Abstract
Purpose of Review
To critically appraise the literature on the application, methods, and advances in emergency electroencephalography (EEG).
Recent Findings
The development of rapid EEG (rEEG) technologies and other reduced montage approaches, along with advances in machine learning over the past decade, has increased the rate and access to EEG acquisition. These achievements have made EEG in the emergency setting a practical diagnostic technique for detecting seizures, suspected nonconvulsive status epilepticus (NCSE), altered mental status, stroke, and in the setting of sedation.
Summary
Growing evidence supports using EEG to expedite medical decision-making in the setting of suspected acute neurological injury. This review covers approaches to acquiring EEG in the emergency setting in the adult and pediatric populations. We also cover the clinical impact of this data, the time associated with emergency EEG, and the costs of acquiring EEG in these settings. Finally, we discuss the advances in artificial intelligence for rapid electrophysiological interpretation.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Bedside clinical exams cannot reliably differentiate nonconvulsive status epilepticus (subclinical seizures) from other paroxysmal non-epileptic movements [1]. Electroencephalography (EEG) is one of the oldest diagnostic tools with demonstrated utility in potentially treatable acute neurological conditions related to vascular, traumatic, infectious, metabolic abnormalities, and delirium. It remains the gold standard for monitoring the brain in critical care settings.
Recently, there has been an increase in digital EEGs contributing significantly to our understanding of the brain during critical injuries. Therefore, one would assume that it is widely integrated into medical practice everywhere. However, conventional EEG depends on hospital access, technician availability, and trained EEG specialists to obtain and interpret the recording. Moreover, the time for acquiring conventional EEG can be delayed by several hours, which has historically limited the application in the emergency setting [2].
This review article summarizes current evidence regarding the use of emergency EEG including monitoring with reduced montage rapid response EEG (RRLM-EEG) technology and advances in artificial intelligence to expedite EEG interpretation. Specifically, we discuss the evidence that supports the use of emergency EEG in NCSE, stroke, and other causes of altered mental status. In addition, we discuss the cost, time to endpoints in the clinical setting, and its utility in pediatric populations.
Nonconvulsive Status Epilepticus
One of the most common indications for continuous EEG during long-term monitoring is to evaluate for NCSE. However, the need to detect NCSE early has given rise to numerous technologies classified as RRLM-EEG, which have enabled rapid detection of NCSE in acute care and emergency settings. These “electrode template systems” have been recommended in an American Clinical Neurophysiological Society (ACNS) consensus opinion to be used in emergencies when technicians are unavailable [3]. This section presents key articles highlighting emergency EEG’s diagnostic and clinical benefits.
In a prospective pilot study of 38 emergency department patients, staff and physicians placed Ceribell® rEEG (RRLM-EEG, rapid response limited montage EEG), and the on-call trained neurologist analyzed the recordings and provided the results [4••]. One patient was diagnosed with NCSE and received antiseizure medications. Emergency physicians used the Brain Stethoscope to aid in interpretation before on-call neurologist review in some cases. RRLM-EEG led to diagnostic confirmation in 42% and changed clinical management in 21% of patients.
Moreover, in a recent large multicenter prospective observational study of 181 ICU patients [5••], the device was placed and interpreted after a non-EEG-trained physician recorded a 2-min segment. The investigators administered a Likert scale questionnaire before and after use, rating the level of suspicion for seizure, confidence in diagnostic assessment, and treatment decisions. The accuracy of the bedside clinical assessment for seizures increased significantly after RRLM-EEG. Sensitivity increased from 77.8 to 100% and specificity from 63.9 to 89%, respectively.
Finally, a retrospective study on RRLM-EEG effects on antiseizure medication usage evaluated 100 consecutive cases suspected of having NCSE from the emergency and ICU departments [6•]. In 19 cases, high-risk patterns or seizures were identified, while the remaining 81 had nonspecific slowing or normal EEGs on expert review. The critical findings were that antiseizure medications were significantly reduced from 84 to 51% in patients with normal or slow patterns, and termination of sedation occurred in 15% of patients after EEG.
Stroke and Emergency EEG
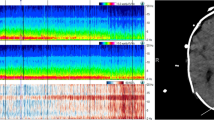
In this section, we discuss EEG during the emergent workup for stroke. Stroke is an acute neurological condition, and hospital-based treatments must be delivered rapidly. Even though the typical workflow involves transport to the computed tomography (C.T.) scanner for image acquisitions to assess the type of stroke, there is a role for expedited evaluation using RRLM-EEG independent of an assessment for post-stroke seizures. It is known that neurophysiological changes in the brain during ischemia lead to a decrease in alpha frequencies and an increase in delta frequencies in the EEG. This scientific basis and the recent advances in acquisition and analytical technology have made the EEG available for exploration in evaluating brain ischemia. A recent study examined if a 3-min EEG in the emergency department identified large vessel occlusion or major strokes and if the EEG measures correlated with the infarct volume [7]. The investigators extracted spectral power from the EEG recordings and obtained infarct volume from the magnetic resonance images or C.T. images demonstrating the index stroke. They used a nominal logistic regression model to assess the relationship between the EEG measures and the infarct volume and large vessel occlusion. This proof-of-concept study showed that detecting large vessel occlusion using an infarct volume of 20 ccs was robust using the 20 electrodes in the 10–20 lead montage. Also, they noted that EEG had a much better correlation with infarct volume than with NIHSS, and contralesional hemisphere findings were strongly correlated with infarct volume compared with ipsilateral hemisphere findings.
Similarly, a European study explored the EEG parameters with the infarct volume and the neurological deficits on admission. They were both proof-of-concept studies with small sample sizes — 24 and 31 — respectively. All admitted stroke unit patients underwent a clinical assessment and C.T. (non-contrast, angiogram, and perfusion) studies. After the perfusion, staff placed a pre-wired head cap, and a wireless EEG device was acquired. The publication provides the details of the acquisition and processing [8].
The authors analyzed the relationship between EEG parameters and the National Institute of Health Stroke Scale and C.T. Perfusion Images. Results showed that EEG parameters Delta/Alpha Ratio (DAR), (Delta+Theta)/(Beta+Alpha) Ratio (DTBAR) and relative delta power correlated directly with the total hypoperfused volume and the ischemic core, while alpha correlated inversely with the imaging findings.
Furthermore, Delta and Theta powers were higher in stroke patients than healthy controls; DAR was the strongest predictor of NIHSS at admission.
In summary, early evidence shows promise for EEG as a diagnostic aid in stroke diagnosis and the severity of stroke. Future studies must confirm the earlier findings before their application in clinical practice becomes a reality.
Other Causes of Altered Mental Status
Delirium is a common cause of altered mental status in the emergency department. Beyond NCSE, EEG in the emergency setting may have a role in identifying other causes of altered mental status. Lee et al. investigated the role of point-of-care EEG in delirium detection in a prospective pilot study at a single academic emergency department. Forty-eight patients were enrolled [9]. Bispectral EEG (two channel EEG or BSEEG) demonstrated diffuse slow waves across all 20 EEG leads in delirious patients. At a BSEEG index (ratio of low to high-frequency brain activity) of 1.45, for delirium, the sensitivity was 88.9%, and specificity was 92.3%. The positive and negative likelihood ratios were 11.6 and 0.12, respectively.
RRLM-EEG may help evaluate patients under infection control precautions [10, 11]. In a small, single-center study conducted in all patient care areas, ten patients in isolation rooms with COVID-19 utilized the RRLM-EEG EEG device to evaluate for status epilepticus compared to a control group of 40 patients with standard EEG monitoring [10]. It is noteworthy that RRLM-EEG was also associated with a statistically significant decrease in on-call EEG technologist workforce utilization, as none of the 10 RRLM-EEG EEG patients required the on-call technologist. On the other hand, EEG technicians placed 15 out of the 40 in the control group. Remarkably, RRLM-EEG was placed on some patients in the prone position, which can present challenges during conventional EEG placement.
Sedation
In the operative theater, anesthesiologists have used the bispectral index monitor (BIS; Medtronic-Covidien) and other similar processed EEG devices to complement the clinical assessment of depth of anesthesia since the late 1990s. With the BIS system, electrodes placed on a patient’s forehead collect EEG signals processed into different component waveforms. The raw EEG data provides a burst suppression ratio, and together with the relative proportions of high- and low-frequency waveforms, this is combined to produce a single numerical BIS value ranging from 0 (cortical electrical silence) and 100 (normal awake activity) [12].
These systems have the advantage of being easy to apply and can be interpreted by unspecialized clinicians. However, its use outside the operating rooms, in emergency settings, and in critical care units has numerous pitfalls. Lack of neuromuscular blockade, lower depths of sedation in non-operating room settings, and even sources of electrical artifacts from other biomedical devices may make the bispectral index and additional processed EEG information less reliable [12–14]. Nevertheless, multiple studies have explored the utility of these limited EEG systems in emergency settings and critical care units.
Perhaps a more reliable use of processed EEG and other rapid response EEG devices in the emergency and critical care setting is for monitoring sedation in patients where deep neuroprotective sedation or burst suppression is desired. Consensus statements from the European Society of Intensive Care and the ACNS recommend frequent (intermittent or continuous EEG) monitoring in critically ill patients for multiple indications, including cerebral ischemia, nonconvulsive status epilepticus, unexplained altered mental status, and post-cardiac-arrest coma [15–18]. New rapid EEG devices may allow more convenient and earlier initiation of such sedation monitoring in the E.D. and ICU while providing greater fidelity than traditional processed EEG devices like the BIS monitor. Rapid EEG devices are more like conventional EEG systems. They could be more helpful in assessing the early trajectories of EEG evolution and prognostication of patients with encephalopathy and coma [19•]. Finally, with the widespread adoption of deeper sedation regimens than previously used for COVID-related ARDS, EEG assessment of sedation depth has received renewed research interest in recent years [11].
Pediatric Emergency EEG
EEG has long been utilized in pediatrics for various indications including concern for NCSE, the diagnostic workup of paroxysmal events concerning seizures, pharmacological paralysis, therapeutic hypothermia, and sudden unexplained changes in mental status [16]. However, few point-of-care EEG trials have been conducted in the pediatric emergency population. Nozowa et al. used a simplified 6-electrode EEG array patterning in amplitude-integrated EEG [20]. Pediatric emergency physicians placed this reduced array in just over 5 min. The patients were selected for study if they had prolonged disturbances of consciousness, suspected NCSE, or in the setting of sedation/neuromuscular blockade. The recordings were classified into two categories: persistent rhythmic waves (suggestive of NCSE) or persistent high-amplitude slow waves (suggestive of encephalopathy/encephalitis), given the reduced array. They found later those two cases had neurologic pathology on standard EEG. However, in most cases, the limited EEG method allowed clinicians to make expeditious and appropriate treatment and disposition decisions [20].
Simma et al. demonstrated that NCSE was identified in six out of 36 patients in a convenience sample, using a limited 2-electrode point-of-care EEG system applied by emergency nurses and interpreted by emergency physicians with the assistance of remote pediatric neurology consultants [21].
The potential benefits of rapid response EEG in pediatric E.D. may be even greater than that in the adult population, given the limited availability of traditional cEEG and pediatric neurologists and children’s poor tolerance of conventional 10–20 EEG systems. Further study of newer rapid response EEG devices in larger populations of children, with validation of collected data against traditional EEG systems, will be needed before more widespread adoption in the pediatric population. Though less studied in the pediatric population, RRLM-EEG studies from adult populations offer advantages over conventional EEG regarding cost, time, and ease of interpretation.
Time to EEG
Time to EEG is a critical variable that can expedite or hinder downstream diagnosis. As discussed in the previous sections, conventional EEGs were limited by logistics, such as needing a specialist staff, time to set up, and an on-call neurologist to review EEG. RRLM-EEG has significantly bolstered and improved the efficiency of obtaining EEGs in emergency conditions.
In the critical care setting, the investigators compared commercially available wireless EEG, an 8-electrode single-use gel electrode headset called CerebAir®, versus control of convention EEG with a similarly placed 8-electrode array [18]. The time for electrode placement was significantly faster with the use of the RRLM-EEG headset with a p < 0.0001 [18]. The wireless capability also allows cloud-based remote interpretation by EEG-trained physicians anywhere in the world. The opportunity to use such headset technology in low-resource settings and emergent settings has opened the doors for rapid evaluation using EEG.
LaMonte et al. compared the use of RRLM-EEG with a standard 18-channel EEG system to diagnose when there was a suspected case of NCSE [10]. The average time to interpret an EEG with the use of the RRLM-EEG was 23.8 min compared with 126.5 min with the control standard 18-channel EEG. A similar study by Vespa et al. evaluated patients with suspected NCSE with RRLM-EEG and reported a median time to EEG of 5 min compared to 239 min for a conventional EEG [5••]. Other devices have shown similar results in other studies [10, 19•, 22•, 23, 24].
Another study evaluated the use of an EEG cap placed by a neurology resident physician versus conventional EEG [22•]. When compared to 104.5 min using a conventional EEG, significant time savings were seen with the EEG cap, which has a median “time to cap” EEG recording of 22.5 min. In summary, as shown in the current studies, rapid diagnosis of NCSE or other diagnoses supported using EEG in the future can be made quicker by wearables [21].
Cost and Accessibility
Access to cEEG in community hospitals may be limited to the high costs of specialized equipment and personnel. However, recent studies suggest the implementation of RRLM-EEG may reduce overall healthcare costs. Ney et al. evaluated RRLM-EEG cost-benefits in the hospital and found that each use of RRLM-EEG as a Rapid-EEG system saved between $3971 and $17,290 [25•]. These cost-benefits result from reduced hospitalizations and unnecessary use of antiseizure medications in those with suspected NCSE [26–28]. Specifically, the deployment of this rapid tool reduced hospital length of stay by 1.2 days and length of stay in the intensive care unit by 0.4 days.
The cost saved by EEG in the emergency department is the downstream being associated with treatment resulting from the initial delay to diagnosis when EEG is unavailable [28]. Other studies have highlighted “overtreatment” in suspected NCSE where EEG was unavailable, leading to potentially preventable sedation, intubation, and intensive care unit stays — all these actions could be mitigated if NCSE could be excluded early during the clinical presentation [5••, 6•].
A recent study also reported that RRLM-EEG reduced the frequency of inter-hospital transfers for cEEG after utilizing RRLM-EEG in a community hospital [29•]. Onsite general neurologists interpreted the initial 68 studies from 40 patients before trained epileptologists conducted remote interpretation on an additional 50 Rapid-EEG studies from 34 patients. There was a 44.6% transfer rate for cEEG due to suspected NCSE. The transfer rate dropped to 5% after RRLM-EEG was deployed at the hospital and interpreted by an onsite non-EEG-trained neurologist. There was then a shift to a hub-and-spoke-EEG model with interpretation by a remote epileptologist, at which point there were no further transfers for NCSE through the study dates. Based on the prior transfer rate without RRLM-EEG, there was a cost-saving of over $39,000 ($1274 per patient) after implementation [29•]. These technologies promise the delivery of EEG to globally underserved and low-resource settings where the device and access to the internet can lead to diagnosis by an expert potentially continents away.
Artificial Intelligence
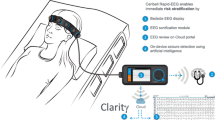
Although expert physicians read EEG recordings in most circumstances, there has been a recent growth in machine learning algorithms for both conventional and RRLM-EEG, such as Clarity®, designed by Ceribell® Inc., to detect epileptiform activity.
A retrospective cohort study reported high performance of clarity in 353 adult patients in the emergency departments and critical care units across six academic and community hospitals who underwent evaluation for altered mental status and NCSE using the RRLM-EEG device [30]. When compared with neurologists, authors reported high sensitivity (100%) and specificity (93%) when evaluating EEG with > 90% seizure burden in status epilepticus. Emergency physicians reported 100% sensitivity and 92% specificity in assessing suspected seizures using the Brain Stethoscope function [4••]. Sanz-García et al. observed a better correlation of the depth of sedation with EEG feature using a machine learning approach than with traditional bispectral index systems in the ICU [14].
A systematic review that compared Bersa 2.0, Encevis 1.7, and Persyst 13 reported similar sensitivities for seizure detection (67.6%, 77.8, and 81%, respectively). However, there were differences in the time to detection — Persyst detection in the 20 s, Encevis in 25 s, and Besa being the slowest in the 30 s. The false positive rate was highest with Persyst, followed by Besa and Encevis [31]. Epileptologists primarily utilize these programs during long-term monitoring, though, in the future, this could change. Ongoing improvements in seizure prediction algorithms may reduce the reliance on visual interpretation by a subspecialist, the time to interpretation, and increase accessibility to community hospitals and emergency departments.
Signal Quality
Multiple FDA-approved RRLM-EEG systems are commercially available, featuring various formats, including dry electrodes, ring electrodes, electrode caps, and others that use single-use gel electrodes. Some have a complete 10–20 pattern, while others are reduced electrode arrays. These can be wired to a junction box or wireless with the ability to transmit to a cloud-based server. The different styles of devices may offer some technical advantages; however, experience and access are not widespread in the medical community yet for larger studies, given the recency of their development.
Dry electrodes offer the advantage of being placed rapidly without needing skin preparation. A recent study compared the F1, Nielsen dry wireless EEG system to conventional and found the recording quality was similar except for delta and gamma bands [32]. The authors note that movement can compromise recording quality. Notably, patients were seated during the EEG, which may limit some translation to clinical practice in the emergency department. However, mitigation of movement artifacts while optimizing a high signal remains the subject of ongoing research with novel amplifiers, software improvement, and electrode configurations in dry systems [9, 32–34].
A prospective study compared the recording quality of 22 patients taken with RRLM-EEG along with simultaneous conventional Ag/AgCl electrodes placed adjacent to the RRLM-EEG electrodes running on two independent systems [35•]. A Wilcoxon signed-rank test comparing each EEG quality metric found no significant difference across the recordings though RRLM-EEG detected less 60 Hz compared to conventional EEG. Moreover, the quality RRLM-EEG of the recordings has been similar when placed by nonspecialized personnel [5••, 10, 23, 36••].
A single-center feasibility study also compared the quality of cEEG recordings acquired RRLM-EEG when placed by a trained technician versus an ICU physician [19•]. The EEG signal quality was adequate for cEEG, and epileptiform abnormalities were similar in the control and study groups. That said, EEG acquired with rapid devices is not without some limitations.
Limitations
It is important to note that these reduced montage RRLM-EEG devices are not designed to be a replacement for the conventional EEG with a complete 10–20 array. Reduced montage systems were designed to capture board field abnormalities sufficient to account for altered mental status. They can be used to assess sedation but lack the spatial resolution to localize minor focal abnormalities, which could account for the patient’s presentation. As such, they will serve as screening tools in emergency care settings.
These brief recordings may come at the price of sensitivity, as was suggested in a narrative review that evaluated the utility of brief RRLM-EEG recordings versus continuous EEG in the elderly to help distinguish NCSE from delirium [37]. They concluded that while RRLM-EEG is faster to acquire recordings in patients who may be agitated or confused, the variable and dynamic changes of NSCE may be better assessed by cEEG.
Although rapid devices produce recordings, studies report that interventions may be necessary to maintain an adequate signal. Though rapid devices have demonstrated significantly faster times-to-EEG, a recent study with a cap placed by residents was only interpretable in 70% of studies versus 95% with conventional EEG. Also, when nonspecialized physicians put the devices, the skin irritation was noted to be worse [19•].
Future Directions
The recent focus is on developing and interpreting ultralong term EEG. Technological advances are increasing the ease of setup and portability while decreasing the bulk and power consumption of EEG devices [34]. Dabbaghian et al. recently described a new flexible 8-channel dry electrode system including onboard motion artifact removal designed to monitor the frontal and temporal lobes that weigh just over 9 g and can be powered by a coin battery [38]. There are also exquisitely subtle small flexible temporary tattoo-based EEG electrodes in development, which can be placed on hairless skin for multiday ambulatory recordings [34].
The increasing volume of long and ultra-long-term data from epilepsy patients, along with increasing utilization of RRLM-EEG, will necessitate a greater reliance on improvements in machine learning. As the sensitivity of these devices continues to improve, there may be a role in EMS implementation to assist in expeditious triage and treatment of seizures. Seizure forecasting may also become a reality with a greater understanding of the multidien patterns through longitudinal data from implanted devices and ultralong term wearable devices [39,40,41]. All of these can translate into technology that benefits the acquisition of EEG acquisition in the emergency environment.
Discussion
Early EEG shows promise to expedite the diagnostic workup of neurological injury in the emergency and critical care settings. Emergency EEG can detect subclinical seizures and limit empiric antiseizure treatment in cases of undifferentiated altered mental status. rEEG offers a practical and cost-effective alternative, given the limitations of conventional EEG in our current medical infrastructure. This likely translates to pediatric populations though the literature is currently sparse, and specific pediatric headsets are still developing. Its role in the standard workup of stroke is an area of ongoing research.
Conventional EEG remains the standard for source localization and identification of more minor focal abnormalities given more excellent spatial resolution; however, RRLM-EEG systems offer significant value in the speed of data acquisition, portability, and cost. RRLM-EEG placement by nonspecialized may require more interventions to maintain an adequate signal quality during cEEG. Larger scale studies are still needed in pediatric populations and stroke patients. Given that RRLM-EEG systems are still a relatively new technology, large-scale studies and comparative evaluations of the available systems may be the subject of potential future studies.
Conclusion
Though the neurodiagnostic benefits of conventional EEG acute neurological injury have been well established, the utility is generally not possible or pragmatic in the emergency setting. While not a replacement for conventional EEG, great strides over the last decade have resulted in the development of RRLM-EEG technologies which can bring about a cost-effective solution for neurophysiological monitoring with less reliance on specialized personnel. Wider implementation of this technology in emergency departments and lower resource settings shows promise to reduce the morbidity and mortality associated with unrecognized NCSE and the differentiation of altered mental status of unknown etiology.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Brophy GM, Bell R, Claassen J, Alldredge B, Bleck TP, Glauser T, et al. Guidelines for the evaluation and management of status epilepticus. Neurocrit Care. 2012;17(1):3–23.
Gururangan K, Razavi B, Parvizi J. Utility of electroencephalography: experience from a U.S. tertiary care medical center. Clin Neurophysiol. 2016;127(10):3335–40.
Herman ST, Abend NS, Bleck TP, Chapman KE, Drislane FW, Emerson RG, et al. Consensus statement on continuous EEG in critically ill adults and children, part I: indications. J Clin Neurophysiol. 2015;32(2):87–95.
•• Wright NMK, Madill ES, Isenberg D, Gururangan K, McClellen H, Snell S, et al. Evaluating the utility of rapid response EEG in emergency care. Emerg med j: EMJ. 2021;38(12):923–6. A two-center pilot study of Ceribell utilization in the emergency department in epileptologists and E.M. physicians interpreted EEGs.
•• Vespa PM, Olson DM, John S, Hobbs KS, Gururangan K, Nie K, et al. Evaluating the clinical impact of rapid response electroencephalography: the DECIDE multicenter prospective observational clinical study. Crit care med. 2020;48(9):1249–57. A large prospective study is comparing the time and clinical impact of Ceribell to conventional EEG.
• Kurup D, Davey Z, Hoang P, Wu C, Werbaneth K, Shah V, et al. Effect of rapid EEG on antiseizure medication usage. Epileptic Disord. 2022;24(5):1–7. A retrospective study demonstrated the effect of rEEG medication treatment decisions.
Shreve L, Kaur A, Vo C, Wu J, Cassidy JM, Nguyen A, et al. Electroencephalography measures are useful for identifying large acute ischemic stroke in the emergency department. J stroke cerebrovasc dis: off J Natl Stroke Assoc. 2019;28(8):2280–6.
Ajčević M, Furlanis G, Miladinović A, Buoite Stella A, Caruso P, Ukmar M, et al. Early EEG alterations correlate with CTP hypoperfused volumes and neurological deficit: a wireless EEG study in hyper-acute ischemic stroke. Ann Biomed Eng. 2021;49(9):2150–8.
Lee S, Yuki K, Chan A, Cromwell J, Shinozaki G. The point-of-care EEG for delirium detection in the emergency department. Am J Emerg Med. 2019;37(5):995–6.
LaMonte MP. Ceribell EEG shortens seizure diagnosis and workforce time and is useful for COVID isolation. Epilepsia open. 2021;6(2):331–8.
Michalak AJ, Mendiratta A, Eliseyev A, Ramnath B, Chung J, Rasnow J, et al. Frontotemporal EEG to guide sedation in COVID-19 related acute respiratory distress syndrome. Clin Neurophysiol. 2021;132(3):730–6.
Hajat Z, Ahmad N, Andrzejowski J. The role and limitations of EEG-based depth of anesthesia monitoring in theatres and intensive care. Anaesthesia. 2017;72(Suppl 1):38–47.
Romagnoli S, Franchi F, Ricci Z. Processed EEG monitoring for anesthesia and intensive care practice. Minerva Anestesiol. 2019;85(11):1219–30.
Sanz-García A, Pérez-Romero M Fau - Pastor J, Pastor J Fau - Sola RG, Sola Rg Fau - Vega-Zelaya L, Vega-Zelaya L Fau - Vega G, Vega G Fau - Monasterio F, et al. Potential EEG biomarkers of sedation doses in intensive care patients unveiled by using a machine learning approach. (1741–2552 (Electronic)).
Claassen J, Taccone FS, Horn P, Holtkamp M, Stocchetti N, Oddo M, et al. Recommendations on the use of EEG monitoring in critically ill patients: consensus statement from the neurointensive care section of the ESICM. Intensive Care Med. 2013;39(8):1337–51.
Herman ST, Abend NS, Bleck TP, Chapman KE, Drislane FW, Emerson RG, et al. Consensus statement on continuous EEG in critically ill adults and children, part I: indications. J Clin Neurophysiol. 2015;32(2):87–95.
Rittenberger JC, Weissman A, Baldwin M, Flickinger K, Repine MJ, Guyette FX, et al. Preliminary experience with point-of-care EEG in post-cardiac arrest patients. Resuscitation. 2019;135:98–102.
Soar J, Callaway CW, Aibiki M, Bottiger BW, Brooks SC, Deakin CD, et al. Part 4: Advanced life support: 2015 International Consensus on Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Science with Treatment Recommendations. Resuscitation. 2015;95:e71-120.
• Caricato A, Della Marca G, Ioannoni E, Silva S, BenziMarkushi T, Stival E, et al. Continuous EEG monitoring by a new simplified wireless headset in the intensive care unit. BMC anesthesiol. 2020;20(1):298. cEEG within the ICU was performed with CerebAir®.
Nozawa M, Terashima H, Tsuji S, Kubota M. A simplified electroencephalogram monitoring system in the emergency room. Pediatr Emerg Care. 2019;35(7):487–92.
Simma L, Bauder F, Schmitt-Mechelke T. Feasibility and usefulness of rapid 2-channel-EEG-monitoring (point-of-care EEG) for acute CNS disorders in the paediatric emergency department: an observational study. Emerg med j: EMJ. 2021;38(12):919–22.
• McKay JH, Feyissa AM, Sener U, DʼSouza C, Smelick C, Spaulding A, et al. Time is brain the use of EEG electrode caps to rapidly diagnose nonconvulsive status epilepticus. J clin neurophysiol off publ Am Electroencephalographic Soc. 2019;36(6):460–6. This prospective study of conventional EEG versus an electrode cap placed emergently by a neurology resident.
Yazbeck M, Sra P, Parvizi J. Rapid response electroencephalography for urgent evaluation of patients in community hospital intensive care practice. J neurosci nurs: J Am Assoc Neurosci Nurses. 2019;51(6):308–12.
Titgemeyer Y, Surges R, Altenmüller D-M, Fauser S, Kunze A, Lanz M, et al. Can commercially available wearable EEG devices be used for diagnostic purposes? An explorative pilot study. Epilepsy behav: E&B. 2020;103(Pt A):106507.
• Ney JP, Gururangan K, Parvizi J. Modeling the economic value of Ceribell rapid response EEG in the inpatient hospital setting. J med econ. 2021;24(1):318. The retrospective cost-benefit model from the DECIDE trial favored the implementation of rEEG.
Wang M, Perera K, Josephson CB, Lamidi M, Lawal OA, Awosoga O, et al. Association between antiseizure medications and quality of life in epilepsy: a mediation analysis. Epilepsia. 2022;63(2):440–50.
Josephson CB, Wiebe S, Delgado-Garcia G, Gonzalez-Izquierdo A, Denaxas S, Sajobi TT, et al. Association of enzyme-inducing antiseizure drug use with long-term cardiovascular disease. JAMA Neurol. 2021;78(11):1367–74.
Raucci U, Pro S, Di Capua M, Di Nardo G, Villa MP, Striano P, et al. A reappraisal of the value of video-EEG recording in the emergency department. Expert Rev Neurother. 2020;20(5):459–75.
Madill ES, Gururangan K, Krishnamohan P. Improved access to rapid electroencephalography at a community hospital reduces inter-hospital transfers for suspected nonconvulsive seizures. Epileptic disorders: international epilepsy journal with videotape. 2022. rEEG reduced the frequency of hospital transfers in a community setting when interpreted by both general neurologists and EEG-trained physicians.
Kamousi B, Karunakaran S, Gururangan K, Markert M, Decker B, Khankhanian P, et al. Monitoring the burden of seizures and highly epileptiform patterns in critical care with a novel machine learning method. Neurocrit Care. 2021;34(3):908–17.
Koren J, Hafner S, Feigl M, Baumgartner C. Systematic analysis and comparison of commercial seizure-detection software. Epilepsia. 2021;62(2):426–38.
Kam JWY, Griffin S, Shen A, Patel S, Hinrichs H, Heinze H-J, et al. Systematic comparison between a wireless EEG system with dry electrodes and a wired EEG system with wet electrodes. Neuroimage. 2019;184:119–29.
Hinrichs H, Scholz M, Baum AK, Kam JWY, Knight RT, Heinze HJ. Comparison between a wireless dry electrode EEG system with a conventional wired wet electrode EEG system for clinical applications. Sci Rep. 2020;10(1):5218.
Casson AJ. Wearable EEG and beyond. Biomed Eng Lett. 2019;9(1):53–71.
• Kamousi B, Grant AM, Bachelder B, Yi J, Hajinoroozi M, Woo R. Comparing the quality of signals recorded with a rapid response EEG and conventional clinical EEG systems. Clin neurophysiol pract. 2019;4:69–75. Simultaneously acquired EEG with Ceribell versus conventional EEG are equivalent.
•• Kurup D, Gururangan K, Desai MJ, Markert MS, Eliashiv DS, Vespa PM, et al. Comparing seizures captured by rapid response EEG and conventional EEG recordings in a multicenter clinical study. Front Neurol. 2022;13:915385. Retrospective evaluation of seizures captured during the DECIDE trial between conventional EEG and Ceribell demonstrated concordant findings, with none occurring solely over the parasagittal region.
Manfredonia F, Saturno E, Lawley A, Gasverde S, Cavanna AE. The role of electroencephalography in the early diagnosis of nonconvulsive status epilepticus in elderly patients with acute confusional state: two possible strategies? Seizure. 2019;73:39–42.
Dabbaghian A, Yousefi T, Fatmi SZ, Shafia P, Kassiri H. A 9.2-g fully-flexible wireless ambulatory EEG monitoring and diagnostics headband with analog motion artifact detection and compensation. IEEE Trans Biomed Circuits Syst. 2019;13(6):1141–51.
Proix T, Truccolo W, Leguia MG, Tcheng TK, King-Stephens D, Rao VR, et al. Forecasting seizure risk in adults with focal epilepsy: a development and validation study. Lancet Neurol. 2021;20(2):127–35.
Brinkmann BH, Karoly PJ, Nurse ES, Dumanis SB, Nasseri M, Viana PF, et al. Seizure diaries and forecasting with wearables: epilepsy monitoring outside the clinic. Front Neurol. 2021;12:690404.
Stirling RE, Cook MJ, Grayden DB, Karoly PJ. Seizure forecasting and cyclic control of seizures. Epilepsia. 2021;62(S1)S2–S14.
Acknowledgements
The authors wish to thank Christopher Stave, MLS Instructional Program Coordinator Lane Medical Library, Stanford Medicine, for his assistance in preparing this manuscript’s search results.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Zachary Davey: none. Pranjal Bodh Gupta: none. David R. Li: none. Rahul Nayak: none. Prasanthi Govindarajan: 7/2019–6/2024, Funder: Agency for Healthcare Research and Quality (R01HS026207-04), Title: Effect of Bypass Policies on Stroke Treatment in a National Sample of Medicare Beneficiaries, Role: PI, 7/2022–6/2023, Funder: Centers for Disease Control and Prevention, Title: Respiratory Virus Transmission Network, Role: Co-Investigator.
Human and Animal Rights and Informed Consent
All reported studies/experiments with human or animal subjects performed by the authors have been previously published and complied with all applicable ethical standards (including the Helsinki declaration and its amendments, institutional/national research committee standards, and international/national/institutional guidelines).
Disclaimer
The views expressed in this article are those of the authors. They do not necessarily reflect the official policy or position of the Department of the Army, Department of Defense, or the US Government.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Zachary Davey and Pranjal Bodh Gupta are shared first authors.
This article is part of the Topical Collection on Critical Care
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Davey, Z., Gupta, P.B., Li, D.R. et al. Rapid Response EEG: Current State and Future Directions. Curr Neurol Neurosci Rep 22, 839–846 (2022). https://doi.org/10.1007/s11910-022-01243-1
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11910-022-01243-1