Abstract
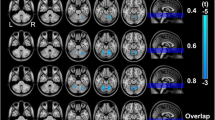
Patients with Crohn’s disease (CD) are shown to have abnormal changes in brain structures. This study aimed to further investigate whether these patients have abnormal brain activities and network connectivity. Sixty patients with CD and 40 healthy controls (HCs) underwent resting-state functional magnetic resonance imaging (fMRI) scans. Amplitude of low-frequency fluctuation (ALFF) and seed-based functional connectivity (FC) were used to assess differences in spontaneous regional brain activity and functional connectivity. Compared to the HCs, patients with CD showed significantly higher ALFF values in hippocampus and parahippocampus (HIPP/paraHIPP), anterior cingulate cortex, insula, superior frontal cortex and precuneus. The ALFF values were significantly lower in secondary somatosensory cortex (S2), precentral gyrus, and medial prefrontal cortex. Functional connectivities between left HIPP and left inferior temporal cortex, and right middle cingulate cortex, HIPP, and fusiform area were significantly lower. The functional connectivities between right HIPP and right inferior orbitofrontal cortex and left HIPP were also significantly lower. Patients with CD showed higher or lower spontaneous activity in multiple brain regions. Altered activities in these brain regions may collectively reflect abnormal function and regulation of visceral pain and sensation, external environmental monitoring, and cognitive processing in these patients. Lower functional connectivity of the hippocampus-limbic system was observed in these patients. These findings may provide more information to elucidate the neurobiological mechanisms of the disease.


Similar content being viewed by others
References
Agostini, A., Benuzzi, F., Filippini, N., Bertani, A., Scarcelli, A., Farinelli, V., et al. (2013). New insights into the brain involvement in patients with Crohn’s disease: a voxel-based morphometry study. Neurogastroenterology & Motility, 25(2), 147-e82.
Al, O. Y., & Aziz, Q. (2014). The brain-gut axis in health and disease. Advances in Experimental Medicine & Biology, 817, 135–153.
Bao, C. H., Liu, P., Liu, H. R., Jin, X. M., Calhoun, V. D., Wu, L. Y., et al. (2016a). Different brain responses to electro-acupuncture and moxibustion treatment in patients with Crohn’s disease. Scientific Reports, 18(6), 36636.
Bao, C. H., Liu, P., Liu, H. R., Wu, L. Y., Jin, X. M., Wang., S. Y., et al. (2016b). Differences in regional homogeneity between patients with Crohn’s disease with and without abdominal pain revealed by resting-state functional magnetic resonance imaging. Pain, 157(5), 1037–1044.
Bao, C. H., Liu, P., Liu, H. R., Wu, L. Y., Shi, Y., Chen, W. F., et al. (2015). Alterations in brain grey matter structures in patients with Crohn’s disease and their correlation with psychological distress. Journal of Crohn S & Colitis, 9(7), 532–540.
Best, W. R., Becktel, J. M., & Singleton, J. W. (1979). Rederived values of the eight coefficients of the Crohn’s Disease Activity Index (CDAI). Gastroenterology, 77(4 Pt 2), 843–846.
Blakemore, S. J. (2008). The social brain in adolescence. Nature Reviews Neuroscience, 9(4), 267–277.
Bonaz, B. L., & Bernstein, C. N. (2013). Brain-gut interactions in inflammatory bowel disease. Gastroenterology, 144(1), 36–49.
Buckner, R. L., Andrews-Hanna, J. R., & Schacter, D. L. (2008). The brain’s default network: anatomy, function, and relevance to disease. Annals of the New York Academy of Sciences, 1124(1), 1–38.
Cavanna, A. E., & Trimble, M. R. (2006). The precuneus: a review of its functional anatomy and behavioural correlates. Brain, 129(Pt3), 564–583.
Chao-Gan, Y., & Yu-Feng, Z. (2010). DPARSF: a MATLAB toolbox for “pipeline” data analysis of resting-state fMRI. Frontiers in Systems Neuroscience, 14(4), 13.
Drevets, W. C., Price, J. L., & Furey, M. L. (2008). Brain structural and functional abnormalities in mood disorders: implications for neurocircuitry models of depression. Brain Structure and Function, 213(1–2), 93–118.
Fair, D. A., Cohen, A. L., Dosenbach, N. U. F., Church, J. A., Miezin, F. M., Barch, D. M., et al. (2008). The maturing architecture of the brain’s default network. Proceedings of the National Academy of Sciences of the United States of America, 105(10), 4028–4032.
Fox, M. D., & Raichle, M. E. (2007). Spontaneous fluctuations in brain activity observed with functional magnetic resonance imaging. Nature Reviews Neuroscience, 8(9), 700–711.
Heydarpour, P., Rahimian, R., Fakhfouri, G., Khoshkish, S., Fakhraei, N., Salehi-Sadaghiani, M., et al. (2016). Behavioral despair associated with a mouse model of Crohn’s disease: Role of nitric oxide pathway. Progress in Neuro-Psychopharmacology & Biological Psychiatry, 4(64), 131–141.
Irvine, E. J., Feagan, B., Rochon, J., Archambault, A., Fedorak, R. N., Groll, A., et al. (1994). Quality of life: a valid and reliable measure of therapeutic efficacy in the treatment of inflammatory bowel disease. Canadian Crohn’s relapse prevention trial study group. Gastroenterology, 106(2), 287–296.
Jones, M. P., Dilley, J. B., Drossman, D., & Crowell, M. D. (2006). Brain-gut connections in functional GI disorders: anatomic and physiologic relationships. Neurogastroenterology & Motility, 18(2), 91–103.
Lathe, R. (2001). Hormones and the hippocampus. Journal of Endocrinology, 169(2), 205.
Li, F., He, N., Li, Y., Chen, L., Huang, X., Lui, S., et al. (2014). Intrinsic brain abnormalities in attention deficit hyperactivity disorder: a resting-state functional MR imaging study. Radiology, 272(2), 514–523.
Li, F., Lui, S., Yao, L., Hu, J., Lv, P., Huang, X., et al. (2016). Longitudinal changes in resting-state cerebral activity in patients with first-episode schizophrenia: a 1-year follow-up functional MR imaging study. Radiology, 279(3), 867–875.
Ma, X., Li, S., Tian, J., Jiang, G., Wen, H., Wang, T., et al. (2015). Altered brain spontaneous activity and connectivity network in irritable bowel syndrome patients: a resting-state fMRI study. Clinical Neurophysiology, 126(6), 1190–1197.
Mantini, D., & Vanduffel, W. (2013). Emerging roles of the brain’s default network. Neuroscientist A Review Journal Bringing Neurobiology Neurology & Psychiatry, 19(1), 76–87.
Margulies, D. S., Vincent, J. L., Kelly, C., Lohmann, G., Uddin, L. Q., Biswal, B. B., et al. (2009). Precuneus shares intrinsic functional architecture in humans and monkeys. Proceedings of the National Academy of Sciences of the United States of America, 106(47), 20069–20074.
Mayer, E. A., Naliboff, B. D., & Craig, A. D. B. (2006). Neuroimaging of the brain-gut axis: from basic understanding to treatment of functional GI disorders. Gastroenterology, 131(6), 1925–1942.
Mikdashi, J. A. (2016). Altered functional neuronal activity in neuropsychiatric lupus: a systematic review of the fMRI investigations. Seminars in Arthritis and Rheumatism, 45(4), 455–462.
Ng, S. C., Tang, W., Ching, J. Y., Wong, M., Chow, C., Hui, M., A. J. et al (2013). Incidence and phenotype of inflammatory bowel disease based on results from the Asia-Pacific Crohn’s and Colitis epidemiology study. Gastroenterology, 145(1), 158–165.e2.
Oldfield, R. C. (1971). The assessment and analysis of handedness: the Edinburgh inventory. Neuropsychologia, 9(1), 97–113.
Riazi, K., Galic, M. A., Kentner, A. C., Reid, A. Y., Sharkey, K. A., & Pittman, Q. J. (2015). Microglia-dependent alteration of glutamatergic synaptic transmission and plasticity in the hippocampus during peripheral inflammation. Journal of Neuroscience the Official Journal of the Society for Neuroscience, 35(12), 4942–4952.
Riazi, K., Galic, M. A., Kuzmiski, J. B., Ho, W., Sharkey, K. A., & Pittman, Q. J. (2008). Microglial activation and TNFalpha production mediate altered CNS excitability following peripheral inflammation. Proceedings of the National Academy of Sciences of the United States of America, 105(44), 17151–17156.
Song, X. W., Dong, Z. Y., Long, X. Y., Li, S. F., Zuo, X. N., Zhu, C. Z., et al. (2011). REST: a toolkit for resting-state functional magnetic resonance imaging data processing. Plos One, 6(9), e25031.
Torres, J., Mehandru, S., Colombel, J. F., & Peyrin-Biroulet, L. (2016). Crohn’s disease. Lancet, 67(27), 822–824.
Van, O. L., Coen, S. J., & Aziz, Q. (2007). Functional brain imaging of gastrointestinal sensation in health and disease. World Journal of Gastroenterology, 13(25), 3438–3445.
Van Hees, S., Mcmahon, K., Angwin, A., De Zubicaray, G., Read, S., & Copland, D. A. (2014). A functional MRI study of the relationship between naming treatment outcomes and resting state functional connectivity in post-stroke aphasia. Human Brain Mapping, 35(8), 3919–3931.
Vermeulen, W., De Man, J. G., Pelckmans, P. A., & De Winter, B. Y. (2014). Neuroanatomy of lower gastrointestinal pain disorders. World Journal of Gastroenterology, 20(4), 1005–1020.
Wei, S. Y., Chao, H. T., Tu, C. H., et al. (2016). Changes in functional connectivity of pain modulatory systems in women with primary dysmenorrhea. Pain, 157(1),92–102.
Wiech, K., Seymour, B., Kalisch, R., Stephan, K. E., Koltzenburg, M., Driver, J., et al. (2005). Modulation of pain processing in hyperalgesia by cognitive demand. Neuroimage, 27(1), 59–69.
Zang, Y. F., He, Y., Zhu, C. Z., Cao, Q. J., Sui, M. Q., Liang, M., et al. (2007). Altered baseline brain activity in children with ADHD revealed by resting-state functional MRI. Brain & Development, 29(2), 83–91.
Zhang, X., Zhu, X., Wang, X., Zhu, X., Zhong, M., Yi, J., et al. (2014). First-episode medication-naive major depressive disorder is associated with altered resting brain function in the affective network. Plos One, 9(1), e85241.
Zhou, G., Liu, P., Wang, J., Wen, H., Zhu, M., Zhao, R., et al. (2013). Fractional amplitude of low-frequency fluctuation changes in functional dyspepsia: A resting-state fMRI study. Magnetic Resonance Imaging, 31(6), 996–1000.
Zigmond, A. S., & Snaith, R. P. (1983). The hospital anxiety and depression scale. Acta Psychiatrica Scandinavica, 67(6), 361–370.
Zonis, S., Pechnick, R. N., Ljubimov, V. A., Mahgerefteh, M., Wawrowsky, K., Michelsen, K. S., et al. (2015). Chronic intestinal inflammation alters hippocampal neurogenesis. Journal of Neuroinflammation, 12, 65.
Acknowledgements
Many thanks to Dr. Lili Ma at Zhongshan Hospital of Fudan University for endoscopy examination and scoring. This work was funded by the National Key Basic Research Program of China (973 program), No. 2009CB522900, 2015CB554501; the Program for Outstanding Medical Academic Leader, No. 80; the Program of Shanghai Academic Research Leader, No. 17XD1403400, the National Natural Science Foundation of China, No. 81471738 and the National Institutes of Health grant (P20GM103472).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors disclose no conflicts.
Research involving human participants
All procedures performed in this study were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from every participant included in the study.
Rights and permissions
About this article
Cite this article
Bao, C., Liu, P., Liu, H. et al. Difference in regional neural fluctuations and functional connectivity in Crohn’s disease: a resting-state functional MRI study. Brain Imaging and Behavior 12, 1795–1803 (2018). https://doi.org/10.1007/s11682-018-9850-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11682-018-9850-z