Abstract
Purpose of Review
The current article aims to provide a comprehensive update on diagnostic criteria for mast cell activation syndrome (MCAS), addressing challenges in diagnosing and classifying MCAS and its variants.
Recent Findings
In recent years, there has been a significant increase in our knowledge regarding the underlying mechanisms responsible for the activation of mast cells (MCs) in various pathological conditions. Furthermore, a set of criteria and a classification for MCASs have been established. MCAS is characterized by the presence of typical clinical symptoms, a substantial elevation in serum tryptase levels during an attack compared to the patient’s baseline tryptase levels, and a response to MC mediator–targeting therapy.
Summary
In this report, a thorough examination was conducted on the contemporary literature relating to MCAS, with a focus on comparing the specificity, sensitivity, and robustness of MCAS-related parameters within proposals for diagnosing and classifying MCAS and its variants. Moreover, the significance of employing specific consensus criteria in the assessment and categorization of MCAS in individual patients was underscored, due to the escalating occurrence of patients receiving a misdiagnosis of MCAS based on nonspecific criteria.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
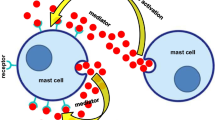
Mast cells (MCs) are granulated, multifunctional immune cells with diverse functions [1]. They can adjust their responses, depending on the stimulus encountered and the tissue in which they are stimulated [1,2,3,4]. MCs can be activated by various mechanisms, but the most common one is through the cross-linking of immunoglobulin E (IgE) molecules bound to the surface by high-affinity FcεRI receptors [5,6,7,8]. Other mechanisms that can activate MCs include the activation of surface G protein–coupled receptors such as Toll-like receptors, complement receptors C3a and C5a, and mas-related G protein receptor (MRGPRX2) [9]. When MCs are activated, they release biologically active mediators and the role of these substances in the clinical symptoms of MC disorders is heterogeneous [1,2,3,4,5,6,7,8,9,10].
The severity of symptoms related to MC activation can vary from mild to severe and even life-threatening. Furthermore, these symptoms can be either acute or chronic in nature. Acute MC activation is commonly observed in allergic reactions and can manifest as localized events specific to the affected tissue or as systemic symptoms resulting from widespread MC activation [10, 11]. Examples of tissue-specific consequences of MC activation include urticaria, allergic rhinitis, or asthma, and the symptoms, in most instances, are limited to the area of the interaction with the trigger. However, there are also instances where generalized tissue-specific symptoms occur, as seen in chronic idiopathic urticaria. Systemic activation of MCs encompasses the conditions of anaphylaxis and MC activation syndrome (MCAS) [12,13,14]. Furthermore, severe or even life-threatening MC activation–related events may occur when MCs are in a “hyperreactive” state and/or the burden of MC is high, as in patients with mastocytosis [15•, 16•].
The purpose of the current article is to provide a clear understanding of the main challenges encountered when diagnosing and classifying MCAS and its variations.
Mast Cell Activation Syndrome
Definition
Mast cell activation syndrome (MCAS) is an uncommon disorder denoted by periodic sudden-onset episodes of severe systemic symptoms, encompassing an array of disorders with multiple etiologies, whether clonal or non-clonal. These symptoms are directly associated with the excessive release of MC mediators and in most cases the episodes present as anaphylaxis [14, 15•, 16•]. MCAS is considered to be part of the spectrum of MC disorders, along with anaphylaxis and mastocytosis. However, it is important to note that while these conditions are interrelated, they are also distinct from each other.
Diagnosis of MCAS
MCAS may be diagnosed when the symptoms of MC activation are systemic (involving more than one organ system), severe, and recurrent and the MCAS criteria are fulfilled [17••, 18••]. There are three sets of criteria required for an MCAS diagnosis as illustrated in Fig. 1: (1) the presence of typical, severe, episodic MC activation symptoms in ≥ 2 organ systems; (2) the detection of a substantial transient increase in a validated marker of MC activation during the symptomatic event; (3) the control of symptoms with MC mediator–targeting drugs.
The clinical criterion of MCAS requires the simultaneous involvement of ≥ 2 organ systems [17••, 18••]. Thus, MCAS events typically meet the clinical criteria of anaphylaxis. For instance, flushing and hypotensive syncope occurring simultaneously strongly suggest MCAS [19•]. When MC activation–related symptoms are severe and recurrent, the possibility of MCAS diagnosis may be considered. These symptoms encompass a range of organ systems, including the skin (urticaria, angioedema, and flushing), the gastrointestinal system (nausea, vomiting, diarrhea, and abdominal cramping), the cardiovascular system (tachycardia, hypotension, syncope), and the upper and lower respiratory systems (conjunctival injection, nasal pruritus, stuffiness, wheezing, dyspnea). Although neurological and/or musculoskeletal symptoms are commonly observed, they are not exclusive to MCAS [18••, 19•].
Secondly, the diagnosis of MCAS requires laboratory proof. Hence, the clinical symptoms of MCAS are associated with an acute, substantial increase in the levels of a validated mediator of systemic MC activation during an episode, either in serum or urine, compared with the patient’s baseline levels. Without including such biochemical markers and their event-related increase, the clinical symptomatology cannot be objectively confirmed. Currently, tryptase is the most MC-specific mediator that best fulfills the laboratory criterion and is used as a gold standard to document MC activation [20,21,22]. The serum tryptase level usually increases during acute events of systemic MC activation (e.g., anaphylaxis, MCAS), peaks in serum about 1 h after clinical onset of the event, and then declines with a t½ of about 2 h, so may remain elevated 3 h (1 t½), 5 h (2 × t½), or longer, depending on the magnitude of the initial elevation, which correlates best with the magnitude of the drop in mean arterial pressure [23,24,25]. Genetically determined normal serum baseline tryptase (sBT) level is generally considered < 8 ng/mL. To diagnose MCAS, the event-related tryptase should be greater than sBT * 1.2 + 2 ng/mL to confirm the clinical suspicion of MC activation, i.e., typical clinical symptoms of anaphylaxis are also present [17••, 18••, 19•]. This approach has been validated and is broadly accepted [26, 27•]. Unfortunately, there are some drawbacks in clinical practice, e.g., if acute sample collection is overlooked or delayed. If there are no previous sBT levels available, such baseline measurement should be determined in serum collected after a minimum of 24 h following the complete recovery from a suspected MC activation episode. Moreover, it should be kept in mind that a normal sBT level does not exclude MCAS, whereas a high sBT alone is not an indication or criterion of MCAS.
Mediators other than tryptase, including urinary metabolites of histamine, prostaglandin D2 (PGD2), and leukotrienes, are also available but less specific for MCs and MCAS [28, 29, 30••]. Additionally, the sensitivity and specificity of these markers have not been determined, nor have the reliable indicators of systemic MC activation, such as significant increase and cut-off levels. However, recently, it has been suggested to consider levels higher than 30% above the upper limit of normal as pathologic [18••, 30••]. Although 24-h samples of urinary metabolites are advised, shorter collection times or spot analyses are also discussed [28, 29].
Urinary metabolites of histamine have been studied and reported to correlate with MC burden and MC activation [28, 31]. N-methyl histamine and 1-methyl-4-imidazole acetic acid are the most commonly measured histamine metabolites [32,33,34]. Measuring plasma histamine levels as a marker of MC activation is not generally recommended, because histamine is often derived from basophils at baseline and can be influenced by a variety of factors during and after blood collection including bacterial flora of the urinary tract, storage conditions, and diet [31]. Furthermore, PGD2 is a well-known product of activated MCs [28, 35,36,37,38,39]. Several studies have shown that during anaphylaxis, as well as in patients with systemic mastocytosis (SM), the levels of the prostaglandin D2 metabolite 9α-11β-PGF2 in urinary samples are elevated compared to healthy controls [28, 35, 40, 41]. However, in most studies, the event-related increases of PGD2 over the individual’s baseline have not been reported. PGD2, while primarily released by MC, is also produced by other immune and nonimmune cell types [42,43,44,45]. This is important to recognize, because elevations in PGD2 might be due to a pathologic process independent of MC activation. Additionally, leukotriene C4 (LTC4) is a lipid mediator that is released during MC activation and undergoes metabolism into leukotriene D4, which is then converted to leukotriene E4 (LTE4) [46]. Urinary LTE4 was reported to be higher in patients with anaphylaxis who developed severe hypotension and also in patients with SM [41, 47,48,49,50]. Although these lipid mediator metabolites may be quite useful at ruling out MC activation when measured in urine produced during the onset and several hours after onset of the MC activation event, assays are difficult to perform and only available in a few laboratories.
Moreover, the clinical utility of serotonin, neuropeptides, heparin, platelet-activating factor (PAF), and chromogranin A (CgA) as potential biomarkers for MC activation remains unproven due to insufficient data, despite ongoing discussions [51,52,53,54,55,56,57]. For instance, the reported rise in plasma heparin activity following venous occlusion in patients with MC activation symptoms does not serve as sufficient validation for utilizing this test as a biomarker for MC activation [54]. Furthermore, no evidence currently exists to demonstrate a causative role of venous occlusion in MC activation. Additionally, there is currently no scientific evidence supporting CgA as a biomarker for MC activation in humans, and reported data show no elevation in CgA levels among mastocytosis patients [57].
Thirdly, the MCAS diagnosis requires a favorable response to agents that act as MC stabilizers or inhibitors of MC mediators, such as histamine receptor antagonists (H1- and H2-antihistamines), leukotriene blockers, MC stabilizers, and aspirin or non-steroidal anti-inflammatory agents (NSAIDs) [15•, 58, 59•]. A stepwise approach is recommended for treating MCAS patients. Ideally, the therapy should focus on addressing the elevated mediators and controlling symptoms with the lowest effective dose. Measuring urinary mediators during flares may help to identify the specific mediator(s) responsible for the symptoms, and therapies are expected to provide relief and decrease MC activation events. In rare cases, anti-IgE therapy or KIT-targeting kinase blockers may be required [60, 61•, 62•, 63,64,65].
Anaphylaxis Versus MCAS: Related but Not Identical
Anaphylaxis is the best recognized systemic MC activation disorder and is caused by excessive release of various MC mediators leading to a constellation of varied symptoms from different organ systems. It is an emergency condition and may potentially lead to death by airway obstruction or cardiovascular collapse, if not promptly treated. Anaphylaxis is usually considered to be a rare condition and the studies from the USA suggest an incidence of up to 40–50 people per 100,000 person-years [66,67,68], whereas the studies from Europe suggest a lower incidence of 1.5–7.9 per 100,000 person-years [69, 70]. Moreover, the lifetime prevalence of anaphylaxis has been estimated to be approximately 0.3% [71]. Furthermore, the food-induced anaphylaxis is the most common cause in children corresponding to 80–92% of the anaphylaxis [72], whereas Hymenoptera venom– or drug-induced anaphylaxis is dominating elicitors among adults [73].
The diagnosis of anaphylaxis may be challenging and the line differentiating an allergic reaction from anaphylaxis is not always easily discernible. According to international consensus on the clinical criteria, the diagnosis of anaphylaxis requires concurrent occurrence of symptoms from minimum two organ systems that are related to the cutaneous, gastrointestinal, respiratory, and cardiovascular systems [74]. These criteria have been widely adopted and both retrospectively [75] and prospectively [76] validated. The required organ system involvement varies depending upon whether there is a “likely” or “known” trigger for the actual patient. Exceptionally, in context of confirmed allergy (e.g., insect venom, drug) for the given patient, an anaphylaxis diagnosis can be made only by cardiovascular system involvement (hypotension and/or syncope) after re-exposure. Additionally, even when there is no likely cause of the reactions, as in unprovoked anaphylaxis, when the onset of illness is acute, a diagnosis of anaphylaxis can be made when either reduced blood pressure (or associated symptoms, such as syncope) and/or respiratory compromise or laryngeal edema is present accompanied by the involvement of the skin–mucosal tissue symptoms (Fig. 2) [74].
Thus, anaphylaxis and MCAS are interrelated, but two distinct conditions. Patients with anaphylaxis are the archetype of MCAS; however, not all anaphylaxis episodes fulfill the diagnostic criteria of MCAS. In order to be qualified as MCAS, it also requires that these clinical reactions are recurrent (at least two episodes) as well as laboratory and response criterion are also fulfilled. Thus, not all anaphylaxis episodes can be classified as MCAS. Likewise, not all MCAS episodes reach the severity of anaphylaxis and fulfill the criteria of anaphylaxis. For instance, in patients with unprovoked episodes of MC activation, concomitant appearance of cutaneous and GI symptoms can be considered the clinical criterion of MCAS; nevertheless, to classify this as unprovoked/idiopathic anaphylaxis, in addition to above-mentioned symptoms, either respiratory or cardiovascular system involvement is required. Hence, not all MCAS episodes fulfill the criteria of anaphylaxis [77•]. Figure 2 illustrates the clinical criteria of anaphylaxis in different context and compares those to clinical criterion of MCAS.
Hence, all above-mentioned three criteria should be fulfilled to confirm a diagnosis of MCAS. Moreover, the documented presence of clonal MCs alone or the diagnosis of cutaneous mastocytosis (CM) or SM alone is not an indication of MC activation, even though such patients are susceptible to severe MC activation–related events that could lead to the diagnosis of MCAS. Additionally, increased levels of sBT or other MC mediators alone should not be employed to diagnose MCAS, if an “event-related” transient increase (from the patient’s baseline) of a specific MC mediator is not confirmed. For instance, tryptase levels may be elevated in unrelated conditions, such as hypereosinophilic syndromes, myelodysplastic syndrome, helminth infestation, end-stage kidney disease, and hereditary alpha-tryptasemia (HαT). Furthermore, given that the clinical symptoms often ascribed to MCAS are not consistently distinct for MC activation, it becomes crucial to establish their association with MC activation. Otherwise, most patients with SM and many with unrelated disorders would be misdiagnosed with MCAS.
Classification of MCAS
Upon confirmation of an MCAS diagnosis, further classification becomes imperative resulting in the categorization of MCAS into three principal variants with varying mechanisms that activate MC in different MCAS phenotypes [17••, 18••].
Primary “Clonal” MCAS
In some instances, patients suffering from MCAS may display coexisting clonal MCs within the bone marrow, as seen in both mastocytosis (SM or CM) or monoclonal mast cell activation syndrome (MMAS) [17••, 18••]. Additionally, patients presenting with clonal MC disorders commonly exhibit varying extents of expansion in the MC compartment derived from a progenitor carrying a genetic defect that presumably reduces the cell’s threshold for activation [15•, 16•]. These patients may have elevated sBT levels, carry KIT D816V mutations in lesional MCs, or have other markers of MC clonality, such as aberrant CD25 expression. Such MCAS patients are considered to have primary (i.e., clonal) MCAS and its diagnosis can only be made after an extracutaneous biopsy, most often after a bone marrow biopsy [17••, 18••]. Thus, patients with clonal MCAS are required to fulfill the diagnostic criteria of both MCAS and clonal MC disease as below.
Mastocytosis
Mastocytosis encompasses a complex heterogeneous multisystem disorder characterized by a pathologic activation and accumulation of clonally aberrant MCs in one or more organs, including the skin, bone marrow, and gastrointestinal tract [78, 79•, 80••]. It is a rare condition, and its prevalence is estimated to be 1 in 10,000 persons in recent studies [81,82,83,84]. In general, mastocytosis can be divided into two main categories: CM and SM involving at least one additional organ than the skin. CM is the main form of the disease in children and the most common form of skin involvement is maculopapular cutaneous lesions, also known as urticaria pigmentosa (UP). The majority of children have a benign course and experience spontaneous improvement; however, patients with adult-onset mastocytosis have a persistent disease and may or may not present with skin lesions. According to the WHO diagnostic criteria, the diagnosis of SM requires the existence of a major and a minor criterion or three minor criteria on extracutaneous biopsy materials, most commonly from the bone marrow (see Table 1) [78, 79•, 80••]. In the majority of adult patients with UP, which is known as mastocytosis in the skin (MIS), MC infiltrates are also found in the bone marrow, corresponding to the final diagnosis of SM [79•]. Moreover, SM has been classified into several subgroups, with more than 85% of affected subjects having indolent SM (ISM) with a good prognosis [83, 84]. The remaining 15% of affected subjects have more aggressive variants, i.e., advanced SM (including aggressive SM, SM with associated hematologic neoplasm, and MC leukemia) with a poor prognosis [78, 79•].
The clinical course of SM varies greatly, ranging from asymptomatic disease to a highly aggressive course. Patients with ISM may exhibit various clinical symptoms such as flushing, itching, rapid heartbeat, dizziness, low blood pressure, fainting, breathing difficulties, abdominal pain, nausea, vomiting, diarrhea, headache, lethargy, fatigue, impaired concentration, irritability, anxiety, depression, arthralgia, myalgia, and osteoporosis due to the local or remote effects of MC mediators [78]. However, not every patient exhibits every one of these symptoms, so the reason for this heterogeneity remains unclear. Nevertheless, a history of flushing is a cardinal symptom. Moreover, some subjects may experience isolated symptoms, whereas others develop a constellation of signs and symptoms indistinguishable from those of anaphylaxis [85, 86]. Typically, patients suddenly feel very warm and then experience palpitations, dizziness, and a decrease in blood pressure due to systemic vasodilatation that often leads to syncope [50]. Acute attacks may be brief or prolonged, but duration is usually 15 to 30 min [50]. Patients often experience severe fatigue lasting around 24 h following the spells [50]. Triggers vary greatly among patients and include physical exertion, cold, heat, insect venoms, consumption of alcohol, infections, non-steroidal anti-inflammatory drugs (NSAIDs), and emotional stress. The mediator levels do not usually show clear association with the clinical phenotypes, although the baseline levels of mediators including tryptase, histamine, and PGD2 are generally elevated [28].
Notably, anaphylaxis is less common in subjects with advanced SM compared to patients with ISM. These patients commonly experience symptoms related to MC infiltration and uncontrolled accumulation, such as cytopenia, hepatosplenomegaly, lymph adenopathy, osteolytic bone lesions, and liver dysfunction [78].
Monoclonal Mast Cell Activation Syndrome
Monoclonal mast cell activation syndrome (MMAS) is a newly recognized variant of clonal MC disorders and is characterized by severe episodes of anaphylaxis with hypotensive syncope in affected patients [87, 88]. While patients diagnosed with MMAS present detectable clonal MCs expressing the D816V mutation and/or CD25 + aberrant markers, they do not meet the diagnostic criteria established by the WHO for classifying as having SM (Table 1). Moreover, the sBT levels of these patients generally show a slight elevation, often ranging between 10 and 20 ng/mL. Additionally, they lack typical skin changes of mastocytosis (MIS).
Secondary MCAS
The majority of patients with symptoms caused by intermittent, recurrent MC activation typically have non-clonal etiologies. These patients, known as secondary MCAS, experience symptoms associated with MC activation due to the involvement of both IgE-mediated (such as food-, drug-, or Hymenoptera venom–induced anaphylaxis) and non-IgE-mediated (e.g., exercise) mechanisms.
Idiopathic MCAS
In certain cases, a patient who undergoes severe, recurrent MC activation may have an unremarkable work-up for allergic causes and exhibit no indication of clonal MC disease (typically ruled out following a bone marrow examination). These patients are evaluated for either IA or idiopathic (non-clonal) MCAS diagnoses, depending on the criteria they meet [77•].
Furthermore, over recent years, an increasing number of studies have indicated that multiple variants of MCAS can coexist within the same patient, putting these patients at the greatest risk for the development of life-threatening MCAS episodes [15•, 16•]. For instance, in patients with SM and an IgE-dependent allergy against bee or wasp venom, both the underlying SM and the underlying venom allergy may act as a trigger of anaphylaxis and thereby induce a mixed (primary + secondary) form of MCAS. Hence, such combined (mixed) form of MCAS should always be considered in patients with severe anaphylaxis. In general, the signs and symptoms of recurrent IgE-mediated anaphylaxis may be the initial presentation of secondary or combined MCAS, whereas IA can consist of the initial symptoms of clonal or idiopathic MCAS.
Hereditary Alpha-Tryptasemia
More recently, additional genetic features have been linked to an elevated risk to develop anaphylaxis and MCAS. One such factor is HαT, a genetic trait defined by extra copies of the TPSAB1 gene encoding for alpha-tryptase, and an elevated sBT concentration in most carriers [89,90,91]. Patients with HαT are generally measured to have sBT levels higher than 8 ng/mL (often > 10 ng/mL) [90]. HαT is found in approximately 6% of the general population and the majority of individuals with HαT appear to be asymptomatic [92, 93•].
However, HαT has been linked to an increased prevalence of SM and an increased risk of severe mediator-related symptoms and MCAS in those with SM [91, 94•, 95•]. Furthermore, HαT is more prevalent in those with ISM than advanced SM. Moreover, a coexisting IgE-dependent allergy, such as an insect venom allergy, is frequently observed in carriers of HαT with SM and MCAS [91, 94•, 95•]. Hence, these patients apparently are the highest risk to develop severe or even life-threatening anaphylaxis or even a combined form of MCAS [91, 94•, 95•]. Presently, however, whether a pure form of hereditary (HαT +) MCAS indeed exists is under debate. Therefore, HαT is currently thought to be a modifying factor that may influence the prevalence and severity of anaphylaxis.
When a Bone Marrow Investigation Should Be Performed
A BM examination should be considered after an initial screening which includes a thorough physical examination with skin inspection, blood counts, serum chemistry, and a sBT level, as well as peripheral blood testing for KIT D816V (Fig. 3). Moreover, if available, tryptase genotyping is recommended for the patients with sBT ≥ 8 ng/mL. If KIT D816V is detectable in an adult patient, a BM examination should be conducted regardless of the sBT and HαT status [18••]. Nevertheless, if KIT D816V mutation is not detected but HαT is found, BM investigations are not necessary unless there are other features that could suggest the presence of SM. Furthermore, in cases where a symptomatic patient presents recurring episodes of anaphylaxis and all these variables demonstrate negative findings, the application of predictive tools such as the Spanish Network on Mastocytosis (Red Española de Mastocitosis [REMA]) score [96], Karolinska score [97], or National Institutes of Health Idiopathic Clonal Anaphylaxis Score [98] becomes essential to estimate the probability of the patient having clonal MC disorder. This is particularly important in symptomatic patients who lack typical skin lesions of mastocytosis.
Diagnostic algorithm for patients with suspected MCAS. Investigations should be adjusted to the case history of individual patients. To establish the diagnosis of MCAS, all three MCAS criteria must be fulfilled. Abbreviations: sBT, serum baseline tryptase; HαT, hereditary alpha-tryptasemia; SM, systemic mastocytosis; MIS, mastocytosis in the skin
MCAS Mimickers
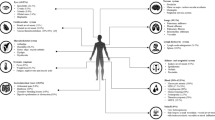
Even though an international consensus group has set diagnostic criteria and classification for MCAS in the past decade [17••, 18••, 19•], debates regarding the usage of the term MCAS in different patient categories persist, leaving unresolved controversies. A significant difficulty lies in the fact that a considerable number of patients, whose symptoms are believed to be caused by MC activation, incorrectly receive a diagnosis of MCAS without any substantial proof that their clinical manifestations and symptoms are indeed derived from MC activation and mediator release [17••, 18••, 19•]. Among these patients, there could be those who may suffer from MC activation disorders (MCADs) or non-specified MC activation reactions [80••]. In these patients, localized MC activation, milder MC activation, or MC activation possibly involving a limited set of mediators or only one organ system may be implicated. Furthermore, some of the attributed symptoms may not even be related to MC activation [80••]. This is because most symptoms attributable to MC activation, including isolated flushing, pruritus, headache, abdominal pain, or tachycardia, are not MC-specific but can also be found in other clinical conditions and disorders (Fig. 4) [99,100,101,102,103,104,105].
Symptoms and conditions mimicking mast cell activation and MCAS [18••]. When patients do not present with the typical symptoms of anaphylaxis or with chronic rather than episodic acute symptoms, it may be particularly challenging for the clinicians to establish a diagnosis. This is because most symptoms attributable to MC activation are not MC-specific but can also be found in other clinical conditions and disorders. Moreover, patients with multiple chemical, environmental, or food intolerances should not be diagnosed with MCAS if they do not meet the criteria
Additionally, a number of other conditions, such as cardiovascular pathologies (myocardial infarction, myocarditis), endocrinologic diseases (e.g., adrenal crisis, thyroid disease, estrogen or testosterone deficiency, adrenal insufficiency, carcinoid), vocal cord dysfunction, cutaneous diseases (e.g., atopic or contact dermatitis, rosacea), neurologic disorders (e.g., seizures, stroke, multiple sclerosis, meningitis, dysautonomia, vasovagal syncope), psychologic disorders (e.g., panic attacks and anxiety, depression), gastrointestinal diseases such as an inflammatory bowel disease, and infections (septicemia), can mimic symptoms of MCA. It is important to note that some of these patients may easily be misdiagnosed as having MCAS when applying less stringent criteria, but not the criteria adopted by the Vienna consensus group [17••, 18••]. Hence, a broad differential diagnosis should be considered before a diagnosis of MCAS is made when evaluating patients with suspected MC activation [17••, 18••, 19•, 106]. This process may take longer than predicted, particularly in patients with idiopathic MCAS (iMCAS), and the diagnostic delay may be approximately 4 years (according to personal experience).
Furthermore, it should also be mentioned here that studies indicating the true prevalence of MCAS using evidence-based diagnostic criteria have been lacking until recently. A newly published study investigated the prevalence and clinical characteristics of patients with iMCAS among 703 adult consecutive patients referred due to suspected mast cell disorders [107]. Interestingly, of the investigated patients, 35% patients had at least one episode of anaphylaxis. An overall prevalence of iMCAS in this study was 4.4%, with a relatively higher prevalence among patients with unprovoked anaphylaxis (27%) [107]. This study supports the notion that anaphylaxis is the archetype of MCAS and that MCAS is an uncommon condition. Thus, clinicians should be cautious when diagnosing iMCAS to avoid misdiagnosis.
Concluding Remarks
Typically presenting as anaphylaxis, MCAS encompasses a severe systemic reaction caused by the acute release of MC mediators. When patients do not present with the typical symptoms of anaphylaxis, MCAS is much less likely to be the correct diagnosis. Because, in the majority of these patients, there is only a slight increase or no increase at all in serum tryptase levels compared to the individual’s baseline [17••, 18••, 19•]. Even the other validated markers of MC activation may not even show increases in biological fluids in these patients. Consequently, these cases often pose a clinical challenge, and it may be hard to rule out the involvement of other inflammatory effector cells such as basophils or eosinophils. Hence, the ultimate diagnosis remains descriptive, as MC involvement can only be speculated.
Understanding the category of MCAS and its underlying etiology should provide a solid basis for establishing a personalized treatment plan for MCAS patients. A stepwise, individual-based approach in pharmacotherapy options appears to be the most convenient strategy [58, 59•]. Acute episodes of any variant of MCAS should be promptly treated with intramuscular epinephrine [108,109,110,111]. Allergen immunotherapy is recommended for MCAS patients with documented Hymenoptera venom allergy, and in patients with mixed MCAS, life-long immunotherapy is standard [112••].
Finally, additional research is required to identify novel biomarkers of MC activation, enabling healthcare providers in differentiating between genuine cases of MCAS and its mimickers, especially in patients with milder or chronic or localized symptoms who do not meet the Vienna consensus criteria for MCAS [17••, 18••].
Data Availability
No datasets were generated or analysed during the current study.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Valent P, Akin C, Hartmann K, Nilsson G, Reiter A, Hermine O, et al. Mast cells as a unique hematopoietic lineage and cell system: from Paul Ehrlich’s visions to precision medicine concepts. Theranostics. 2020;10(23):10743–68.
Varricchi G, Marone G. Mast cells: fascinating but still elusive after 140 years from their discovery. Int J Mol Sci. 2020;21(2):464.
Galli SJ, Borregaard N, Wynn TA. Phenotypic and functional plasticity of cells of innate immunity: macrophages, mast cells and neutrophils. Nat Immunol. 2011;12:1035–44.
da Silva EZ, Jamur MC, Oliver C. Mast cell function: a new vision of an old cell. J Histochem Cytochem. 2014;62:698–738.
Galli SJ, Kalesnikoff J, Grimbaldeston MA, Piliponsky AM, Williams CM, Tsai M. Mast cells as “tunable” effector and immunoregulatory cells: recent advances. Annu Rev Immunol. 2005;23:749–86.
Iwaki S, Tkaczyk C, Metcalfe DD, et al. Roles of adaptor molecules in mast cell activation. Chem Immunol Allergy. 2005;87:43–58.
Galli SJ, Tsai M. Mast cells in allergy and infection: versatile effector and regulatory cells in innate and adaptive immunity. Eur J Immunol. 2010;40(7):1843–51.
Gilfillan AM, Beaven MA. Regulation of mast cell responses in health and disease. Crit Rev Immunol. 2011;31(6):475–529.
Kelso JM. MRGPRX2 signaling and skin test results. J Allergy Clin Immunol Pract. 2020;8(1):426.
Castells M. Mast cell mediators in allergic inflammation and mastocytosis. Immunol Allergy Clin North Am. 2006;26(3):465–85.
Kalesnikoff J, Galli SJ. Anaphylaxis: mechanisms of mast cell activation. Chem Immunol Allergy. 2010;95:45–66.
Peavy RD, Metcalfe DD. Understanding the mechanisms of anaphylaxis. Curr Opin Allergy Clin Immunol. 2008;8:310–5.
Metcalfe DD, Peavy RD, Gilfillan AM. Mechanisms of mast cell signaling in anaphylaxis. J Allergy Clin Immunol. 2009;124(4):639–46.
Akin C, Valent P, Metcalfe DD. Mast cell activation syndrome: proposed diagnostic criteria. J Allergy Clin Immunol. 2010;126(6):1099–104.
• Gülen T, Akin C. Anaphylaxis and mast cell disorders. Immunol Allergy Clin North Am. 2022;42(1):45–63. This article focuses on the potential mechanisms leading to severe, systemic mast cell activation, as well as the differential diagnosis of range of symptoms attributable to mast cell mediator release.
• Gülen T. A puzzling mast cell trilogy: anaphylaxis, MCAS, and mastocytosis. Diagnostics. 2023;13:3307. https://doi.org/10.3390/diagnostics13213307. This paper provides a comprehensive clinical update and highlights the primary challenges encountered in the diagnosis and differential diagnosis of anaphylaxis, mast cell activation syndrome, and mastocytosis in medical practice.
•• Valent P, Akin C, Bonadonna P, Hartmann K, Brockow K, Niedoszytko M, et al. Proposed diagnostic algorithm for patients with suspected mast cell activation syndrome. J Allergy Clin Immunol Pract. 2019;7(4):1125–33. This is a key paper proposing a diagnostic algorithm through which a clinically relevant systemic mast cell activation can be suspected and mast cell activation syndrome can subsequently be diagnosed, while also distinguishing it from other conditions that may present with similar symptoms and characteristics.
•• Gülen T, Akin C, Bonadonna P, Siebenhaar F, Broesby-Olsen S, Brockow K, et al. Selecting the right criteria and proper classification to diagnose mast cell activation syndromes: a critical review. J Allergy Clin Immunol Pract. 2021;9(11):3918–28. https://doi.org/10.1016/j.jaip.2021.06.011. This is an important clinical appraisal of the current literature on mast cell activation syndrome (MCAS), focusing on the specificity, sensitivity, and strength of MCAS-related parameters proposed for diagnosing, classifying, and distinguishing MCAS and its variants from MCAS mimickers.
• Weiler CR, Austen KF, Akin C, Barkoff MS, Bernstein JA, Bonadonna P, et al. AAAAI Mast Cell Disorders Committee Work Group Report: mast cell activation syndrome (MCAS) diagnosis and management. J Allergy Clin Immunol. 2019;144:883–96. This paper aims to offer clinicians practical diagnostic criteria that exhibit both high sensitivity and specificity to diagnose most cases of mast cell activation syndrome without overdiagnosing the disorder in patients who likely have other conditions.
Schwartz LB, Metcalfe DD, Miller JS, Earl H, Sullivan T. Tryptase levels as an indicator of mast-cell activation in systemic anaphylaxis and mastocytosis. N Engl J Med. 1987;316:1622–6.
Schwartz LB. Diagnostic value of tryptase in anaphylaxis and mastocytosis. Immunol Allergy Clin North Am. 2006;26(3):451–63.
Schwartz LB. Clinical utility of tryptase levels in systemic mastocytosis and associated hematologic disorders. Leuk Res. 2001;25:553–62.
Shanmugam G, Schwartz LB, Khan DA. Prolonged elevation of serum tryptase in idiopathic anaphylaxis. J Allergy Clin Immunol. 2006;117:950–1.
Van der Linden PW, Hack CE, Poortman J, Vivié-Kipp YC, Struyvenberg A, van der Zwan JK. Insect-sting challenge in 138 patients: relation between clinical severity of anaphylaxis and mast cell activation. J Allergy Clin Immunol. 1992;90:110–8.
Schwartz LB, Bradford TR, Rouse C, Irani AM, Rasp G, Van der Zwan JK, et al. Development of a new, more sensitive immunoassay for human tryptase: use in systemic anaphylaxis. J Clin Immunol. 1994;14:190–204.
Baretto RL, Beck S, Heslegrave J, Melchior C, Mohamed O, Ekbote A, et al. Validation of international consensus equation for acute serum total tryptase in mast cell activation: a perioperative perspective. Allergy. 2017;72:2031–4.
• Valent P, Bonadonna P, Hartmann K, Broesby-Olsen S, Brockow K, Butterfield JH, et al. Why the 20% + 2 tryptase formula is a diagnostic gold standard for severe systemic mast cell activation and mast cell activation syndrome. Int Arch Allergy Immunol. 2019;180:44–51. This paper highlights the emerging importance and value of the 20% + 2 formula in clinical practice and its role as a criterion of severe systemic mast cell activation and mast cell activation syndrome.
Gulen T, Moller Westerberg C, Lyberg K, Ekoff M, Kolmert J, Bood J, et al. Assessment of in vivo mast cell reactivity in patients with systemic mastocytosis. Clin Exp Allergy. 2017;47:909–17.
Butterfield J, Weiler CR. The utility of measuring urinary metabolites of mast cell mediators in systemic mastocytosis and mast cell activation syndrome. J Allergy Clin Immunol Pract. 2020;8:2533–41.
•• Butterfield JH. Increased excretion of mast cell mediator metabolites during mast cell activation syndrome. J Allergy Clin Immunol Pract. 2023;11(8):2542–6. https://doi.org/10.1016/j.jaip.2023.02.017. This study establishes the ratios of acute/baseline levels for urinary metabolites of prostaglandin D2, histamine, or leukotriene E4 in conjunction with a tryptase increase of 20% plus 2 ng/mL as a reliable indicator for diagnosing mast cell activation syndrome and identifies a substantial increase from baseline.
Keyzer JJ, de Monchy JG, van Doormaal JJ, van Voorst Vader PC. Improved diagnosis of mastocytosis by measurement of urinary histamine metabolites. N Engl J Med. 1983;309:1603–5.
Granerus G, Roupe G. Increased urinary methylimidazoleacetic acid (MelmAA) as an indicator of systemic mastocytosis. Agents Actions. 1982;12:29–31.
Van Doormaal JJ, van der Veer E, van Voorst Vader PC, Kluin PM, Mulder AB, van der Heide S, et al. Tryptase and histamine metabolites as diagnostic indicators of indolent systemic mastocytosis without skin lesions. Allergy. 2012;67:683–90.
Divekar R, Butterfield J. Urinary 11b-PGF2a and N-methyl histamine correlate with bone marrow biopsy findings in mast cell disorders. Allergy. 2015;70:1230–8.
Roberts LJ 2nd, Sweetman BJ, Lewis RA, Austen KF, Oates JA. Increased production of prostaglandin D2 in patients with systemic mastocytosis. N Engl J Med. 1980;303:1400–4.
Awad JA, Morrow JD, Roberts LJ 2nd. Detection of the major urinary metabolite of prostaglandin D2 in the circulation: demonstration of elevated levels in patients with disorders of systemic mast cell activation. J Allergy Clin Immunol. 1994;93:817–24.
Dahlen SE, Kumlin M. Monitoring mast cell activation by prostaglandin D2 in vivo. Thorax. 2004;59:453–5.
Butterfield JH, Weiler CR. Prevention of mast cell activation disorder associated clinical sequelae of excessive prostaglandin D (2) production. Int Arch Allergy Immunol. 2008;147:338–43.
Ravi A, Butterfield J, Weiler CR. Mast cell activation syndrome: improved identification by combined determinations of serum tryptase and 24-hour urine 11b-prostaglandin2a. J Allergy Clin Immunol Pract. 2014;2:775–8.
Ono E, Taniguchi M, Mita H, Fukutomi Y, Higashi N, Miyazaki E, et al. Increased production of cysteinyl leukotrienes and prostaglandin D2 during human anaphylaxis. Clin Exp Allergy. 2009;39:72–80.
Nassiri M, Eckermann O, Babina M, Edenharter G, Worm M. Serum levels of 9a,11b-PGF2 and cysteinyl leukotrienes are useful biomarkers of anaphylaxis. J Allergy Clin Immunol. 2016;137:312-314.e7.
Tanaka K, Ogawa K, Sugamura K, Nakamura M, Takano S, Nagata K. Cutting edge: differential production of prostaglandin D2 by human helper T cell subsets. J Immunol. 2000;164:2277–80.
Gallant MA, Samadfam R, Hackett JA, Antoniou J, Parent JL, de Brum-Fernandes AJ. Production of prostaglandin D(2) by human osteoblasts and modulation of osteoprotegerin, RANKL, and cellular migration by DP and CRTH2 receptors. J Bone Miner Res. 2005;20:672–81.
Shimura C, Satoh T, Igawa K, Aritake K, Urade Y, Nakamura M, et al. Dendritic cells express hematopoietic prostaglandin D synthase and function as a source of prostaglandin D2 in the skin. Am J Pathol. 2010;176:227–37.
Luna-Gomes T, Magalhães KG, Mesquita-Santos FP, Bakker-Abreu I, Samico RF, Molinaro R, et al. Eosinophils as a novel cell source of prostaglandin D2: autocrine role in allergic inflammation. J Immunol. 2011;187:6518–26.
Fanning LB, Boyce JA. Lipid mediators and allergic diseases. Ann Allergy Asthma Immunol. 2013;111:155–62.
Denzlinger C, Haberl C, Wilmanns W. Cysteinyl leukotriene production in anaphylactic reactions. Int Arch Allergy Immunol. 1995;108:158–64.
Tolar J, Tope WD, Neglia JP. Leukotriene-receptor inhibition for the treatment of systemic mastocytosis. N Engl J Med. 2004;350:735–6.
Butterfield JH. Increased leukotriene E4 excretion in systemic mastocytosis. Prostaglandins Other Lipid Mediat. 2010;92:73–6.
Gulen T, Hagglund H, Dahlen SE, Sander B, Dahlen B, Nilsson G. Flushing, fatigue, and recurrent anaphylaxis: a delayed diagnosis of mastocytosis. Lancet. 2014;383:1608.
Kushnir-Sukhov NM, Brittain E, Scott L, Metcalfe DD. Clinical correlates of blood serotonin levels in patients with mastocytosis. Eur J Clin Invest. 2008;38:953–8.
Ritter M, El-Nour H, Hedblad MA, Butterfield JH, Beck O, Stephanson N, et al. Serotonin and its 5-HT1 receptor in human mastocytosis. Immunopharmacol Immunotoxicol. 2012;34:679–85.
Theoharides TC, Valent P, Akin C. Mast cells, mastocytosis, and related disorders. N Engl J Med. 2015;373:163–72.
Vysniauskaite M, Hertfelder HJ, Oldenburg J, Dreßen P, Brettner S, Homann J, et al. Determination of plasma heparin level improves identification of systemic mast cell activation disease. PLoS ONE. 2015;10: e0124912.
Vadas P, Gold M, Perelman B, Liss GM, Lack G, Blyth T, et al. Platelet activating factor, PAF acetylhydrolase, and severe anaphylaxis. N Engl J Med. 2008;358:28–35.
Vadas P, Perelman B, Liss G. Platelet-activating factor, histamine, and tryptase levels in human anaphylaxis. J Allergy Clin Immunol. 2013;131:144–9.
Hanjra P, Lee CR, Maric I, Carter M, Olivera A, Metcalfe DD, et al. Chromogranin A is not a biomarker of mastocytosis. J Allergy Clin Immunol Pract. 2018;6:687-689.e4.
Gulen T, Akin C. Pharmacotherapy of mast cell disorders. Curr Opin Allergy Clin Immunol. 2017;17(4):295–303.
• Gulen T. Management of mediator symptoms, allergy, and anaphylaxis in mastocytosis. Immunol Allergy Clin N Am. 2023;43(4):681–98. https://doi.org/10.1016/j.iac.2023.04.010. This paper comprehensively evaluates management of mast cell mediator–related symptoms, including allergy and anaphylaxis, among patients with mastocytosis.
Broesby-Olsen S, Vestergaard H, Mortz CG, et al. Omalizumab prevents anaphylaxis and improves symptoms in systemic mastocytosis: efficacy and safety observations. Allergy. 2018;73(1):230–8.
• Akin C, Arock M, Valent P. Tyrosine kinase inhibitors for the treatment of indolent systemic mastocytosis: are we there yet? J Allergy Clin Immunol. 2022;149(6):1912–8. https://doi.org/10.1016/j.jaci.2022.04.020. This article discusses the current state in the treatment of indolent systemic mastocytosis with tyrosine kinase inhibitors, with special emphasis on treatment responses and potential adverse effects.
• Akin C. Tyrosine kinase inhibitors in non-advanced systemic mastocytosis. Immunol Allergy Clin North Am. 2023;43(4):743–50. https://doi.org/10.1016/j.iac.2023.05.001. A comprehensive update on management of non-advanced systemic mastocytosis with tyrosine kinase inhibitors, their treatment responses, and potential toxicity and short- and long-term safety.
Hartmann K, Gotlib J, Akin C, et al. Midostaurin improves quality of life and mediator-related symptoms in advanced systemic mastocytosis. J Allergy Clin Immunol. 2020;146(2):356–66.
Akin C, Elberink HO, Gotlib J, et al. PIONEER: a randomized, double-blind, placebo-controlled, phase 2 study of avapritinib in patients with indolent or smoldering systemic mastocytosis (SM) with symptoms inadequately controlled by standard therapy. J Allergy Clin Immunol 2020;145(2):AB336.
Gotlib J, Kluin-Nelemans HC, George TI, et al. Efficacy and safety of midostaurin in advanced systemic mastocytosis. N Engl J Med. 2016;374(26):2530–41.
Bagos-Estevez AG, Ledford DK. Anaphylaxis: definition, epidemiology, diagnostic challenges, grading system. Immunol Allergy Clin North Am. 2022;42(1):1–11. https://doi.org/10.1016/j.iac.2021.09.001.
Wood RA, Camargo CA Jr, Lieberman P, et al. Anaphylaxis in America: the prevalence and characteristics of anaphylaxis in the United States. J Allergy Clin Immunol. 2014;133(2):461–7.
Decker WW, Campbell RL, Manivannan V, et al. The etiology and incidence of anaphylaxis in Rochester, Minnesota: a report from the Rochester Epidemiology Project. J Allergy Clin Immunol. 2008;122(6):1161–5.
Worm M. Epidemiology of anaphylaxis. Chem Immunol Allergy. 2010;95:12–21.
Panesar SS, Javad S, de Silva D, et al. The epidemiology of anaphylaxis in Europe: a systematic review. Allergy. 2013;68(11):1353–61.
Turner PJ, Jerschow E, Umasunthar T, et al. Fatal anaphylaxis: mortality rate and risk factors. J Allergy Clin Immunol Pract. 2017;5(5):1169–78.
Grabenhenrich LB, Dölle S, Moneret-Vautrin A, Köhli A, Lange L, Spindler T, et al. Anaphylaxis in children and adolescents: the European Anaphylaxis Registry. J Allergy Clin Immunol. 2016;137(4):1128-1137.e1. https://doi.org/10.1016/j.jaci.2015.11.015. Epub 2016 Jan 21.
Worm M, Eckermann O, Dölle S, Aberer W, Beyer K, Hawranek T, et al. Triggers and treatment of anaphylaxis: an analysis of 4,000 cases from Germany. Austria and Switzerland Dtsch Arztebl Int. 2014;111(21):367–75. https://doi.org/10.3238/arztebl.2014.0367.
Sampson HA, Munoz-Furlong A, Campbell RL, Adkinson NF Jr, Bock SA, Branum A, et al. Second symposium on the definition and management of anaphylaxis: summary report–second National Institute of Allergy and Infectious Disease/Food Allergy and Anaphylaxis Network symposium. Ann Emerg Med. 2006;47(4):373–80.
Campbell RL, Hagan JB, Manivannan V, et al. Evaluation of national institute of allergy and infectious diseases/food allergy and anaphylaxis network criteria for the diagnosis of anaphylaxis in emergency department patients. J Allergy Clin Immunol. 2012;129(3):748–52.
Loprinzi Brauer CE, Motosue MS, Li JT, et al. Prospective validation of the NIAID/FAAN criteria for emergency department diagnosis of anaphylaxis. J Allergy Clin Immunol Pract. 2016;4(6):1220–6.
• Gulen T, Akin C. Idiopathic anaphylaxis: a perplexing diagnostic challenge for allergists. Curr Allergy Asthma Rep. 2021;21(2):11. A comprehensive review that focuses on all practical issues in patients with idiopathic anaphylaxis including its diagnostic and management.
Gulen T, Hagglund H, Dahlen B, Nilsson G. Mastocytosis: the puzzling clinical spectrum and challenging diagnostic aspects of an enigmatic disease. J Intern Med. 2016;279(3):211–28.
• Valent P, Akin C, Hartmann K, Alvarez-Twose I, Brockow K, Hermine O, et al. Updated diagnostic criteria and classification of mast cell disorders: a consensus proposal. Hemasphere. 2021;5(11): e646. This is a consensus proposal providing updated information on diagnostic evaluations and prognostication of mast cell disorders in daily practice.
•• Valent P, Hartmann K, Bonadonna P, Gülen T, Brockow K, Alvarez-Twose I, Hermine O, et al. Global classification of mast cell activation disorders: an ICD-10-CM-Adjusted Proposal of the ECNM-AIM Consortium. J Allergy Clin Immunol Pract. 2022;10(8):1941–50. https://doi.org/10.1016/j.jaip.2022.05.007. This is an essential paper discussing diagnostic features and criteria for disorders associated with mast cell activation and propose an ICD-10-CM-adjusted de novo classification of mast cell activation disorders.
van Doormaal JJ, Arends S, Brunekreeft KL, van der Wal VB, Sietsma J, van Voorst Vader PC, et al. Prevalence of indolent systemic mastocytosis in a Dutch region. J Allergy Clin Immunol. 2013;131(5):1429–31.
Cohen SS, Skovbo S, Vestergaard H, Kristensen T, Møller M, Bindslev-Jensen C, et al. Epidemiology of systemic mastocytosis in Denmark. Br J Haematol. 2014;166(4):521–8.
Zanotti R, Bonifacio M, Isolan C, Tanasi I, Crosera L, Olivieri F, et al. A multidisciplinary diagnostic approach reveals a higher prevalence of indolent systemic mastocytosis: 15-years’ experience of the GISM Network. Cancers. 2021;13:6380.
Ungerstedt J, Ljung C, Klimkowska M, Gülen T. Clinical outcomes of adults with systemic mastocytosis: a 15-year multidisciplinary experience. Cancers. 2022;14:3942. https://doi.org/10.3390/cancers14163942.
Gulen T, Hagglund H, Dahlen B, Nilsson G. High prevalence of anaphylaxis in patients with systemic mastocytosis - a single-centre experience. Clin Exp Allergy. 2014;44(1):121–9.
Brockow K, Jofer C, Behrendt H. Anaphylaxis in patients with mastocytosis: a study on history, clinical features and risk factors in 120 patients. Allergy. 2008;63(2):226–32.
Akin C, Scott LM, Kocabas CN, Kushnir-Sukhov N, Brittain E, Noel P, Metcalfe DD. Demonstration of an aberrant mast-cell population with clonal markers in a subset of patients with “idiopathic” anaphylaxis. Blood. 2007;110(7):2331–3.
Sonneck K, Florian S, Mullauer L, Wimazal F, Födinger M, Sperr WR, Valent P. Diagnostic and subdiagnostic accumulation of mast cells in the bone marrow of patients with anaphylaxis: Monoclonal mast cell activation syndrome. Int Arch Allergy Immunol. 2007;142(2):158–64.
Lyons JJ, Sun G, Stone KD, Nelson C, Wisch L, O’Brien M, et al. Mendelian inheritance of elevated serum tryptase associated with atopy and connective tissue abnormalities. J Allergy Clin Immunol. 2014;133(5):1471–4.
Lyons JJ, Yu X, Hughes JD, Le QT, Jamil A, Bai Y, et al. Elevated basal serum tryptase identifies a multisystem disorder associated with increased TPSAB1 copy number. Nat Genet. 2016;48(12):1564–9.
Sprinzl B, Greiner G, Uyanik G, Arock M, Haferlach T, Sperr WR, et al. Genetic regulation of tryptase production and clinical impact: hereditary alpha tryptasemia, mastocytosis and beyond. Int J Mol Sci. 2021;22(5):2458.
Robey RC, Wilcock A, Bonin H, et al. Hereditary alpha-tryptasemia: UK prevalence and variability in disease expression. J Allergy Clin Immunol Pract. 2020;8(10):3549–56.
• Chollet MB, Akin C. Hereditary alpha tryptasemia is not associated with specific clinical phenotypes. J Allergy Clin Immunol. 2021;148(3):889–94. Study highlighting for the first time that patients with hereditary alpha-tryptasemia do not have any specific clinical phenotype.
• Greiner G, Sprinzl B, Górska A, Ratzinger F, Gurbisz M, Witzeneder N, et al. Hereditary alpha tryptasemia is a valid genetic biomarker for severe mediator-related symptoms in mastocytosis. Blood. 2021;137(2):238–47. This study demonstrates that co-existence of hereditary alpha-tryptasemia among patients with mastocytosis increases susceptibility to severe mast cell mediator–related symptoms.
• Lyons JJ, Chovanec J, O’Connell MP, Liu Y, Šelb J, Zanotti R, et al. Heritable risk for severe anaphylaxis associated with increased alpha-tryptase-encoding germline copy number at TPSAB1. J Allergy Clin Immunol. 2021;147(2):622–32. This study highlights that risk for severe anaphylaxis in humans is associated with inherited differences in α-tryptase-encoding copies at TPSAB1.
Alvarez-Twose I, Gonzalez de Olano D, Sanchez-Munoz L, et al. Clinical, biological, and molecular characteristics of clonal mast cell disorders presenting with systemic mast cell activation symptoms. J Allergy Clin Immunol 2010;125(6):1269–78.
Gulen T, Hagglund H, Sander B, et al. The presence of mast cell clonality in patients with unexplained anaphylaxis. Clin Exp Allergy. 2014;44(9):1179–87.
Carter MC, Desai A, Komarow HD, et al. A distinct biomolecular profile identifies monoclonal mast cell disorders in patients with idiopathic anaphylaxis. J Allergy Clin Immunol. 2018;141(1):180–8.
Yale SH, Vasudeva S, Mazza JJ, Rolak L, Arrowood J, Stichert S, et al. Disorders of flushing. Compr Ther. 2005;31:59–71.
Van der Lely AJ, de Herder WW. Carcinoid syndrome: diagnosis and medical management. Arq Bras Endocrinol Metabol. 2005;49:850–60.
Heymann WR. Flushing, pheochromocytoma, and the dermatologist. J Am Acad Dermatol. 2006;55:1075–7.
Boutzios G, Kaltsas G. Clinical syndromes related to gastrointestinal neuroendocrine neoplasms. Front Horm Res. 2015;44:40–57.
Huang H, Hohler AD. The dermatological manifestations of postural tachycardia syndrome: a review with illustrated cases. Am J Clin Dermatol. 2015;16:425–30.
Hannah-Shmouni F, Stratakis CA, Koch CA. Flushing in (neuro)endocrinology. Rev Endocr Metab Disord. 2016;17:373–80.
Rastogi V, Singh D, Mazza JJ, Parajuli D, Yale SH. Flushing disorders associated with gastrointestinal symptoms: part 1, neuroendocrine tumors, mast cell disorders and hyperbasophila. Clin Med Res. 2018;16:16–28.
Valent P, Akin C. Doctor, I think I am suffering from MCAS: differential diagnosis and separating facts from fiction. J Allergy Clin Immunol Pract. 2019;7:1109–14.
•• Zaghmout T, Maclachlan L, Bedi N, Gülen T. Low prevalence of idiopathic mast cell activation syndrome among 703 patients with suspected mast cell disorders. J Allergy Clin Immunol Pract. 2023 Dec 4:S2213–2198(23)01310–7. https://doi.org/10.1016/j.jaip.2023.11.041. Epub ahead of print. PMID: 38056692. This is the first systematic study that provides epidemiological data on patients with idiopathic MCAS diagnosed according to the evidence-based diagnostic criteria and evaluates and compares its clinical and laboratory characteristics with clonal MCAS patients.
Roberts LJ 2nd, Turk JW, Oates JA. Shock syndrome associated with mastocytosis: pharmacologic reversal of the acute episode and therapeutic prevention of recurrent attacks. Adv Shock Res. 1982;8:145–52.
Valent P, Akin C, Arock M. Diagnosis and treatment of anaphylaxis in patients with mastocytosis. Curr Treat Options Allergy. 2014;1(3):247–61.
Baalmann DV, Hagan JB, Li JT, Hess EP, Campbell RL. Appropriateness of epinephrine use in ED patients with anaphylaxis. Am J Emerg Med 2016;34(2):174–9.
Lieberman PL. Recognition and first-line treatment of anaphylaxis. Am J Med. 2014;127(1 Suppl):S6-11.
•• Jarkvist J, Salehi C, Akin C, Gulen T. Venom immunotherapy in patients with clonal mast cell disorders: IgG4 correlates with protection. Allergy. 2020;75(1):169–77. Findings from this study suggest that the elevated levels of specific IgG4 antibodies during venom immunotherapy in venom allergy patients with mastocytosis indicate protection from field re-stings and may be a potential biomarker for efficacy of the treatment.
Funding
Open access funding provided by Karolinska Institute. T. Gülen was supported by grants from the Konsul T.H.C. Bergh Foundation, Sweden; from the Swedish Society of Medicine, Sweden; and through the regional agreement on medical training and clinical research (ALF) between Stockholm County Council and Karolinska Institutet, Stockholm, Sweden.
Author information
Authors and Affiliations
Contributions
The author confirms sole responsibility for the study conception and design, and manuscript preparation.
Corresponding author
Ethics declarations
Conflict of Interest
The author has no financial or nonfinancial relationships to disclose that are relevant to the content of this article.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by the author.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Gulen, T. Using the Right Criteria for MCAS. Curr Allergy Asthma Rep 24, 39–51 (2024). https://doi.org/10.1007/s11882-024-01126-0
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11882-024-01126-0