Abstract
Background
Cognitive behavioral therapy for insomnia (CBT-I) is the treatment of choice for chronic insomnia. In the metacognitive model of Ong et al., a current model of the pathogenesis of chronic insomnia, sleep-related metacognitions are considered to be an insomnia-promoting factor.
Objective
The objective of this study is to investigate the role of metacognitions in insomnia and CBT‑I. Are metacognitions reduced by CBT-I? Can the pretreatment scores of sleep-related metacognitions predict the effectiveness of the therapy? Does treatment response improve when sleep-related metacognitions are directly addressed?
Materials and methods
A total of 92 persons with chronic insomnia participated in CBT‑I with seven 90-min group sessions. Of these patients, 52 received CBT‑I and 40 received CBT‑I with integrated metacognitive elements (CBT-I + MCE). Sleep-related metacognitions and insomniac complaints were quantified using the Metacognitions Questionnaire—Insomnia (MCQ‑I 20) and the Insomnia Severity Index (ISI).
Results
CBT‑I improved subjective sleep quality (effect sizes d > 2.0) and decreased sleep-related metacognitions (effect sizes d > 0.8). Neither the presence of comorbidities nor the extent of sleep-related metacognitions affected treatment response. Treatment response did not differ between the CBT‑I and CBT-I + MCE groups.
Conclusion
Sleep-related metacognitions seem to play an important role in insomnia etiology but did not predict treatment response. The introduction of elements from metacognitive therapy (MCT) is as effective as the classical CBT‑I and might therefore be considered as an addition to the standard cognitive strategies of CBT‑I.
Zusammenfassung
Hintergrund
Die kognitive Verhaltenstherapie für Insomnie (KVT-I) stellt die Therapie erster Wahl bei chronischer Insomnie dar. Im metakognitiven Modell von Ong et al., einem aktuellen Modell zur Pathogenese der chronischen Insomnie, werden schlafbezogene Metakognitionen als ein insomniebegünstigender Faktor erachtet.
Zielsetzung
Ziel dieser Studie ist es, die Rolle von Metakognitionen bei Insomnie und KVT‑I zu untersuchen. Werden diese durch KVT‑I reduziert? Können die Ausprägung schlafbezogener Metakognitionen vor der Behandlung die Wirksamkeit der KVT‑I vorhersagen? Verbessert sich das Therapieansprechen, wenn die Arbeit an schlafbezogenen Metakognitionen in die KVT‑I integriert werden?
Material und Methoden
Für die Studie nahmen 92 Personen mit chronischer Insomnie an einer KVT‑I mit sieben 90-minütigen Gruppensitzungen teil. Von diesen Patienten erhielten 52 KVT‑I, und 40 erhielten KVT‑I mit integrierten metakognitiven Elementen. Schlafbezogene Metakognitionen und insomnische Beschwerden wurden mittels des Metacognitions Questionnaire – Insomnia (MCQ‑I 20) und des Insomnia Severity Index (ISI) quantifiziert.
Ergebnisse
Die KVT‑I verbesserte die subjektive Schlafqualität (Effektstärken d > 2,0) und verringerte auch die schlafbezogenen Metakognitionen (Effektstärken d > 0,8). Weder das Vorhandensein von Komorbiditäten noch das Ausmaß schlafbezogener Metakognitionen hatte einen Einfluss auf das Therapieansprechen. Das Therapieansprechen unterschied sich nicht zwischen der Gruppe mit KVT‑I und der Gruppe mit KVT‑I mit integrierten metakognitiven Elementen.
Schlussfolgerungen
Schlafbezogene Metakognitionen scheinen bei der Ätiologie der Insomnie eine wichtige Rolle zu spielen, obwohl sie den Therapieerfolg nicht vorhersagen. Die Einführung von Elementen der metakognitiven Therapie (MCT) ist ebenso wirksam wie die klassische KVT‑I und könnten somit als eine Ergänzung zu den bekannten kognitiven Elementen der KVT‑I in Betracht gezogen werden.
Similar content being viewed by others
Insomnia is a sleep disorder with high prevalence. Sleep-related metacognitions are cognitions related to interpretation, monitoring, reacting to, or controlling of sleep-related thoughts. One current insomnia model assigns an important role to sleep-related metacognitions. Cognitive behavioral therapy for insomnia (CBT-I), the first-line treatment for insomnia, was shown to also reduce sleep-related metacognitions. In our research, we studied the interplay between CBT‑I and sleep-related metacognitions.
Insomnia is a sleep disorder characterized by problems in sleep initiation, maintenance, duration, and quality—despite adequate opportunity—leading to impaired daytime functioning [1]. Chronic insomnia, with symptoms persisting for over 3 months at least 3 days a week [1], shows a prevalence of between 5% and 15% in the general population [12, 18, 23].
Spielman’s 3P model describes the predisposing, precipitating, and perpetuating factors resulting in difficulties in sleep initiation and maintenance and their improvement by behavioral interventions [25]. Morin’s cognitive behavioral model of insomnia [14] displays the vicious circle of insomnia containing hyperarousal, dysfunctional cognitions, maladaptive behavior, and daytime consequences, suggesting that cognitive strategies be appended to insomnia therapy [14]. The attention–intention–effort (AIE) pathway of Espie et al. [6] proposes that sleep initiates automatically in healthy individuals, whereas in psychophysiological insomnia, giving attention to sleep, actively intending to fall asleep, and putting effort into it result in inhibition of the natural de-arousal [6].
Sleep-related cognitions are unrealistic expectations, erroneous beliefs, or biases about sleep [16]. Sleep-related metacognitions, on the other hand, are the reaction to and interpretation, monitoring, or control of sleep-related cognitions [8, 31]. The metacognitive model by Ong et al. [20] adds these metacognitive processes to the cognitive arousal theories of insomnia [22] as so-called secondary arousal. In conclusion, this approach focuses less on restructuring the content of dysfunctional sleep-related cognitions but rather on changing one’s handling of them [24, 31]. Patients suffering from insomnia show more sleep-related metacognitions than healthy controls [21] or patients with other sleep disorders [21, 24].
Cognitive behavioral therapy for insomnia (CBT-I) is a very effective insomnia treatment [9,10,11, 19, 28]. It was also shown to reduce sleep-related metacognitions in a former study [8]. CBT‑I in the study was performed according to Espie [5], consisted of seven group sessions of 90 min each, and reduced sleep-related metacognitions (MCQ-I) in the pretreatment to posttreatment comparison with a large effect size (d = −1.186) [8]. Regarding factors influencing CBT‑I effectiveness, previous reports found no effect of age and gender; however, current psychiatric comorbidity may predict less effectiveness [27].
In our research, we aimed to investigate if and to what extent CBT‑I can reduce sleep-related metacognitions, whether the baseline level of metacognitions can predict the outcome of CBT‑I, and whether a therapy integrating elements of metacognitive therapy into CBT‑I improves its outcome.
Materials and methods
Participants
A total of 92 patients with chronic insomnia disorder diagnosed according to the third edition of the International Classification of Sleep Disorders (ICSD‑3; mean age = 49.4; standard deviation [SD] = 12.01) participated in group therapy for chronic insomnia. Demographic information, comorbidities, and use of sleep medication are displayed in Table 1. Antidepressant medication in the patient group without affective comorbidity was used as sleep-promoting medication. A subgroup analysis was performed for those 69 insomnia patients without any psychiatric or sleep-related comorbidity (mean age [M] = 50.20, SD = 12.16). There was a significant age difference (total sample: t(90) = −2.65, p = 0.010; subsample without comorbidities: t(67) = −2.68, p = 0.009), with women (total sample: M = 51.31, SD = 11.72, N = 68; subsample without comorbidities: M = 52.26, SD = 11.45, N = 53) being older than men (total sample: M = 44.00, SD = 11.37, N = 24; subsample without comorbidities: M = 43.38, SD = 12.29, N = 16).
Therapy
CBT‑I was conducted according to [17]. It consisted of seven 90-minute group sessions. The first four sessions were held on a weekly basis, the fifth and sixths session each after 2 weeks. The last session after 8 weeks of therapy is here referred to as “post visit.” A seventh follow-up visit was offered 3 months after the post visit (here referred to as “follow-up visit”). A licensed specialist in psychiatry and psychotherapy, certified in sleep medicine and with a diploma in metacognitive therapy (MCT) from the MCT Institute, conducted the group sessions. The therapy consisted of the development of a disease model, sleep restriction monitored by sleep diaries, psychoeducation about sleep-related topics, restructuring of dysfunctional sleep-related beliefs, relaxation techniques, and exchange of experiences during therapy between the group members.
For 40 out of 92 patients with insomnia receiving treatment from 2019 onwards, CBT‑I integrated elements MCT. Approximately 25% of the total therapy time was allocated to metacognitive interventions. The allocated time was obtained by omission of restructuring of dysfunctional sleep-related beliefs and reducing time spent on psychoeducation about sleep architecture and relaxation techniques from the original program. Sleep-related cognitions and metacognitions were collected by the group members, and a metacognitive case formulation inspired by the generalized anxiety disorder case formulation from Wells was developed with the group [31]. The metacognitive interventions in subsequent therapy sessions referred to this case formulation. It contained sleep-related cognitions like “If I don’t sleep now, I won’t be able to be active tomorrow,” sleep-related metacognitions like “Thinking in bed means I won’t get to sleep,” and the cognitive, emotional, behavioral, and physiological reactions to them. The technique of “detached mindfulness” was introduced. Behavioral experiments and exercises were used to show how to let go of thoughts without giving them further attention. Metaphors were introduced to facilitate its use. Another technique is postponing worrying and rumination. The purpose of this technique is to reduce dysfunctional thought processes and show that thought processes are controllable, i.e., to challenge the negative metacognitive belief of uncontrollability of excessive thinking [31]. The goal of another technique, the “attention training technique,” is to focus attention outward, away from dysfunctional thought processes [31].
Questionnaires
The Insomnia Severity Index (ISI) [2, 14, 15] consists of seven items covering the nature and severity of insomniac complaints, both at nighttime and during the daytime, during the previous 2 weeks on a five-point Likert scale ranging from 0 to 4, with 4 indicating a very severe problem. A sum score is calculated reaching values between 0 and 28, with higher values representing more insomnia symptoms: a score of 0–7 indicates no clinically significant insomnia, 8–14 subthreshold insomnia, 15–21 clinical insomnia (moderate severity), and 22–28 clinical insomnia (severe) [2, 15]. The German version was used [4]. In the current study the reliability coefficients (Cronbach’s alpha) for the three measurement points were 0.711 (pretest), 0.798 (posttest), and 0.809 (follow-up).
The Metacognitions Questionnaire—Insomnia was originally created by Waine et al. [30] and includes 60 questions about sleep-related metacognitions [30]. Each question is answered on a four-point Likert scale from “do not agree” (1) to “agree very much” (4). A sum score of all items is calculated, with higher values representing more maladaptive sleep-related metacognitions [30]. A short form of the questionnaire, the MCQ-I 20, was developed by Schredl [24]. Three certified MCT therapists independently agreed on 20 translated items that unambiguously captured sleep-related metacognitions, e.g., “Before I fall asleep, I must get things sorted in my mind.” The MCQ-I 20 showed high internal consistency (rtt = 0.906) and high test–retest reliability (r = 0.916). The sum scores were previously shown to be higher for patients diagnosed with insomnia disorder as well as for those with nightmare disorder and depression disorder [24]. In the current study, the reliability coefficients (Cronbach’s alpha) for the two measurement points were 0.885 (pretest) and 0.818 (posttest).
Two questions related to the uncontrollability of excessive thinking were presented at the beginning and after the intervention. These questions were adapted from the CAS module “cognitive attentional syndrome” published in [31]. The questions used were 1) “Nocturnal chains of thoughts are uncontrollable” and 2) “Thought circles happen automatically.” Participants rated their level of conviction in these statements on a scale of 0 to 100, with 0 representing “I don’t believe in this belief at all” and 100 representing “I am absolutely convinced that this belief is true.”
Procedures
The CBT‑I program was offered to patients who underwent clinical diagnostics in the sleep laboratory of the Central Institute of Mental Health Mannheim, Germany, and who had received a diagnosis of chronic insomnia disorder. Each group consisted of 4 to 9 patients. The therapy was carried out between March 2015 and November 2020, whereby 52 patients received standard CBT‑I therapy and 40 patients received CBT‑I with integrated metacognitive elements.
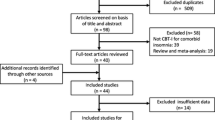
Patients completed paper–pencil self-assessment questionnaires at the beginning of the therapy (pre), after 8 weeks (post), and after 20 weeks (follow-up visit; Fig. 1). If the patients were not able to join a meeting, they were asked to send the completed questionnaires. Not all participants completed the ISI at all timepoints. Some completed it only at the pre visit (total sample n = 11; sample without comorbidities n = 6), at the pre and post visits (total sample n = 23; sample without comorbidities n = 20), at the pre and follow-up visits (total sample n = 22; sample without comorbidities n = 19), and some completed the ISI at pre, post, and follow-up visits (total sample n = 21; sample without comorbidities n = 13). The effect of metacognitive interventions was evaluated by presenting two questions related to the uncontrollability of excessive thinking at the beginning and after the intervention (only in the CBT-I + MCE group).
Visits over time and completed questionnaires. Therapy duration was 8 weeks followed by a 3-month follow-up phase. Questionnaires were completed before the start of the therapy (Pre), after the therapy (Post), and at the end of follow-up (Follow-up). The Insomnia Severity Index (ISI) was completed at all timepoints and the short version Metacognitions Questionnaire—Insomnia (MCQ‑I 20) was completed at pre and post visits. Not all participants completed the questionnaires at all timepoints
The Ethics Committee II of the Medical Faculty Mannheim/University Heidelberg approved the retrospective analysis of the clinical data.
Statistical analysis
Data analysis was performed using the SPSS statistical software package, version 27 (IBM Corp., Armonk, NY, USA). Paired t-tests were used to test differences in mean scores comparing the pre, post, and follow-up timepoints. For the ISI, Bonferroni adjustment for multiple comparisons was performed. Cohen’s d was calculated between the three timepoints [3].
Associations between patient-reported psychometric measures (ISI, MCQ-I 20) and the demographic data (age, gender, comorbidities) at the pre visit were calculated using the Pearson correlation coefficient.
Mixed linear models were used to assess interactions of demographics or the pretreatment MCQ-I 20 score and therapy effectiveness based on the ISI scores over time (ISI score as dependent variable and time as the fixed factor, i.e., pre, post, follow-up). Demographic data (age, gender, comorbidities) and the pretreatment MCQ-I 20 score were set as covariates. The random factor was the subjects ID. We ran multiple linear models with one covariate in each model. For the treatment comparison of the CBT‑I (CBT-I) with the CBT‑I with integrated metacognitive elements (CBT-I+MCE), mixed linear models were calculated.
Results
Associations between ISI, MCQ-I, and other variables at baseline
The ISI showed a medium-size statistically significant correlation with the MCQ-I 20 score in the total sample (patients with and without comorbidities; r(54) = 0.46, p = < 0.001) and a high correlation in the subsample without comorbidities (r(41) = 0.57, p = < 0.001). There was no correlation between the baseline ISI or MCQ-I 20 with demographic data (age, gender, comorbidities). Women were slightly older than men (small correlation in the total sample, medium correlation in the subsample without comorbidities).
Changes in insomnia severity and metacognitions between pre, post, and follow-up visits
Statistical analyses are summarized in Tables 2 and 3. Compared to the pre visit, the ISI scores were significantly lower at the post visit and at the follow-up visit (large effect sizes). Comparing the post to the follow-up visit, the ISI score also became significantly lower over time, with medium (total sample) or large (without comorbidities) effect sizes. The MCQ-I 20 scores also displayed a significant reduction between the pre and the post visits with large effect sizes. The degree of conviction regarding the uncontrollability of excessive thinking decreased significantly upon comparing measures assessed prior to and after the metacognitive intervention (“Uncontrollable nocturnal chains of thoughts”: M = 49.17, SD = 24.66 at pre and M = 22.50, SD = 20.27 at post, Wilcoxon test: z = −3.7; p < 0.0001; “Automatic thought circles”: M = 58.75, SD = 32.21 at pre and M = 29.58, SD = 22.36 at post, Wilcoxon test: z = −3.8; p < 0.0001).
In addition to the abovementioned improvements in questionnaire data, several participants stopped their sleep medication (total sample: n = 2; subsample without comorbidities: n = 1) or their sedative antidepressants (total sample: n = 8; subsample without comorbidities: n = 6) during the course of therapy.
Predictors of therapy effectiveness
Interactions between time and the covariates determine if therapy effectiveness is based on a given predictor. There were no significant interactions (Table 4). On the other hand, the fixed factor time was significant in all calculated models except for the MCQ-I 20 in the subsample without comorbidities. In both samples, the covariate pretreatment MCQ-I 20 was statistically significant.
Comparison of CBT-I and CBT-I+MCE
Therapy outcome did not differ between the treatment conditions CBT‑I only and CBT‑I with metacognitive elements (Table 5). The fixed factor time was significant in all calculated models, replicating the findings that the therapy worked. The summed-up data between the two compared treatment groups did not differ.
Discussion
Our study shows that CBT‑I results in a decrease in sleep-related metacognitions. Therapy outcome was not dependent on the level of pretreatment sleep-related metacognitions. Also, CBT‑I and CBT‑I with integrated metacognitive elements were equally effective.
Prior to discussing the findings in detail, a few methodological issues will be addressed. The study was carried out in a clinical setting over several years. Therefore, not all questionnaires were completed at all timepoints, as there were changes in the procedures over time. On the other hand, the real-world character of the data offered the possibility to control for comorbidities, and the decrease in ISI scores due to therapy showed large effect sizes—fitting very well with a previous meta-analysis regarding the efficacy of CBT‑I [9, 28].
In addition to the reduction of insomnia symptoms measured by the ISI, CBT‑I also reduced the MCQ‑I scores with large effect sizes. Our effect size of about d = 0.80 was somewhat higher than the effect size (d = −0.525) reported by Galbiati et al. [8]. Thus, the improvement in sleep quality (the primary aim of CBT-I) is paralleled by a reduction in dysfunctional sleep-related metacognitions. As no difference between classical CBT‑I and CBT‑I including metacognitive elements was observed, one might speculate that the effect on dysfunctional sleep-related metacognitions may be explained by a general improvement in sleep. However, repeated ratings on the conviction about uncontrollability of excessive thought processes showed that the metacognitive interventions worked in the sleep therapy setting. It would be very interesting to test whether purely metacognitive approaches to insomnia without applying techniques like sleep restriction would also yield large effect sizes regarding subjective sleep quality. According to the metacognitive model of Ong et al., a high level of dysfunctional sleep-related metacognitions can cause secondary arousal, which can result in a perpetuation of negative behavior and emotions and therefore perpetuate the vicious cycle of chronic insomnia. Within this framework, an effect of metacognitive therapy [31] would be expected.
The literature regarding demographic predictors of CBT‑I effectiveness shows no effect of gender or age [7, 26, 29], but current psychiatric conditions seem to predict lower therapy effectiveness [27]. This was not confirmed by our study. In our clinical setting, CBT‑I was highly effective in patients suffering from insomnia disorder only, as well as in patients with insomnia disorder plus comorbid mental disorders. We did not see an effect of the level of pretreatment sleep-related metacognitions on therapy outcome. This finding is interesting in the context of the model of Ong et al., showing that even though sleep-related metacognitions play a role in insomnia etiology, their baseline level had no effect on therapy outcome.
For 40 out of 92 participants, classical CBT‑I was complemented by metacognitive strategies. The rationale behind this was that the classical cognitive restructuring of thoughts such as “If my insomnia continues like this, I will get sick” [17] was not seen as satisfactory, especially as recent research [13] has shown that chronic insomnia has many negative health consequences. That is, the content of the thought is correct, and therefore, it could be beneficial for patients to focus on dealing with sleep-related cognitions in a constructive way instead of questioning the plausibility of sleep-related cognitions. As stated above, investigating the effects of MCT alone and comparing it to classical CBT‑I would give us a better understanding about the interplay between dysfunctional sleep-related metacognitions and general sleep quality, and provide support for the metacognitive model of Ong et al. [20]. It would also be interesting to study whether changes in sleep-related metacognitions during therapy predict long-term improvements. In this study, the introduction of MCT elements was as effective as classical CBT‑I; thus, the findings might stimulate a “modernization” of CBT‑I regarding the techniques dealing with sleep-related cognitions and metacognitions.
Conclusion
To summarize, a better understanding of the role of sleep-related metacognitions within the insomnia model might be useful to adapt the well-established therapeutic techniques for treating insomnia. One possible option is incorporation of metacognitive elements. In addition to studying the efficacy of these new approaches, it would also be very interesting to see whether a metacognitive approach to sleep-related cognitions is perceived as more positive by the patients than the classical technique of cognitive restructuring.
Practical conclusion
-
Cognitive behavioral therapy for insomnia (CBT-I) decreases sleep-related metacognitions.
-
The therapy outcome did not depend on the level of pretreatment sleep-related metacognitions.
-
Introducing elements of metacognitive therapy (MCT) was as effective as classical CBT‑I.
-
The introduction of MCT elements might be a valuable addition to the standard cognitive strategies of CBT‑I.
References
American Academy of Sleep Medicine (2014) International classification of sleep disorders. (ICSD-3). American Academy of Sleep Medicine, Darien
Bastien C (2001) Validation of the insomnia severity index as an outcome measure for insomnia research. Sleep Med 4:297–307
Cohen J (1988) Statistical power analysis for the behavioral sciences, 2nd edn. Erlbaum, Hillsdale, NJ
Dieck A, Morin CM, Backhaus J (2018) A German version of the insomnia severity index. Somnologie 1:27–35
Espie CA (1991) The psychological treatment of insomnia. Wiley, Chichester
Espie CA, Broomfield NM, MacMahon KMA et al (2006) The attention-intention-effort pathway in the development of psychophysiologic insomnia: a theoretical review. Sleep Med Rev 4:215–245
Espie CA, Inglis SJ, Harvey L (2001) Predicting clinically significant response to cognitive behavior therapy for chronic insomnia in general medical practice: analysis of outcome data at 12 months posttreatment. J Consult Clin Psychol 1:58–66
Galbiati A, Sforza M, Scarpellino A et al (2021) “Thinking about thinking” in insomnia disorder: the effect of cognitive-behavioral therapy for insomnia on sleep-related metacognition. Front Psychol. https://doi.org/10.3389/fpsyg.2021.705112
Geiger-Brown JM, Rogers VE, Liu W et al (2015) Cognitive behavioral therapy in persons with comorbid insomnia: a meta-analysis. Sleep Med Rev 23:54–67. https://doi.org/10.1016/j.smrv.2014.11.007
Irwin MR, Cole JC, Nicassio PM (2006) Comparative meta-analysis of behavioral interventions for insomnia and their efficacy in middle-aged adults and in older adults 55+ years of age. Health Psychol 1:3–14
Koffel EA, Koffel JB, Gehrman PR (2015) A meta-analysis of group cognitive behavioral therapy for insomnia. Sleep Med Rev 19:6–16. https://doi.org/10.1016/j.smrv.2014.05.001
LeBlanc M, Mérette C, Savard J et al (2009) Incidence and risk factors of insomnia in a population-based sample. Sleep 8:1027–1037
Medic G, Wille M, Hemels ME (2017) Short- and long-term health consequences of sleep disruption. Nat Sci Sleep 9:151–161
Morin CM (1993) Insomnia. Psychological assessment and management, 1st edn. Guilford, New York
Morin CM, Belleville G, Bélanger L et al (2011) The insomnia severity index: psychometric indicators to detect insomnia cases and evaluate treatment response. Sleep 5:601–608
Morin CM, Vallières A, Ivers H (2007) Dysfunctional beliefs and attitudes about sleep (DBAS): validation of a brief version (DBAS-16). Sleep 11:1547–1554
Müller TH, Paterok B (2010) Schlaftraining. Ein Therapiemanual zur Behandlung von Schlafstörungen, 2nd edn. Hogrefe, Göttingen, Bern, Wien
Ohayon MM (2002) Epidemiology of insomnia: what we know and what we still need to learn. Sleep Med Rev 2:97–111
Okajima I, Komada Y, Inoue Y (2011) A meta-analysis on the treatment effectiveness of cognitive behavioral therapy for primary insomnia. Sleep Biol Rhythms 1:24–34
Ong JC, Ulmer CS, Manber R (2012) Improving sleep with mindfulness and acceptance: a metacognitive model of insomnia. Behav Res Ther 11:651–660
Palagini L, Ong JC, Riemann D (2017) The mediating role of sleep-related metacognitive processes in trait and pre-sleep state hyperarousal in insomnia disorder. J Psychosom Res 99:59–65. https://doi.org/10.1016/j.jpsychores.2017.03.001
Riemann D, Spiegelhalder K, Feige B et al (2010) The hyperarousal model of insomnia: a review of the concept and its evidence. Sleep Med Rev 1:19–31
Schlack R, Hapke U, Maske U et al (2013) Häufigkeit und Verteilung von Schlafproblemen und Insomnie in der deutschen Erwachsenenbevölkerung: Ergebnisse der Studie zur Gesundheit Erwachsener in Deutschland (DEGS1). Bundesgesundheitsblatt Gesundheitsforschung Gesundheitsschutz 5–6:740–748
Schredl M, Schackert M, Feld GB et al (2021) Ein Fragebogen zur Erfassung von schlafbezogenen Metakognitionen: Deutsche Kurzform des MCQ‑I. Somnologie 3:205–211
Spielman AJ, Caruso LS, Glovinsky PB (1987) A behavioral perspective on insomnia treatment. Psychiatr Clin North Am 4:541–553
Troxel WM, Conrad TS, Germain A et al (2013) Predictors of treatment response to brief behavioral treatment of insomnia (BBTI) in older adults. J Clin Sleep Med 12:1281–1289
van de Laar M, Pevernagie D, van Mierlo P et al (2015) Psychiatric comorbidity and aspects of cognitive coping negatively predict outcome in cognitive behavioral treatment of psychophysiological insomnia. Behav Sleep Med 2:140–156
van der Zweerde T, Bisdounis L, Kyle SD et al (2019) Cognitive behavioral therapy for insomnia: a meta-analysis of long-term effects in controlled studies. Sleep Med Rev 48:101208. https://doi.org/10.1016/j.smrv.2019.08.002
Van Houdenhove L, Buyse B, Gabriëls L et al (2011) Treating primary insomnia: clinical effectiveness and predictors of outcomes on sleep, daytime function and health-related quality of life. J Clin Psychol Med Settings 3:312–321
Waine J, Broomfield NM, Banham S et al (2009) Metacognitive beliefs in primary insomnia: developing and validating the metacognitions questionnaire—insomnia (MCQ-I). J Behav Ther Exp Psychiatry 1:15–23
Wells A (2011) Metakognitive Therapie bei Angststörungen und Depression, 1st edn. Beltz, Weinheim, Basel
Funding
Open Access funding enabled and organized by Projekt DEAL.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
A.-L. Jenewein, M. Schredl and C. Schilling declare that they have no competing interests.
All procedures followed were in accordance with the ethical standard of the responsible ethics committee and the Helsinki Declaration of 1975 (in its most recently amended version). The local ethics committee approved the retrospective analyses of the clinical data.
Additional information

Scan QR code & read article online
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Jenewein, AL., Schredl, M. & Schilling, C. Sleep-related metacognitions and cognitive behavioral therapy for insomnia. Somnologie 27, 109–116 (2023). https://doi.org/10.1007/s11818-023-00404-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11818-023-00404-9