Abstract
Introduction
Anatomical and functional influences on gastric bypass (GBP) results are often poorly evaluated and not yet fully understood.
Purpose
The purpose of this study is to evaluate the influence of the gastric pouch volume and its emptying rate on long-term weight loss and food tolerance after GBP.
Materials and Methods
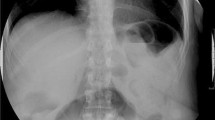
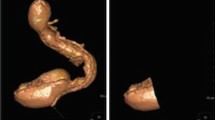
Weight loss, food tolerance, pouch volumetry (V) by three-dimensional reconstruction, and pouch emptying rate by 4 h scintigraphy were evaluated in 67 patients. Cutoffs were identified for V and retention percentage (%Ret) at 1 h (%Ret1). From these parameters, the sample was categorized, looking for associations between V, %Ret, weight loss, and food tolerance, assessed by a questionnaire for quick assessment of food tolerance (SS).
Results
PO median follow-up time was 47 months; median V was 28 mL; %Ret at 1, 2, and 4 h were 8, 2, and 1%, respectively. There were associations between V ≤ 40 mL and higher emptying rates up to 2 h (V ≤ 40 mL: %Ret1 = 6, %Ret2 = 2, p = 0.009; V > 40 mL: %Ret1 = 44, %Ret2 = 13.5, p = 0.045). An association was found between higher emptying speed in 1 h and higher late weight loss (WL), represented by lower percentage of excess weight loss (%EWL) regain (p = 0.036) and higher %EWL (p = 0.033) in the group with %Ret1 ≤ 12%, compared to the group %Ret1 ≥ 25%. Better food tolerance (SS > 24), was associated with lower %Ret1 (p = 0.003).
Conclusion
Smaller pouch size is associated with a faster gastric emptying, greater WL maintenance, and better food tolerance. These data suggest that a small pouch with rapid emptying rate is an important technical parameter for good outcomes in GBP.




Similar content being viewed by others
References
Buchwald H, Buchwald JN. Evolution of operative procedures for the management of morbid obesity 1950–2000. Obes Surg. 2002;12:705–17.
Fobi MA, Fleming AW. Vertical banded gastroplasty vs gastric bypass in the treatment of obesity. J Natl Med Assoc. 1986;78(11):1091–8.
Wittgrove AC, Clark GW, Schubert K. Laparoscopic gastric bypass, Roux-en-Y: technique and results 75 patients with 3–30 month follow-up. Obes Surg. 1996;6:500–4.
Capella RF, Iannace VA, Capela JF. An analysis of gastric pouch anatomy in bariatric surgery. Obes Surg. 2008;18:782–90.
le Roux CW, Aylwin SJ, Batterham RL, et al. Gut hormones profiles following bariatric surgery favor an anoretic state, facilitate weight loss, and improve metabolic parameters. Ann Surg. 2006;243(1):108–14.
Näslund E, Kral JG. Impact of gastric bypass surgery on gut hormones and glucose homeostasis in type 2 diabetes. Diabetes. 2006;55(S2):S92–7.
Cummings DE, Overduin J. Gastrointestinal regulation of food intake. J Clin Invest. 2007;117(1):13–23.
Miras AD, le Roux CW. Mechanisms underlying weight loss after bariatric surgery. Nat Rev Gastroenterol Hepatol. 2013;10(10):575–84.
Dirksen C, Damgaard M, Bojsen-Møller KN, et al. Fast pouch emptying, delayed small intestinal transit, and exaggerated gut hormone responses after Roux-en-Y gastric bypass. Neurogastroenterol Motil. 2013;25(4):346–e255.
Karmali S, Balpreet B, Shi X, et al. Weight recidivism post-bariatric surgery: a systematic review. Obes Surg. 2013;23:1922–33.
Toppino M, Cesarini F, Comba A, et al. The role of early radiological studies after gastric bariatric surgery. Obes Surg. 2001;11:447–54.
Brethauer SA, Nfonsam V, Sherman V, et al. Endoscopy and upper gastrointestinal contrast studies are complimentary in evaluation of weight regain after bariatric surgery. Surg Obes Relat Dis. 2006;2(6):643–8.
Alva S, Eisenberg D, Duffy A, et al. A new modality to evaluate the gastric remnant after Roux-en-Y gastric bypass. Surg Obes Relat Dis. 2008;4:46–9.
Blanchet M, Mesmann C, Yanes M, et al. 3D gastric computed tomography as a new imaging in patients with failure or complication after bariatric surgery. Obes Surg. 2010;20:1727–33.
Flanagan L. Measurement of functional pouch volume following the gastric bypass procedure. Obes Surg. 1996;6(1):38–43.
Seok JW. How to interpret gastric emptying scintigraphy. J Neurogastroenterol Motil. 2011;17(2):189–91.
Santo MA, Riccioppo D, Pajecki D, et al. Preoperative weight loss in super-obese patients: study of the rate of weight loss and its effects on surgical morbidity. Clinics (Sao Paulo). 2014;69(12):828–34.
Suter M, Calmes J, Paroz A, et al. A new questionnaire for quick assessment of food tolerance after bariatric surgery. Obes Surg. 2007;17:2–8.
Hothorn T, Lausen B. On the exact distribution of maximally selected rank statistics. Computational Statistics & Data Analysis. 2003;43:121–37.
Magro DO, Geloneze B, Delfini D, et al. Long-term weight regain after gastric bypass: a 5-year prospective study. Obes Surg. 2008;18:648–51.
Faria SL, de Oliveira KE, Faria OP, et al. Snack-eating patients experience lesser weight loss after Roux-en-Y gastric bypass surgery. Obes Surg. 2009;19(9):1293–6.
Hsieh T, Zurita L, Grover H, et al. 10-year outcomes of the vertical transected gastric bypass for obesity: a systematic review. Obes Surg. 2014;24:456–61.
Mechanick JI, Kushner RF, Sugerman HJ, et al. American Association of Clinical Endocrinologists, The Obesity Society, and American Society for Metabolic and Bariatric Surgery medical guide lines for clinical practice for the perioperative nutritional, metabolic and nonsurgical support of the bariatric surgery patient. Surg Obes Relat Dis. 2008;4(5 Suppl):S109–84.
Heneghan HM, Annaberdyev S, Eldar S, et al. Banded Roux-en-Y gastric bypass for the treatment of morbid obesity. Surg Obes Relat Dis. 2014;10(2):210–6.
Ernst B, Thurnheer M, Wilms B, et al. Differential changes in dietary habits after gastric bypass versus gastric banding operations. Obes Surg. 2009;19(3):274–80.
Buchwald H, Avidor Y, Braunwald E, et al. Bariatric surgery: a systematic review and meta analysis. JAMA. 2004;292:1724–37.
Sjöström L. Review of the key results from the Swedish Obese Subjects (SOS) trial—a prospective controlled intervention study of bariatric surgery. J Int Med. 2013;273:219–34.
Valezi AC, Brito SJ, Mali Jr J, et al. Estudo do padrão alimentar tardio em obesos submetidos à derivação gástrica com bandagem em Y-de-Roux: comparação entre homens e mulheres [Late meal pattern in obese people after banded Roux-en-Y gastric bypass: comparison between male and female]. Rev Col Bras Cir. 2008;35(6):387–91.
Reinhold RB. Critical analysis of long-term weight loss following gastric bypass. Surg Gynecol Obstet. 1982;155:385–94.
Higa KD, Ho T, Boone KB. Laparoscopic Roux-en-Y gastric bypass: technique and 3-year follow-up. J Laparoendosc Adv Surg Tech A. 2001;11(6):377–82.
Madan AK, Tichansky DS, Phillips JC. Does pouch size matter? Obes Surg. 2007;17:317–20.
Campos GM, Rabl C, Mulligan K, et al. Factors associated with weight loss after gastric bypass. Arch Surg. 2008;143(9):877–84.
Patel S, Szomstein S, Rosenthal RJ. Reasons and outcomes of reoperative bariatric surgery for failed and complicated procedures (excluding adjustable gastric banding). Obes Surg. 2011;21:1209–19.
Topart P, Becouarn G, Ritz P. Pouch size after gastric bypass does not correlate with weight loss outcome. Obes Surg. 2011;21:1350–4.
Palermo M, Acquafresca PA, Rogula T, et al. Late surgical complications after gastric by-pass: a literature review. Arq Bras Cir Dig. 2015;28(2):139–43.
Rasera Jr I, Coelho TH, Ravelli MN, et al. A comparative, prospective and randomized evaluation of Roux-en-Y gastric bypass with and without the silastic ring: a 2-year follow up preliminary report on weight loss and quality of life. Obes Surg. 2016;26(4):762–8.
Colles SL, Dixon JB, O’Brien PE. Grazing and loss of control related to eating: two high-risk factors following bariatric surgery. Obesity (Silver Spring). 2008;16(3):615–22.
Mallory GN, Macgregor AM, Rand CS. The influence of dumping on weight loss after gastric restrictive surgery for morbid obesity. Obes Surg. 1996;6(6):474–8.
Dapri G, Cadière GB, Himpens J. Laparoscopic placement of non-adjustable silicone ring for weight regain after Roux-en-Y gastric bypass. Obes Surg. 2009;19:650–4.
Horgan S, Jacobsen G, Weiss GD, et al. Incisionless revision of post Roux-en-Y bypass stomal and pouch dilatation: multicenter registry results. Surg Obes Rel Dis. 2010;6:290–5.
Dirksen C, Jørgensen NB, Bojsen-Møller KN, et al. Gut hormones, early dumping and resting energy expenditure in patients with good and poor weight loss response after Roux-en-Y gastric bypass. Int J Obes. 2013;37(11):1452–9.
Santo MA, Riccioppo D, Pajecki D, et al. Weight regain after gastric bypass: influence of gut hormones. Obes Surg. 2016;26(5):919–25.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent was obtained from all individual participants included in the study.
Conflict of Interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Riccioppo, D., Santo, M.A., Rocha, M. et al. Small-Volume, Fast-Emptying Gastric Pouch Leads to Better Long-Term Weight Loss and Food Tolerance After Roux-en-Y Gastric Bypass. OBES SURG 28, 693–701 (2018). https://doi.org/10.1007/s11695-017-2922-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-017-2922-0