Abstract
Objective
Prolonged air leakage (PAL) is the most common postoperative complication after segmentectomy and chemical pleurodesis (CP) is one of the common procedures for managing PAL. However, the impact of CP on postoperative pulmonary function remains unclear.
Methods
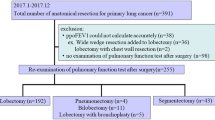
We performed a propensity score matching analysis for postoperative pulmonary function in lung cancer patients who underwent segmentectomy. The percentage of postoperative functional change of forced vital capacity (δFVC) and forced expiratory volume in 1 s (δFEV1.0) at postoperative 6 and 12 months were compared between patients who were managed for PAL by CP (CP group, n = 21) and those who did not receive CP (non-CP, n = 21). The predicted δFVC and δFEV1.0 after segmentectomy and lobectomy were also assessed to evaluate the loss of preserved lung function.
Results
δFVC and δFEV1.0 in the CP group were confirmed by a significantly larger decline in postoperative pulmonary function than that seen in the non-CP group at postoperative 6 and 12 months (δFVC at 6 months, − 21.1% versus − 5.1%, − 20.8% versus − 6.8% at 12 months, δFEV1.0 at 6 months, − 19.1% versus − 7.2%, − 19.6% versus − 9.7%, at 12 months, p < 0.05 respectively). Both δFVC and δFEV1.0 in the CP group were significantly lower than those predicted after segmentectomy (p < 0.01). They were not statistically different from the values predicted if lobectomy was performed.
Conclusions
CP after segmentectomy caused the same amount of loss in pulmonary function that was predicted if lobectomy was performed. The benefit of segmentectomy compared to lobectomy for preservation of pulmonary function is impaired by CP.




Similar content being viewed by others
Abbreviations
- CP:
-
Chemical pleurodesis
- FVC:
-
Forced vital capacity
- FEV1.0 :
-
Forced expiratory volume in 1 s
- PAL:
-
Prolonged air leakage
References
Okada M, Koike T, Higashiyama M, Yamato Y, Kodama K, Tsubota N. Radical sublobar resection for small-sized non-small cell lung cancer: a multicenter study. J Thorac Cardiovasc Surg. 2006;132:769–75.
Landreneau RJ, Normolle DP, Christie NA, Awais O, Wizorek JJ, Abbas G, et al. Recurrence and survival outcomes after anatomic segmentectomy versus lobectomy for clinical stage I non-small-cell lung cancer: a propensity-matched analysis. J Clin Oncol. 2014;32:2449–55.
Kodama K, Higashiyama M, Okami J, Tokunaga T, Imamura F, Nakayama T, et al. Oncologic Outcomes of Segmentectomy Versus Lobectomy for Clinical T1a N0 M0 Non-Small Cell Lung Cancer. Ann Thorac Surg. 2016;101:504–11.
Bedetti B, Bertolaccini L, Rocco R, Schmidt J, Solli P, Scarci M. Segmentectomy versus lobectomy for stage I non-small cell lung cancer: a systematic review and meta-analysis. J Thorac Dis. 2017;9:1615–23.
Keenan RJ, Landreneau RJ, Maley RH Jr, Singh D, Macherey R, Bartley S, et al. Segmental resection spares pulmonary function in patients with stage I lung cancer. Ann Thorac Surg. 2004;78:228–33 discussion 228–233.
Harada H, Okada M, Sakamoto T, Matsuoka H, Tsubota N. Functional advantage after radical segmentectomy versus lobectomy for lung cancer. Ann Thorac Surg. 2005;80:2041–5.
Charloux A, Quoix E. Lung segmentectomy: does it offer a real functional benefit over lobectomy? Eur Respir Rev. 2017;26:170079.
Suzuki K, Saji H, Aokage K, Watanabe SI, Okada M, Mizusawa J, et al. Comparison of pulmonary segmentectomy and lobectomy: safety results of a randomized trial. J Thorac Cardiovasc Surg. 2019;158:895–907.
Shapiro M, Weiser TS, Wisnivesky JP, Chin C, Arustamyan M, Swanson SJ. Thoracoscopic segmentectomy compares favorably with thoracoscopic lobectomy for patients with small stage I lung cancer. J Thorac Cardiovasc Surg. 2009;137:1388–93.
Brunelli A, Xiume F, Al Refai M, Salati M, Marasco R, Sabbatini A. Air leaks after lobectomy increase the risk of empyema but not of cardiopulmonary complications: a case-matched analysis. Chest. 2006;130:1150–6.
Yokomise H, Satoh K, Ohno N, Tamura K. Autoblood plus OK432 pleurodesis with open drainage for persistent air leak after lobectomy. Ann Thorac Surg. 1998;65:563–5.
Rivas de Andres JJ, Blanco S, de la Torre M. Postsurgical pleurodesis with autologous blood in patients with persistent air leak. Ann Thorac Surg. 2000;70:270–2.
Liberman M, Muzikansky A, Wright CD, Wain JC, Donahue DM, Allan JS, et al. Incidence and risk factors of persistent air leak after major pulmonary resection and use of chemical pleurodesis. Ann Thorac Surg. 2010;89:891–7.
Venuta F, Rendina EA, De Giacomo T, Coloni GF. Postoperative strategies to treat permanent air leaks. Thorac Surg Clin. 2010;20:391–7.
Lange P, Mortensen J, Groth S. Lung function 22-35 years after treatment of idiopathic spontaneous pneumothorax with talc poudrage or simple drainage. Thorax. 1988;43:559–61.
Fernandez FG, Falcoz PE, Kozower BD, Salati M, Wright CD, Brunelli A. The Society of Thoracic Surgeons and the European Society of Thoracic Surgeons general thoracic surgery databases: joint standardization of variable definitions and terminology. Ann Thorac Surg. 2015;99:368–76.
Nakahara K, Ohno K, Hashimoto J, Miyoshi S, Maeda H, Matsumura A, et al. Prediction of postoperative respiratory failure in patients undergoing lung resection for lung cancer. Ann Thorac Surg. 1988;46:549–52.
Kashiwabara K, Sasaki J, Mori T, Nomori H, Fujii K, Kohrogi H. Relationship between functional preservation after segmentectomy and volume-reduction effects after lobectomy in stage I non-small cell lung cancer patients with emphysema. J Thorac Oncol. 2009;4:1111–6.
Kuzniar TJ, Blum MG, Kasibowska-Kuzniar K, Mutlu GM. Predictors of acute lung injury and severe hypoxemia in patients undergoing operative talc pleurodesis. Ann Thorac Surg. 2006;82:1976–81.
Cerfolio RJ, Bass CS, Pask AH, Katholi CR. Predictors and treatment of persistent air leaks. Ann Thorac Surg. 2002;73:1727–30 discussion 1730-1721.
Brunelli A, Monteverde M, Borri A, Salati M, Marasco RD, Fianchini A. Predictors of prolonged air leak after pulmonary lobectomy. Ann Thorac Surg. 2004;77:1205–10 discussion 1210.
Brunelli A, Varela G, Refai M, Jimenez MF, Pompili C, Sabbatini A, et al. A scoring system to predict the risk of prolonged air leak after lobectomy. Ann Thorac Surg. 2010;90:204–9.
Gilbert S, Maghera S, Seely AJ, Maziak DE, Shamji FM, Sundaresan SR, et al. Identifying patients at higher risk of prolonged air leak after lung resection. Ann Thorac Surg. 2016;102:1674–9.
Tao H, Tanaka T, Hayashi T, et al. Influence of stapling the intersegmental planes on lung volume and function after segmentectomy. Interact Cardiovasc Thorac Surg. 2016;23(4):548–52.
Chen X, Jin R, Xiang J, Han D, Zhang Y, Li C, et al. Methods for dissecting intersegmental planes in segmentectomy: a randomized controlled trial. Ann Thorac Surg. 2020;110(1):258–64.
Sienel W, Stremmel C, Kirschbaum A, Hinterberger L, Stoelben E, Hasse J, et al. Frequency of local recurrence following segmentectomy of stage IA non-small cell lung cancer is influenced by segment localisation and width of resection margins–implications for patient selection for segmentectomy. Eur J Cardiothorac Surg. 2007;31:522–7 discussion 527–528.
Whitson BA, Groth SS, Andrade RS, Maddaus MA, Habermann EB, D’Cunha J. Survival after lobectomy versus segmentectomy for stage I non-small cell lung cancer: a population-based analysis. Ann Thorac Surg. 2011;92:1943–50.
Cao C, Chandrakumar D, Gupta S, Yan TD, Tian DH. Could less be more?-A systematic review and meta-analysis of sublobar resections versus lobectomy for non-small cell lung cancer according to patient selection. Lung Cancer. 2015;89:121–32.
Nishio W, Yoshimura M, Maniwa Y, Kitamura Y, Tane K, Takenaka D, et al. Re-Assessment of intentional extended segmentectomy for clinical T1aN0 non-small cell lung cancer. Ann Thorac Surg. 2016;102:1702–10.
Acknowledgments
This study was supported in part by a Grant–in–Aid for Cancer Research from the Ministry of Health, Labor and Welfare of Japan and the Smoking Research Foundation.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Maeyashiki, T., Takamochi, K., Matsunaga, T. et al. Negative impact of chemical pleurodesis on postoperative pulmonary function for managing prolonged air leakage after segmentectomy. Gen Thorac Cardiovasc Surg 69, 707–715 (2021). https://doi.org/10.1007/s11748-020-01534-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11748-020-01534-9