi.org/10.1038/s41419-018-0552-7
Pan X, Zhang X, Sun H, Zhang J, Yan M, Zhang H (2013) Autophagy inhibition promotes 5-fluorouraci-induced apoptosis by stimulating ROS formation in human non-small cell lung cancer A549 cells. PLoS One 8(2):e56679. https://doi.org/10.1371/journal.pone.0056679
Wang Y, Zhao H, Wang D, Hao M, Kong C, Zhao X, Gao Y, Li J, Liu B, Yang B, Zhang H, Jiang J (2019) Inhibition of autophagy promoted apoptosis and suppressed growth of hepatocellular carcinoma upon photothermal exposure. J Biomed Nanotechnol 15(4):813–821. https://doi.org/10.1166/jbn.2019.2714
Shi M, Cheng L, Zhang Z, Liu Z, Mao X (2015) Ferroferric oxide nanoparticles induce prosurvival autophagy in human blood cells by modulating the Beclin 1/Bcl-2/VPS34 complex. Int J Nanomedicine 10:207–216. https://doi.org/10.2147/IJN.S72598
Chew KC, Ang ET, Tai YK, Tsang F, Lo SQ, Ong E, Ong WY, Shen HM, Lim KL, Dawson VL, Dawson TM, Soong TW (2011) Enhanced autophagy from chronic toxicity of iron and mutant A53T alpha-synuclein: implications for neuronal cell death in Parkinson disease. J Biol Chem 286(38):33380–33389. https://doi.org/10.1074/jbc.M111.268409
Zhang T, Li Y, Park KA, Byun HS, Won M, Jeon J, Lee Y, Seok JH, Choi SW, Lee SH, Man Kim J, Lee JH, Son CG, Lee ZW, Shen HM, Hur GM (2012) Cucurbitacin induces autophagy through mitochondrial ROS production which counteracts to limit caspase-dependent apoptosis. Autophagy 8(4):559–576. https://doi.org/10.4161/auto.18867
Funding
This study was supported by the National Natural Science Foundation of China [grant No. 81671811].
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Code Availability
Not applicable.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Xu, G., Li, X., Zhu, Z. et al. Iron Overload Induces Apoptosis and Cytoprotective Autophagy Regulated by ROS Generation in Mc3t3-E1 Cells. Biol Trace Elem Res 199, 3781–3792 (2021). https://doi.org/10.1007/s12011-020-02508-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12011-020-02508-x