Abstract
Background and Aims
Transoral outlet reduction (TORe) by devitalization and/or endoscopic suturing (ES) has been implemented in the management of weight regain post-RYGB. This study aims to assess the efficacy and safety of TORe following an insurance-based algorithm.
Methods
A prospectively maintained database of patients who underwent TORe between September 2015 and January 2018 at a single academic center was reviewed. An algorithm was followed whereby management was based on insurance coverage. As part of the algorithm, all patients presented for a repeat endoscopy at 8 weeks. Patients did not receive any diet, lifestyle intervention, or pharmacotherapy.
Results
In total, 55 patients were included (median age 48 years), out of which 50 were females (90.9%). Patients presented for evaluation at a mean of 8.7 years post-RYGB. The main presenting symptom was combined dumping syndrome (DS) and weight regain (49.1%), followed by weight regain alone (45.5%). Twenty-nine patients required treatment at their second procedure, and 11 required treatment at their third procedure. Average percent total body weight loss (%TBWL) after TORe observed at 3-, 6-, 9-, and 12-month follow-up was 8.2, 9.3, 8.4, and 5.5%, respectively. The mean DS Severity Score was significantly reduced from 23.3 ± 12.4 before TORe to 16.3 ± 6.51 after TORe (p < 0.01). The adverse event rate from TORe was 14.5%.
Conclusion
TORe is effective in halting ongoing weight regain and achieving moderate short-term weight loss as well as improving DS in post-RYGB patients. Durability at 1 year remains questionable due to weight recidivism.





Similar content being viewed by others
References
Kang JH, Le QA. Effectiveness of bariatric surgical procedures: a systematic review and network meta-analysis of randomized controlled trials. Medicine (Baltimore). 2017;96(46):e8632.
Emous M, Wolffenbuttel BHR, Totté E, et al. The short- to mid-term symptom prevalence of dumping syndrome after primary gastric-bypass surgery and its impact on health-related quality of life. Surg Obes Relat Dis. 2017;13(9):1489–500.
Christou NV, Look D, Maclean LD. Weight gain after short- and long-limb gastric bypass in patients followed for longer than 10 years. Ann Surg. 2006;244(5):734–40.
Magro DO, Geloneze B, Delfini R, et al. Long-term weight regain after gastric bypass: a 5-year prospective study. Obes Surg. 2008;18(6):648–51.
Monaco-Ferreira DV, Leandro-Merhi VA. Weight regain 10 years after Roux-en-Y gastric bypass. Obes Surg. 2017;27(5):1137–44.
English WJ, DeMaria EJ, Brethauer SA, et al. American Society for Metabolic and Bariatric Surgery estimation of metabolic and bariatric procedures performed in the United States in 2016. Surg Obes Relat Dis. 2018;14(3):259–63.
Tran DD, Nwokeabia ID, Purnell S, et al. Revision of Roux-En-Y gastric bypass for weight regain: a systematic review of techniques and outcomes. Obes Surg. 2016;26(7):1627–34.
Bjorklund P et al. Is the Roux limb a determinant for meal size after gastric bypass surgery? Obes Surg. 2010;20(10):1408–14.
le Roux CW, Welbourn R, Werling M, et al. Gut hormones as mediators of appetite and weight loss after Roux-en-Y gastric bypass. Ann Surg. 2007;246(5):780–5.
Sinclair P, Brennan DJ, le Roux CW. Gut adaptation after metabolic surgery and its influences on the brain, liver and cancer. Nat Rev Gastroenterol Hepatol. 2018;15(10):606–24.
Shantavasinkul PC, Omotosho P, Corsino L, et al. Predictors of weight regain in patients who underwent Roux-en-Y gastric bypass surgery. Surg Obes Relat Dis. 2016;12(9):1640–5.
Abu Dayyeh BK, Lautz DB, Thompson CC. Gastrojejunal stoma diameter predicts weight regain after Roux-en-Y gastric bypass. Clin Gastroenterol Hepatol. 2011;9(3):228–33.
Ramadan M et al. Risk of dumping syndrome after sleeve gastrectomy and Roux-en-Y gastric bypass: early results of a multicentre prospective study. Gastroenterol Res Pract. 2016;2016:2570237.
Kumar N, Thompson CC. Transoral outlet reduction for weight regain after gastric bypass: long-term follow-up. Gastrointest Endosc. 2016;83(4):776–9.
Patel LY, Lapin B, Brown CS, et al. Outcomes following 50 consecutive endoscopic gastrojejunal revisions for weight gain following Roux-en-Y gastric bypass: a comparison of endoscopic suturing techniques for stoma reduction. Surg Endosc. 2017;31(6):2667–77.
Thompson CC, Jacobsen GR, Schroder GL, et al. Stoma size critical to 12-month outcomes in endoscopic suturing for gastric bypass repair. Surg Obes Relat Dis. 2012;8(3):282–7.
Vargas EJ, Bazerbachi F, Rizk M, et al. Transoral outlet reduction with full thickness endoscopic suturing for weight regain after gastric bypass: a large multicenter international experience and meta-analysis. Surg Endosc. 2017.
Jirapinyo P, Dayyeh BK, Thompson CC. Gastrojejunal anastomotic reduction for weight regain in roux-en-y gastric bypass patients: physiological, behavioral, and anatomical effects of endoscopic suturing and sclerotherapy. Surg Obes Relat Dis. 2016;12(10):1810–6.
Jirapinyo P, Slattery J, Ryan MB, et al. Evaluation of an endoscopic suturing device for transoral outlet reduction in patients with weight regain following Roux-en-Y gastric bypass. Endoscopy. 2013;45(7):532–6.
Kumar N, Thompson CC. Comparison of a superficial suturing device with a full-thickness suturing device for transoral outlet reduction (with videos). Gastrointest Endosc. 2014;79(6):984–9.
Thompson CC, Chand B, Chen YK, et al. Endoscopic suturing for transoral outlet reduction increases weight loss after Roux-en-Y gastric bypass surgery. Gastroenterology. 2013;145(1):129–137 e3.
Barola S et al. Demonstration of transoral gastric outlet reduction: 2-fold running suture technique. VideoGIE. 2017;2(1):2–3.
Baretta GA et al. Argon plasma coagulation of gastrojejunal anastomosis for weight regain after gastric bypass. Obes Surg. 2015;25(1):72–9.
King WC, Hinerman AS, Belle SH, et al. Comparison of the performance of common measures of weight regain after bariatric surgery for association with clinical outcomes. JAMA. 2018;320(15):1560–9.
Laurenius A, Olbers T, Näslund I, et al. Dumping syndrome following gastric bypass: validation of the dumping symptom rating scale. Obes Surg. 2013;23(6):740–55.
Jirapinyo P, Kroner PT, Thompson CC. Purse-string transoral outlet reduction (TORe) is effective at inducing weight loss and improvement in metabolic comorbidities after Roux-en-Y gastric bypass. Endoscopy. 2018;50(4):371–7.
Author information
Authors and Affiliations
Contributions
Study conception and design: Schweitzer, Michael; Oberbach, Andreas; Kumbhari, Vivek; Fayad, Lea
Acquisition of data: Dunlap, Margo K.; Shah, Tazkia; Fayad, Lea
Analysis and interpretation of data: Raad, Micheal; Doshi, Jay; Oleas, Roberto; El Asmar, Margueritta, Fayad, Lea
Drafting of manuscript: Kumbhari, Vivek
Critical revision: Kalloo, Anthony N.; Khashab, Mouen A.; Steele, Kimberly; Magnussen, Thomas
Corresponding author
Ethics declarations
Ethical Approval
For this type of study formal consent is not required.
Informed Consent
Informed consent does not apply.
Conflict of Interest
Mouen A Khashab is on the medical advisory board for Boston scientific and Olympus America and is a consultant for Boston scientific, Olympus America, and Medtronic.
Anthony N Kalloo is a founding member, equity Holder, and consultant for Apollo Endosurgery.
Vivek Kumbhari is a consultant for Medtronic, Reshape Lifesciences, Boston Scientific, and Apollo Endosurgery. He also receives research support from ERBE USA and Apollo Endosurgery.
All other authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Video 3
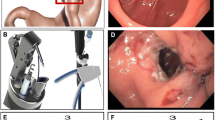
APC application to a GJA at follow-up EGD post-TORe with ES-APC (MP4 375,433 kb)
Rights and permissions
About this article
Cite this article
Fayad, L., Schweitzer, M., Raad, M. et al. A Real-World, Insurance-Based Algorithm Using the Two-Fold Running Suture Technique for Transoral Outlet Reduction for Weight Regain and Dumping Syndrome After Roux-En-Y Gastric Bypass. OBES SURG 29, 2225–2232 (2019). https://doi.org/10.1007/s11695-019-03828-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-019-03828-1