Abstract
Background
The Roux-en-Y gastric bypass (RYGB) is a common bariatric surgery to treat obesity. Its metabolic consequences are favourable and long-term clinical corollaries beneficial. However, detailed assessments of various affected metabolic pathways and their mediating physiological factors are scarce.
Methods
We performed a clinical study with 30 RYGB patients in preoperative and 6-month postoperative visits. NMR metabolomics was applied to profiling of systemic metabolism via 80 molecular traits, representing core cardiometabolic pathways. Glucose, glycated haemoglobin (HbA1c), insulin, and apolipoprotein B-48 were measured with standard assays. Logistic regression models of the surgery effect were used for each metabolic measure and assessed individually for multiple mediating physiological factors.
Results
Changes in insulin concentrations reflected those of BMI with robust decreases due to the surgery. Six months after the surgery, triglycerides, remnant cholesterol, and apolipoprotein B-100 were decreased −24%, −18%, and −14%, respectively. Lactate and glycoprotein acetyls, a systemic inflammation biomarker, decreased −16% and −9%, respectively. The concentrations of branched-chain (BCAA; leucine, isoleucine, and valine) and aromatic (phenylalanine and tyrosine) amino acids decreased after the surgery between −17% for tyrosine and −23% for leucine. Except for the most prominent metabolic changes observed for the BCAAs, all changes were almost completely mediated by weight change and insulin. Glucose and type 2 diabetes had clearly weaker effects on the metabolic changes.
Conclusions
The comprehensive metabolic analyses indicate that weight loss and improved insulin sensitivity during the 6 months after the RYGB surgery are the key physiological outcomes mediating the short-term advantageous metabolic effects of RYGB.
The clinical study was registered at ClinicalTrials.gov as NCT01330251.
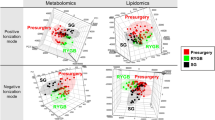
Graphical Abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Bariatric surgeries are a globally increasing trend to treat patients with obesity [1]. The key clinical reasons include evident long-term advantages on weight and appetite control, blood pressure, inflammation, mortality, liver health, as well as remission and prevention of type 2 diabetes [2,3,4,5,6]. Recent studies have demonstrated beneficial consequences of bariatric surgeries on multiple metabolic pathways [6,7,8,9,10,11,12,13,14,15,16,17]. However, limited attention has been paid on the potential mediating physiological factors explaining the abundant postoperative changes in circulating biomarkers [9,10,11, 16]. It is these physiological factors that are the primary result from the bariatric surgeries, not the metabolic changes per se. Thus, increased understanding of the metabolic effects of altered physiology is likely more important than just looking at how various metabolic biomarkers change [16]. Nonetheless, the comprehensive biomarker approach is a prerequisite to recognise the relative effects of resulting physiological changes on various metabolic pathways with potentially different clinical corollaries [6, 8,9,10,11,12, 14,15,16]. Understanding of the affected key physiology together with the detailed heterogeneous effects on multiple metabolic pathways will also facilitate itemised comparisons to non-surgical interventions of obesity [7, 16].
Here, we report a clinical study with 30 RYGB patients (16 with type 2 diabetes and 14 without) who completed the preoperative and 6-month postoperative study visits, including a comprehensive metabolic profiling of systemic metabolism. The 84 quantitative molecular traits, representing multiple core pathways in cardiometabolic health, facilitated wide-ranging analyses on the effects of weight loss and improved insulin sensitivity on the RYGB-induced systemic metabolic changes.
Research Design and Methods
Clinical Study Protocol and Patients
The study protocol has been described previously by Härma et al. [18], and more details are provided in the Supplementary Material. The study was registered at ClinicalTrials.gov as NCT01330251. Results are reported here for the 30 RYGB patients who completed both the pre- and postoperative study visits (16 with type 2 diabetes and 14 without). An outline of the study protocol with the metabolomic data characteristics is shown in Supplementary Fig. 1.
Clinical Data
The use of medications was recorded at the study visits, and standard clinical measurements were performed. Insulin, glucose, and haemoglobin A1c (HbA1c) were determined by standard clinical assays. Apolipoprotein B-48 (apoB-48) was measured with an enzyme-linked immunosorbent assay. More details for the clinical measurements are given in the Supplementary Material. Clinical characteristics for the pre- and postoperative patients are given in Table 1.
Metabolomic Data
A high-throughput nuclear magnetic resonance (NMR) metabolomic platform was applied [19, 20]. The 80 molecular outputs analysed feature 14 lipoprotein subclasses [21], apolipoprotein A-I (apoA-I) and B (apoB), multiple clinical cholesterol and triglyceride measures, albumin, various fatty acids, and numerous low-molecular-weight metabolites, including amino acids, glycolysis related measures, ketone bodies and a new inflammation marker glycoprotein acetyls (GlycA)—most of them in central pathways related to cardiometabolic health (Supplementary Fig. 1). The lipoprotein subclass data are described in detail in the Supplementary Material. The platform has been used in numerous epidemiological and genetic studies over the past 10 years, and it has also been adopted by the UK Biobank [19,20,21,22].
Statistical Analyses
To manage multiple testing over the large set of metabolic measures, we first conducted principal component analysis to determine the effective number of independent variables. Sixteen principal components were enough to explain >95% of variation in the metabolic data. Therefore, we set the 5% Bonferroni-adjusted type 1 error threshold at p < 0.05/16 = 0.0031.
Logistic regression models of the surgery effect were constructed for each metabolic measure to manage potentially confounding factors such as sex and age as well as to analyse if the metabolic changes would be mediated by physiological co-variation because of the surgery. The dependent variable was set to 0 for the preoperative and 1 for the postoperative samples. Various models, namely sex + age, sex + age + BMI, sex + age + insulin, sex + age + glucose, and sex + age + history of type 2 diabetes, were tested to assess how the physiological co-variation between the pre- and postoperative time points would affect the metabolic changes. Before modelling, the inputs were scaled to unit standard deviation.
All analyses were undertaken on the R statistical platform (version 3.6.2).
Results
Only two metabolites showed a different response to the RYGB operation between the patients with and without type 2 diabetes: glucose (p = 0.8*10−3) and alanine (p = 0.001) decreased more for those patients that had type 2 diabetes in the pre-RYGB time point. Thus, all the metabolic data were analysed and presented as combining these groups pre- and post-operation.
BMI, Insulin, Glucose and HbA1c
The pre- and postoperative BMI ranges were 36.3 kg/m2 ≤ BMI ≤ 55.2 kg/m2 and 25.4 kg/m2 ≤ BMI ≤ 46.6 kg/m2, respectively. The expected, clear reduction in BMI 6 months after the RYBG surgery for both patient groups is shown in Fig. 1A; for the type 2 diabetes group (n = 16) from (median (interquartile range)) 41.55 (38.08–44.12) kg/m2 to 32.05 (30.40–33.73) kg/m2 and for the nondiabetic group (n = 14) from 48.05 (43.90–51.60) kg/m2 to 38.90 (33.58–41.35) kg/m2. Changes in insulin concentrations reflect those of BMI with robust decreases from 16.5 (13.3–27.5) mU/L to 8.0 (7.0–10.8) mU/L for the type 2 diabetes group and from 16.5 (9.0–26.5) mU/L to 10.0 (7.8–14.0) mU/L for the nondiabetic group. For both glucose and HbA1c, similar trends are seen in the median values, however with marked overlap between the pre- and postoperative distributions.
A Preoperative and 6-month postoperative distributions of BMI, insulin, glucose, and HbA1c. The box plots represent medians with interquartile ranges and with 10th percentile minimum and 90th percentile maximum whiskers. Open circles refer to outliers. Metabolite concentrations were compared using the paired t test. *Robust association for all the RYGB patients (n = 30) (i.e. including those who had and did not have type 2 diabetes) at the Bonferroni-corrected threshold p < 0.0031. B Regression modelling on changes in BMI, insulin, glucose, and HbA1c from the preoperative visit to the 6-month postoperative visit. Analyses with individual adjustments for sex + age, sex + age + BMI, sex + age + insulin, sex + age + glucose, and sex + age + type 2 diabetes are shown
Apolipoprotein B, Triglyceride, Cholesterol and Lipoprotein Subclass Particle Concentrations
Serum triglycerides, VLDL cholesterol, and remnant cholesterol (i.e. non-HDL, non-LDL cholesterol [23]) show robust decreases of around −24%, −26%, and −18%, respectively, after the surgery (Fig. 2). The lipoprotein subclass data indicates that all the VLDL subclass particle concentrations follow a similar robust trend of decrease. Circulating apoB concentrations show a robust decrease of around −14% after the RYGB surgery, reflecting the trends of all the individual apoB-containing lipoprotein subclass particles (Fig. 2 and Supplementary Fig. 2).
Preoperative and 6-month postoperative distributions for various lipoprotein measures. The box plots represent medians with interquartile ranges and with 10th percentile minimum and 90th percentile maximum whiskers. Open circles refer to outliers. Metabolite concentrations were compared using the paired t test. *Robust association for all the RYGB patients (n = 30) (i.e. including those who had and did not have type 2 diabetes) at the Bonferroni-corrected threshold p < 0.0031
Fatty Acids and Amino Acids
The concentrations of total (−17%) as well as saturated (SFA, −16%) and monounsaturated (MUFA, −19%) fatty acids were robustly decreased after the operation for both patient groups as illustrated in Fig. 3. In relative terms of total fatty acids, the proportion of SFA robustly decreases similar to the decrease in the absolute concentration. The proportion of PUFAs shows a robust increase in contradiction to the decreasing trend in absolute concentrations (Supplementary Fig. 2).
Preoperative and 6-month postoperative distributions for various fatty acid concentrations and relative abundances. Corresponding distributions are also shown for seven circulating amino acid concentrations, lactate, and the inflammation marker GlycA. The box plots represent medians with interquartile ranges and with 10th percentile minimum and 90th percentile maximum whiskers. Open circles refer to outliers. Metabolite concentrations were compared using a paired t test. *Robust association for all the RYGB patients (n = 30) (i.e. including those who had and did not have type 2 diabetes) at the Bonferroni-corrected threshold p < 0.0031
The concentrations of branched-chain amino acids (BCAAs; leucine, isoleucine, and valine), aromatic amino acids (phenylalanine and tyrosine), as well as histidine and alanine show robust decreases 6 months after the RYGB surgery (Fig. 3). The decrease varies between −17% for tyrosine and −23% for leucine.
Glycolysis-Related Metabolites and Inflammation
Lactate and GlycA, a recently emerged inflammation biomarker [24], show a robust decrease of −16% and −9%, respectively, after the surgery (Fig. 3).
The results for the metabolic distributions and their changes after the RYGB surgery, corresponding to Figs. 1A, 2, and 3, for all the 84 metabolic measures plus BMI are illustrated in Supplementary Fig. 2.
Regression Models
Figure 1B depicts results from regression modelling, together with the effects of various adjustments (sex + age, sex + age + BMI, sex + age + insulin, sex + age + glucose, and sex + age + history of type 2 diabetes), on how BMI, insulin, glucose, and HbA1c changed between the 6-month time point after the RYGB surgery and the preoperative time point. The BMI change is not explained by adjusting for insulin or glucose changes, but the effect of the insulin adjustment is larger. The adjustment for BMI abolishes and the adjustment for glucose have a marked effect on the change in insulin concentrations. The associations for glucose and HbA1c are weak in all the models. Adjusting for type 2 diabetes has very little effect on the associations for all the clinical variables. It should be noted that all the patients using oral antidiabetic medications before RYGB had stopped the medications prior to the 6-month visit.
The results from the abovementioned regression modelling are illustrated for the various lipid, lipoprotein, and apolipoprotein measures in Fig. 4. Overall, both BMI and insulin change have strong effects on the models, and the effects of both glucose change and type 2 diabetes are minor. Very similar results are seen for the fatty acids, amino acids, glycolysis-related metabolites, and the inflammation biomarker GlycA (Fig. 5). The associations for the changes in the BCAAs are prominent and remain robust after adjusting for glucose change. Moreover, they are not abolished after adjusting for BMI and insulin. The associations for leucine are slightly stronger than those for isoleucine and valine.
Regression modelling on metabolic changes in the concentrations of various lipoprotein measures from the preoperative visit to the 6-month postoperative visit. Analyses with individual adjustments for sex + age, sex + age + BMI, sex + age + insulin, sex + age + glucose, and sex + age + type 2 diabetes are shown
Regression modelling on metabolic changes in various fatty acid concentrations and relative abundances from the preoperative visit to the 6-month postoperative visit. Corresponding analyses are also shown for seven circulating amino acid concentrations, lactate, and the inflammation marker GlycA. Analyses with individual adjustments for sex and age, sex and age + BMI, sex and age + insulin, sex and age + glucose, and sex and age + type 2 diabetes are shown
The results for the regression modelling, corresponding to Figs. 1B, 4, and 5, for all the 84 metabolic measures and BMI are illustrated in Supplementary Fig. 3.
Discussion
This study focused on the 6-month postoperative changes in the systemic metabolism of patients who went through the Roux-en-Y gastric bypass surgery to treat morbid obesity. The clinical characteristics and outcomes were as expected with a substantial decrease in BMI and markedly improved insulin sensitivity (Fig. 1). The systemic metabolomic approach, utilising 84 quantitative molecular traits, enabled detection of accompanying characteristic changes in multiple core metabolic pathways related to cardiometabolic health. The current results replicate many known metabolic consequences of RYGB alongside providing more nuance, for example, for the lipoprotein subclass sequels, inflammation, amino acids, glycolysis-related measures, and ketone bodies (Figs. 2 and 3). We also showed that the ample postoperative metabolic changes along diverse metabolic pathways are, to a great degree, mediated by the weight loss and by the concomitant increase in insulin sensitivity, but not by changes in circulating glucose concentrations (Figs. 4 and 5).
The characteristic effects of the RYGB surgery on lipoprotein and lipid metabolism are well-known at the level of standard clinical lipid measures [5]. The primary effect was, as expected, a clear decrease in the circulating triglyceride concentrations. The extensive lipoprotein data acquired here illustrate that this effect is coherently seen in the circulating particle concentrations of all the VLDL subclasses and reflected by the decreases in remnant and VLDL cholesterol as well as in the circulating apoB concentrations. Our results are broadly similar to those in a recent study that used another NMR-based method to analyse changes in detailed lipoprotein profiles due to bariatric surgeries [17]. As a logical result of decreased concentrations of circulating triglycerides, all the circulating concentrations of fatty acids showed a decreasing trend after the RYGB surgery. Alongside these absolute decreases in concentrations, the relative amount of saturated fatty acids decreased and that of polyunsaturated fatty acids increased.
Most literature related to circulating fatty acids in RYGB focuses particularly on non-esterified fatty acids, i.e. free fatty acids (FFAs) [10, 15]. The fatty acid measures here from the NMR metabolomics platform include all fatty acids in the serum samples, and therefore, these measures mostly reflect the average fatty acid composition in all the major lipid classes in all the circulating lipoprotein particles with only minor contributions from lipid molecules not transported in the lipoprotein particles, e.g. those bound to albumin [19, 20]. However, while being summary measures, they are associated with insulin resistance [25] and more generally with cardiometabolic risk [26] although detailed comparisons to studies in which only FFAs have been analysed are not feasible.
Branched-chain amino acids have been studied extensively in relation to obesity and type 2 diabetes [25] as well as to the RYBG and other bariatric procedures [15, 27, 28]. Our new findings are compatible with previous results and illustrate that all BCAA concentrations are markedly decreased after the RYBG operation for patients with and without type 2 diabetes. Consistent decreasing trends were also noted for the aromatic amino acids (phenylalanine and tyrosine) as well as for alanine. All these amino acid findings conform to multiple previous studies as reviewed by Vaz et al. [15]. Previous studies have reported inconsistent findings for the circulating concentrations of histidine after bariatric surgery, but here, with the RYGB procedure, the histidine concentration was decreased. The inconsistencies with histidine may relate to dissimilarities in the various types of bariatric surgery [15, 27].
Concurrent with previous results for the C-reactive protein (CRP) [3], a recently introduced systemic inflammation biomarker, glycoprotein acetyls [24], also decreased after the RYGB surgery. GlycA is a heterogeneous biomarker associated with both acute and chronic inflammation, and it provides partly CRP-independent information on various disease risks and frailty [29]. The current result thus adds support for systemic anti-inflammatory effects after the RYGB surgery. However, similarly to CRP [3], changes in circulating GlycA concentrations relate strongly to changes in insulin sensitivity.
For those metabolic measures that robustly changed after the RYGB surgery, the typical change was in the order of one SD from the baseline value. This was the case for the lipoprotein subclasses and lipids, most fatty acids and the amino acids alanine and histidine. The magnitude of change was also around one SD for glucose and HbA1c, but these associations were not robust. Slightly larger changes were seen for the saturated fatty acid concentration, GlycA and the aromatic amino acids phenylalanine and tyrosine. The largest magnitudes were around 2.5 times baseline SD for BMI, insulin, and BCAAs. These degrees of changes after the RYGB surgery are in the ballpark of metabolic changes detected in longitudinal observational studies in relation to changes in BMI, i.e. typical changes in metabolic measures are between 0.1 and 0.2 SD per BMI-unit [30].
Almost all the above-mentioned metabolic changes after the RYGB surgery were statistically explained by changes in BMI and insulin. In contradiction, adjustments for changes in circulating glucose concentrations had only minor or no effects. The same was the case for adjusting for the type 2 diabetes status, suggesting that the metabolic effects of the RYGB surgery were similar for all the patients with obesity whether they did or did not have type 2 diabetes before the operation. Previous metabolomic studies of RYGB, and bariatric surgeries in general, have paid limited attention on the potential factors explaining the abundant postoperative metabolic changes [9,10,11, 16]. The coherent role of weight loss [16] and insulin in explaining changes over diverse metabolic pathways, evident from the current results, is in accordance with the known concomitant increase of insulin sensitivity along the long-term weight loss after RYGB [31]. The genetic background for insulin resistance is highly pleiotropic with effects on lipoprotein metabolism, peripheral adipose tissue characteristics, and risk of cardiometabolic diseases [32]. Recent genetic analyses on the causal effects of insulin resistance on the systemic metabolism also give explicit support on the key role of insulin in explaining the metabolic findings [33].
The current analyses also pinpointed pronounced decreases in the circulating concentrations of alanine and lactate after the RYGB surgery, the associations being also strongly affected by the change in insulin sensitivity. Nonetheless, the abovementioned genetic causality analyses for insulin resistance substantiated neither of these circulating metabolites [33]. High circulating alanine and lactate levels associate with liver fat [34] and with non-optimal functioning of hypoxia-inducible factors (HIFs) [35], the key regulators of oxygen homeostasis in response to hypoxia. HIFs are known to be repressed in diabetic conditions [36]. Thus, while insulin resistance is likely associated with all these interrelated phenomena, their relative contributions for circulating alanine and lactate concentrations might be heavily overlapped making the dissection of the underlying physiological origins problematic [37].
Wide-ranging metabolic studies on the effects of bariatric surgeries have started to accumulate only recently [7,8,9,10,11,12,13,14,15,16, 38]. The strengths of this work are the comprehensive metabolic and statistical analyses that substantiate the view that weight loss and the concomitant improvement in insulin sensitivity are the key physiological mediators for multiple beneficial metabolic consequences of the RYGB surgery. This study, as most bariatric surgery studies, is limited by the number of patients and thus has statistical limitations to detect minor changes due to the RYGB operation. Nonetheless, robust metabolic changes were observed for multiple molecular pathways, and the statistical power for the regression modelling on the mediating physiological factors was good.
Data Availability
The data for the clinical RYGB study are available from the corresponding authors upon reasonable request.
References
Madsbad S, Dirksen C, Holst JJ. Mechanisms of changes in glucose metabolism and bodyweight after bariatric surgery. Lancet Diabetes Endocrinol. 2014;2:152–64.
Sjöström L, Lindroos A-K, Peltonen M, Torgerson J, Bouchard C, Carlsson B, et al. Lifestyle, diabetes, and cardiovascular risk factors 10 years after bariatric surgery. N Engl J Med. 2004;351:2683–93.
Holdstock C, Lind L, Engstrom BE, Ohrvall M, Sundbom M, Larsson A, et al. CRP reduction following gastric bypass surgery is most pronounced in insulin-sensitive subjects. Int J Obes. 2005;29:1275–80.
Sjöström L, Narbro K, Sjöström CD, Karason K, Larsson B, Wedel H, et al. Effects of bariatric surgery on mortality in Swedish obese subjects. N Engl J Med. 2007;357:741–52.
Adams TD, Davidson LE, Litwin SE, Kim J, Kolotkin RL, Nanjee MN, et al. Weight and metabolic outcomes 12 years after gastric bypass. N Engl J Med. 2017;377:1143–55.
Lalloyer F, Mogilenko DA, Verrijken A, Haas JT, Lamazière A, Kouach M, et al. Roux-en-Y gastric bypass induces hepatic transcriptomic signatures and plasma metabolite changes indicative of improved cholesterol homeostasis. J Hepatol. 2023;79:898–909.
Lips MA, Van Klinken JB, van Harmelen V, Dharuri HK, ’t Hoen PAC, JFJ L, et al. Roux-en-Y gastric bypass surgery, but not calorie restriction, reduces plasma branched-chain amino acids in obese women independent of weight loss or the presence of type 2 diabetes. Diabetes Care. 2014;37:3150–6.
Sarosiek K, Pappan KL, Gandhi AV, Saxena S, Kang CY, McMahon H, et al. Conserved metabolic changes in nondiabetic and type 2 diabetic bariatric surgery patients: global metabolomic pilot study. J Diabetes Res. 2016;2016:3467403.
Magouliotis DE, Tasiopoulou VS, Sioka E, Chatedaki C, Zacharoulis D. Impact of bariatric surgery on metabolic and gut microbiota profile: a systematic review and meta-analysis. Obes Surg. 2017;27:1345–57.
Samczuk P, Ciborowski M, Kretowski A. Application of metabolomics to study effects of bariatric surgery. J Diabetes Res. 2018;2018:6270875.
Wijayatunga NN, Sams VG, Dawson JA, Mancini ML, Mancini GJ, Moustaid-Moussa N. Roux-en-Y gastric bypass surgery alters serum metabolites and fatty acids in patients with morbid obesity. Diabetes Metab Res Rev. 2018;34:e3045.
Abidi W, Nestoridi E, Feldman H, Stefater M, Clish C, Thompson CC, et al. Differential metabolomic signatures in patients with weight regain and sustained weight loss after gastric bypass surgery: a pilot study. Dig Dis Sci. 2020;65:1144–54.
Ahlin S, Cefalo C, Bondia-Pons I, Trošt K, Capristo E, Marini L, et al. Metabolite changes after metabolic surgery - associations to parameters reflecting glucose homeostasis and lipid levels. Front Endocrinol. 2021;12:786952.
Ha J, Kwon Y, Park S. Metabolomics in bariatric surgery: towards identification of mechanisms and biomarkers of metabolic outcomes. Obes Surg. 2021;31:4564–74.
Vaz M, Pereira SS, Monteiro MP. Metabolomic signatures after bariatric surgery - a systematic review. Rev Endocr Metab Disord. 2022;23:503–19.
Angelidi AM, Kokkinos A, Sanoudou D, Connelly MA, Alexandrou A, Mingrone G, et al. Early metabolomic, lipid and lipoprotein changes in response to medical and surgical therapeutic approaches to obesity. Metabolism. 2023;138:155346.
Pérez Zapata AI, Varela Rodríguez C, Martín-Arriscado Arroba C, Durán Ballesteros M, de Quirós B, Fernández M, Amigo Grau N, et al. Advanced lipoproteins and lipidomic profile in plasma determined by nuclear magnetic resonance before and after bariatric surgery. Obes Surg. 2023;33:3981–7.
Härma M-A, Adeshara K, Istomin N, Lehto M, Blaut M, Savolainen MJ, et al. Gastrointestinal manifestations after Roux-en-Y gastric bypass surgery in individuals with and without type 2 diabetes. Surg Obes Relat Dis Off J Am Soc Bariatr Surg. 2021;17:585–94.
Soininen P, Kangas AJ, Würtz P, Suna T, Ala-Korpela M. Quantitative serum nuclear magnetic resonance metabolomics in cardiovascular epidemiology and genetics. Circ Cardiovasc Genet. 2015;8:192–206.
Würtz P, Kangas AJ, Soininen P, Lawlor DA, Davey Smith G, Ala-Korpela M. Quantitative serum nuclear magnetic resonance metabolomics in large-scale epidemiology: a primer on -omic technologies. Am J Epidemiol. 2017;186:1084–96.
Ala-Korpela M, Zhao S, Järvelin M-R, Mäkinen V-P, Ohukainen P. Apt interpretation of comprehensive lipoprotein data in large-scale epidemiology: disclosure of fundamental structural and metabolic relationships. Int J Epidemiol. 2021;51:996–1011.
Julkunen H, Cichońska A, Tiainen M, Koskela H, Nybo K, Mäkelä V, et al. Atlas of plasma NMR biomarkers for health and disease in 118,461 individuals from the UK Biobank. Nat Commun. 2023;14:604.
Würtz P, Kangas AJ, Soininen P, Lehtimäki T, Kähönen M, Viikari JS, et al. Lipoprotein subclass profiling reveals pleiotropy in the genetic variants of lipid risk factors for coronary heart disease: a note on Mendelian randomization studies. J Am Coll Cardiol. 2013;62:1906–8.
Ritchie SC, Würtz P, Nath AP, Abraham G, Havulinna AS, Fearnley LG, et al. The biomarker GlycA is associated with chronic inflammation and predicts long-term risk of severe infection. Cell Syst. 2015;1:293–301.
Würtz P, Mäkinen V-P, Soininen P, Kangas AJ, Tukiainen T, Kettunen J, et al. Metabolic signatures of insulin resistance in 7,098 young adults. Diabetes. 2012;61:1372–80.
Würtz P, Havulinna AS, Soininen P, Tynkkynen T, Prieto-Merino D, Tillin T, et al. Metabolite profiling and cardiovascular event risk: a prospective study of 3 population-based cohorts. Circulation. 2015;131:774–85.
Bradley D, Magkos F, Klein S. Effects of bariatric surgery on glucose homeostasis and type 2 diabetes. Gastroenterology. 2012;143:897–912.
Magkos F, Bradley D, Schweitzer GG, Finck BN, Eagon JC, Ilkayeva O, et al. Effect of Roux-en-Y gastric bypass and laparoscopic adjustable gastric banding on branched-chain amino acid metabolism. Diabetes. 2013;62:2757–61.
Kettunen J, Ritchie SC, Anufrieva O, Lyytikäinen L-P, Hernesniemi J, Karhunen PJ, et al. Biomarker glycoprotein acetyls is associated with the risk of a wide spectrum of incident diseases and stratifies mortality risk in angiography patients. Circ Genomic Precis Med. 2018;11:e002234.
Würtz P, Wang Q, Kangas AJ, Richmond RC, Skarp J, Tiainen M, et al. Metabolic signatures of adiposity in young adults: Mendelian randomization analysis and effects of weight change. PLoS Med. 2014;11:e1001765.
Camastra S, Gastaldelli A, Mari A, Bonuccelli S, Scartabelli G, Frascerra S, et al. Early and longer term effects of gastric bypass surgery on tissue-specific insulin sensitivity and beta cell function in morbidly obese patients with and without type 2 diabetes. Diabetologia. 2011;54:2093–102.
Lotta LA, Gulati P, Day FR, Payne F, Ongen H, van de Bunt M, et al. Integrative genomic analysis implicates limited peripheral adipose storage capacity in the pathogenesis of human insulin resistance. Nat Genet. 2017;49:17–26.
Wang Q, Holmes MV, Davey Smith G, Ala-Korpela M. Genetic support for a causal role of insulin resistance on circulating branched-chain amino acids and inflammation. Diabetes Care. 2017;40:1779–86.
Kaikkonen JE, Würtz P, Suomela E, Lehtovirta M, Kangas AJ, Jula A, et al. Metabolic profiling of fatty liver in young and middle-aged adults: cross-sectional and prospective analyses of the Young Finns Study. Hepatol Baltim Md. 2017;65:491–500.
Auvinen J, Tapio J, Karhunen V, Kettunen J, Serpi R, Dimova EY, et al. Systematic evaluation of the association between hemoglobin levels and metabolic profile implicates beneficial effects of hypoxia. Sci Adv. 2021;7:eabi4822.
Catrina S-B, Zheng X. Hypoxia and hypoxia-inducible factors in diabetes and its complications. Diabetologia. 2021;64:709–16.
Hoozemans J, de Brauw M, Nieuwdorp M, Gerdes V. Gut microbiome and metabolites in patients with NAFLD and after bariatric surgery: a comprehensive review. Metabolites. 2021;11:353.
Ben-Zvi D, Meoli L, Abidi WM, Nestoridi E, Panciotti C, Castillo E, et al. Time-dependent molecular responses differ between gastric bypass and dieting but are conserved across species. Cell Metab. 2018;28:310–323.e6.
Funding
Open Access funding provided by University of Oulu (including Oulu University Hospital). M.A.-K. was supported by a research grant from the Sigrid Jusélius Foundation, the Finnish Foundation for Cardiovascular Research, and the Research Council of Finland (grant no. 357183). J.H. was supported by the Finnish Foundation for Cardiovascular Research, the Northern Finland Health Care Support Foundation, Finnish Government Grants for Health Research, and the Finnish Medical Foundation.
Author information
Authors and Affiliations
Contributions
SZ: conceptualization, methodology, formal analysis, data curation, writing—review and editing, visualisation; SH: investigation, resources, writing—review and editing, funding acquisition; MJS: resources, writing—review and editing; VK: conceptualization, investigation, resources, writing—review and editing; V-PM: conceptualization, methodology, writing—review and editing, supervision; MA-K: conceptualization, methodology, resources, writing—original draft, writing—review and editing, visualisation, supervision, project administration, funding acquisition; JH: conceptualization, investigation, resources, writing—review and editing, supervision, project administration, funding acquisition
Corresponding authors
Ethics declarations
Ethics Approval and Consent to Participate
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and national research committee and followed the ethical standards of the Helsinki Declaration, as revised in 2000. The study protocol was approved by the Ethics Committee of the Northern Ostrobothnia Hospital District. All patients provided written informed consent before any study-related procedure.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Key Points
• RYGB led to favourable short-term effects on multiple metabolic pathways.
• Systemic inflammation was reduced 6 months post-RYGB.
• Branched-chain amino acids were the most affected metabolites 6 months post-RYGB.
• Physiological changes via weight and insulin mediated the post-RYGB metabolism.
Supplementary Information
ESM 1
(DOCX 8.84 MB)
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Zhao, S., Hörkkö, S., Savolainen, M.J. et al. Short-Term Metabolic Changes and Their Physiological Mediators in the Roux-en-Y Gastric Bypass Bariatric Surgery. OBES SURG 34, 625–634 (2024). https://doi.org/10.1007/s11695-023-07042-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-023-07042-y