Abstract
Purpose
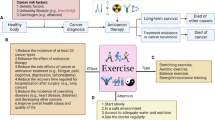
Since physical activity (PA) has been shown to be associated with better prognosis and quality of life (QOL) in colorectal cancer (CRC) patients, this study focuses on the barriers of PA among CRC survivors.
Methods
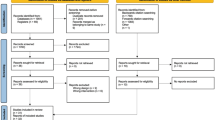
This study is based on a population-based study from Germany of 1343 women and men, diagnosed with CRC between 2003 and 2008 and being alive five years later. Multivariable logistic regression was used to explore associations between baseline as well as five-year follow-up (5YFU) characteristics and physical inactivity (PIA) at 5YFU. Quartiles were calculated based on metabolic equivalent hours per week of PA at baseline and at 5YFU. Participants in quartile 1 were defined as physically inactive, and patients in quartile 2 to quartile 4 were defined as physically active.
Results
Cancer-specific factors such as having a stoma (odds ratio (OR) = 1.51, 95% confidence interval (CI) = 1.12–2.04), demographic factors such as living in a small town or city (OR = 1.46, 95% CI = 1.05–2.02; OR = 1.42, 95% CI = 1.01–2.02), older age (OR = 1.44, 95% CI = 0.80–2.58), or being divorced (OR = 1.72, 95% CI = 0.96–3.07), as well as lifestyle factors such as being a current smoker (OR = 1.54, 95% CI = 1.04–2.29) or being obese (OR = 1.43, 95% CI = 0.96–2.13) were associated with PIA at 5YFU. Subgroup analyses showed that the association between body mass index and PIA was stronger in women than in men. Baseline PA was identified as a strong predictor of PIA at 5YFU.
Conclusions
Findings suggest that predominately patients with a stoma, patients living in a more populated area, being older, divorced, a current smoker, or obese were more likely to be physically inactive and therefore could be targeted to be more physically active.
Implications for Cancer Survivors
Addressing barriers for PA might help to develop specific, individually tailored PA interventions to overcome PIA and improve the long-term outcome of CRC survivors.
Similar content being viewed by others
References
Ferlay J, Soerjomataram I, Dikshit R, Eser S, Mathers C, Rebelo M, et al. Cancer incidence and mortality worldwide: sources, methods and major patterns in GLOBOCAN 2012. Int J Cancer. 2015;136(5):E359–86.
Krebs in Deutschland für 2013/2014. 11. Ausgabe. Robert Koch-Institut (Hrsg) und die Gesellschaft der epidemiologischen Krebsregister in Deutschland e.V. (Hrsg). Berlin, 2017.
Brenner H, Stegmaier C, Ziegler H. Long-term survival of cancer patients in Germany achieved by the beginning of the third millennium. Ann Oncol: Official Journal of the European Society for Medical Oncology/ESMO. 2005;16(6):981–6.
Jansen L, Castro FA, Gondos A, Krilaviciute A, Barnes B, Eberle A, et al. Recent cancer survival in Germany: an analysis of common and less common cancers. Int J Cancer. 2015;136(11):2649–58.
Walter V, Jansen L, Knebel P, Chang-Claude J, Hoffmeister M, Brenner H. Physical activity and survival of colorectal cancer patients: population-based study from Germany. Int J Cancer. 2017;140(9):1985–97.
Schmid D, Leitzmann MF. Association between physical activity and mortality among breast cancer and colorectal cancer survivors: a systematic review and meta-analysis. Ann Oncol: Official Journal of the European Society for Medical Oncology/ESMO. 2014;25(7):1293–311.
Denlinger CS, Engstrom PF. Colorectal cancer survivorship: movement matters. Cancer Prevention Research (Philadelphia, PA). 2011;4(4):502–11.
Grimmett C, Bridgewater J, Steptoe A, Wardle J. Lifestyle and quality of life in colorectal cancer survivors. Qual Life Res Int J Qual Life Asp Treat Care Rehab. 2011;20(8):1237–45.
Mols F, Beijers AJ, Vreugdenhil G, Verhulst A, Schep G, Husson O. Chemotherapy-induced peripheral neuropathy, physical activity and health-related quality of life among colorectal cancer survivors from the PROFILES registry. J Cancer Surviv: Res Prac. 2015;9(3):512–22.
Kushi LH, Doyle C, McCullough M, Rock CL, Demark-Wahnefried W, Bandera EV, et al. American Cancer Society guidelines on nutrition and physical activity for cancer prevention: reducing the risk of cancer with healthy food choices and physical activity. CA Cancer J Clin. 2012;62(1):30–67.
Courneya KS, Friedenreich CM, Quinney HA, Fields AL, Jones LW, Vallance JK, et al. A longitudinal study of exercise barriers in colorectal cancer survivors participating in a randomized controlled trial. Ann Behav Med: Publ Soc Behav Med. 2005;29(2):147–53.
van Putten M, Husson O, Mols F, Luyer MDP, van de Poll-Franse LV, Ezendam NPM. Correlates of physical activity among colorectal cancer survivors: results from the longitudinal population-based profiles registry. Supportive Care in Cancer: Official Journal of the Multinational Association of Supportive Care in Cancer. 2016;24(2):573–83.
Lynch BM, Owen N, Hawkes AL, Aitken JF. Perceived barriers to physical activity for colorectal cancer survivors. Support Care Cancer: Official Journal of the Multinational Association of Supportive Care in Cancer. 2010;18(6):729–34.
Chambers SK, Lynch BM, Aitken J, Baade P. Relationship over time between psychological distress and physical activity in colorectal cancer survivors. J Clin Oncol: Official Journal of the American Society of Clinical Oncology. 2009;27(10):1600–6.
McGowan EL, Speed-Andrews AE, Rhodes RE, Blanchard CM, Culos-Reed SN, Friedenreich CM, et al. Sport participation in colorectal cancer survivors: an unexplored approach to promoting physical activity. Support Care Cancer: Official Journal of the Multinational Association of Supportive Care in Cancer. 2013;21(1):139–47.
Fisher A, Wardle J, Beeken RJ, Croker H, Williams K, Grimmett C. Perceived barriers and benefits to physical activity in colorectal cancer patients. Support Care Cancer: Official Journal of the Multinational Association of Supportive Care in Cancer. 2016;24(2):903–10.
Brenner H, Chang-Claude J, Seiler CM, Rickert A, Hoffmeister M. Protection from colorectal cancer after colonoscopy: a population-based, case-control study. Ann Intern Med. 2011;154(1):22–30.
Hoffmeister M, Jansen L, Rudolph A, Toth C, Kloor M, Roth W, et al. Statin use and survival after colorectal cancer: the importance of comprehensive confounder adjustment. J Natl Cancer Inst. 2015;107(6):djv045.
Jansen L, Hoffmeister M, Arndt V, Chang-Claude J, Brenner H. Stage-specific associations between beta blocker use and prognosis after colorectal cancer. Cancer. 2014;120(8):1178–86.
Craig CL, Marshall AL, Sjostrom M, Bauman AE, Booth ML, Ainsworth BE, et al. International physical activity questionnaire: 12-country reliability and validity. Med Sci Sports Exerc. 2003;35(8):1381–95.
Ainsworth BE, Haskell WL, Herrmann SD, Meckes N, Bassett DR Jr, Tudor-Locke C, et al. 2011 Compendium of physical activities: a second update of codes and MET values. Med Sci Sports Exerc. 2011;43(8):1575–81.
Chastin SF, Buck C, Freiberger E, Murphy M, Brug J, Cardon G, et al. Systematic literature review of determinants of sedentary behaviour in older adults: a DEDIPAC study. Int J Behav Nutr Phys Act. 2015;12:127.
Koeneman MA, Verheijden MW, Chinapaw MJ, Hopman-Rock M. Determinants of physical activity and exercise in healthy older adults: a systematic review. Int J Behav Nutr Phys Act. 2011;8:142.
Van Roekel EH, Bours MJ, Breedveld-Peters JJ, Meijer K, Kant I, Van Den Brandt PA, et al. Light physical activity is associated with quality of life after colorectal cancer. Med Sci Sports Exerc. 2015;47(12):2493–503.
Thraen-Borowski KM, Trentham-Dietz A, Edwards DF, Koltyn KF, Colbert LH. Dose-response relationships between physical activity, social participation, and health-related quality of life in colorectal cancer survivors. J Cancer Surviv: Res Prac. 2013;7(3):369–78.
Acknowledgements
The authors thank Ute Handte-Daub, Ansgar Brandhorst, and Petra Bächer for their excellent technical assistance. The authors thank the study participants and the interviewers who collected the data. The authors also thank the following hospitals and cooperating institutions that recruited patients for this study: Chirurgische Universitätsklinik Heidelberg, Klinik am Gesundbrunnen Heilbronn, St. Vincentiuskrankenhaus Speyer, St. Josefskrankenhaus Heidelberg, Chirurgische Universitätsklinik Mannheim, Diakonissenkrankenhaus Speyer, Krankenhaus Salem Heidelberg, Kreiskrankenhaus Schwetzingen, St. Marienkrankenhaus Ludwigshafen, Klinikum Ludwigshafen, Stadtklinik Frankenthal, Diakoniekrankenhaus Mannheim, Kreiskrankenhaus Sinsheim, Klinikum am Plattenwald Bad Friedrichshall, Kreiskrankenhaus Weinheim, Kreiskrankenhaus Eberbach, Kreiskrankenhaus Buchen, Kreiskrankenhaus Mosbach, Enddarmzentrum Mannheim, Kreiskrankenhaus Brackenheim, and Cancer Registry of Rhineland-Palatinate, Mainz.
Funding
This work was supported by the German Research Council (BR 1704/6-1, BR 1704/6-3, BR 1704/6-4, CH 117/1-1) and the German Federal Ministry of Education and Research (01KH0404, 01ER0814, 01ER0815, 01ER1505A, and 01ER1505B).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Electronic supplementary material
Supplementary Table 1
(DOCX 37 kb)
Rights and permissions
About this article
Cite this article
Eyl, R.E., Koch-Gallenkamp, L., Jansen, L. et al. Potential determinants of physical inactivity among long-term colorectal cancer survivors. J Cancer Surviv 12, 679–690 (2018). https://doi.org/10.1007/s11764-018-0705-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11764-018-0705-9