Abstract
Purpose
Metabolic and bariatric surgery (MBS) is the most effective treatment for metabolic syndrome (MetS). However, the mechanism of MetS remission after MBS remains unclear. We aimed to explore the relationship between sex differences, body composition, and the remission of MetS after MBS.
Materials and Methods
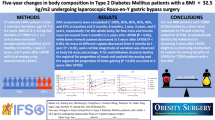
Cross-sectional study of 80 patients with obesity and MetS who underwent MBS with case-control design. The International Diabetes Federation criteria were used to define MetS. Body composition was measured using dual-energy X-ray absorptiometry before and 1 year after the operation. In addition to calculating changes in MetS and its prevalence, we performed a multiple logistic regression to determine predictors of MetS remission.
Results
There were significant differences in body composition between males and females after MBS. Both males and females had significant improvements in the overall prevalence of MetS, decreasing from 100 to 21.74% (P <0.001) and from 100 to 35.29% (P <0.001), respectively. A higher percentage of visceral adipose tissue (VAT) reduction tends to be associated with a higher chance of MetS remission in men. In females, the MetS nonremission subgroup had a higher %Trunk lean body mass (LBM), and %Android LBM reduction than the remission subgroup, but the multiple logistic regression analysis result was not statistically significant.
Conclusion
After MBS, reduced VAT might be related to MetS reversibility in males, while reduced LBM may result in MetS nonremission in females.
Graphical Abstract



Similar content being viewed by others
Data Availability
The datas used and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
NCD Risk Factor Collaboration (NCD-RisC). Trends in adult body-mass index in 200 countries from 1975 to 2014: a pooled analysis of 1698 population-based measurement studies with 19.2 million participants. Lancet. 2016(387):1377–96.
Mitchell JD. Personalizing risk assessment in diabetes mellitus and metabolic syndrome. J Am Coll Cardiol Img. 2021;14:230–2.
Hanipah ZN, Schauer PR. Bariatric surgery as a long-term treatment for type 2 diabetes/metabolic syndrome. Annu Rev Med. 2020;71:1–15.
Batterham RL, Cummings DE. Mechanisms of diabetes improvement following bariatric/metabolic surgery. Diabetes Care. 2016;39:893–901.
Madsbad S, Dirksen C, Holst JJ. Mechanisms of changes in glucose metabolism and bodyweight after bariatric surgery. Lancet Diabetes Endocrinol. 2014;2:152–64.
Cho YM. A gut feeling to cure diabetes: potential mechanisms of diabetes remission after bariatric surgery. Diabetes Metab J. 2014;38:406–15.
Alomar AO, Shaheen MF, Almaneea AS, et al. The effect of bariatric surgery on metabolic syndrome: a three-center experience in Saudi Arabia. Obes Surg. 2021;31:3630–6.
Yu H, Zhang L, Bao Y, et al. Metabolic syndrome after Roux-en-Y gastric bypass surgery in Chinese obese patients with type 2 diabetes. Obes Surg. 2016;26:2190–7.
Silva LB, Oliveira B, Correia F. Evolution of body composition of obese patients undergoing bariatric surgery. Clinical Nutrition ESPEN. 2019;31:95–9.
Tchernof A, Després JP. Pathophysiology of human visceral obesity: an update. Physiol Rev. 2013;93:359–404.
Ibrahim MM. Subcutaneous and visceral adipose tissue: structural and functional differences. Obes Rev. 2010;11:11–8.
Després JP, Allard C, Tremblay A, et al. Evidence for a regional component of body fatness in the association with serum lipids in men and women. Metabolism. 1985;34:967–73.
Sharma AM, Engeli S, Pischon T. New developments in mechanisms of obesity-induced hypertension: role of adipose tissue. Curr Hypertens Rep. 2001;3:152–6.
Rocchini AP. Obesity hypertension. Am J Hypertens. 2002;15:50s–2s.
Qian J, Scheer F. Sex-dependent link between circadian misalignment and adiposity. Nat Rev Endocrinol. 2020;16:13–5.
Reue K. Sex differences in obesity: X chromosome dosage as a risk factor for increased food intake, adiposity and co-morbidities. Physiol Behav. 2017;176:174–82.
Powell-Wiley TM, Poirier P, Burke LE, et al. Obesity and cardiovascular disease: a scientific statement from the American Heart Association. Circulation. 2021;143:CIR0000000000000973.
CZ JL, Wang Y, et al. Guidelines for surgical treatment of obesity and type 2 diabetes mellitus in China. Chin J Pract Surg. 2014;34:6.
Agha R, Abdall-Razak A, Crossley E, et al. STROCSS 2019 Guideline: strengthening the reporting of cohort studies in surgery. Int J Surg. 2019;72:156–65.
Brethauer SA, Kim J, El Chaar M, et al. Standardized outcomes reporting in metabolic and bariatric surgery. Obes Surg. 2015;25:587–606.
Alberti G, Zimmet P, Shaw J, et al. The IDF consensus worldwide definition of the metabolic syndrome. The Lancet. 2005;366:1059–62.
Wilding J. Weight loss is the major player in bariatric surgery benefits. Nat Med. 2020;26:1678–9.
To VT, Hüttl TP, Lang R, et al. Changes in body weight, glucose homeostasis, lipid profiles, and metabolic syndrome after restrictive bariatric surgery. Exp Clin Endocrinol Diabetes. 2012;120:547–52.
Busetto L, Pisent C, Rinaldi D, et al. Variation in lipid levels in morbidly obese patients operated with the LAP-BAND adjustable gastric banding system: effects of different levels of weight loss. Obes Surg. 2000;10:569–77.
Guerreiro V, Neves JS, Salazar D, et al. Long-term weight loss and metabolic syndrome remission after bariatric surgery: the effect of sex, age, metabolic parameters and surgical technique - a 4-year follow-up study. Obes Facts. 2019;12:639–52.
Gloy VL, Briel M, Bhatt DL, et al. Bariatric surgery versus non-surgical treatment for obesity: a systematic review and meta-analysis of randomised controlled trials. Bmj. 2013;347:f5934.
Maïmoun L, Lefebvre P, Aouinti S, et al. Acute and longer-term body composition changes after bariatric surgery. Surg Obes Relat Dis. 2019;15:1965–73.
Haghighat N, Kazemi A, Asbaghi O, et al. Long-term effect of bariatric surgery on body composition in patients with morbid obesity: a systematic review and meta-analysis. Clin Nutr. 2021;40:1755–66.
Davidson LE, Yu W, Goodpaster B, et al. Fat weight increases while fat-free mass decreases in women 5 years after gastric bypass surgery. Obes Rev. 2016;17:60.
Domínguez Alvarado GA, Otero Rosales MC, Cala Duran JC, et al. The effect of bariatric surgery on metabolic syndrome: a retrospective cohort study in Colombia. Health science reports. 2023;6:e1090.
Menguer RK, Weston AC, Schmid H. Evaluation of metabolic syndrome in morbidly obese patients submitted to laparoscopic bariatric surgery: comparison of the results between Roux-en-Y gastric bypass and sleeve gastrectomy. Obes Surg. 2017;27:1719–23.
Mahawar KK, Graham Y, Carr WR, et al. Revisional Roux-en-Y gastric bypass and sleeve gastrectomy: a systematic review of comparative outcomes with respective primary procedures. Obes Surg. 2015;25:1271–80.
Coblijn UK, Verveld CJ, van Wagensveld BA, et al. Laparoscopic Roux-en-Y gastric bypass or laparoscopic sleeve gastrectomy as revisional procedure after adjustable gastric band--a systematic review. Obes Surg. 2013;23:1899–914.
Knopp KB, Stakleff KS, Thomas TM, et al. Gender influence on weight and body composition following sleeve gastrectomy: outcomes suggest potential bariatric surgery body composition goals. Bariatric Surgical Practice and Patient Care. 2020;15:205–10.
Blouin K, Boivin A, Tchernof A. Androgens and body fat distribution. J Steroid Biochem Mol Biol. 2008;108:272–80.
Blouin K, Després JP, Couillard C, et al. Contribution of age and declining androgen levels to features of the metabolic syndrome in men. Metabolism. 2005;54:1034–40.
Gapstur SM, Gann PH, Kopp P, et al. Serum androgen concentrations in young men: a longitudinal analysis of associations with age, obesity, and race. The CARDIA male hormone study. Cancer Epidemiol Biomarkers Prev. 2002;11:1041–7.
Laaksonen DE, Niskanen L, Punnonen K, et al. Testosterone and sex hormone-binding globulin predict the metabolic syndrome and diabetes in middle-aged men. Diabetes Care. 2004;27:1036–41.
Pasquali R, Casimirri F, Cantobelli S, et al. Effect of obesity and body fat distribution on sex hormones and insulin in men. Metabolism. 1991;40:101–4.
Liu J, Fox CS, Hickson DA, et al. Impact of abdominal visceral and subcutaneous adipose tissue on cardiometabolic risk factors: the Jackson Heart Study. J Clin Endocrinol Metab. 2010;95:5419–26.
Neeland IJ, Yokoo T, Leinhard OD, et al. 21st century advances in multimodality imaging of obesity for care of the cardiovascular patient. J Am Coll Cardiol Img. 2021;14:482–94.
Xia L, Hua J, Dray X, et al. Endoscopic visceral fat removal as therapy for obesity and metabolic syndrome: a sham-controlled pilot study (with video). Gastrointest Endosc. 2011;74:637–44.
Vaurs C, Diméglio C, Charras L, et al. Determinants of changes in muscle mass after bariatric surgery. Diabetes Metab. 2015;41:416–21.
Kaneko S, Iida RH, Suga T, et al. Changes in triacylglycerol-accumulated fiber type, fiber type composition, and biogenesis in the mitochondria of the soleus muscle in obese rats. Anat Rec. 2011;294:1904–12.
Nuijten MAH, Eijsvogels TMH, Monpellier VM, et al. The magnitude and progress of lean body mass, fat-free mass, and skeletal muscle mass loss following bariatric surgery: a systematic review and meta-analysis. Obesity reviews. 2021;23:e13370.
Park SH, Park JH, Park HY, et al. Additional role of sarcopenia to waist circumference in predicting the odds of metabolic syndrome. Clin Nutr. 2014;33:668–72.
Funding
This research was supported by the Wisdom Accumulation and Talent Cultivation Project of the Third Xiangya Hospital of Central South University (YX202102).
Author information
Authors and Affiliations
Contributions
Study design: LZ, SZ. Conduct/data collection: XY, WL, PL. Data extraction: XS, GW, HZ. Data analysis: XY, HT, JL, BC, PL, ZF. Writing manuscript: XY, WL. Critical revision: LZ, SZ. All authors have participated sufficiently in the study and approved the final version.
Corresponding authors
Ethics declarations
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Consent to Participate
Informed consent was obtained from all individual participants included in the study.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Key Points
1. Both males and females had significant improvements in MetS after MBS.
2. Reduced VAT might be related to MetS reversibility in males after MBS.
3. While reduced LBM may result in MetS nonremission in females.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yi, X., Li, W., Wang, G. et al. Sex-Specific Changes in Body Composition Following Metabolic and Bariatric Surgery Are Associated with the Remission of Metabolic Syndrome. OBES SURG 33, 2780–2788 (2023). https://doi.org/10.1007/s11695-023-06741-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-023-06741-w