Abstract
Purpose of Review
Type 2 diabetes mellitus (DM) is a major risk factor for the development of heart failure (HF). In patients with DM, preventing HF using diabetes medications should be an imperative for primary care physicians and cardiologists alike.
Recent Findings
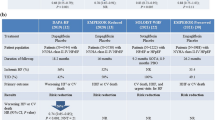
Prior studies with DPP-IV inhibitors, thiazolidinediones (TZDs), and GLP-1 agonists have demonstrated either a neutral effect on HF or increased HF hospitalizations. Two recent large-scale randomized controlled trials (RCTs), EMPA-REG OUTCOME and CANVAS, compared sodium glucose transporter-2 inhibitor (SGLT-2i) to placebo. Use of SGLT-2i led to a substantial reduction in HF events and hospitalizations in patients with DM, with or without history of HF.
Summary
Use of SGLT-2i therapy has been shown to reduce HF in patients with DM.
Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
CDC National Diabetes Statistics Report, 2017: Estimates of Diabetes and its Burden in the United States. https://www.cdc.gov/diabetes/pdfs/data/statistics/national-diabetes-statistics-report.pdf
Moss SE, Klein R, Klein BE. Cause-specific mortality in a population-based study of diabetes. Am J Public Health. 1991;81:1158–62.
McMurray JJV, Gerstein HC, Holman RR, Pfeffer MA. Heart failure: a cardiovascular outcome in diabetes that can no longer be ignored. Lancet Diabetes Endocrinol. 2014;2:843–51.
Kannel WB, McGee DL. Diabetes and cardiovascular disease: the Framingham study. JAMA. 1979;241:2035–8.
Nichols GA, Gullion CM, Koro CE, et al. The incidence of congestive heart failure in type 2 diabetes. Diabetes Care. 2004;27(8):1879–84.
Iribarren C, Karter AJ, Go AS, et al. Glycemic control and heart failure among adult patients with diabetes. Circulation. 2001;103:2668–73.
Bertoni AG, Hundley WG, Massing MW, et al. Heart failure prevalence, incidence, and mortality in the elderly with diabetes. Diabetes Care. 2004;27(3):699–703.
Gustafsson I, Brendorp B, Seibaek M, et al. Influence of diabetes and diabetes-gender interaction on the risk of death in patients hospitalized with congestive heart failure. JACC. 2004;43:771–7.
Carr AA, Kowey PR, Devereux RB, et al. Hospitalizations for new heart failure among subjects with diabetes mellitus in the RENAAL and LIFE studies. Am J Cardiol. 2005;96:1530–6.
American Diabetes Association. Cardiovascular disease and risk management: standards of medical care in diabetes-2018. Diabetes Care. 2018;41(Suppl 1):S86–S104. https://doi.org/10.2337/dc18-S009.
The Look AHEAD Research Group. Cardiovascular effects of intensive lifestyle intervention in type 2 diabetes. N Engl J Med. 2013;369:145–54.
Gaede P, Vedel P, Larsen N, et al. Multifactorial intervention and cardiovascular disease in patients with type 2 diabetes. N Eng J Med. 2003;348:383–93.
Oellgaard J, Gaede P, Rossing P, et al. Reduced risk of heart failure with intensified multifactorial intervention in individuals with type 2 diabetes and microalbuminuria: 21 years of follow-up in the randomized Steno-2 study. Diabetologia. 2018;61:1724–33.
UK Prospective Diabetes Study Group. Tight blood pressure control and risk of macrovascular and microvascular complications in type 2 diabetes: UKPDS 38. BMJ. 1998;317:703–13.
Whelton PK, Carey RM, Aronow WS, et al. ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA guideline for the prevention, detection, evaluation, and management of high blood pressure in adults: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines [published online November 13, 2017]. Hypertension. https://doi.org/10.1161/HYP.0000000000000065.
HOPE Study Investigators. Effects of ramipril on cardiovascular and microvascular outcomes in patients with diabetes mellitus: results of the HOPE study and Micro-HOPE substudy. Lancet. 2000;355:253–9.
Stone NJ, Robinson JG, Lichtenstein AH, et al. 2013 ACC/AHA guideline on the treatment of blood cholesterol to reduce atherosclerotic cardiovascular risk in adults: a report of the American college of cardiology/American heart association task force on practice guidelines. Circulation. 2014;129:S1–45.
Preiss D, Campbell RT, Murray HM, et al. The effect of statin therapy on heart failure events: collaborative meta-analysis of unpublished data from major randomized trials. Eur Heart J. 2015;36:1536–46.
Turnbull FM, Abraira C, Anderson RJ, et al. Intesive glucose control and macrovascular outcomes in type 2 diabetes. Diabetologia. 2009;52:2288–98.
Turner, R for the UKPDS group. Effect of intensive blood glucose control with metformin on complications in overweight patients with type 2 diabetes (UKPDS 34). Lancet. 1998;352:854–65.
Boussageon R, Supper I, Bejan-Angoulvant T, et al. Reappraisal of Metformin Efficacy in the Treatment of Type 2 Diabetes: A Meta-Analysis of Randomized Controlled Trials. PLoS Med. 2012;9(4):e1001204.
Tzoulaki I, Molokhia M, Curcin V, et al. Risk of cardiovascular disease and all cause mortality among patients with type 2 diabetes prescribed oral antidiabetes drugs: retrospective cohort study using UK general practice research database. BMJ. 2009;339:b4731.
UK Prospective Diabetes Study (UKPDS) Group. Intensive blood-glucose control with sulphonylureas or insulin compared with conventional treatment and risk of complications in patients with type 2 diabetes (UKPDS 33). Lancet. 1998;352:837–53.
Patel A, MacMahon S, Chalmers J, et al. Intensive blood glucose control and vascular outcomes in patients with type 2 diabetes. N Eng J Med. 2008;358:2560–72.
Gerstein HC, Miller ME, Byington RP, et al. Effect of intensive glucose lowering in type 2 diabetes. N Eng J Med. 2008;358:2545–59.
Dormandy JA, Charbonnel B, Eckland DJA, et al. Secondary prevention of macrovascular events in patients with type 2 diabetes in the PROactive study (Prospective pioglitazone clinical trial in macrovascular events): a randomized controlled trial. Lancet. 2005;366:1279–89.
Home PD, Pocock SJ, Beck-Nielsen H, et al. Rosiglitazone evaluated for cardiovascular outcomes in oral agent combination therapy for type 2 diabetes (RECORD): a multicentre, randomized, open label trial. Lancet. 2009;373:2125–35.
Gerstein HC, Bosch J, Dagenais GR, et al. Basal insulin and cardiovascular and other outcomes in dysglycemia. N Engl J Med. 2012;367:319–28.
Gerstein HC, Jung H, Ryden L, et al. Effect of Basal Insulin Glargine on First and Recurrent Episodes of Heart Failure Hospitalization: the ORIGIN trial. Circulation. 2018;137:88–90.
Scirica BM, Bhatt DL, Braunwald E, et al. Saxagliptin and cardiovascular outcomes in type 2 diabetes mellitus. N Engl J Med. 2013;369:1317–26.
White WB, Cannon CP, Heller SR, et al. Alogliptin after acute coronary syndrome in patients with type 2 diabetes. N Eng J Med. 2013;369:1327–35.
Zannad F, Cannon CP, Cushman WC, et al. Heart failure and mortality outcomes in patients with type 2 diabetes taking aloglipitin versus placebo in EXAMINE: a multicentre, randomized, double-blind trial. Lancet. 2015;385:2067–76.
Green JB, Bethel A, Armstrong PW, et al. Effect of sitagliptin on cardiovascular outcomes in type 2 diabetes. N Engl J Med. 2015;373:232–42.
Pfeffer MA, Claggett B, Diaz R, et al. Lixisenatide in patients with type 2 diabetes and acute coronary syndrome. N Engl J Med. 2015;373:2247–57.
Marso SP, Daniels GH, Brown-Frandsen K, et al. Liraglutide and cardiovascular outcomes in type 2 diabetes. N Eng J Med. 2016;375:311–22.
Marso SP, Bain SC, Consoli A, et al. Semaglutide and Cardiovascular Outcomes in Patients with Type 2 Diabetes. N Engl J Med. 2016;375:1834–44.
Holman RR, Bethel MA, Mentz RJ, et al. Effects of once-weekly exenatide on cardiovascular outcomes in type 2 diabetes. N Engl J Med. 2017;377:1228–39.
Abdul-Ghani MA, Norton L, DeFranzo RA. Efficacy and safety of SGLT2 inhibitors in the treatment of type 2 diabetes mellitus. Curr Diab Rep. 2012;12:230–8.
Heise T, Seewaldt-Becker E, Macha S, et al. Safety, tolerability, pharmacokinetics and pharmacodynamics following 4 weeks’ treatment with empagliflozin once daily in patients with type 2 diabetes. Diabetes Obes Metab. 2013;15:613–21.
Lytvyn Y, Bjornstad P, Udell JA, et al. SGLT2 Inhibitors in Heart Failure: potential mechanisms, clinical applications, and summary of clinical trials. Circulation. 2017;136:1643–58.
Baker WL, Smyth LR, Riche DM, et al. Effects of sodium-glucose co-transporter 2 inhibitors on blood pressure: a systematic review and meta-analysis. J Am Soc Hypertens. 2014;8:262–75.e9.
•• Zinman B, Wanner C, Lachin JM, et al. Empagliflozin, Cardiovascular Outcomes, and Mortality in Type 2 Diabetes. N Engl J Med. 2015;373:2117–28. https://doi.org/10.1056/NEJMoa1504720. The first randomized trial of an antidiabetic agent (the SGLT-2i empagliflozin) to demonstrate a meaningful reduction in HF
Kaul S. Mitigating Cardiovascular Risk in Type 2 Diabetes With Antidiabetes Drugs: A Review of Principal Cardiovascular Outcome Results of EMPA-REG OUTCOME, LEADER, and SUSTAIN-6 Trials. Diabetes Care. 2017;40(7):821–31.
Jessup M. Neprilysin inhibition – a novel therapy for heart failure. N Engl J Med. 2014;371:1062–4.
• Neal B, Perkovic V, Mahaffey K, et al. Canagliflozin and Cardiovascular and Renal Events in Type 2 Diabetes. N Engl J Med. 2017;377:644–57. Landmark trial showing reduction in HF with use of SGLT-2i canagliflozin
• Zheng SL, Roddick AJ, Aghar-Jaffar R, et al. Association between use of sodium-glucose cotransporter 2 inhibitors, glucagon-like peptide 1 agonists, and dipeptidyl peptidase 4 inhibitors with all-cause mortality in patients with type 2 diabetes: a systematic review and meta-analysis. JAMA. 2018;319(15):1580–91. A comprehensive meta-analysis of antidiabetic medications, showing superiority of SGLT-2i on HF outcomes
Kosiborod M, Cavender MA, Fu AZ. Lower risk of heart failure and death in patients initiated on sodium-glucose cotransporter-2 inhibitors versus other glucose-lowering drugs: the CVD-REAL study. Circulation. 2017;136:249–59.
Birkeland KI, Jorgensen ME, Carstensen B, et al. Cardiovascular mortality and morbidity in patients with type 2 diabetes following initiation of sodium-glucose co-transporter-2 inhibitors versus other glucose-lowering drugs (CVD-REAL Nordic): a multinational observational analysis. Lancet Diabetes Endocrinol. 2017;5(9):709–17.
Kosiborod M, Lam CSP, Kohsaka S, on behalf of the CVD-REAL Investigators and Study Group, et al. Lower Cardiovascular Risk Associated with SGLT-2i in >400,000 Patients: The CVD-REAL 2 Study. JACC. 2018; https://doi.org/10.1016/j.jacc.2018.03.009.
Cooper HA, Dries DL, Davis CE, et al. Diuretics and risk of arrhythmic death in patients with left ventricular dysfunction. Circulation. 1999;100:1311–5.
Packer M, Anker SD, Butler J, et al. Effects of sodium-glucose cotransporter 2 inhibitors for the treatment of patients with heart failure. JAMA Cardiology. 2017;2(9):1025–9.
Lytvyn Y, Bjornstad P, Udell JA. Sodium glucose cotransporter-2 inhibition in heart failure: potential mechanisms, clinical applications, and summary of clinical trials. Circulation. 2017;136:1643–58.
Wiviott SD, Raz I, Bonaca MP, et al. The design and rationale for the dapagliflozin effect on cardiovascular events (DECLARE)-TIMI 58 trial. Am Heart J. 2018;200:83–9.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Nikhil Bassi reports no relevant disclosures.
Gregg C. Fonarow reports significant consulting for Novartis, and modest consulting for Amgen, Bayer, Gambro, Medtronic, St. Jude, and Janssen, and research funding from the NIH. Dr. Fonarow holds the Eliot Corday Chair of Cardiovascular Medicine at UCLA and is also supported by the Ahmanson Foundation (Los Angeles, California).
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Diabetes and Cardiovascular Disease
Rights and permissions
About this article
Cite this article
Bassi, N., Fonarow, G.C. Prevention of Heart Failure in Patients with Diabetes: Role of Diabetes Medications. Curr Cardiol Rep 20, 112 (2018). https://doi.org/10.1007/s11886-018-1050-3
Published:
DOI: https://doi.org/10.1007/s11886-018-1050-3