Abstract
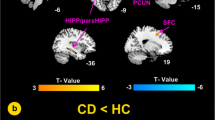
Multiple reports for brain functional and structural alterations in patients with Crohn’s disease (CD) were published. The current study aimed to meta-analyze the existing neuroimaging data and hence produce a brain map revealing areas with functional and structural differences between patients with CD and healthy controls. Original studies published until 2019 were identified from Scopus, Web of Science and PubMed databases, and included into the analysis if they reported relevant results from task-related or resting state functional magnetic resonance imaging (fMRI or rsfMRI) or voxel-based morphometry (VBM), in the form of standardized brain coordinates based on whole-brain analysis. The brain coordinates and sample size of significant results were extracted from eligible studies to be meta-analyzed with the activation likelihood estimation method using the GingerALE software. Sixteen original studies comprised of a total of 865 participants fulfilled the inclusion criteria. Compared to healthy controls, patients with CD had reduced resting state brain connectivity in the paracentral lobule and cingulate gyrus as well as reduced grey matter volume in the medial frontal gyrus. No significant results were found vice versa. These neural correlates allow a better understanding on the effects of CD on the pain expectation, emotion, and quality of life of patients and potentially serve as useful biomarkers for evaluating treatment efficacy.


Similar content being viewed by others
Abbreviations
- ALE:
-
Activation likelihood estimation
- CD:
-
Crohn’s disease
- fMRI:
-
Functional magnetic resonance imaging
- rsfMRI:
-
Resting state functional magnetic resonance imaging
- TNF:
-
Tumor necrosis factor
- UC:
-
Ulcerative colitis
- VBM:
-
Voxel-based morphometry
References
Agostini, A., Ballotta, D., Righi, S., Moretti, M., Bertani, A., Scarcelli, A.,.. . Campieri, M. (2017). Stress and brain functional changes in patients with Crohn’s disease: A functional magnetic resonance imaging study. Neurogastroenterology & Motility, 29(10), 1–10.
Agostini, A., Benuzzi, F., Filippini, N., Bertani, A., Scarcelli, A., Farinelli, V.,.. . Gionchetti, P. (2013a). New insights into the brain involvement in patients with Crohn’s disease: a voxel-based morphometry study. Neurogastroenterology & Motility, 25(2), 147–182.
Agostini, A., Campieri, M., Bertani, A., Scarcelli, A., Ballotta, D., Calabrese, C.,.. . Benuzzi, F. (2015). Absence of change in the gray matter volume of patients with ulcerative colitis in remission: a voxel based morphometry study. Biopsychosocial Medicine, 9(1), 1.
Agostini, A., Filippini, N., Benuzzi, F., Bertani, A., Scarcelli, A., Leoni, C.,.. . Calabrese, C. (2013b). Functional magnetic resonance imaging study reveals differences in the habituation to psychological stress in patients with Crohn’s disease versus healthy controls. Journal of Behavioral Medicine , 36(5), 477–487.
Agostini, A., Filippini, N., Cevolani, D., Agati, R., Leoni, C., Tambasco, R.,.. . Ercolani, M. (2011). Brain functional changes in patients with ulcerative colitis: a functional magnetic resonance imaging study on emotional processing. Inflammatory Bowel Diseases, 17(8), 1769–1777.
Appenzeller, S., Bonilha, L., Rio, P. A., Li, L. M., Costallat, L. T. L., & Cendes, F. (2007). Longitudinal analysis of gray and white matter loss in patients with systemic lupus erythematosus. Neuroimage, 34(2), 694–701.
Bao, C., Liu, P., Liu, H., Jin, X., Calhoun, V. D., Wu, L.,.. . Ma, L. (2016a). Different brain responses to electro-acupuncture and moxibustion treatment in patients with Crohn’s disease. Scientific Reports, 6, 36636.
Bao, C., Liu, P., Liu, H., Jin, X., Shi, Y., Wu, L., & Calhoun, V. D. (2018). Difference in regional neural fluctuations and functional connectivity in Crohn’s disease: a resting-state functional MRI study. Brain Imaging and Behavior, 12(6), 1795–1803.
Bao, C., Liu, P., Liu, H.-R., Wu, L.-Y., Jin, X.-M., Wang, S.-Y.,.. . Ma, L.-L. (2016b). Differences in regional homogeneity between patients with Crohn’s disease with and without abdominal pain revealed by resting-state functional magnetic resonance imaging. Pain, 157(5), 1037–1044.
Bao, C., Liu, P., Liu, H. R., Wu, L. Y., Shi, Y., Chen, W. F.,.. . Jin, X. M. (2015). Alterations in Brain Grey Matter Structures in Patients With Crohn’s Disease and Their Correlation With Psychological Distress. Journal of Crohn’s and Colitis, 9(7), 532–540.
Bao, C., Liu, P., Shi, Y., Wu, L., Jin, X., Zeng, X.,.. . Wu, H. (2017). Differences in brain gray matter volume in patients with Crohn’s disease with and without abdominal pain. Oncotarget, 8(55), 93624.
Buntinx, M., Moreels, M., Vandenabeele, F., Lambrichts, I., Raus, J., Steels, P., & Ameloot, M. (2004). Cytokine-induced cell death in human oligodendroglial cell lines: I. Synergistic effects of IFN‐γ and TNF‐α on apoptosis. Journal of Neuroscience Research, 76(6), 834–845.
Canavan, C., Abrams, K., & Mayberry, J. (2006). Meta-analysis: colorectal and small bowel cancer risk in patients with Crohn’s disease. Alimentary Pharmacology and Therapeutics, 23(8), 1097–1104.
Cosnes, J., Gower–Rousseau, C., Seksik, P., & Cortot, A. (2011). Epidemiology and natural history of inflammatory bowel diseases. Gastroenterology, 140(6), 1785–1794.e1784.
Eickhoff, S. B., Bzdok, D., Laird, A. R., Kurth, F., & Fox, P. T. (2012). Activation likelihood estimation meta-analysis revisited. Neuroimage, 59(3), 2349–2361.
Eickhoff, S. B., Laird, A. R., Grefkes, C., Wang, L. E., Zilles, K., & Fox, P. T. (2009). Coordinate-based ALE meta-analysis of neuroimaging data: a random-effects approach based on empirical estimates of spatial uncertainty. Human Brain Mapping, 30(9), 2907–2026.
Fan, Y., Bao, C., Wei, Y., Wu, J., Zhao, Y., Zeng, X., & Liu, P. (2019). Altered functional connectivity of the amygdala in Crohn’s disease. Brain Imaging and Behavior. https://doi.org/10.1007/s11682-11019-00159-11688.
Ford, A. C., & Peyrin-Biroulet, L. (2013). Opportunistic infections with anti-tumor necrosis factor-α therapy in inflammatory bowel disease: meta-analysis of randomized controlled trials. The American Journal of Gastroenterology, 108(8), 1268–1276.
Gray, M. A., Chao, C., Staudacher, H. M., Kolosky, N. A., Talley, N. J., & Holtmann, G. (2018). Anti-TNFα therapy in IBD alters brain activity reflecting visceral sensory function and cognitive-affective biases. PloS One, 13(3), e0193542.
Holmes, C. J., Hoge, R., Collins, L., Woods, R., Toga, A. W., & Evans, A. C. (1998). Enhancement of MR images using registration for signal averaging. Journal of Computer Assisted Tomography, 22(2), 324–333.
Hou, J. K., El-Serag, H., & Thirumurthi, S. (2009). Distribution and manifestations of inflammatory bowel disease in Asians, Hispanics, and African Americans: a systematic review. American Journal of Gastroenterology, 104(8), 2100–2109.
Hsieh, J. -C., Stone-Elander, S., & Ingvar, M. (1999). Anticipatory coping of pain expressed in the human anterior cingulate cortex: a positron emission tomography study. Neuroscience Letters, 262(1), 61–64.
Kaplan, G. G., & Ng, S. C. (2017). Understanding and preventing the global increase of inflammatory bowel disease. Gastroenterology, 152(2), 313–321.e312.
Kong, J., Loggia, M. L., Zyloney, C., Tu, P., LaViolette, P., & Gollub, R. L. (2010). Exploring the brain in pain: activations, deactivations and their relation. Pain, 148(2), 257–267.
Lancaster, J. L., Tordesillas-Gutiérrez, D., Martinez, M., Salinas, F., Evans, A., Zilles, K., & Fox, P. T. (2007). Bias between MNI and Talairach coordinates analyzed using the ICBM-152 brain template. Human Brain Mapping, 28(11), 1194–1205.
Liu, P., Li, R., Bao, C., Wei, Y., Fan, Y., Liu, Y., & Qin, W. (2018). Altered topological patterns of brain functional networks in Crohn’s disease. Brain Imaging and Behavior, 12(5), 1466–1478.
Loftus Jr, E. V., Guérin, A., Andrew, P. Y., Wu, E. Q., Yang, M., Chao, J., & Mulani, P. M. (2011). Increased risks of developing anxiety and depression in young patients with Crohn’s disease. American Journal of Gastroenterology, 106(9), 1670–1677.
Loftus Jr, E. V., Silverstein, M. D., Sandborn, W. J., Tremaine, W. J., Harmsen, W. S., & Zinsmeister, A. R. (1998). Crohn’s disease in Olmsted County, Minnesota, 1940–1993: incidence, prevalence, and survival. Gastroenterology, 114(6), 1161–1168.
Mallio, C. A., Piervincenzi, C., Gianolio, E., Cirimele, V., Papparella, L. G., Marano, M.,.. . Parizel, P. M. (2019). Absence of dentate nucleus resting-state functional connectivity changes in nonneurological patients with gadolinium‐related hyperintensity on T1‐weighted images. Journal of Magnetic Resonance Imaging, 50(2), 445–455.
May, A. (2008). Chronic pain may change the structure of the brain. Pain, 137(1), 7–15.
Mizrahi, M. C., Reicher-Atir, R., Levy, S., Haramati, S., Wengrower, D., Israeli, E., & Goldin, E. (2012). Effects of guided imagery with relaxation training on anxiety and quality of life among patients with inflammatory bowel disease. Psychology and Health, 27(12), 1463–1479.
Müller, V. I., Cieslik, E. C., Laird, A. R., Fox, P. T., Radua, J., Mataix-Cols, D.,.. . Turkeltaub, P. E. (2018). Ten simple rules for neuroimaging meta-analysis. Neuroscience & Biobehavioral Reviews, 84, 151–161.
Murphy, B. P., Inder, T. E., Huppi, P. S., Warfield, S., Zientara, G. P., Kikinis, R.,.. . Volpe, J. J. (2001). Impaired cerebral cortical gray matter growth after treatment with dexamethasone for neonatal chronic lung disease. Pediatrics, 107(2), 217–221.
Nahon, S., Lahmek, P., Durance, C., Olympie, A., Lesgourgues, B., Colombel, J. -F., & Gendre, J. -P. (2012). Risk factors of anxiety and depression in inflammatory bowel disease. Inflammatory Bowel Diseases, 18(11), 2086–2091.
Nair, V. A., Beniwal-Patel, P., Mbah, I., Young, B. M., Prabhakaran, V., & Saha, S. (2016). Structural imaging changes and behavioral correlates in patients with Crohn’s Disease in remission. Frontiers in Human Neuroscience, 10, 460.
Nair, V. A., Dodd, K., Rajan, S., Santhanubosu, A., Beniwal-Patel, P., Saha, S., & Prabhakaran, V. (2019). A Verbal Fluency Task‐Based Brain Activation fMRI Study in Patients with Crohn’s Disease in Remission. Journal of Neuroimaging, 29(5).
Ng, S. C., Shi, H. Y., Hamidi, N., Underwood, F. E., Tang, W., Benchimol, E. I.,.. . Chan, F. K. (2017). Worldwide incidence and prevalence of inflammatory bowel disease in the 21st century: a systematic review of population-based studies. Lancet, 390(10114), 2769–2778.
Ng, W. K., Wong, S. H., & Ng, S. C. (2016). Changing epidemiological trends of inflammatory bowel disease in Asia. Intestinal Research, 14(2), 111–119.
Peyrin–Biroulet, L., Deltenre, P., De Suray, N., Branche, J., Sandborn, W. J., & Colombel, J. F. (2008). Efficacy and safety of tumor necrosis factor antagonists in Crohn’s disease: meta-analysis of placebo-controlled trials. Clinical Gastroenterology and Hepatology, 6(6), 644–653.
Porro, C. A., Baraldi, P., Pagnoni, G., Serafini, M., Facchin, P., Maieron, M., & Nichelli, P. (2002). Does anticipation of pain affect cortical nociceptive systems? Journal of Neuroscience, 22(8), 3206–3214.
Research Imaging Institute. (2018). GingerALE Version 2.3.6. Retrieved from http://www.brainmap.org/ale/.
Research Imaging Institute, & UTHSCSA. (2018). Mango for the Desktop. Retrieved from http://rii.uthscsa.edu/mango/mango.html.
Rubio, A., Pellissier, S., Van Oudenhove, L., Ly, H. G., Dupont, P., Tack, J.,.. . Bonaz, B. (2016). Brain responses to uncertainty about upcoming rectal discomfort in quiescent Crohn’s disease–a fMRI study. Neurogastroenterology and Motility, 28(9), 1419–1432.
Schmid, J., Langhorst, J., Gaß, F., Theysohn, N., Benson, S., Engler, H.,.. . Elsenbruch, S. (2015). Placebo analgesia in patients with functional and organic abdominal pain: a fMRI study in IBS, UC and healthy volunteers. Gut, 64(3), 418–427.
Seminowicz, D. A., Labus, J. S., Bueller, J. A., Tillisch, K., Naliboff, B. D., Bushnell, M. C., & Mayer, E. A. (2010). Regional gray matter density changes in brains of patients with irritable bowel syndrome. Gastroenterology, 139(1), 48–57.e42.
Solberg, I. C., Vatn, M. H., Høie, O., Stray, N., Sauar, J., & Jahnsen, J... . IBSEN Study Group. (2007). Clinical course in Crohn’s disease: results of a Norwegian population-based ten-year follow-up study. Clinical Gastroenterology and Hepatology, 5(12), 1430–1438.
Stacey, D., Redlich, R., Büschel, A., Opel, N., Grotegerd, D., Zaremba, D.,.. . Förster, K. (2017). TNF receptors 1 and 2 exert distinct region-specific effects on striatal and hippocampal grey matter volumes (VBM) in healthy adults. Genes, Brain and Behavior, 16(3), 352–360.
Sundermann, B., Olde lütke Beverborg, M., & Pfleiderer, B. (2014). Toward literature-based feature selection for diagnostic classification: a meta-analysis of resting-state fMRI in depression. Frontiers in Human Neuroscience, 8, 692.
Tan, L. L., Pelzer, P., Heinl, C., Tang, W., Gangadharan, V., Flor, H., & Kuner, R. (2017). A pathway from midcingulate cortex to posterior insula gates nociceptive hypersensitivity. Nature Neuroscience, 20(11), 1591–1601.
Thomann, A. K., Griebe, M., Thomann, P. A., Hirjak, D., Ebert, M. P., Szabo, K., & Wolf, R. C. (2017). Intrinsic neural network dysfunction in quiescent Crohn’s Disease. Scientific Reports, 7(1), 11579.
Thomann, A. K., Thomann, P. A., Wolf, R. C., Hirjak, D., Schmahl, C., Ebert, M. P., & Griebe, M. (2016). Altered markers of brain development in Crohn’s Disease with extraintestinal manifestations–a pilot study. PloS One, 11(9), e0163202.
Tillisch, K., Mayer, E. A., & Labus, J. S. (2011). Quantitative meta-analysis identifies brain regions activated during rectal distension in irritable bowel syndrome. Gastroenterology, 140(1), 91–100.
Torres, J., Mehandru, S., Colombel, J.-F., & Peyrin-Biroulet, L. (2017). Crohn’s disease. Lancet, 389(10080), 1741–1755.
van Tol, M. -J., van der Wee, N. J., van den Heuvel, O. A., Nielen, M. M., Demenescu, L. R., Aleman, A., & Veltman, D. J. (2010). Regional brain volume in depression and anxiety disorders. Archives of General Psychiatry, 67(10), 1002–1011.
Vogt, B. (2013). Inflammatory bowel disease: perspectives from cingulate cortex in the first brain. Neurogastroenterology & Motility, 25(2), 93–98.
Yeung, A. W. K., Wong, N. S. M., Lau, H., & Eickhoff, S. B. (2019). Human brain responses to gustatory and food stimuli: a meta-evaluation of neuroimaging meta-analyses. Neuroimage, 202, 116111.
Author information
Authors and Affiliations
Contributions
AY is responsible for all parts of the study.
Corresponding author
Ethics declarations
This study did not use original human or animal data.
Conflict of interest
The authors declared no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yeung, A.W.K. Structural and functional changes in the brain of patients with Crohn’s disease: an activation likelihood estimation meta-analysis. Brain Imaging and Behavior 15, 807–818 (2021). https://doi.org/10.1007/s11682-020-00291-w
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11682-020-00291-w