Abstract
Background
Sleeve gastrectomy has been considered a primary bariatric surgery; however, surgeons concerned with staple line leakage often query whether staples selected during stomach resection are of an appropriate size. This study aimed to measure gastric wall thickness using pathology laboratory measurements and to identify variables correlated with stomach wall thickness in patients who had undergone laparoscopic sleeve gastrectomy.
Methods
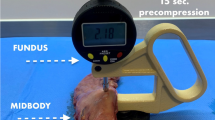
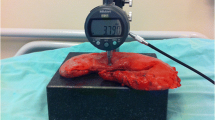
We obtained fresh resected stomach wall specimens from 30 patients. Stomach wall thickness was immediately measured postoperatively, comprising the muscle layer of the antrum, body, and fundus. Results were correlated with body mass index (BMI), age, and sex and with diagnoses of presurgical diabetes, hypertension, hyperlipidemia, and fatty liver.
Results
Stomach wall thickness ranged from 3.4 ± 4.3 mm to 1.0 ± 9.6 mm at the antrum. Except for the whole layer at the body wall, there was no significant correlation between wall thickness and other factors. At the body wall, whole layer wall thickness was found to positively correlate with age, sex, diabetes, and smoking (r = 0.469, − 0.391, 0.396, and 0.349, respectively; p < 0.05 in all patients).
Conclusion
Stomach wall thickness varied among patients who had undergone laparoscopic sleeve gastrectomy according to samples taken at three stomach wall sites. The range in wall thickness was normal, and thus, surgeons need not hesitate in selecting the staple height. Also, our study may be helpful to guide surgeon choice concerning the third or fourth staple around the body area when considering a patient’s independent factors.

Similar content being viewed by others
References
Nguyen NT, Root J, Zainabadi K, et al. Accelerated growth of bariatric surgery with the introduction of minimally invasive surgery. Arch Surg. 2005;140:1198–202; discussion 1203. https://doi.org/10.1001/archsurg.140.12.1198.
McCracken J, Steinbeisser M, Kharbutli B. Does size matter? Correlation of excised gastric specimen size in sleeve gastrectomy to postoperative weight loss and comorbidities. Obes Surg. 2018;28:1002–6. https://doi.org/10.1007/s11695-017-2975-0.
ElGeidie A, ElHemaly M, Hamdy E, et al. The effect of residual gastric antrum size on the outcome of laparoscopic sleeve gastrectomy: a prospective randomized trial. Surg Obes Relat Dis. 2015;11:997–1003. https://doi.org/10.1016/j.soard.2014.12.025.
Bohdjalian A, Langer FB, Shakeri-Leidenmuhler S, et al. Sleeve gastrectomy as sole and definitive bariatric procedure: 5-year results for weight loss and ghrelin. Obes Surg. 2010;20:535–40. https://doi.org/10.1007/s11695-009-0066-6.
Shi X, Karmali S, Sharma AM, et al. A review of laparoscopic sleeve gastrectomy for morbid obesity. Obes Surg. 2010;20:1171–7. https://doi.org/10.1007/s11695-010-0145-8.
Derici S, Atila K, Bora S. The effect of the cartridge used in laparoscopic sleeve gastrectomy on the development of a staple-line leak. Am Surg. 2018;84:1499–503. PMID: 30268184
Huang R, Gagner M. A thickness calibration device is needed to determine staple height and avoid leaks in laparoscopic sleeve gastrectomy. Obes Surg. 2015;25:2360–7. https://doi.org/10.1007/s11695-015-1705-8.
Boeker C, Mall J, Reetz C, et al. Laparoscopic sleeve gastrectomy: investigation of fundus wall thickness and staple height-an observational cohort study: fundus wall thickness and leaks. Obes Surg. 2017;27:3209–14. https://doi.org/10.1007/s11695-017-2755-x.
Abu-Ghanem Y, Meydan C, Segev L, et al. Gastric wall thickness and the choice of linear staples in laparoscopic sleeve gastrectomy: challenging conventional concepts. Obes Surg. 2017;27:837–43. https://doi.org/10.1007/s11695-016-2516-2.
Barski K, Binda A, Kudlicka E, et al. Gastric wall thickness and stapling in laparoscopic sleeve gastrectomy — a literature review. Wideochir Inne Tech Maloinwazyjne. 2017;13:122–7. https://doi.org/10.5114/wiitm.2018.73362.
Colquitt JL, Pickett K, Loveman E, et al. Surgery for weight loss in adults. Cochrane Database Syst Rev. 2014;8:Cd003641. https://doi.org/10.1002/14651858.cd003641.pub4.
Gagner M. Decreased incidence of leaks after sleeve gastrectomy and improved treatments. Surg Obes Relat Dis. 2014;10:611–2. https://doi.org/10.1016/j.soard.2014.04.002.
Rawlins L, Rawlins MP, Teel II D. Human tissue thickness measurements from excised sleeve gastrectomy specimens. Surg Endosc. 2014;28:811–4. https://doi.org/10.1007/s00464-013-3264-1.
Acknowledgments
We would like to express our wholehearted gratitude to all participating patients.
Funding
This research was supported by a grant of Korea University Anam Hospital, Seoul, Repulic of Korea (Grant No. O1904911).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflicts of interest.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Statement of Informed Consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Lee, Y.J., Kim, Y.N. & Park, S. Measurement of Stomach Wall Thickness to Guide Staple Selection during Sleeve Gastrectomy. OBES SURG 30, 2140–2146 (2020). https://doi.org/10.1007/s11695-020-04439-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-020-04439-x