Abstract
Background
The estimated incidence of testicular torsion (TT) is 4 per 100,000 males under 25 years [1]. Age, region and health insurance status have been associated with a higher risk of orchidectomy following TT [2].
Aims
This study aimed to establish incidence rates for TT in Ireland for the first time. Sociodemographic characteristics were analysed to assess risk factors for undergoing orchidectomy.
Methods
A retrospective analysis of a national database, Hospital In-Patient Enquiry (HIPE), was carried out. Cases of TT treated between 2009 and 2018 were identified. Incidence and age-specific rates were calculated in conjunction with census data. Descriptive statistics, non-parametric tests and logistic regression were used to evaluate risk factors for orchidectomy.
Results
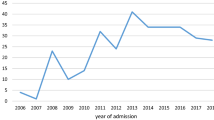
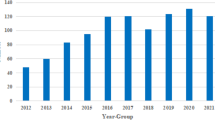
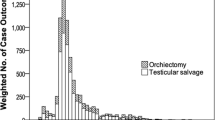
Between 2009 and 2018, 1746 males under 25 years underwent scrotal exploration for TT. The crude incidence was 21.76 per 100,000 population. The age-standardised rate rose from 16.85 per 100,000 in 2009 to 26.31 per 100,000 in 2018. TT was most common in the 10–14 years age-group (n = 766, 43%) with a normal distribution across age-groups. TT most commonly occurred in spring (27.55%, 95% CI 25.46–29.71%), and was least common in summer (21.65%, 95% CI 19.46–23.36%, p < 0.01). Age, lack of private insurance, province of residence and transfer from another hospital were associated with orchidectomy.
Conclusions
The incidence of TT appears to be higher in Ireland than elsewhere. Epidemiological data for TT in Ireland will help inform health policy and clinical guidelines, facilitate comparison with other jurisdictions and improve public awareness. Further research is needed to identify modifiable risk factors that predict treatment outcomes.



Similar content being viewed by others
Data availability
Data and codebook are available upon request.
Notes
Defined as non-elective patients who were admitted to an inpatient bed, irrespective of LOS.
References
Zhao LC, Lautz TB, Meeks JJ, Maizels M (2011) Pediatric testicular torsion epidemiology using a national database: incidence, risk of orchiectomy and possible measures toward improving the quality of care. J Urol 186:2009–2013. https://doi.org/10.1016/j.juro.2011.07.024
Cost NG, Bush NC, Barber TD et al (2011) Pediatric testicular torsion: demographics of national orchiopexy versus orchiectomy rates. In: Journal of Urology. pp 2459–2463
Huang W-Y, Chen Y-F, Chang H-C et al (2013) The incidence rate and characteristics in patients with testicular torsion: a nationwide, population-based study. Acta Paediatr 102:e363–e367. https://doi.org/10.1111/apa.12275
Mansbach JM, Forbes P, Peters C (2005) Testicular torsion and risk factors for orchiectomy. Arch Pediatr Adolesc Med 159:1167–1171. https://doi.org/10.1001/archpedi.159.12.1167
Visser AJ, Heyns CF (2003) Testicular function after torsion of the spermatic cord. BJU Int 92:200–203. https://doi.org/10.1046/j.1464-410x.2003.04307.x
Health Insurance Authority (2018) 2018 Annual Report & Accounts
Organisation for Economic Co-operation and Development (OECD) & European Observatory on Health Systems and Policies, (2019) Ireland: Country Health Profile 2019. European Commission, Brussels
Mueller M, Socha-Dietrich K (2020) Reassessing private practice in public hospitals in Ireland
Central Statistics Office (2020) Databases. https://www.cso.ie/en/databases/. Accessed 29 Dec 2020
Ahmad OB, Boschi-Pinto C, Lopez Christopher AD et al (2001) Age standardization of rates: a new WHO standard
Healthcare Pricing Office (2019) Activity in acute public hospitals in Ireland - 2018 Annual Report. Dublin
Healthcare Pricing Office (2020) Hospital in-patient enquiry scheme (HIPE). http://www.hpo.ie/. Accessed 20 Jun 2020
Lee SM, Huh J-SS, Baek M et al (2014) A nationwide epidemiological study of testicular torsion in Korea. Journal of Korean medical science 29:1684–1687. https://doi.org/10.3346/jkms.2014.29.12.1684
StataCorp (2019) Stata Statistical Software: Release 16
Anderson JB, Williamson RC (1988) Testicular torsion in Bristol: a 25-year review. Br J Surg 75:988–992. https://doi.org/10.1002/bjs.1800751015
Raine JE (2011) An analysis of successful litigation claims in children in England. Arch Dis Child 96:838–840. https://doi.org/10.1136/adc.2011.212555
Selbst SM, Friedman MJ, Singh SB (2005) Epidemiology and etiology of malpractice lawsuits involving children in US emergency departments and urgent care centers. Pediatr Emerg Care 21:165–169
Medical Protection Society (2015) Challenging the cost of clinical negligence: the case for reform. Dublin
Korkes F, dos Cabral PR, A, Alves CDM, et al (2012) Testicular torsion and weather conditions: analysis of 21,289 cases in Brazil. International braz j urol : official journal of the Brazilian Society of Urology 38:222–229
Shukla RB, Kelly DG, Daly L, Guiney EJ (1982) Association of cold weather with testicular torsion. Br Med J (Clin Res Ed) 285:1459–1460. https://doi.org/10.1136/bmj.285.6353.1459
Srinivasan AK, Freyle J, Gitlin JS, Palmer LS (2007) Climatic conditions and the risk of testicular torsion in adolescent males. The Journal of urology 178:2585–8; discussion 2588. https://doi.org/10.1016/j.juro.2007.08.049
MacDonald C, Kronfli R, Carachi R, O’Toole S (2018) A systematic review and meta-analysis revealing realistic outcomes following paediatric torsion of testes. J Pediatr Urol 14:503–509
Peeraully R, Jancauskaite M, Dawes S et al (2019) Does the source of referral affect outcomes for paediatric testicular torsion? Ann R Coll Surg Engl 101:411–414. https://doi.org/10.1308/rcsann.2019.0045
Royal College of Surgeons of England (2016) Commissioning guide: management of paediatric torsion. London
Bayne AP, Madden-Fuentes RJ, Jones EA et al (2010) Factors associated with delayed treatment of acute testicular torsion-do demographics or interhospital transfer matter? J Urol 184:1743–1747. https://doi.org/10.1016/j.juro.2010.03.073
Walsh B, Silles M, O’Neill C (2012) The role of private medical insurance in socio-economic inequalities in cancer screening uptake in ireland. Health Economics (United Kingdom) 21:1250–1256. https://doi.org/10.1002/hec.1784
Ubee SS, Hopkinson V, Srirangam SJ (2014) Parental perception of acute scrotal pain in children. Ann R Coll Surg Engl 96:618–620. https://doi.org/10.1308/003588414X14055925058878
Yap LC, Keenan R, Khan J et al (2018) Parental awareness of testicular torsion amongst Irish parents. World J Urol 36:1485–1488. https://doi.org/10.1007/s00345-018-2269-8
Green C, Stubbs V, Green JS (2020) Public health education initiatives for testicular torsion. Trends in Urology & Men’s Health 11:14–16. https://doi.org/10.1002/tre.775
Nason GJ, Tareen F, McLoughlin D et al (2013) Scrotal exploration for acute scrotal pain: a 10-year experience in two tertiary referral paediatric units. Scandinavian journal of urology 47:418–422. https://doi.org/10.3109/00365599.2012.752403
Acknowledgements
Many thanks to Prof. Jan Van Der Meulen and Dr. Annelieke Driessen at LSHTM, who helped formulate the research design. A special thanks to the staff at University College Dublin School of Public Health who advised on statistical analyses.
Funding
Not applicable.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
Ethical approval was granted by London School of Hygiene and Tropical Medicine Research Ethics Committee (reference number: 22007).
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sugrue, D.D., O’Connor, E. & Davis, N. Testicular torsion in Ireland: a 10-year analysis of incidence and risk of orchidectomy. Ir J Med Sci 191, 2267–2274 (2022). https://doi.org/10.1007/s11845-021-02816-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11845-021-02816-8