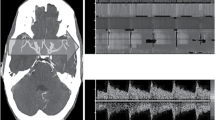
Opinion statement
Embolism is considered to be the main mechanism leading to brain infarction today; with the introduction of sophisticated neuroimaging tools, its impact is increasingly appreciated. Transcranial Doppler ultrasound allows noninvasive monitoring of in vivo embolism. Acute stroke, internal carotid artery stenosis, several cardiac conditions, internal carotid endarterectomy, and coronary artery bypass graft surgery have been extensively monitored. These investigations and other clinical and neuroimaging studies have expanded the understanding of brain embolism; they suggest it may be appropriate to think of it as a process that occurs in the context of other hemodynamic factors. Differences have been identified among several conditions regarding the temporal profile of embolism and the characteristics of embolic particles. This article presents a brief review of brain embolism monitoring with transcranial Doppler ultrasound.
Similar content being viewed by others
References and Recommended Reading
Caplan LR, Hennerici M: Impaired clearance of emboli (washout) is an important link between hypoperfusion, embolism, and ischemic stroke. Arch Neurol 1998, 55:1475–1482.
O’Donoghue ME, Dangond F, Burger AJ, et al.: Spontaneous calcific embolization to the supraclinoid internal carotid artery from a regurgitant bicuspid aortic valve. Neurology 1993, 43:2715–2717.
Wijman CAC, Kase CS, Jacobs AK, Whitehead RE: Cerebral air embolism as a cause of stroke during cardiac catheterization. Neurology 1998, 51:318–319.
Uribe Roca C, Gatto EM, Micheli F: Isolated weakness of index finger due to small cortical infarction. Neurology 2002, 59:2010–2011.
Aly A, Babikian VL, Barest G, et al.: Brain microembolism. J Neuroimaging 2003, in press.
Fieschi C, Argentino C, Lenzi GL, et al.: Clinical and instrumental evaluation of patients with ischemic stroke within the first six hours. J Neurol Sci 1989, 91:311–322.
Padayachee TS, Gosling RG, Bishop CC, et al.: Monitoring middle cerebral artery blood velocity during carotid endarterectomy. Br J Surg 1986, 73:98–100.
Spencer MP, Thomas GI, Nicholls SC, Sauvage LR: Detection of middle cerebral artery emboli during carotid endarterectomy. Stroke 1990, 21:415–423.
Russell D, Madden KP, Clark WM, et al.: Detection of arterial emboli using Doppler ultrasound in rabbits. Stroke 1991, 22:253–258.
Markus HS, Brown MM: Differentiation between different pathological cerebral embolic materials using transcranial Doppler in an in vitro model. Stroke 1993, 24:1–5.
Rodriguez AZ, Giachino A, Hosking M, Nathan HJ: Transcranial Doppler characteristics of different embolic materials during in vivo testing. J Neuroimaging 2002, 12:259–266. Laboratory study that suggests supporting the notion that ultrasonic signals correspond to actual emboli.
Ohki T, Roubin GS, Veith FJ, et al.: Efficacy of a filter device in the prevention of embolic events during carotid angioplasty and stenting: an ex vivo analysis. J Vasc Surg 1999, 30:1034–1044.
Droste DW, Hansberg T, Kemeny V, et al.: Oxygen inhalation can differentiate gaseous from nongaseous microemboli detected by transcranial Doppler ultra-sound. Stroke 1997, 28:2453–2456.
Russell D, Brucher R: Online automatic discrimination between solid and gaseous microemboli with the first multifrequency transcranial Doppler. Stroke 2002, 33:1975–1980.
Moehring MA, Spencer MP: Power M-mode Doppler (PMD) for observing cerebral blood flow and tracking emboli. Ultrasound Med Biol 2002, 28:49–57.
Alexandrov AV, Demchuk AM, Burgin WS: Insonation method and diagnostic flow signatures for transcranial power motion (M-mode) Doppler. J Neuroimaging 2002, 12:236–244.
Evans DH: Detection of microemboli. In Transcranial Doppler Ultrasonography, edn 2. Edited by Babikian VL, Wechsler LR. Boston: Butterworth Heinemann; 1999:141–156.
Basic identification criteria of Doppler microembolic signals. Consensus Committee of the Ninth International Cerebral Hemodynamics Symposium [no authors listed]. Stroke 1995, 26:11–23.
Ringelstein EB, Droste DW, Babikian VL, et al.: Consensus on microembolus detection by TCD. Stroke 1998, 29:725–729.
Droste DW, Decker W, Siemens HJ, et al.: Variability in occurrence of embolic signals in long term transcranial Doppler recordings. Neurol Res 1996, 18:25–30.
Alexandrov AV, Burgin S, Demchuk AM, et al.: Speed of intracranial clot lysis with intravenous tissue plasminogen activator therapy. Circulation 2001, 103:2897–2902.
Levi CR, Bladin CF, Chambers BC, et al.: Microembolic watershed infarction complicating carotid endarterectomy. Cerebrovasc Dis 1997, 7:185–186.
Babikian VL, Cantelmo NL, Wijman CAC: Neurovascular monitoring during carotid endarterectomy. In Transcranial Doppler Ultrasonography, edn 2. Edited by Babikian VL, Wechsler LR. Boston: Butterworth Heinemann; 1999:231–245.
Babikian VL, Hyde C, Pochay V, Winter MR: Clinical correlates of high-intensity signals detected on transcranial Doppler sonography in patients with cerebrovascular disease. Stroke 1994, 25:1570–1573.
Valton L, Larrue V, Arrue P, et al.: Asymptomatic cerebral embolic signals in patients with carotid stenosis. Correlation with appearance of plaque ulceration on angiography. Stroke 1995, 26:813–815.
Forteza AM, Babikian VL, Hyde C, Winter M: Effect of time and cerebrovascular symptoms on the prevalence of microembolic signals in patients with cervical carotid stenosis. Stroke 1996, 27:687–690.
Wong KS, Gao S, Chan YL, et al.: Mechanisms of acute cerebral infarctions in patients with middle cerebral artery stenosis: a diffusion-weighted imaging and microemboli monitoring study. Ann Neurol 2002, 52:74–81. Brain embolism and type of infarction in MCA stenosis.
Sliwka U, Klotzsch C, Popescu O, et al.: Do chronic middle cerebral artery stenoses represent an embolic focus? Stroke 1997, 28:1324–1327.
Gao S: Mechanism of ischemic stroke in patients with middle cerebral artery stenosis [MA thesis]. Hong Kong: The Chinese University of Hong Kong; 2001.
The French Study of Aortic Arch Plaques in Stroke Group. Atherosclerotic disease of the aortic arch as a risk factor for recurrent ischemic stroke [no authors listed]. N Engl J Med 1996, 334:1216–1221.
Rundek T, Di Tullio MR, Sciacca RR, et al.: Association between large aortic arch atheromas and high-intensity signals in elderly stroke patients. Stroke 1999, 30:2683–2686.
Babikian VL, Wijman CAC, Hyde C, et al.: Cerebral microembolism and early recurrent cerebral or retinal ischemic events. Stroke 1997, 28:1314–1318.
Valton L, Larrue V, le Traon AP, et al.: Microembolic signals and risk of early recurrence in patients with stroke or transient ischemic attack. Stroke 1998, 29:2125–2128.
Molloy J, Markus HS: Asymptomatic embolization predicts stroke and TIA risk in patients with carotid artery stenosis. Stroke 1999, 30:1440–1443.
Goertler M, Baeumer M, Kross R, et al.: Rapid decline of cerebral microemboli of arerial origin after intravenous acetylsalicylic acid. Stroke 1999, 30:60–69.
Sliwka U, Georgiadis D: Clinical correlations of Doppler microembolic signals in patients with prosthetic cardiac valves. Stroke 1998, 29:140–143.
Kaps M, Hansen J, Weiher M, et al.: Clinically silent microemboli in patients with artificial prosthetic aortic valves are predominantly gaseous and not solid. Stroke 1997, 28:322–325.
Sturzenegger M, Beer JH, Rihs F: Monitoring combined antithrombotic treatments in patients with prosthetic heart valves using transcranial Doppler and coagulation markers. Stroke 1995, 26:63–69.
Infeld B, Bowser DN, Gerraty RP, et al.: Cerebral microemboli in atrial fibrillation detected by transcranial Doppler ultrasonography. Cerebrovasc Dis 1996, 6:339–345.
Nadareishvili ZG, Choudary Z, Joyner C, et al.: Cerebral microembolism in acute myocardial infarction. Stroke 1999, 30:2679–2682.
Nabavi DG, Georgiadis D, Mumme T, et al.: Clinical relevance of intracranial microembolic signals in patients with left ventricular assist devices. Stroke 1996, 27:891–896.
Hartmann A, Hupp T, Koch HC, et al.: Prospective study on the complication rate of carotid surgery. Cerebrovasc Dis 1999, 9:152–156.
Spencer MP: Transcranial Doppler monitoring and causes of stroke from carotid endarterectomy. Stroke 1997, 28:685–691.
Gavrilescu T, Babikian VL, Cantelmo NL, et al.: Cerebral microembolism during carotid endarterectomy. Am J Surg 1995, 170:159–164.
Johnston WE, Stump DA, DeWitt DS, et al.: Significance of gaseous microemboli in the cerebral circulation during cardiopulmonary bypass in dogs. Circulation 1993, 88:319–329.
Ackerstaff RG, Moons KG, van de Vlasakker CJ, et al.: Association of intraoperative transcranial Doppler monitoring variables with stroke from carotid endarterectomy. Stroke 2000, 31:1817–1823.
Jansen C, Ramos LMP, van Heesewijk JPM, et al.: Impact of microembolism and hemodynamic changes in the brain during carotid endarterectomy. Stroke 1994, 25:992–997.
Cantelmo NL, Babikian VL, Samaraweera RN, et al.: Cerebral microembolism and ischemic changes associated with carotid endarterectomy. J Vasc Surg 1998, 27:1024–1031.
Levi CR, O’Malley HM, Fell G, et al.: Transcranial Doppler detected cerebral microembolism following carotid endarterectomy. Brain 1997, 120:621–629.
Lennard N, Smith J, Dumville J, et al.: Prevention of post-operative stroke after carotid endarterectomy: the role of transcranial Doppler. J Vasc Surg 1997, 26:579–584.
Jaeger HJ, Mathias KD, Hauth E, et al.: Cerebral ischemia detected with diffusion-weighted MR imaging after stent implantation in the carotid artery. AJNR Am J Neuroradiol 2002, 23:200–207.
Kaposzta Z, Clifton A, Molloy J, et al.: S-nitosoglutathione reduces asymptomatic embolization after carotid angioplasty. Circulation 2002, 106:3057–3062.
Stamou SC, Hill P, Dangas G, et al.: Stroke after coronary artery bypass. Stroke 2001, 32:1508–1513.
Libman RB, Wirkowski E, Neystat M, et al.: Stroke associated with cardiac surgery. Arch Neurol 1997, 54:83–87.
Dashe JF, Pessin MS, Murphy RE, Payne DD: Carotid occlusive disease and stroke risk in coronary artery bypass graft surgery. Neurology 1997, 49:678–686.
Newman MF, Kirchner JL, Phillips-Bute B, et al.: Longitudinal assessment of neurocognitive function after coronary-artery bypass surgery. N Engl J Med 2001, 344:395–402.
Moody DM, Bell MA, Challa VR, et al.: Brain microemboli during cardiac surgery or aortography. Ann Neurol 1990, 28:477–486.
Restrepo L, Wityk RJ, Grega MA, et al.: Diffusion and perfusion weighted magnetic resonance imaging of the brain before and after coronary artery bypass grafting surgery. Stroke 2002, 33:2909–2915.
Reichenspurner H, Navia JA, Robbins RC, et al.: Capture of particulate emboli during cardiac surgery: a new cannulation and filter device [abstract]. Circulation 1998, 98:I-100.
Barbut D, Hinton RB, Szatrowski TP, et al.: Cerebral emboli detected during bypass surgery are associated with clamp removal. Stroke 1994, 25:2398–2402.
Braekken SK, Russell D, Brucher R, et al.: Cerebral microembolic signals during cardiopulmonary bypass surgery. Stroke 1997, 28:1988–1992.
Pugsley W, Klinger L, Paschalis C, et al.: The impact of microemboli during cardiopulmonary bypass on neuropsychological functioning. Stroke 1994, 25:1393–1399.
Clark RE, Brillman J, Davis DA, et al.: Microemboli during coronary artery bypass grafting. J Thorac Cardiovasc Surg 1995, 109:249–258.
Hammon JW, Stump DA, Kon ND, et al.: Risk factors and solutions for the development of neurobehavioral changes after coronary artery bypass grafting. Ann Thorac Surg 1997, 63:1613–1618.
Forteza AM, Koch S, Romano JG, et al.: Transcranial Doppler detection of fat microemboli. Stroke 1999, 30:2687–2691.
Valdueza J, Harms L, Doepp F, et al.: Venous microembolic signals detected in patients with cerebral sinus thrombosis. Stroke 1997, 28:1607–1609.
Babikian VL, Caplan LR: Brain embolism is a dynamic process with variable characteristics. Neurology 2000, 54:797–801.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Babikian, V.L., Wijman, C.A. Brain embolism monitoring with transcranial Doppler ultrasound. Curr Treat Options Cardio Med 5, 221–232 (2003). https://doi.org/10.1007/s11936-003-0006-z
Issue Date:
DOI: https://doi.org/10.1007/s11936-003-0006-z