Abstract
Purpose of Review
Maternal hypertension is a common and serious condition associated with increased maternal and foetal morbidity and mortality, with early detection and management improving outcomes.
Recent Findings
Blood pressure (BP) changes of pre-eclampsia are defined after 20 gestational weeks, while haemodynamic changes can be detected at 5–11 weeks using a specialised non-invasive Doppler stroke volume (SV) monitor. Thus, advanced haemodynamic monitoring allows for physiologically precise identification of circulatory abnormalities, and implementation of appropriate therapy within the first trimester. We measured the oscillometric BP and advanced haemodynamics (USCOM 1A) of 3 unselected women with singleton pregnancies, consecutively listed for therapeutic induction for maternal hypertension at 32–41 weeks gestational age. While the BP’s of the patients varied, it was the haemodynamics, particularly SV, cardiac output, systemic vascular resistance, Smith Madigan Inotropy Index, and oxygen deliver, that identified differing patterns of circulatory dysfunction, therapeutic objectives, and predicted post-partum complications of the mother and child.
Summary
First trimester screening of maternal haemodynamics may allow for earlier detection of circulatory derangements, selection of patient precise interventions, and improved maternal-foetal outcomes.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Hypertension in pregnancy is a common and serious condition associated with significantly increased maternal and foetal morbidity and mortality, as well as increased cost of care [1,2,3,4,5]. While there has been an increasing awareness and focus on maternal hypertension, morbidity and mortality outcomes remain persistently poor despite promotion of widespread blood pressure (BP)-guided management protocols [6•, 7•, 8].
The heart and vessels function to deliver oxygen and substrates to the cells and are regulated by the autonomic nervous system (ANS) and its sensors, predominantly baroreceptors, which act to preserve BP. As Guyton demonstrated, BP is the product of cardiac and vascular function with its interdependence described by the equation [9].
where MAP = mean arterial pressure (mmHg), SVR = systemic vascular resistance (dynes.s.cm-5) SV = stroke volume (mls), HR = heart rate (bpm) and CO = cardiac output (l/min). This distinction of pressure and flow remains incompletely appreciated in the clinical assessment of the circulation and its management, particularly in hypertension. Therefore, in the compensatory or pre-hypertensive phase of circulatory dysfunction, small changes in SV, CO, and SVR can be masked by ANS modulated compensation to baroreceptor determined set points (Table 1). This mathematical coupling ensures that normal BP may mask underlying circulatory dysfunction in the compensated phase. With increasing dysfunction, the compensatory mechanism is exceeded and the BP rises in hypertension and decreases in hypotension (Table 2). However, even in the decompensated or expressed phase, with an elevated BP, the distinction between SV and or SVR dysfunction cannot be resolved and appropriate physiologic targeting of therapies is not possible.
 =increased,
=increased,  =greatly increased,
=greatly increased,  =decreased,
=decreased,  =greatly decreased)
=greatly decreased) =increased,
=increased,  =greatly increased,
=greatly increased,  =decreased,
=decreased,  =greatly decreased)
=greatly decreased)While BP is both a poor surrogate of cardiovascular function and DO2 [10], and a poor guide for therapy, direct measurement of SV and SVR provides objective measures of circulatory dysfunction and identifies physiologic targets for therapy in normotensive and hypertensive subjects.
In normal pregnancy oxygen consumption, VO2 in ml/min is increased, and oxygen delivery, DO2 in ml/min, is upregulated to maintain adequate utero-placental perfusion to support the growing foetus. This upregulation involves general vasodilation, predominantly in the 5th to 16th weeks [11], resulting in a reduced SVR [12], and an increased SV, CO, SMII and DO2. Fluid retention also increases the total blood volume, and the preload and consequently the SV, CO, SMII and DO2. This paradoxic decrease in SVR and increase in SV generally preserves the BP throughout a normal pregnancy, even as DO2 is upregulated [13].
Maternal hypertension is thought to have its pathogenesis in the maladaptation of the spiral arteries in the uterus and placenta leading to failure of normal adaptive vasodilation [12]. This maladaptation results in a relatively increased maternal SVR and a compensatory decrease in SV, CO, DO2 and SMII, resulting in relative placental-foetal hypoxia. Tiralongo observed that “As the normal maternal hemodynamic adaptation to pregnancy is an increase in SV, CO and SMII, accompanied by a reduced SVR, it is unsurprising that a decreased SV, CO and SMII and an accompanying increase in SVR results in poor maternal-fetal outcomes” [14••].
The range of normal maternal haemodynamics varies considerably throughout pregnancy [15, 16], with obesity [17, 18], and with the degree and origin of any dysfunction, and in response to ANS compensation [15, 19••, 20, 21]. This creates a moving target for therapy and limits the potential for simple protocolised interventions, an observation supported by the relative ineffectiveness of current BP-guided therapeutic guidelines [6•, 7•, 8]. A shift to physiologic, patient precise therapy is necessary to improve the effectiveness of maternal hypertension management.
Hypertension is treated by reducing CO, SVR or both. CO is reduced by reducing preload, and thus SV, with a diuretic, and/or, by reducing HR and myocyte contractility, or by decreasing SVR using a vasodilator (Fig. 1) [6•]. Therefore, direct measurement of the SV and SVR is essential for early detection of circulatory dysregulation and appropriate choice of, and monitoring of, therapeutic interventions, particularly in the early latent or compensated phase of hypertension.
Relationship of BP, and the haemodynamic variables of SV and SVR [9], demonstrating the direct (continuous lines) and ANS-regulated (dashed lines) action of antihypertensive therapies. Hypertensive therapies do not act directly on BP
The non-invasive USCOM 1A Doppler monitor (Uscom Limited, Sydney Australia) has recently been validated for advanced point of care monitoring of haemodynamics in pregnancy [22,23,24]. The device directly measures transvalvular ventriculoarterial blood flow and generates beat to beat measures of SV, CO, SVR, SMII and DO2, plus 20 additional advanced haemodynamic parameters [25]. SMII is a novel measure of ventricular inotropy based on quantitation of the potential and kinetic energy of the circulation indexed to the time of ventricular ejection [26] and is an improved index of total cardiovascular load in W/m2. The USCOM 1A has been proven to be reliable, reproducible and more sensitive than bio-impedance [18, 27••, 28•, 29], and more feasible to use than echocardiography [27••], with measurements acquired in a few minutes [14••]. Established normal haemodynamic reference values across pregnancy [14••, 19••] and a high sensitivity to SV change ensure early detection of circulatory dysregulation and accurate identification of appropriate therapy and monitoring of therapeutic response. Using this method, Tiralonga et al. identified the haemodynamic changes of pre-eclampsia at 5 to 11 weeks [14••], while Valensise et al. demonstrated that a low CO and high SVR, > 1069 dynes s cm−5, at the end of pregnancy are associated with higher risks of foetal distress and maternal complications [30] and preterm delivery [21]. Tiralonga also demonstrated that 2 weeks of treatment of women with maternal hypertension and foetal growth restriction using NO donors and volume expansion at 30 weeks gestational age significantly changed SV, CO and SVR and improved maternal and foetal outcomes [31••]. While the diagnostic criteria for pre-eclampsia is a BP > 140/90 after twenty gestational weeks [6•, 7•], the adoption of normal haemodynamic reference values is more intuitive and may provide diagnostic and therapeutic guidance at 5–11 weeks, and therefore improve outcomes [20, 31•, 32, 33].
Maternal hypertension is often treated with induction and Caesarean section [6•], which may increase risks in consecutive pregnancies [34]. Early detection of maternal hypertension and precision management may facilitate earlier and improved management and reduce the incidence of these interventions, reducing risks in first and successive pregnancies.
The monitoring of maternal haemodynamics has demonstrated promising results for the early identification and patient precise targeting of treatment of maternal hypertension [31•, 35, 36, 37•]. We present a series of three consecutive case studies to demonstrate the principles supporting this promising and rapidly evolving clinical approach to maternal hypertension.
Method
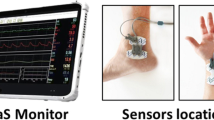
Contemporaneously measured BP and Doppler SV haemodynamic examinations were performed on three randomly selected women with singleton pregnancies at 32 to 41 weeks gestational age following informed consent. Participants were consecutively listed for therapeutic induction for maternal hypertension in the 24 h following testing at a maternal tertiary referral centre in a Chinese provincial hospital. Maternal haemodynamics were measured using the USCOM 1A MATERNAL haemodynamic monitor (Uscom Limited, Sydney, Australia) and BP measures acquired using routine brachial oscillometry (Omron, Japan), with all measures acquired 5 min following the subjects placed in the supine resting position. The BP and USCOM haemodynamic measures were collated and compared. Normal values for pregnant haemodynamics were referenced from Vinayagam et al. [19••]. Grading of maternal hypertension was according to the NICE guidelines (mild hypertension 140–149/90–99 mmHg, moderate hypertension 150–159/100–109 mmHg, and severe hypertension > 160/110 mmHg [6•]). Clinical observations and maternal and foetal outcomes post partum were assessed.
Findings
Case 1
Normal adaptive circulation
Thirty-two-year-old (160 cm, 75Kg, BSA 1.87 m2) with a normal BP of 119/65, MAP 83, and one prior normal pregnancy with mild late term hypertension, for induction under anaesthesia at 41 weeks
Normal vaginal delivery of a 4130-g baby at 41 weeks gestational age with an Apgar of 10. Returned from the ICU 1 day post parturition
Summary—Normal adaptive haemodynamics with increased SV, CO, DO2 and SMII, with decreased SVR, and upregulated DO2 to meet increased VO2 of pregnancy (Fig. 2). Physiologically guided therapy—non-intervention with normal serial haemodynamic monitoring.
Outcome: uneventful birth and outcome.
Case 2
Mild cardiogenic hypertension
Thirty-three-year-old (155 cm, 60.5Kg, BSA 1.65 m2, AV OTD 1.80) presenting with mild hypertension, 137/92 and MAP 107 mmHg and a history of one prior pregnancy complicated by mild hypertension. For planned induction at 36 weeks.
Normal vaginal delivery of a 2780-g baby at 32 gestational weeks with an Apgar score of 8. Mother and baby recovered quickly with an overnight observational ICU stay.
Summary—Mild cardiogenic hypertension (137/92 and MAP 107 mmHg) with moderately elevated SV, CO, HR, SMII and DO2, with a mildly decreased SVR (Fig. 3). To maintain the increased output, the cardiovascular system is overloaded despite a low normal SVR. Physiologically guided therapy would have targeted at reducing the SV using a diuretic. Outcome—At birth, the baby had a slightly decreased APGAR which quickly resolved, and both mother and child recovered after 24 h ICU observation.
Case 3
Severe vasogenic hypertension with severely impaired cardiac function.
A 33-year-old obese mother (162 cm, 95.5 kg, BSA 2.14 m2) with 3 prior pregnancy’s complicated by moderate hypertension, presented at 32 weeks gestational age with severe hypertension, BP 165/95 (MAP = 118) and increasing oedema and leg pitting. The patient was scheduled for a therapeutic induction at 32 weeks gestational age.
Caesarean section delivered small for dates baby, 1550 g at 32 weeks gestational age with an Apgar score at 1 min of 9, at 5 min 7, and at 10 min 9, followed by a 3-day ICU stay.
Summary—Severe vasogenic hypertension, with a severely elevated SVR (2332 v normal 1100 dyne s cm−5). Additionally, there was severe impairment of the SV (46 v normal 79 ml), CO (4 v 6.9 L/min), SMII (1.1 v 2.0 W/m2) and, importantly, DO2 was approximately 60% of normal (594 v 900 ml/m2) (Fig. 4).
Case 3 aortic CO profile demonstrating severe vasogenic hypertension, with a severely elevated SVR, 2332 dyne s cm−5 (Normal 800–1000 dyne s cm−5), and severe impairment of SV of 46 ml (> 79 ml normal), CO of 3.5 L/min (normal 7–8 L/min) and SMII of 1.1 W/m2 (normal 1.1–2 W/m2), while DO2 was severely impaired, delivering approximately 60% of normal (594 v 900 ml/m2)
Physiologically guided therapy would have targeted reducing the SVR with a vasodilator, and an inotrope to stimulate the LV function.
Outcome—The baby, after Caesarean birth, had a depressed 5 point APGAR score, which recovered over the first hour, while the mother required 3 days of ICU care. It is probable that this significant haemodynamic dysfunction would have been expressed in the first trimester and would have been detected by haemodynamic monitoring. This may have led to improved physiologically targeted management and a more stable haemodynamic course through pregnancy and improved outcome.
Advanced Haemodynamics
Table 3 allows comparison of haemodynamic values in the 3 hypertensive subjects with normal values. Plotting MAP, SV, CO, SVR, SMII and DO2 for normal and hypertensive subjects (Figs. 5, 6, 7, 8, 9 and 10), demonstrates a unique haemodynamic pattern for each subject, and each parameter, and therefore a unique therapeutic approach. Neither SV, CO, SVR, SMII nor DO2, the therapeutic targets, correlated with MAP, the current method of defining and guiding therapy in maternal hypertension.
Normal reference MAP, normotensive pregnancy (Exam 1), mild hypertension (Exam 2) and severe hypertensive (Exam 3) [19••]
Normal SV, normal SV (Exam 1), mildly elevated SV in mild cardiogenic hypertension (Exam 2), and severe SV impairment, 2° to severely increased SVR in severe vasogenic hypertension (Exam 3) [19••]
Normal CO, normal CO (Exam 1), mild to moderately elevated CO with mild cardiogenic hypertension (Exam 2) and severely impaired CO in severe vasogenic hypertension (Exam 3) [19••]
Normal reference SVR, low normal SVR in normal and mild cardiogenic hypertension (exams 1 and 2) and severely elevated in severe vasogenic hypertension (Exam 3) [19••]
Normal reference DO2 in pregnancy, high normal DO2 in normal upregulation (exam 1), moderately increased DO2 in mild cardiogenic hypertension (Exam 2) and severely reduced DO2 in severe vasogenic hypertension (Exam 3) [19••]
Normal reference SMII, low normal SMII in normal upregulated pregnancy (Exam 1), moderately increased SMII to deliver a 50% increased DO2 in mild cardiogenic hypertension (Exam2), and moderately reduced SMII in severe vasogenic hypertension (Exam 3) [19••]
Discussion
These three case studies of third trimester hypertensive pregnant subjects demonstrate the variability and unpredictability of maternal outcomes by BP, while abnormal haemodynamics more closely predicted outcomes (Table 1). Advanced haemodynamic monitoring of maternal circulation provided pathophysiologic understanding that was not provided by BP monitoring alone. The mathematical coupling of, and physiologic interdependence of, BP and cardiovascular function explains the systematic inadequacy of BP alone for guidance and management of maternal hypertension. First trimester haemodynamic monitoring may improve our understanding of the development of deranged maternal circulation, and the complex interaction of SV, CO, SVR, DO2 and SMII and their impact on maternal-foetal outcomes. This improved understanding may allow for early implementation of patient precise therapy.
Limitations
This observational study demonstrates the simple principles and application of advanced haemodynamic monitoring in identifying and managing maternal hypertension but is limited in its scope. Study of more subjects, randomised across a range of BPs, is required to better define the potential benefits of this physiologically guided approach. Further study of the temporal evolution of normal and pathological maternal haemodynamics may identify new personalised therapeutic approaches to its management and establish the utility of a routine first trimester scan.
Conclusion
Advanced haemodynamic monitoring in pregnancy provides identification of circulatory pathophysiology at 5 to 11 weeks, and defines quantitative therapeutic targets not identified by BP alone. First trimester screening of SV, CO, SVR, SMII and DO2 may lead to an earlier and more accurate diagnosis, more precise therapy and improved outcomes in maternal hypertension.
Change history
24 August 2020
The original publication of this article, unfortunately, contains the following errors.
Abbreviations
- BP:
-
blood pressure in mmHg
- MAP:
-
mean arterial pressure in mmHg
- SV:
-
stroke volume in ml
- CO:
-
cardiac output in l/min
- SVR:
-
systemic vascular resistance in dyne s cm−5
- HR:
-
heart rate in beats/min
- DO2 :
-
oxygen delivery in ml/min
- VO2:
-
oxygen consumption in ml/min
- SMII:
-
Smith Madigan Inotropy Index in W/m2
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Khan KS, Wojdyla D, Say L, Gulmezoglu AM, Van Look PFA. WHO analysis of causes of maternal death: a systematic review. Lancet. 2006;367(9516):1066–74.
Abalos E, Cuesta C, Grosso AL, Chou D, Say L. Global and regional estimates of preeclampsia and eclampsia: a systematic review. Eur J Obstet Gynecol Reprod Biol. 2013;170(1):1–7.
Mackay AP, Berg CJ, Atrash HK. Pregnancy-related mortality from preeclampsia and eclampsia. Obstet Gynecol. 2001;97(4):533–8.
Mangham LJ, Petrou S, Doyle LW, Draper ES, Marlow N. The cost of preterm birth throughout childhood in England and Wales. Pediatrics. 2009;123(2):e312–27.
von Dadelszen P, Payne B, Li J, PIERS Study Group, et al. Prediction of adverse maternal outcomes in pre-eclampsia: development and validation of the fullPIERS model. Lancet. 2011;377:219–27.
• Visintin C, Mugglestone MA, Almerie MQ, Nherera LM, James D, Walkinshaw S, et al. Management of hypertensive disorders during pregnancy: summary of NICE guidance. Brit Med J. 2010;341:499–502. https://doi.org/10.1136/bmj.c2207. UK Guidelines for definition and management of hypertension in pregnancy.
• Roberts JM, August PA, Bakris G, for the task force on hypertension in pregnancy, et al. Hypertension in Pregnancy. Am Coll Obstetricians and Gynaecologists. 2013;122:1122–31. US Guidelines for definition and management of hypertension in pregnancy.
Gillon TER, Pels A, von Dadekszen P, Macdonell K, Magee LA. Hypertensive disorders of pregnancy: a systematic review of international clinical practice guidelines. PLoS One. 2014;9(12):e113715. https://doi.org/10.1371/journal.pone.0113715.
Guyton AC, Lindsey AW, Kaufmann BN. Effect of mean circulatory filling pressure and other peripheral circulatory factors on cardiac output. Am J Phys. 1955;180:463468.
Wo CCJ, Shoemaker WC, Appel PL, Bishop MH, Kram HB, Hardin E. Unreliability of blood pressure and heart rate to evaluate cardiac output in emergency resuscitation and critical illness. Crit Care Med. 1993;21:218–23.
Bosio PM, Mc Kenna PJ, Conroy R, O’Herlihy C. Maternal central hemodynamics in hypertensive disorders of pregnancy. Obstet Gynecol. 1999;94:978–84.
Phipps E, Prasanna D, Brima W, Jim B. Preeclampsia: updates in pathogenesis, definitions, and guidelines. Clin J Am Soc Nephrol. 2016;11:1102–13. https://doi.org/10.2215/CJN.12081115.
Reddy M, Kroushev, Palmer K, Rolnik D, Da Silva Costa F. Fetal growth restriction – Ch 15 maternal cardiovascular involvement. https://doi.org/10.1007/978-3-030-00051-6_15.
•• Tiralongo GM, Lo Presti D, Pisani I, Gagliardi G, Scala RL, Novelli GP, et al. Assessment of total vascular resistance and total body water in normotensive women during the first trimester of pregnancy. A key for the prevention of preeclampsia. Pregnancy Hypertens. 2015. https://doi.org/10.1016/j.preghy.2015.02.001. This study demonstrates that USCOM 1A advanced haemodynamics detects circulatory abnormalities at 5–11 weeks gestational age supporting the adoption of first trimester monitoring and intervention.
Khalil A. Maternal systemic circulation in normotensive pregnancies and those complicated by pre-eclampsia. J Preg Hypertension. 2015;5(22-OR):11. https://doi.org/10.1016/j.preghy.2014.10.026.
Lihme F, Persson L, Basit S, Lykke JA, Pihl K, Halse K, et al. Comparison of cardiac function parameters measured longitudinally in pregnancies with late-onset preeclampsia and normotensive pregnancies. Pregnancy Hypertens. 2017;9:49. https://doi.org/10.1016/j.preghy.2017.07.105.
Teoh W., Nagarajan S. Ultrasonic Doppler measurements and maternal cardiac output indices of morbidly obese term parturients differ from the non-obese. Eur J Anaesthesiol. 2014;31:e-Supplement 52(11 AP2–10).
Pisani I, Tiralongo GM, Lo Presti D, Gagliardi G, Farsetti D, Vasapollo B, et al. Correlation between maternal body composition and haemodynamic changes in pregnancy: different profiles for different hypertensive disorders. Pregnancy Hypertens. 2017;10:131–4.
•• Vinayagam D, Thilaganathan B, Stirrup O, Mantovani E, Khalil A. Maternal hemodynamics in normal pregnancy: reference ranges and the role of maternal characteristics. Ultrasound Obstet Gynecol. 2017. https://doi.org/10.1002/uog.17504. All gestational age normal multi-parametric haemodynamic reference values for pregnancy derived from 627 normal singleton pregnancies.
Valensise H, Vasapollo B, Gagliardi G, Novelli GP. Early and late preeclampsia. Two different maternal hemodynamic states in the latent phase of the disease. Hypertension. 2008 Nov;52(5):873–80.
Valensise H, Faresetti D, Prestia DL, Pisani LO, Tiralongo GM, Gagliardia G, et al. Preterm delivery and elevated maternal total vascular resistance: signs of suboptimal cardiovascular adaptation to pregnancy. Ultrasound Obstet Gynecol. 2016;48:491–5. https://doi.org/10.10012/uog.15910.
van der Graf AM, Zeeman GG, Groen H, Roberts C, Dekker GA. Non-invasive assessment of maternal haemodynamics in early pregnancy. Pregnancy Hypertens. 2013;3:261–9.
McNamara H, Barclay P, Sharma V. Accuracy and precision of the ultrasound cardiac output monitor (USCOM 1A) in pregnancy: comparison with three-dimensional transthoracic echocardiography. Br J Anaesth. 2014;113:669–76. https://doi.org/10.1093/bja/aeu162.
Vinayagam D, Patey O, Thilaganathan B, Khalil A. Cardiac output assessment in pregnancy: comparison of two automated monitors with echocardiography. Ultrasound Obstet Gynecol. 2017;49(1):32–8. https://doi.org/10.1002/uog.15915.
Phillips RA, Smith BE, Madigan VM. Stroke volume monitoring: novel continuous wave Doppler parameters, algorithms and advanced noninvasive haemodynamic concepts. Curr Anesthesiol Rep. 2017;7:387–98. https://doi.org/10.1007/s40140-017-0235-4.
Smith BE, Madigan VM. Non-invasive method for rapid bedside estimation of inotropy: theory and preliminary clinical validation. Br J Anaesth. 2013;111(4):580–8. https://doi.org/10.1093/bja/aet118.
•• Smith BE, Madigan VM. Understanding the haemodynamics of hypertension. Curr Hypertens Rep. 2018;20:29. https://doi.org/10.1007/s11906-018-0832-8. This review demonstrates the relationship of advanced haemodynamics, hypertension and therapy.
• van der Graaf AM, Zeeman GG, Groen H, Lumbers ER, Roberts C, Dekker GA. Noninvasive assessment of hemodynamics in early pregnancy. Pregnancy Hypertens. 2011;1(3–4):264. This study validates and proves feasibility of non-invasive USCOM 1A monitoring in pregnancy.
Kager CCM, Dekker GA, Stam MC. Measurement of cardiac output in normal pregnancy by a non-invasive two-dimensional independent Doppler device. Aust N Z J Obstet Gynaecol. 2009;49:142–4. https://doi.org/10.1111/j.1479-828X.2009.00948.x.
Valensise H, Tiralongo GM, Pisani D, Farsetti D, LoPresti D, Gagliardi G, et al. Maternal cardiac output in early labour: a possible link with obstetrics risks? Ultrasound Obstet Gynecol. 2017;51:514–8. https://doi.org/10.1002/uog.17454.
• Tiralongo G, Pisani I, Vasapollo B, Khalil A, Thilaganathan B, Valensise H. Nitric oxide (NO) donors and haemodynamic changes in fetal growth restriction. Ultrasound Obstet Gynecol. 2017. https://doi.org/10.1002/uog.17454. This study demonstrates that nitric oxide therapy at 30 weeks improves haemoydnamics and outcomes in hypertensive pregnancies.
States U. Diagnosis and management of preeclampsia and eclampsia. Int J Gynecol Obstet. 2002;77(1):67–75.
Nardozza L, et al. (eds.). Fetal growth restriction, Ch 15, Reddy M, Kroushev, Palmer K, Rolnik D, Da Silva Costa F. Maternal cardiovascular involvement. 2019. https://doi.org/10.1007/978-3-030-00051-6_15.
Nisenblat V, Shlomi B, Griness OB, Barnett O, Degani S, Ohel G, et al. Maternal complications associated with multiple cesarean deliveries. Obstet Gynaecol. 2006;108(1):21–6. https://doi.org/10.1097/01.AOG.0000222380.11069.11.
Ali W, Bakris G. The management of hypertension in 2018: what should the targets be? Curr Hypertens Rep. 2019;21:4. https://doi.org/10.1007/s11906-019-0946-7.
Vonck S, Staelens VS, Bollen I, Broekx L, Gyselaers W. Why non-invasive maternal hemodynamics assessment is clinically relevant in early pregnancy: a literature review. BMC Pregnancy Childbirth. 2016;16:302. https://doi.org/10.1186/s12884-016-1091-9.
• Khalil A, Perry H, Bowe S, Thilaganathan B. The interaction between the maternal systemic and uteroplacental circulations in pregnancies resulting in small for gestational age newborns. Pregnancy Hypertens. 2017;9(4–7 9):22. https://doi.org/10.1016/j.preghy.2017.07.052. This study establishes the relationship between circulation, hypertension and small for gestation newborns.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Dr. Phillips is a shareholder and employee of Uscom Limited. All the other authors have no interests to declare.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Preeclampsia
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Phillips, R.A., Ma, Z., Kong, B. et al. Maternal Hypertension, Advanced Doppler Haemodynamics and Therapeutic Precision: Principles and Illustrative Cases. Curr Hypertens Rep 22, 49 (2020). https://doi.org/10.1007/s11906-020-01060-2
Published:
DOI: https://doi.org/10.1007/s11906-020-01060-2