Background
Mechanical restriction, malabsorption, and hormonal changes appear to play a role in weight loss after Roux-en-Y gastric bypass (RYGBP). This investigation chose to investigate one aspect of the restrictive role of gastric bypass: the pouch size. Our hypothesis was that a small pouch size with no fundus after laparoscopic RYGBP (LRYGBP) would lead to greater loss of excess weight and weight loss success.
Methods
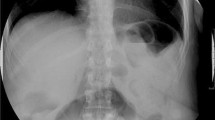
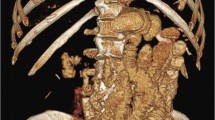
Upper gastrointestinal radiological (UGI) studies were retrospectively reviewed by three blinded experts (2 bariatric surgeons and 1 expert radiologist), to determine pouch size and fundus size. The following grading system was utilized: Size I - smaller than average pouch, Size II - average pouch, Size III - larger than average pouch, and Size IV - over 3 times the size of an average pouch. Fundus 0 - no fundus appreciated, Fundus I - slight amount of fundus barely noted, Fundus II - fundus noted, Fundus III - large amount of fundus noted, and Fundus IV - majority of the pouch was fundus. Percentage of excess weight loss (%EWL) and successful weight loss (A. >50% EWL, B. within 50% of ideal body weight, C. loss of >25% of preoperative weight) were calculated.
Results
There were 59 patients in this study with 97% follow-up of >1 year. No Size IV or Fundus IV were noted. There were no statistically significant differences between in %EWL or success for either pouch size or fundus size.
Conclusions
While there may be a trend for the mean %EWL to be lower with larger pouches and larger amounts of fundus, no significant differences were found. Larger pouches and the presence of fundus (within reason) still result in a high rate of success after LRYGBP.
Similar content being viewed by others
References
Buchwald H, Williams SE. Bariatric surgery worldwide 2003. Obes Surg 2004; 14: 1157–64.
Maggard MA, Shugarman LR, Suttorp M et al. Metaanalysis: Surgical treatment of obesity. Ann Intern Med 2005; 142: 547–59.
Sjostrom L, Lindroos AK, Peltonen M et al. Lifestyle, diabetes, and cardiovascular risk factors 10 years after bariatric surgery. N Engl J Med 2004; 351: 2683–93.
Madan AK, Frantzides CT. Triple-stapling technique for jejunojejunostomy in laparoscopic gastric bypass. Arch Surg 2003; 138: 1029–32.
Deitel M, Greenstein RJ. Recommendations for reporting weight loss. Obes Surg 2003; 13: 159–60.
Flanagan L Jr. Measurement of functional pouch volume following the gastric bypass procedure. Obes Surg 1996;6:38–43.
Bechtold DL. Pouch size in failed vertical banded gastroplasty: comparison of upper GI and surgical measurements. American Society for Bariatric Surgery, Iowa City, IA, June 3,1988 (Poster 11).
Miskowiak J, Fleckenstein P, Anderson B. Radiologic findings and weight loss following gastroplasty for morbid obesity. Acta Radiol Diagn 1986; 27: 553–5.
Salmon PA. Failure of gastroplasty pouch and stoma size to correlate with postoperative weight loss. Can J Surg 1986; 29: 60–3.
Anderson T, Pedersen BH, Henriksen JH et al. Food intake in relation to pouch volume, stoma diameter, and pouch emptying after gastroplasty for morbid obesity. Scan J Gastroenterol 1988; 23: 1057–62.
Andersen T, Pedersen BH. Pouch volume, stoma diameter, and clinical outcome after gastroplasty for morbid obesity. A prospective study. Scand J Gastroenterol 1984; 19: 643–9.
Backman L, Rosenborg M. The significance of gastric pouch size and emptying time for results of gastric surgery for massive obesity. Acta Chir Scand 1984; 150: 549–55.
Lundell L, Forssell H, Jensen J et al. Measurement of pouch volume and stoma diameter after gastroplasty. Int J Obes 1987; 11: 169–74.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Madan, A.K., Tichansky, D.S. & Phillips, J.C. Does Pouch Size Matter?. OBES SURG 17, 317–320 (2007). https://doi.org/10.1007/s11695-007-9058-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-007-9058-6