Abstract
Objective
To observe the clinical efficacy of herbal cake-partitioned moxibustion for ulcerative colitis (UC) and elucidate its mechanism by targeting the vitamin D receptor (VDR) signaling pathway.
Methods
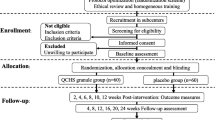
A total of 63 patients with UC were randomly divided into an observation group (30 cases, treated with herbal cake-partitioned moxibustion) and a control group (33 cases, treated with sham herbal cake-partitioned moxibustion). Moxibustion treatment was performed at Qihai (CV6) and bilateral Tianshu (ST25) and Shangjuxu (ST37), 3 times per week for 12 weeks. The total effective rate, visual analog scale (VAS) score for abdominal bloating and pain, and hospital anxiety and depression scale (HADS) score were compared between the two groups. Enzyme-linked immunosorbent assay was used to detect the concentrations of serum C-reactive protein (CRP), 25-hydroxyvitamin D [25(OH)D], and interleukin-12 (IL-12)/interleukin-23 (IL-23) p40. Immunohistochemistry was used to observe the expression levels of VDR and regenerating gene IV (Reg IV) proteins in colonic mucosa. The expression levels of VDR, cytochrome p450 27B1 (CYP27B1), and Reg IV mRNAs were detected by real-time fluorescence quantitive polymerase chain reaction.
Results
After treatment, the total effective rate in the observation group was 86.7%, which was significantly higher than 51.5% in the control group (P<0.05). After treatment, the VAS scores for abdominal bloating and pain in the observation group were significantly decreased (P<0.01), as well as the HADS-depression subscale (HADS-D) and HADS-anxiety subscale (HADS) scores (P<0.05), while only the VAS score for abdominal pain in the control group was reduced (P<0.05), and the improvements of the scores in the observation group were more significant than those in the control group (P<0.05). After treatment, the serum CRP concentrations in both groups and the IL-12/IL-23 p40 concentration in the observation group were significantly decreased (P<0.05), and the concentrations in the observation group were lower than those in the control group (P<0.05). The expression levels of VDR protein and mRNA in the colon in both groups were all increased (P<0.01), and the expression levels of Reg IV protein and mRNA and CYP27B1 mRNA were all decreased in the two groups (P<0.05 or P<0.01); the improvements in the observation group were more notable than those in the control group (P<0.05 or P<0.01).
Conclusion
Herbal cake-partitioned moxibustion can effectively alleviate abdominal pain and diarrhea in patients with UC, improve depression and anxiety disorders, and regulate the expression of related proteins in the VDR signaling pathway. The mechanism may be related to inhibiting intestinal inflammation by reducing the release of the proinflammatory cytokine IL-12/IL-23 p40.
摘要
目的
观察隔药饼灸治疗溃疡性结肠炎(UC)的临床疗效, 并从维生素D受体(VDR)信号通路角度阐释其效应机 制。
方法
将63例UC患者随机分为观察组30例(采用隔药饼灸治疗)和对照组33例(采用假隔药饼灸治疗)。两组均取气 海和双侧天枢、上巨虚治疗, 每周3次, 共治疗12周。比较两组的总有效率、患者腹胀和腹痛视觉模拟量表(VAS)和医 院焦虑抑郁量表(HADS)评分; 酶联免疫吸附测定法检测血清C反应蛋白(CRP)、25羟维生素D[25(OH)D]、白细胞介素-12 (IL-12)/白细胞介素-23(IL-23)p40的浓度; 免疫组化法检测结肠VDR和再生基因蛋白IV(Reg IV)蛋白的表达; 实时荧光 定量聚合酶链反应检测结肠黏膜VDR、细胞色素P450家族成员27B1(CYP27B1)和Reg IV mRNA的表达。
结果
治疗后, 观察组总有效率为86.7%, 明显高于对照组的51.5%(P<0.05)。治疗后, 观察组腹痛和腹胀VAS评分降低(P<0.01), HADS 的抑郁亚量表(HADS-D)和焦虑亚量表(HADS-A)评分均降低(P<0.05), 对照组仅腹痛VAS评分明显降低(P<0.05); 观察组 评分改善情况均优于对照组(P<0.05)。治疗后, 两组患者血清CRP浓度、观察组血清IL-12/IL-23 p40浓度均降低(P<0.05), 观察组的浓度均低于对照组(P<0.05); 两组患者结肠VDR蛋白和mRNA的表达明显升高(P<0.01), 而Reg IV蛋白和 mRNA以及CYP27B1 mRNA的表达均明显降低(P<0.05或P<0.01), 观察组较对照组改善更为显著(P<0.05或P<0.01)。
结论
隔药饼灸能有效缓解UC患者腹痛、腹泻症状, 改善抑郁、焦虑情绪, 并能调节VDR信号通路相关蛋白的表达。其作用 机制可能是通过减少促炎细胞因子IL-12/IL-23 p40的释放来抑制肠道炎症。
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
ORDÁS I, ECKMANN L, TALAMINI M, BAUMGART D C, SANDBORN W J. Ulcerative colitis. Lancet, 2012, 380(9853): 1606–1619.
KAPLAN G G, NG S C. Understanding and preventing the global increase of inflammatory bowel disease. Gastroenterology, 2017, 152(2): 313–321.
GAJENDRAN M, LOGANATHAN P, JIMENEZ G, CATINELLA A P, NG N, UMAPATHY C, ZIADE N, HASHASH J G. A comprehensive review and update on ulcerative colitis. Dis Mon, 2019, 65(12): 100851.
KOBAYASHI T, SIEGMUND B, LE BERRE C, WEI S C, FERRANTE M, SHEN B, BERNSTEIN C N, DANESE S, PEYRIN-BIROULET L, HIBI T. Ulcerative colitis. Nat Rev Dis Primers, 2020, 6(1): 74.
ZHAO J, WANG Y, GU Q, DU Z, CHEN W. The association between serum vitamin D and inflammatory bowel disease. Medicine (Baltimore), 2019, 98(18): e15233.
L BISHOP E, ISMAILOVA A, DIMELOE S, HEWISON M, WHITE J H. Vitamin D and immune regulation: antibacterial, antiviral, anti-inflammatory. JBMR Plus, 2020, 5(1): e10405.
TSUCHIDA C, SAKURAMOTO-TSUCHIDA S, TAKED M, ITAYA-HIRONAKA A, YAMAUCHI A, MISU M, SHOBATAKE R, UCHIYAMA T, MAKINO M, PUJOL-AUTONELL I, VIVES-PI M, OHBAYASHI C, TAKASAWA S. Expression of REG family genes in human inflammatory bowel diseases and its regulation. Biochem Biophys Rep, 2017, 12: 198–205.
STEIN D J. Massage acupuncture, moxibustion, and other forms of complementary and alternative medicine in inflammatory bowel disease. Gastroenterol Clin North Am, 2017, 46(4): 875–880.
QI Q, LIU Y N, JIN X M, ZHANG L S, WANG C, BAO C H, LIU H R, WU H G, WANG X M. Moxibustion treatment modulates the gut microbiota and immune function in a dextran sulphate sodium-induced colitis rat model. World J Gastroenterol, 2018, 24(28): 3130–3144.
WANG Z Q, HUANG Y, WANG D, WANG R M, LI K S, QI Q, MA Z, GU M E, ZHENG H D, LU Y, WU L Y. Genome-wide regulation of acupuncture and moxibustion on ulcerative colitis rats. Evid Based Complement Alternat Med, 2021, 2021: 9945121.
LIN Y Y, ZHAO JM, JI Y J, MA Z, ZHENG H D, HUANG Y, CUI Y H, LU Y, WU H G. Typical ulcerative colitis treated by herbs-partitioned moxibustion: a case report. World J Clin Cases, 2020, 8(8): 1515–1524.
ZHOU E H, LIU H R, WU H G, SHI Z, ZHANG W, ZHU Y, SHI D R, ZHOU S. Down-regulation of protein and mRNA expression of IL-8 and ICAM-1 in colon tissue of ulcerative colitis patients by partition-herb moxibustion. Dig Dis Sci, 2009, 54(10): 2198–2206.
LIU H R, SHI D R, WU H G, ZHONG Y S, LI S. Effect of herbal cake-partitioned moxibustion on the expression of COX-2 TNF-a in the colonic mucosa of patients with ulcerative colitis. Zhongyiyao Xuekan, 2005, 23(6): 989–992.
WU H G, SHI Z, ZHU Y, MA X P, YAO Y, CUI Y H, ZHAO T P, LIU H R. Clinical study of herbal cake-partitioned moxibustion in the treatment of ulcerative colitis. Shanghai Zhenjiu Zazhi, 2007, 26(4): 3–4.
YANG L, ZHAO J M, GUAN X, WANG X M, ZHAO C, LIU H R, WU L Y, JI J, CHENG F, LIU X R, WU H G. Observation on the effects of different partitioned moxibustion in treating ulcerative colitis. J Acupunct Tuina Sci, 2016, 14(4): 231–241.
Inflammatory Bowel Disease Group, Chinese Society of Gastroenterology. Consensus on the diagnosis and treatment of inflammatory bowel disease (Guangzhou, 2012). Zhonghua Neike Zazhi, 2012, 51(10): 818–831.
SNAITH R P, ZIGMOND A S. The hospital anxiety and depression scale. Br Med J (Clin Res Ed), 1986, 292(6516): 344.
ANASTASI J K, CAPILI B, CHANG M. Development of acupuncture and moxibustion protocol in a clinical trial for irritable bowel syndrome. J Acupunct Meridian Stud, 2017, 10(1): 62–66.
BAO C H, ZHANG J Z, LIU J M, LIU H R, WU L Y, SHI Y, LI J, HU Z H, DONG Y Z, WANG S Y, ZENG X Q, WU H G. Moxibustion treatment for diarrhea-predominant irritable bowel syndrome: study protocol for a randomized controlled trial. BMC Complement Altern Med, 2016, 16(1): 408.
LI Z P, ZHENG Z, WANG L J, XIAO W Y, ZENG J Q, HAO J, CHEN R X, XIE D Y. Efficacy evaluation of heat-sensitive moxibustion for chemotherapy symptoms of large intestine cancer. Zhongguo Zhen Jiu, 2015, 35(10): 1010–1013.
BAO C H, WU L Y, WANG D, CHEN L M, JIN X M, SHI Y, LI G N, ZHANG J Z, ZENG X Q, CHEN J H, LIU H R, WU H G. Acupuncture improves the symptoms, intestinal microbiota, and inflammation of patients with mild to moderate Crohn’s disease: a randomized controlled trial. EClinicalMedicine, 2022, 45: 101300.
QI Q, LIU Y N, LÜ S Y, WU H G, ZHANG L S, CAO Z, LIU H R, WANG X M, WU L Y. Gut microbiome alterations in colitis rats after moxibustion at bilateral Tianshu acupoints. BMC Gastroenterol, 2022, 22(1): 62.
QI Q, WU H G, JIN X M, JIN D Y, WANG Y Y, WANG C, LIU Y N, WANG X M. Effect of moxibustion on the expression of GDNF and its receptor GFRα3 in the colon and spinal cord of rats with irritable bowel syndrome. Acupunct Med, 2019, 37(4): 244–251.
BAO C H, WU L Y, WU H G, LIU H R, ZHAO J M, ZENG X Q, MA L L, LI J, ZHAO C, WANG S Y. Active Crohn’s disease treated with acupuncture and moxibustion: a randomized controlled trial. Zhongguo Zhen Jiu, 2016, 36(7): 683–688.
SCHOULTZ M. The role of psychological factors in inflammatory bowel disease. Br J Community Nurs, 2012, 17(8): 370–374.
DE RIDDER D, GEENEN R, KUIJER R, VAN MIDDENDORF− H. Psychological adjustment to chronic disease. Lancet, 2008, 372(9634): 246–255.
CHENG W F, SHI R H. Investigation on psychological characteristics in ulcerative colitis. Weichangbingxue He Ganbingxue Zazhi, 2013, 16(5): 437–439.
GRAFF L A, WALKER J R, CLARA I, LIX L, MILLER N, ROGALA L, RAWSTHORNE F, BERNSTEIN C N. Stress coping, distress, and health perceptions in inflammatory bowel disease and community controls. Am J Gastroenterol, 2009, 104(12): 2959–2969.
HÄUSER W, JANKE K H, KLUMP B, HINZ A. Anxiety and depression in patients with inflammatory bowel disease: comparisons with chronic liver disease patients and the general population. Inflamm Bowel Dis, 2011, 17(2): 621–632.
BLANCK S, ABERRA F. Vitamin D deficiency is associated with ulcerative colitis disease activity. Dig Dis Sci, 2013, 58(6): 1698–1702.
FLETCHER J, COOPER S C, GHOSH S, HEWISON M. The role of vitamin D in inflammatory bowel disease: mechanism to management. Nutrients, 2019, 11(5): 1019.
OOI J H, LI Y, ROGERS C J, CANTORNA M T. Vitamin D regulates the gut microbiome and protects mice from dextran sodium sulfate-induced colitis. J Nutr, 2013, 143(10): 1679–1686.
MILLER H L, FARRAYE F A, COUKOS J, HOWARD L A, HOLICK M F, STUCCHI A F, BECKER J M. Vitamin D deficiency and insufficiency are common in ulcerative colitis patients after ileal pouch-anal anastomosis. Inflamm Bowel Dis, 2013, 19(2): E25–E26.
ULITSKY A, ANANTHAKRISHNAN A N, NAIK A, SKAROS S, ZADVORNOVA Y, BINION D G, ISSA M. Vitamin D deficiency in patients with inflammatory bowel disease: association with disease activity and quality of life. JFEN J Farenter Enteral Nutr, 2011, 35(3): 308–316.
FAGNINI C, DI PAOLO M C, GRAZIANI M G, DELLEFAVE G. Probiotics and vitamin D/vitamin D receptor pathway interaction: potential therapeutic implications in inflammatory bowel disease. Front Pharmacol, 2021, 12: 747856.
LI C X, CHEN Y, ZHU H T, ZHANG X M, HAN L, ZHAO Z D, WANG J H, NING L G, ZHOU W H, LU C, XU L, SANG J Z, FENG Z M, ZHANG Y W, LOU X H, BO X C, ZHU B, YU C H, ZHENG M, LI Y M, SUN J, SHEN Z. Inhibition of histone deacetylation by MS-275 alleviates colitis by activating the vitamin D receptor. J Crohns Colitis, 2020, 14(8): 1103–1118.
MOSCHEN A R, TILG H, RAINE T. IL-12, IL-23 and IL-17 in IBD: immunobiology and therapeutic targeting. Nat Rev Gastroenterol Hepatol, 2019, 16(3): 185–196.
SANDBORN W J, FEAGAN B G, FEDORAK R N, SCHERL E, FLEISHER M R, KATZ S, JOHANNS J, BLANK M, RUTGEERTS P; Ustekinumab Crohn’s Disease Study Group. A randomized trial of ustekinumab, a human interleukin-12/23 monoclonal antibody, in patients with moderate-to-severe Crohn’s disease. Gastroenterology, 2008, 135(4): 1130–1141.
DANIEL C, SARTORY N A, ZAHN N, RADEKE H H, STEIN J M. Immune modulatory treatment of trinitrobenzene sulfonic acid colitis with calcitriol is associated with a change of a T helper (Th)1/Th17 to a Th2 and regulatory T cell profile. J Pharmacol Exp Ther, 2008, 324(1): 23–33.
BATTISTINI C, BALLAN R, HERKENHOFF M E, SAAD S M I, SUN J. Vitamin D modulates intestinal microbiota in inflammatory bowel diseases. Int J Mol Sci, 2020, 22(1): 362.
WANG H Q, HE X, LIANG S M, CHEN X. Role of vitamin D in ulcerative colitis: an update on basic research and therapeutic applications. Expert Rev Gastroenterol Hepatol, 2022, 16(3): 251–264.
O’SULLIVAN M. Vitamin D as a novel therapy in inflammatory bowel disease: new hope or false dawn?. Proc Nutr Soc, 2015, 74(1): 5–12.
WU S, ZHANG Y G, LU R, XIA Y, ZHOU D, PETROF E O, CLAUD E C, CHEN D, CHANG E B, CARMELIET G, SUN J. Intestinal epithelial vitamin D receptor deletion leads to defective autophagy in colitis. Gut, 2015, 64(7): 1082–1094.
NANAKIN A, FUKUI H, FUJII S, SEKIKAWA A, KANDA N, HISATSUNE H, SENO H, KONDA Y, FUJIMORI T, CHIBA T. Expression of the REG IV gene in ulcerative colitis. Lab Invest, 2007, 87(3): 304–314.
LAI M G, ZHANG Y L. Increased expression of Reg V in ulcerative colitis provides a potential predictor of the disease activity. Xiandai Xiaohua Ji Jieru Zhenliao, 2010, 15(2): 71–73.
Acknowledgments
This work was supported by the Projects of National Natural Science Foundation of China (国家自然科学基金 项目, No. 81973955, No. 82174501, No. 81973953); Scientific Research Project of Shanghai Municipal Health Commission (上海市卫生健康委员会科研项目, No. 20194Y0005); Shanghai Sailing Program of Science and Technology Commission of Shanghai (上海市科学技术委 员会青年科技英才扬帆计划项目, No. 20YF1445200); In-budget Project of Shanghai Education Commission (上 海市教委预算内科研项目, No. 2021LK094).
Author information
Authors and Affiliations
Corresponding authors
Additional information
Conflict of Interest
Author WU Huangan is editor-in-chief of the Journal of Acupuncture and Tuina Science. The paper was handled by other editors and has undergone a rigorous peer review process. Author WU Huangan was not involved in the journal’s review or decisions related to this manuscript.
Statement of Informed Consent
Informed consent was obtained from all individual participants.
Co-first Authors: IM Hyoyoung, M.D., resident physician; WANG Wenjia, M.M., attending physician
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits use, duplication, adaptation, distribution, and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provided a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Im, H., Wang, W., Qi, Q. et al. Clinical efficacy of moxibustion for ulcerative colitis and its influence on vitamin D receptor. J. Acupunct. Tuina. Sci. 21, 40–50 (2023). https://doi.org/10.1007/s11726-023-1357-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11726-023-1357-5
Keywords
- Moxibustion Therapy
- Medicinal Cake-partitioned Moxibustion
- Colitis, Ulcerative
- Mucous Membrane
- Vitamin D Receptor
- Clinical Trial