Abstract
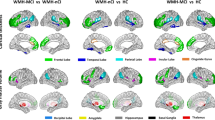
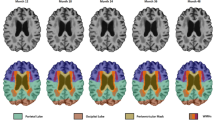
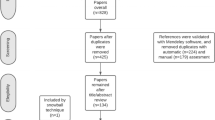
Prior meta-analyses have provided important information regarding which brain areas are structurally compromised in individuals with mild cognitive impairment (MCI). These studies have not however separated volume, density, and thickness, controlled for important demographic influences, considered null findings, or recognized studies indicating increased brain volumes in MCI individuals. Furthermore, there is a question as to whether deficits extend into cortical regions, and also into the thalamus. This study aims to address these issues using activation likelihood estimation (ALE) analyses with a sample size more than twice that of prior meta-analyses. A total of 71 studies were identified and entered into the ALE analysis which consisted of 2262 with MCI and 1902 healthy controls. Three major clusters were identified showing decreased gray matter volume in the MCI group compared to controls, with the most salient decreases being in the hippocampus, parahippocampal gyrus, and the amygdala. Reduced thalamic volume was also observed, but to a lesser extent. Density was reduced in the left hippocampus, while thickness was reduced in the uncus. No significant cluster emerged from an ALE meta-analysis of studies finding volume increases in MCI individuals. While the MCI group was significantly older and less educated than controls, controlling for these factors still resulted in significant, albeit attenuated findings. These results support hippocampal and parahippocampal deficits in MCI, and further highlight the amygdala, thalamus, and uncus as other areas to be considered in future MCI studies.



Similar content being viewed by others
Data availability
Upon reasonable request.
References
Albajes-Eizagirre, A., Solanes, A., Vieta, E., & Radua, J. (2019, Feb). Voxel-based meta-analysis via permutation of subject images (PSI): Theory and implementation for SDM. Neuroimage, 186, 174–184. https://doi.org/10.1016/j.neuroimage.2018.10.077
Amina, S. (2014). Uncus. In M. J. Aminoff & R. B. Daroff (Eds.), Encyclopedia of the neurological sciences (2nd ed.). Elsevier.
Cohen, J. (1988). Statistical power analysis for the behavioral sciences (2nd ed.). Lawrence Erlbaum.
Eickhoff, S. B., Bzdok, D., Laird, A. R., Kurth, F., & Fox, P. T. (2012). Activation likelihood estimation revisited. Neuroimage, 59, 2349–2361.
Eickhoff, S. B., Laird, A. R., Grefkes, C., Wang, L. E., Zilles, K., & Fox, P. T. (2009). Coordinate-based activation likelihood estimation meta-analysis of neuroimaging data: A random-effects approach based on empirical estimates of spatial uncertainty. Human Brain Mapping, 30, 2907–2926.
Eickhoff, S. B., Nichols, T. E., Laird, A. R., Hoffstaedter, F., Amunts, K., Fox, P. T., . . . Eickhoff, C. R. (2016). Behavior, sensitivity, and power of activation likelihood estimation characterized by massive empirical simulation. Neuroimage, 137, 70–85. https://doi.org/10.1016/j.neuroimage.2016.04.072.
Fisher, S. D., Ferguson, L. A., Bertran-Gonzalez, J., & Balleine, B. W. (2020). Amygdala-cortical control of striatal plasticity drives the Acquisition of Goal-Directed Action. Current Biology, 30(22). https://doi.org/10.1016/j.cub.2020.08.090
Garcia, A. D., & Buffalo, E. A. (2020). Anatomy and function of the primate entorhinal cortex. In J. A. Movshon & B. A. Wandell (Eds.), Annual review of vision science, Vol 6, 2020 (Vol. 6, pp. 411–432).
Gauthier, S., Reisberg, B., Zaudig, M., Petersen, R. C., Ritchie, K., Broich, K., et al. (2006). Mild cognitive impairment. The Lancet, 367(9518), 1262–1270. https://doi.org/10.1016/S0140-6736(06)68542-5
Gennatas, E. D., Avants, B. B., Wolf, D. H., Satterthwaite, T. D., Ruparel, K., Ciric, R., . . . Gur, R. C. (2017). Age-related effects and sex differences in gray matter density, volume, mass, and cortical thickness from childhood to young adulthood. Journal of Neuroscience, 37(20), 5065–5073. https://doi.org/10.1523/jneurosci.3550-16.2017.
Giannouli, V., & Tsolaki, M. (2019). Are left angular gyrus and amygdala volumes important for financial capacity in mild cognitive impairment? Hellenic Journal of Nuclear Medicine, 22, 160-164. Retrieved from <go to ISI>://WOS:000474893400015.
Gu, L. H., & Zhang, Z. J. (2019). Exploring structural and functional brain changes in mild cognitive impairment: A whole brain ALE Meta-analysis for multimodal MRI. ACS Chemical Neuroscience, 10(6), 2823–2829. https://doi.org/10.1021/acschemneuro.9b00045
Hallab, A., Lange, C., Apostolova, I., Ozden, C., Gonzalez-Escamilla, G., Klutmann, S., . . . Alzheimers Dis Neuroimaging, I. (2020). Impairment of everyday spatial navigation abilities in mild cognitive impairment is weakly associated with reduced Grey matter volume in the medial part of the entorhinal cortex. Journal of Alzheimers Disease, 78(3), 1149–1159. https://doi.org/10.3233/jad-200520.
Janak, P. H., & Tye, K. M. (2015). From circuits to behaviour in the amygdala. Nature, 517(7534), 284–292. https://doi.org/10.1038/nature14188
Langa, K. M., & Levine, D. A. (2014). The diagnosis and Management of Mild Cognitive Impairment a Clinical Review. Jama-Journal of the American Medical Association, 312(23), 2551–2561. https://doi.org/10.1001/jama.2014.13806
Martin, E., & Velayudhan, L. (2020). Neuropsychiatric symptoms in mild cognitive impairment: A literature review. Dementia and Geriatric Cognitive Disorders, 49(2), 146–155. https://doi.org/10.1159/000507078
McClelland, J. L., McNaughton, B. L., & O'Reilly, R. C. (1995). Why are there complementary learning systems in the hippocampus and neocortex: Insights from the successes and failures of connectionist models of learning and memory. Psychological Review, 102(3), 419–457. https://doi.org/10.1037/0033-295x.102.3.419
Mitchell, A. S. (2015). The mediodorsal thalamus as a higher order thalamic relay nucleus important for learning and decision-making. Neuroscience and Biobehavioral Reviews, 54, 76–88. https://doi.org/10.1016/j.neubiorev.2015.03.001
Mitchell, B., Partida, G. C., Grasby, K., Strike, L., Thompson, P., Medland, S., . . . Renteria, M. (2019). Educational attainment polygenic risk scores predict surface area of cortical regions important for language and memory. Behavior Genetics, 49(6), 540-541. Retrieved from <go to ISI>://WOS:000494050500191.
Nickl-Jockschat, T., Kleiman, A., Schulz, J. B., Schneider, F., Laird, A. R., Fox, P. T., . . . Reetz, K. (2012). Neuroanatomic changes and their association with cognitive decline in mild cognitive impairment: A meta-analysis. Brain Structure & Function, 217(1), 115–125. https://doi.org/10.1007/s00429-011-0333-x.
Nordin, K., Herlitz, A., Larsson, E. M., & Soderlund, H. (2017). Overlapping effects of age on associative memory and the anterior hippocampus from middle to older age. Behavioural Brain Research, 317, 350–359. https://doi.org/10.1016/j.bbr.2016.10.002
Petersen, R. C., Lopez, O., Armstrong, M. J., Getchius, T. S. D., Ganguli, M., Gloss, D., . . . Amer Acad, N. (2018). Practice guideline update summary: Mild cognitive impairment: Report of the guideline development, dissemination, and implementation Subcommittee of the American Academy of neurology. Neurology, 90(3), 126–135. https://doi.org/10.1212/wnl.0000000000004826.
Petersen, R. C., Roberts, R. O., Knopman, D. S., Boeve, B. F., Geda, Y. E., Ivnik, R. J., . . . Jack, C. R. (2009). Mild cognitive impairment ten years later. Archives of Neurology, 66(12), 1447–1455. https://doi.org/10.1001/archneurol.2009.266.
Phelps, E. A. (2006). Emotion and cognition: Insights from studies of the human amygdala. Annual Review of Psychology, 57, 27–53. https://doi.org/10.1146/annurev.psych.56.091103.070234.
Sweeney-Reed, C. M., Buentjen, L., Voges, J., Schmitt, F. C., Zaehle, T., Kam, J. W. Y., . . . Rugg, M. D. (2021). The role of the anterior nuclei of the thalamus in human memory processing. Neuroscience and Biobehavioral Reviews, 126, 146–158. https://doi.org/10.1016/j.neubiorev.2021.02.046.
Talwar, P., Kushwaha, S., Chaturvedi, M., & Mahajan, V. (2021). Systematic review of different Neuroimaging correlates in mild cognitive impairment and Alzheimer's disease. Clinical Neuroradiology. https://doi.org/10.1007/s00062-021-01057-7
Taubert, M., Roggenhofer, E., Melie-Garcia, L., Muller, S., Lehmann, N., Preisig, M., . . . Draganski, B. (2020). Converging patterns of aging-associated brain volume loss and tissue microstructure differences. Neurobiology of Aging, 88, 108–118. https://doi.org/10.1016/j.neurobiolaging.2020.01.006.
Turkeltaub, P. E., Eickhoff, S. B., Laird, A. R., Fox, M., Wiener, M., & Fox, P. (2012). Minimizing within-experiment and within-group effects in activation likelihood estimation meta-analyses. Human Brain Mapping, 33(1), 1–13. https://doi.org/10.1002/hbm.21186
Vythilingam, M., Luckenbaugh, D. A., Lam, T., Morgan, C. A., Lipschitz, D., Charney, D. S., . . . Southwick, S. M. (2005). Smaller head of the hippocampus in gulf war-related posttraumatic stress disorder. Psychiatry Research-Neuroimaging, 139(2), 89–99. https://doi.org/10.1016/j.pscychresns.2005.04.003.
Wassum, K. M., & Izquierdo, A. (2015). The basolateral amygdala in reward learning and addiction. Neuroscience and Biobehavioral Reviews, 57, 271–283. https://doi.org/10.1016/j.neubiorev.2015.08.017
WHO. (2020). Dementia. World Health Organization.
Wilckens, K. A., Stillman, C. M., Waiwood, A. M., Kang, C., Leckie, R. L., Peven, J. C., . . . Erickson, K. I. (2021). Exercise interventions preserve hippocampal volume: A meta-analysis. Hippocampus, 31(3), 335–347. https://doi.org/10.1002/hipo.23292.
Yang, J., Pan, P., Song, W., Huang, R., Li, J., Chen, K., . . . Shang, H. (2012). Voxelwise meta-analysis of gray matter anomalies in Alzheimer's disease and mild cognitive impairment using anatomic likelihood estimation. Journal of the Neurological Sciences, 316(1), 21–29. https://doi.org/10.1016/j.jns.2012.02.010.
Yang, T., Shen, B. L., Wu, A. Q., Tang, X. L., Chen, W., Zhang, Z. Z., . . . Liu, X. Z. (2021). Abnormal Functional Connectivity of the Amygdala in Mild Cognitive Impairment Patients With Depression Symptoms Revealed by Resting-State fMRI. Frontiers in Psychiatry, 12. https://doi.org/10.3389/fpsyt.2021.533428.
Zeidman, P., Lutti, A., & Maguire, E. A. (2015). Investigating the functions of subregions within anterior hippocampus. Cortex, 73, 240–256. https://doi.org/10.1016/j.cortex.2015.09.002
Zhang, J. H., Liu, Y. F., Lan, K., Huang, X. X., He, Y. H., Yang, F. X., et al. (2021). Gray Matter Atrophy in Amnestic Mild Cognitive Impairment: A Voxel-Based Meta-Analysis. Frontiers in Aging Neuroscience, 13. https://doi.org/10.3389/fnagi.2021.627919
References for Papers Included in the ALE Meta-Analyses
Bai, F., Zhang, Z. J., Watson, D. R., Yu, H., Shi, Y. M., Yuan, Y. G., et al. (2009). Abnormal integrity of association fiber tracts in amnestic mild cognitive impairment. Journal of the Neurological Sciences, 278(1–2), 102–106. https://doi.org/10.1016/j.jns.2008.12.009
Bai, F., Zhang, Z. J., Yu, H., Shi, Y. M., Yuan, Y. G., Zhu, W. L., . . . Qian, Y. (2008). Default-mode network activity distinguishes amnestic type mild cognitive impairment from healthy aging: A combined structural and resting-state functional MRI study. Neuroscience Letters, 438(1), 111–115. https://doi.org/10.1016/j.neulet.2008.04.021.
Barbeau, E. J., Ranjeva, J. P., Didic, M., Confort-Gouny, S., Felician, O., Soulier, E., . . . Poncet, M. (2008). Profile of memory impairment and gray matter loss in amnestic mild cognitive impairment. Neuropsychologia, 46(4), 1009–1019. https://doi.org/10.1016/j.neuropsychologia.2007.11.019.
Bastin, C., Feyers, D., Jedidi, H., Bahri, M. A., Degueldre, C., Lemaire, C., et al. (2013). Episodic autobiographical memory in amnestic mild cognitive impairment: What are the neural correlates? Human Brain Mapping, 34(8), 1811–1825. https://doi.org/10.1002/hbm.22032
Bell-McGinty, S., Lopez, O. L., Meltzer, C. C., Scanlon, J. M., Whyte, E. M., Dekosky, S. T., & Becker, J. T. (2005). Differential cortical atrophy in subgroups of mild cognitive impairment. Archives of Neurology, 62(9), 1393–1397. https://doi.org/10.1001/archneur.62.9.1393
Benavides-Varela, S., Burgio, F., Weis, L., Mitolo, M., Palmer, K., Toffano, R., . . . Semenza, C. (2020). The role of limbic structures in financial abilities of mild cognitive impairment patients. Neuroimage Clin, 26, 102222. https://doi.org/10.1016/j.nicl.2020.102222.
Bharath, S., Joshi, H., John, J. P., Balachandar, R., Sadanand, S., Saini, J., . . . Varghese, M. (2017). A multimodal structural and functional Neuroimaging study of amnestic mild cognitive impairment. American Journal of Geriatric Psychiatry, 25(2), 158–169. https://doi.org/10.1016/j.jagp.2016.05.001.
Bonekamp, D., Yassa, M. A., Munro, C. A., Geckle, R. J., Yousem, D. M., Barker, P. B., . . . Horska, A. (2010). Gray matter in amnestic mild cognitive impairment: Voxel-based morphometry. Neuroreport, 21(4), 259–263. https://doi.org/10.1097/WNR.0b013e328335642a.
Bozzali, M., Filippi, M., Magnani, G., Cercignani, M., Franceschi, M., Schiatti, E., . . . Falini, A. (2006). The contribution of voxel-based morphometry in staging patients with mild cognitive impairment. Neurology, 67(3), 453–460. https://doi.org/10.1212/01.wnl.0000228243.56665.c2.
Brambati, S. M., Belleville, S., Kergoat, M. J., Chayer, C., Gauthier, S., & Joubert, S. (2009). Single- and multiple-domain amnestic mild cognitive impairment: Two sides of the same coin? Dementia and Geriatric Cognitive Disorders, 28(6), 541–549. https://doi.org/10.1159/000255240
Chen, B., Wang, S., Sun, W., Shang, X., Liu, H., Liu, G., et al. (2017). Functional and structural changes in gray matter of parkinson's disease patients with mild cognitive impairment. European Journal of Radiology, 93, 16–23. https://doi.org/10.1016/j.ejrad.2017.05.018
Chen, J., Yan, Y., Gu, L., Gao, L., & Zhang, Z. (2020). Electrophysiological processes on motor imagery mediate the association between increased gray matter volume and cognition in amnestic mild cognitive impairment. Brain Topography, 33(2), 255–266. https://doi.org/10.1007/s10548-019-00742-8
Chetelat, G., Desgranges, B., de la Sayette, V., Viader, F., Eustache, F., & Baron, J. C. (2002). Mapping gray matter loss with voxel-based morphometry in mild cognitive impairment. Neuroreport, 13(15), 1939-1943. Retrieved from <go to ISI>://WOS:000179479700022.
Clerx, L., Jacobs, H. I., Burgmans, S., Gronenschild, E. H., Uylings, H. B., Echávarri, C., . . . Aalten, P. (2013). Sensitivity of different MRI-techniques to assess gray matter atrophy patterns in Alzheimer's disease is region-specific. Current Alzheimer Research, 10(9), 940–951. https://doi.org/10.2174/15672050113109990158.
de Rover, M., Pironti, V. A., McCabe, J. A., Acosta-Cabronero, J., Arana, F. S., Morein-Zamir, S., . . . Sahakian, B. J. (2011). Hippocampal dysfunction in patients with mild cognitive impairment: A functional neuroimaging study of a visuospatial paired associates learning task. Neuropsychologia, 49(7), 2060–2070. https://doi.org/10.1016/j.neuropsychologia.2011.03.037.
Derflinger, S., Sorg, C., Gaser, C., Myers, N., Arsic, M., Kurz, A., et al. (2011). Grey-matter atrophy in Alzheimer's disease is asymmetric but not lateralized. Journal of Alzheimer's Disease, 25(2), 347–357. https://doi.org/10.3233/jad-2011-110041
Donzuso, G., Monastero, R., Cicero, C. E., Luca, A., Mostile, G., Giuliano, L., . . . Nicoletti, A. (2021). Neuroanatomical changes in early Parkinson's disease with mild cognitive impairment: A VBM study; the Parkinson's disease cognitive impairment study (PaCoS). Neurological Sciences, https://doi.org/10.1007/s10072-020-05034-9.
Duarte, A., Hayasaka, S., Du, A. T., Schuff, N., Jahng, G. H., Kramer, J., . . . Weiner, M. (2006). Volumetric correlates of memory and executive function in normal elderly, mild cognitive impairment and Alzheimer's disease. Neuroscience Letters, 406(1–2), 60–65. https://doi.org/10.1016/j.neulet.2006.07.029.
Ford, A. H., Almeida, O. P., Flicker, L., Garrido, G. J., Greenop, K. R., Foster, J. K., . . . Lautenschlager, N. T. (2014). Grey matter changes associated with deficit awareness in mild cognitive impairment: A voxel-based morphometry study. Journal of Alzheimer's Disease,, 42(4), 1251–1259. https://doi.org/10.3233/jad-132678.
Gao, Y., Nie, K., Huang, B., Mei, M., Guo, M., Xie, S., . . . Wang, L. (2017). Changes of brain structure in Parkinson's disease patients with mild cognitive impairment analyzed via VBM technology. Neuroscience Letters, 658, 121–132. https://doi.org/10.1016/j.neulet.2017.08.028.
Gili, T., Cercignani, M., Serra, L., Perri, R., Giove, F., Maraviglia, B., . . . Bozzali, M. (2011). Regional brain atrophy and functional disconnection across Alzheimer's disease evolution. Journal of Neurology, Neurosurgery, and Psychiatry, 82(1), 58–66. https://doi.org/10.1136/jnnp.2009.199935.
Grau-Olivares, M., Bartres-Faz, D., Arboix, A., Soliva, J. C., Rovira, M., Targa, C., & Junque, C. (2007). Mild cognitive impairment after lacunar infarction: Voxel-based morphometry and neuropsychological assessment. Cerebrovascular Diseases, 23(5–6), 353–361. https://doi.org/10.1159/000099134
Guedj, E., Barbeau, E. J., Didic, M., Felician, O., de Laforte, C., Ranjeva, J. P., . . . Ceccaldi, M. (2009). Effects of medial temporal lobe degeneration on brain perfusion in amnestic MCI of AD type: Deafferentation and functional compensation? European Journal of Nuclear Medicine and Molecular Imaging, 36(7), 1101–1112. https://doi.org/10.1007/s00259-009-1060-x.
Gupta, Y., Kim, J. I., Kim, B. C., & Kwon, G. R. (2020). Classification and graphical analysis of Alzheimer's disease and its prodromal stage using multimodal features from structural, diffusion, and functional Neuroimaging data and the APOE genotype. Frontiers in Aging Neuroscience, 12, 238. https://doi.org/10.3389/fnagi.2020.00238
Haller, S., Montandon, M. L., Rodriguez, C., Moser, D., Toma, S., Hofmeister, J., . . . Giannakopoulos, P. (2014). Acute caffeine administration effect on brain activation patterns in mild cognitive impairment. Journal of Alzheimer's Disease, 41(1), 101–112. https://doi.org/10.3233/jad-132360.
Hamalainen, A., Tervo, S., Grau-Olivares, M., Niskanen, E., Pennanen, C., Huuskonen, J., . . . Soininen, H. (2007). Voxel-based morphometry to detect brain atrophy in progressive mild cognitive impairment. Neuroimage, 37(4), 1122–1131. https://doi.org/10.1016/j.neuroimage.2007.06.016.
Han, S. H., Pyun, J. M., Yeo, S., Kang, D. W., Jeong, H. T., Kang, S. W., . . . Youn, Y. C. (2021). Differences between memory encoding and retrieval failure in mild cognitive impairment: Results from quantitative electroencephalography and magnetic resonance volumetry. Alzheimers Research & Therapy, 13(1). https://doi.org/10.1186/s13195-020-00739-7.
Han, Y., Lui, S., Kuang, W., Lang, Q., Zou, L., & Jia, J. (2012). Anatomical and functional deficits in patients with amnestic mild cognitive impairment. PLoS One, 7(2), e28664. https://doi.org/10.1371/journal.pone.0028664
Hong, Y. J., Yoon, B., Shim, Y. S., Ahn, K. J., Yang, D. W., & Lee, J. H. (2015). Gray and white matter degenerations in subjective memory impairment: Comparisons with Normal controls and mild cognitive impairment. Journal of Korean Medical Science, 30(11), 1652–1658. https://doi.org/10.3346/jkms.2015.30.11.1652
Jauhiainen, A. M., Kangasmaa, T., Rusanen, M., Niskanen, E., Tervo, S., Kivipelto, M., . . . Soininen, H. (2008). Differential hypometabolism patterns according to mild cognitive impairment subtypes. Dementia and Geriatric Cognitive Disorders, 26(6), 490–498. https://doi.org/10.1159/000167880.
Kim, G. W., Park, S. E., Park, K., & Jeong, G. W. (2021). White matter connectivity and gray matter volume changes following donepezil treatment in patients with mild cognitive impairment: A preliminary study using probabilistic Tractography. Frontiers in Aging Neuroscience, 12. https://doi.org/10.3389/fnagi.2020.604940.
Kim, H. G., Park, S., Rhee, H. Y., Lee, K. M., Ryu, C. W., Rhee, S. J., . . . Jahng, G. H. (2017). Quantitative susceptibility mapping to evaluate the early stage of Alzheimer's disease. Neuroimage Clin, 16, 429–438. https://doi.org/10.1016/j.nicl.2017.08.019.
Kunst, J., Marecek, R., Klobusiakova, P., Balazova, Z., Anderkova, L., Nemcova-Elfmarkova, N., & Rektorova, I. (2019). Patterns of Grey matter atrophy at different stages of Parkinson's and Alzheimer's diseases and relation to cognition. Brain Topography, 32(1), 142–160. https://doi.org/10.1007/s10548-018-0675-2
Lei, Y., Su, J., Guo, Q., Yang, H., Gu, Y., & Mao, Y. (2016). Regional gray matter atrophy in vascular mild cognitive impairment. Journal of Stroke and Cerebrovascular Diseases, 25(1), 95–101. https://doi.org/10.1016/j.jstrokecerebrovasdis.2015.08.041
Li, C., Zuo, Z. W., Liu, D. H., Jiang, R., Li, Y., Li, H. T., . . . Xiong, K. L. (2020). Type 2 diabetes mellitus may exacerbate gray matter atrophy in patients with early-onset mild cognitive impairment. Frontiers in Neuroscience, 14. https://doi.org/10.3389/fnins.2020.00856.
Li, M. Y., Meng, Y., Wang, M. Z., Yang, S., Wu, H., Zhao, B., & Wang, G. B. (2017). Cerebral gray matter volume reduction in subcortical vascular mild cognitive impairment patients and subcortical vascular dementia patients, and its relation with cognitive deficits. Brain and Behavior, 7(8). https://doi.org/10.1002/brb3.745
Liang, P. P., Wang, Z. Q., Yang, Y. H., Jia, X. Q., & Li, K. C. (2011). Functional disconnection and compensation in mild cognitive impairment: Evidence from DLPFC connectivity using resting-state fMRI. PLoS One, 6(7). https://doi.org/10.1371/journal.pone.0022153.
Meyer, P., Feldkamp, H., Hoppstadter, M., King, A. V., Frolich, L., Wessa, M., & Flor, H. (2013). Using voxel-based morphometry to examine the relationship between regional brain volumes and memory performance in amnestic mild cognitive impairment. Frontiers in Behavioral Neuroscience, 7. https://doi.org/10.3389/fnbeh.2013.00089.
Migo, E. M., Mitterschiffthaler, M., O'Daly, O., Dawson, G. R., Dourish, C. T., Craig, K. J., . . . Morris, R. G. (2015). Alterations in working memory networks in amnestic mild cognitive impairment. Neuropsychology, Development, and Cognition. Section B, Aging, Neuropsychology and Cognition, 22(1), 106–127. https://doi.org/10.1080/13825585.2014.894958.
Mitolo, M., Gardini, S., Fasano, F., Crisi, G., Pelosi, A., Pazzaglia, F., & Caffarra, P. (2013). Visuospatial memory and neuroimaging correlates in mild cognitive impairment. Journal of Alzheimer's Disease, 35(1), 75–90. https://doi.org/10.3233/jad-121288
Novellino, F., López, M. E., Vaccaro, M. G., Miguel, Y., Delgado, M. L., & Maestu, F. (2019). Association between Hippocampus, thalamus, and caudate in mild cognitive impairment APOEε4 carriers: A structural covariance MRI study. Frontiers in Neurology, 10, 1303. https://doi.org/10.3389/fneur.2019.01303
Pa, J., Boxer, A., Chao, L. L., Gazzaley, A., Freeman, K., Kramer, J., . . . Johnson, J. K. (2009). Clinical-neuroimaging characteristics of dysexecutive mild cognitive impairment. Annals of Neurology, 65(4), 414–423. https://doi.org/10.1002/ana.21591.
Pennanen, C., Testa, C., Laakso, M. P., Hallikainen, M., Helkala, E. L., Hanninen, T., . . . Soininen, H. (2005). A voxel based morphometry study on mild cognitive impairment. Journal of Neurology Neurosurgery and Psychiatry, 76(1), 11–14. https://doi.org/10.1136/jnnp.2004.035600.
Saykin, A. J., Wishart, H. A., Rabin, L. A., Santulli, R. B., Flashman, L. A., West, J. D., . . . Mamourian, A. C. (2006). Older adults with cognitive complaints show brain atrophy similar to that of amnestic MCI. Neurology, 67(5), 834–842. https://doi.org/10.1212/01.wnl.0000234032.77541.a2.
Schmidt-Wilcke, T., Poljansky, S., Hierlmeier, S., Hausner, J., & Ibach, B. (2009). Memory performance correlates with gray matter density in the ento−/perirhinal cortex and posterior hippocampus in patients with mild cognitive impairment and healthy controls - a voxel based morphometry study. Neuroimage, 47(4), 1914–1920. https://doi.org/10.1016/j.neuroimage.2009.04.092
Serra, L., Giulietti, G., Cercignani, M., Spanò, B., Torso, M., Castelli, D., et al. (2013). Mild cognitive impairment: Same identity for different entities. Journal of Alzheimer's Disease, 33(4), 1157–1165. https://doi.org/10.3233/jad-2012-121663
Sheelakumari, R., Kesavadas, C., Lekha, V. S., Justus, S., Sarma, P. S., & Menon, R. (2018). Structural correlates of mild cognitive impairment: A clinicovolumetric study. Neurology India, 66(2), 370–376. https://doi.org/10.4103/0028-3886.227298
Shiino, A., Watanabe, T., Maeda, K., Kotani, E., Akiguchi, I., & Matsuda, M. (2006). Four subgroups of Alzheimer's disease based on patterns of atrophy using VBM and a unique pattern for early onset disease. Neuroimage, 33(1), 17–26. https://doi.org/10.1016/j.neuroimage.2006.06.010
Son, J. H., Han, D. H., Min, K. J., & Kee, B. S. (2013). Correlation between gray matter volume in the temporal lobe and depressive symptoms in patients with Alzheimer's disease. Neuroscience Letters, 548, 15–20. https://doi.org/10.1016/j.neulet.2013.05.021
Sun, P., Lou, W. T., Liu, J. H., Shi, L., Li, K. C., Wang, D. F., et al. (2019). Mapping the patterns of cortical thickness in single- and multiple-domain amnestic mild cognitive impairment patients: A pilot study. Aging-Us, 11(22), 10000–10015. https://doi.org/10.18632/aging.102362
Suo, X., Lei, D., Cheng, L., Li, N., Zuo, P., Wang, D. J. J., . . . Gong, Q. (2019). Multidelay multiparametric arterial spin labeling perfusion MRI and mild cognitive impairment in early stage Parkinson's disease. Human Brain Mapping, 40(4), 1317–1327. https://doi.org/10.1002/hbm.24451.
Threlkeld, Z. D., Jicha, G. A., Smith, C. D., & Gold, B. T. (2011). Task deactivation reductions and atrophy within parietal default mode regions are overlapping but only weakly correlated in mild cognitive impairment. Journal of Alzheimers Disease, 27(2), 415–427. https://doi.org/10.3233/jad-2011-110206
Toniolo, S., Serra, L., Olivito, G., Marra, C., Bozzali, M., & Cercignani, M. (2018). Patterns of cerebellar gray matter atrophy across Alzheimer's disease progression. Frontiers in Cellular Neuroscience, 12, 430. https://doi.org/10.3389/fncel.2018.00430
Trivedi, M. A., Wichmann, A. K., Torgerson, B. M., Ward, M. A., Schmitz, T. W., Ries, M. L., . . . Johnson, S. C. (2006). Structural MRI discriminates individuals with mild cognitive impairment from age-matched controls: A combined neuropsychological and voxel based morphometry study. Alzheimers Dement, 2(4), 296–302. https://doi.org/10.1016/j.jalz.2006.06.001.
Venneri, A., Gorgoglione, G., Toraci, C., Nocetti, L., Panzetti, P., & Nichelli, P. (2011). Combining neuropsychological and structural neuroimaging indicators of conversion to Alzheimer's disease in amnestic mild cognitive impairment. Current Alzheimer Research, 8(7), 789–797. https://doi.org/10.2174/156720511797633160
Wang, P. N., Chou, K. H., Lirng, J. F., Lin, K. N., Chen, W. T., & Lin, C. P. (2012). Multiple diffusivities define white matter degeneration in amnestic mild cognitive impairment and Alzheimer's disease. Journal of Alzheimers Disease, 30(2), 423–437. https://doi.org/10.3233/jad-2012-111304
Xie, C., Bai, F., Yuan, B., Yu, H., Shi, Y., Yuan, Y., . . . Zhang, Z. J. (2015a). Joint effects of gray matter atrophy and altered functional connectivity on cognitive deficits in amnestic mild cognitive impairment patients. Psychological Medicine, 45(9), 1799–1810. https://doi.org/10.1017/s0033291714002876.
Xie, C. M., Li, W. J., Chen, G., Ward, B. D., Franczak, M. B., Jones, J. L., . . . Goveas, J. S. (2012). The co-existence of geriatric depression and amnestic mild cognitive impairment detrimentally affect gray matter volumes: Voxel-based morphometry study. Behavioural Brain Research, 235(2), 244–250. https://doi.org/10.1016/j.bbr.2012.08.007.
Xie, Y., Cui, Z., Zhang, Z., Sun, Y., Sheng, C., Li, K., . . . Jia, J. (2015b). Identification of amnestic mild cognitive impairment using multi-modal brain features: A combined structural MRI and diffusion tensor imaging study. Journal of Alzheimer's Disease, 47(2), 509–522. https://doi.org/10.3233/jad-150184.
Yao, Z., Hu, B., Liang, C., Zhao, L., & Jackson, M. (2012). A longitudinal study of atrophy in amnestic mild cognitive impairment and normal aging revealed by cortical thickness. PLoS One, 7(11), e48973. https://doi.org/10.1371/journal.pone.0048973
Yi, D., Choe, Y. M., Byun, M. S., Sohn, B. K., Seo, E. H., Han, J., . . . Lee, D. Y. (2015). Differences in functional brain connectivity alterations associated with cerebral amyloid deposition in amnestic mild cognitive impairment. Frontiers in Aging Neuroscience, 7. https://doi.org/10.3389/fnagi.2015.00015.
Yi, L., Wang, J., Jia, L., Zhao, Z., Lu, J., Li, K., . . . Han, Y. (2012). Structural and functional changes in subcortical vascular mild cognitive impairment: A combined voxel-based morphometry and resting-state fMRI study. PLoS One, 7(9), e44758. https://doi.org/10.1371/journal.pone.0044758.
Yu, J., Li, R., Jiang, Y., Broster, L. S., & Li, J. (2016). Altered brain activities associated with neural repetition effects in mild cognitive impairment patients. Journal of Alzheimer's Disease, 53(2), 693–704. https://doi.org/10.3233/jad-160086
Zhang, H. B., Sachdev, P. S., Wen, W., Kochan, N. A., Crawford, J. D., Brodaty, H., . . . Trollor, J. N. (2012). Gray matter atrophy patterns of mild cognitive impairment subtypes. Journal of the Neurological Sciences, 315(1–2), 26–32. https://doi.org/10.1016/j.jns.2011.12.011.
Zhang, J., Zhang, Y. T., Hu, W. D., Li, L., Liu, G. Y., & Bai, Y. P. (2015). Gray matter atrophy in patients with Parkinson's disease and those with mild cognitive impairment: A voxel-based morphometry study. International journal of clinical and experimental medicine, 8(9), 15383-15392. Retrieved from <go to ISI>://WOS:000367911200040.
Zhang, T. H., & Davatzikos, C. (2013). Optimally-discriminative voxel-based morphometry significantly increases the ability to detect group differences in schizophrenia, mild cognitive impairment, and Alzheimer's disease. Neuroimage, 79, 94–110. https://doi.org/10.1016/j.neuroimage.2013.04.063
Zhao, Z. L., Fan, F. M., Lu, J., Li, H. J., Jia, L. F., Han, Y., & Li, K. C. (2015). Changes of gray matter volume and amplitude of low-frequency oscillations in amnestic MCI: An integrative multi-modal MRI study. Acta Radiologica, 56(5), 614–621. https://doi.org/10.1177/0284185114533329
Code availability
Not applicable.
Author information
Authors and Affiliations
Contributions
Concept and design, interpretation of results, manuscript revision, approval of final version (PJR and HR); data collection, statistical analysis (PJR),
Corresponding author
Ethics declarations
Ethics approval
Exempt from review.
Consent to participate
Not relevant.
Consent for publication
(include appropriate statements)
Conflicts of interest/competing interests
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Raine, P.J., Rao, H. Volume, density, and thickness brain abnormalities in mild cognitive impairment: an ALE meta-analysis controlling for age and education.. Brain Imaging and Behavior 16, 2335–2352 (2022). https://doi.org/10.1007/s11682-022-00659-0
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11682-022-00659-0