Abstract
As concomitant hyperlaxity has been identified as an independent risk factor for failure following anterior shoulder stabilization, the treatment of this special pathology remains challenging. There is a broad consensus that a clear differentiation to multidirectional instability and isolated anteroinferior instability should be ensured to avoid unsatisfactory outcomes. Typical features of this patient collective include positive clinical tests for anteroinferior instability and multidirectional shoulder hyperlaxity, findings of an anterior labral lesion and general capsular redundancy in the radiologic assessment, while tests for posterior instability are negative. Surgical treatment should consist of an anteroinferior capsulolabroplasty with concomitant posteroinferior plication to reduce pathological capsular volume. Although there is a lack of clinical evidence, biomechanical investigations suggest that a four-anchor construct with three anterior anchors and one posteroinferior anchor may be sufficient to restore glenohumeral stability. This surgical approach is presented and discussed in the current article.
Zusammenfassung
Die Behandlung der anteroinferioren Schulterinstabilität mit begleitender multidirektionaler Hyperlaxität als unabhängiger Risikofaktor für das Fehlschlagen einer chirurgischen Stabilisierung stellt weiterhin eine klinische Herausforderung dar. Es besteht ein Konsens, dass dieses Krankheitsbild klar von der multidirektionalen und der isolierten anteroinferioren Schulterinstabilität differenziert werden sollte, um unbefriedigende klinische Ergebnisse zu vermeiden. Das Patientenkollektiv wird charakterisiert durch positive klinische Tests für anteroinferiore Instabilität und multidirektionale Schulterhyperlaxität sowie radiologische Befunde einer anterioren Labrumläsion und kapsulären Hyperlaxität, während die klinischen Tests für posteriore Instabilität negativ sind. Die chirurgische Behandlung besteht in einer anteroinferioren Rekonstruktion des Kapsel-Labrum-Komplexes mit gleichzeitiger posteroinferiorer Kapselplikatur zur Reduktion des supraphysiologischen Kapselvolumens. Bei insgesamt spärlicher klinischer Datenlage zu dieser Thematik legen biomechanische Untersuchungen nahe, dass ein Vier-Anker-Konstrukt mit drei anterioren Fadenankern und einem posteroinferior platzierten Anker suffizient für die Wiederherstellung der glenohumeralen Stabilität ist. Dieser chirurgische Ansatz wird im vorliegenden Beitrag vorgestellt und diskutiert.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Glenohumeral dislocations and subsequent shoulder instability represent a frequent and well-studied pathology [35, 86]. While there is a broad consensus throughout the literature concerning the definition of this pathology, therapeutic strategies in certain patient subgroups remain subject to ongoing controversy. Within the dominating entity of anteroinferior shoulder instabilities, which account for approximately 74–97% of cases [34, 35, 55], the treatment of patients presenting with concomitant supraphysiological joint laxity (defined as hyperlaxity) remains challenging and controversially discussed. In general, hyperlaxity has been identified as an independent risk factor for the incidence of recurrent shoulder instability with an odds ratio of 2.68 [53, 54] and can be found in approximately 13% of patients suffering from first-time shoulder dislocations [34]. Furthermore, hyperlaxity has been shown to be predictive for failure of arthroscopic Bankart repair in both primary [5, 10, 62, 77] and revision cases [72, 75]. Consequently, hyperlaxity is included in risk scoring systems as a major factor predictive of failure of arthroscopic Bankart repair [5]. To mitigate this risk, a reliable diagnosis and appropriate treatment are crucial for the successful management of this high-risk patient population. The present article aims to elucidate the distinct clinical patterns of patients suffering from anteroinferior shoulder instability with concomitant multidirectional hyperlaxity and provides a current concept of an arthroscopic technique to address this complex pathology.
Classification of shoulder instability
To adequately identify the subgroup at risk mentioned above, correct classification along the continuum of shoulder instabilities is essential. Multiple factors such as direction of dislocation, joint hyperlaxity, muscular dysbalances, bony defects, type and mechanism of event at onset of instability, number of dislocations as well as surgical history need to be considered in the classification of shoulder instability [46]. Consequently, there are various attempts in the literature to classify combinations of these features into the different types of instability, resulting in a complex system of overlapping, non-comprehensive classifications [23, 39, 49, 76].
Most of these classification systems do not allow for concise identification of the anteriorly unstable, “hyperlax subgroup” at risk, reflecting the clinical problem of correct identification and subsequent choice of therapeutic algorithm. For example, in the classification proposed by Matsen et al., the patients affected by anteroinferior instability and concomitant multidirectional hyperlaxity tend towards AMBRI-type (Atraumatic, Multidirectional, Bilateral, Rehabilitation, Inferior Capsular Shift) instability while also incorporating certain characteristics of the TUBS-type (Traumatic, Unilateral, Bankart defect, Surgery) instability [76]. In the Stanmore classification, the subgroup is located on the structurally defective axis tending towards Polar Group II [39]. Only Gerber and Nyffeler proposed a classification explicitly including hyperlaxity and direction of the instability, thereby allowing for the identification of the anteriorly unstable, multidirectionally hyperlax subgroup in their classification system [23].
Clinically, a strict separation of patients with anteroinferior instability and general hyperlaxity from traumatic anteroinferior instability without hyperlaxity is crucial in the selection of a subsequent treatment algorithm, but prone to errors. A seemingly adequate traumatic event at the onset of symptoms may lead to misclassification as a traumatic Polar Group I, TUBS type of instability and concomitantly to suboptimal treatment.
Inversely, a clear differentiation from multidirectional instability (MDI) is also necessary. MDI is rare—accounting for only 2–10% of all cases of shoulder instability [46, 55]—and definitions vary significantly [31, 41, 79]. However, unidirectional instability with multidirectional hyperlaxity, while infrequently termed and classified as multidirectional instability in the literature [32], should be understood as a separate entity and distinguished from the term MDI, which should be used exclusively for patients with symptomatic instability in the anterior, inferior and posterior direction [50].
Diagnosis
To avoid misclassification, clinical assessment should focus on an evaluation of the appropriateness of the trauma, the existence of signs of hyperlaxity of the (contralateral) shoulder and should include a thorough radiographic assessment. More precisely, the patient should be questioned regarding the exact mechanism of dislocation, previous episodes of shoulder instability as well as potential recurrent shoulder dislocations. In the clinical assessment, besides positive “classical” anterior instability tests such as the anterior apprehension test, relocation release test and anterior load and shift tests, clinical hyperlaxity is indicated by supraphysiological translation in the anterior/posterior drawer test, positive Sulcus sign and Gagey test and possibly a Beighton score > 3 [20]. Posterior instability tests such as the posterior load and shift test or Jerk test are typically negative and should also be routinely performed [20]. In the presence of an appropriate traumatic mechanism at primary dislocation, which is usually associated with reduced tolerance to the clinical assessment of the ipsilateral side, specific attention needs to be paid to the clinical assessment of the contralateral side to detect clinical hyperlaxity.
The radiographic assessment consisting of standard radiographs in anteroposterior direction, axial view as well as y‑view is commonly not associated with pathological findings in “hyperlax” patients. In contrast, magnetic resonance imaging (MRI) clearly identifies labral lesions such as an anterior Bankart lesion, often associated with a hypoplastic posterior labrum configuration [41] and, occasionally, concomitant asymptomatic posterior labral defects [30, 41]. The injection of contrast medium into the joint (arthro-MRI) further enhances soft tissue definition and facilitates superior visualization of the generally enlarged capsular volume indicative of shoulder joint hyperlaxity ([19, 32]; Fig. 1). While there is a low prevalence of concomitant bony defects in this collective, three-dimensional (3D) computed tomography can be employed in exceptional cases for quantification [9, 44] and risk-analysis [85] in cases of suspected critical bone lesions.
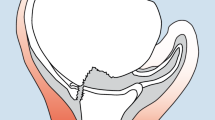
Comparison of typical findings in (arthro-)magnetic resonance imaging of an anteroinferiorly unstable shoulder with concomitant multidirectional hyperlaxity (a) and without hyperlaxity (b). Typical findings in patients with anteroinferior instability and concomitant multidirectional hyperlaxity include an anteroinferior Bankart lesion (white arrow, aI) and capsular redundancy with a wide inferior recess (white arrow, aII), compared to patients without hyperlaxity where bony defects, such as a prominent Hill–Sachs lesion (white arrow, bI&II), are typically found
Treatment
Patient-specific criteria warranting a non-operative strategy after primary shoulder dislocation include the absence of concomitant injuries, a patient age over 25 years and low-risk functional requirements [27, 54, 73]. In these cases, the established regimes include posttraumatic immobilization and early rehabilitation with increasingly permitted range of motion and actively assisted physiotherapy after 6 weeks [40, 69]. While an improvement of the insufficiency of passive shoulder stabilizers is not the primary aim, the focus of subsequent non-operative rehabilitation is the optimization of toning and proprioceptive capacities of the active glenohumeral stabilizers in (predominantly anteroinferior) humeral head centering and scapular control [11, 32, 80]. The physiotherapy regime is based on the principle of progressive resistance and relies on exercises targeting the deltoid muscles, rotator cuff muscles and scapulothoracic stabilizers employing elastic bands of progressively increasing stiffness within increasing degrees of elevation [11, 80]. After an initial phase of supervised therapy, lifelong self-guided maintenance exercises are recommended.
Operative treatment of anteroinferior instability with multidirectional hyperlaxity is generally warranted in patients younger than 25 years [27, 40], in the presence of concomitant injuries and after failure of non-operative treatment indicated by recurrent symptoms of anteroinferior instability such as (sub-)luxations or subjective signs of persistent anteroinferior instability after more than 6 months. Typical patterns of a patient indicated for surgical treatment are illustrated in Fig. 2.
Arthroscopic treatment
Arthroscopic labral repair and capsular plication are the gold standard when glenoid bone loss is below a critical threshold of approximately 15%, with decision-making depending on the presence of an on-track Hill–Sachs lesion (HSL) and the functional requirements of the patient [1, 60, 71].
In general, arthroscopic shoulder stabilization can be performed in either the lateral decubitus position with the advantages of better visualization and instrument access, or the beach chair position with a quick, more anatomical setup and improved possibility for open conversion [16]. While results across multiple studies show comparable results, systematic reviews and a meta-regression analysis identify slightly lower recurrence rates (14.65% ± 8.4% vs. 8.5% ± 7.1%) and marginally higher patient satisfaction in patients treated in the lateral decubitus position compared to the beach chair position (93–100% vs. 85–87.5%) [16, 22].
To address the anteroinferior instability component of the pathology, a capsulolabral repair with the arthroscopic placement of a minimum of three suture anchors is necessary for sufficient biomechanical stability [45], anatomic restoration of anteroinferior stabilizers [17] and favourable clinical results [1, 10]. Conventional biocompatible anchors, as well as the recently introduced all-suture anchors in a knotted and knotless configuration can be employed for the capsulolabral repair, since no differences in biomechanical strength [36, 38] or clinical results are reported anywhere in the literature [6, 51, 84].
Since MR-arthrographic investigations revealed that possibly increased capsular volume rather than ligamentous laxity itself is the critical morphological feature of shoulder hyperlaxity, multiple studies advocate the role of capsular volume reduction as a key component in the treatment of shoulder instability [2, 7, 19, 19, 21]. Additionally, biomechanical models show efficient reduction of glenohumeral translation by performing a capsular shift and capsulolabroplasty [3, 7, 63, 70, 78], thereby restoring physiological capsular volume [21].
In the anteroinferior quadrant, capsular volume reduction is achieved by a capsulolabroplasty, which has proved biomechanical effectiveness [3, 70, 78] and produces favourable clinical results [7, 21]. Typically, a minimum of three anchors are used at the 5:30, 4:00 and 3:00 o’clock position (right shoulder) to achieve maximum stability. Postoperative clinical and radiological evaluations advocate a special role for the most inferior anchor at the 5:30 o’clock position (right shoulder) and the “bumper” height created by capsular plication in this position for the postoperative success of the procedure [37].
However, biomechanical studies show that unidirectional anterior plication may lead to increased posterior translation and subluxation [3, 78], which may ultimately lead to degenerative joint wear [3, 8, 25]. While posteroinferior plication does not significantly influence anterior translation [59], biomechanical investigations suggest that an additional posteroinferior capsular volume reduction in addition to anteroinferior capsular plication is required for the optimal restoration of physiologic joint biomechanics [47, 67].
In recent decades, numerous different techniques for posteroinferior capsular volume reduction have been proposed [21, 52, 64]. Of these, capsular plication using simple sutures without any form of glenoid fixation has traditionally achieved favourable clinical results [21, 41]. However, while capsular plication to an intact labrum via sutures delivers similar strength of the construct compared to suture anchors, a suture-only technique is shown to cause a higher degree of labral displacement [67]. More specifically, dissociation of up to 1.5 mm has to be expected when not using glenoid anchors [67]. As the posterior capsule is known to be of a thinner, biomechanically less robust configuration [52], the literature advocates a low threshold in the decision for the use of suture anchors in posteroinferior capsulolabral surgery [52, 64]. For fixation, a simple stitch configuration is shown to be biomechanically sufficient [52]. Upon completion, a reduction of the capsular volume by up to 57% can be expected after combined posteroinferior and anteroinferior capsular plication [42, 82]. Furthermore, restoration of the physiologic tension of the posterior band of the inferior glenohumeral ligament (PIGHL), inserting at the 7:30–8:50 position (right shoulder), can be achieved in this procedure [17]. Directing the plication stitch from inferior to superior has proved to be biomechanically superior to a medial-to-lateral stitch direction, preserving the range of rotation while achieving equal reduction of glenohumeral translation [3]. Finally, in the rare presence of a critical off-track HSL, posteroinferior plication as an adjunct to a Bankart repair delivers similar resistance to anterior translation and Hill–Sachs engagement compared to a remplissage procedure while preserving the range of external rotation [81].
The management of concomitant injuries to the long head of the biceps tendon (LHBT) in the context of anteroinferior instability in the multidirectionally hyperlax shoulder is challenging. Biomechanical models have shown the LHBT to be a passive stabilizer of the glenohumeral joint by restricting omnidirectional glenohumeral translation by concavity compression [4, 29, 56], resisting torsional forces in the vulnerable ABER (abduction, external rotation) position [24, 68] and diminishing stress on the IGHL [68]. Furthermore, injuries to the superior labral anterior to posterior (SLAP) complex—especially the posterior part including the biceps anchor—have been demonstrated to biomechanically result in increased glenohumeral anterior and posterior translation [57, 58], which cannot be fully restored by biceps tenodesis [74]. While studies presenting data from biplane fluoroscopy investigations, which do not fully confirm these findings in vivo [24], do exist, the role for the LHBT as a passive glenohumeral stabilizer is still firmly postulated in the current literature. Thus, to preserve the LHBT as an additional stabilizer in the clinically hyperlax, anteroinferiorly unstable patient, a reconstructive procedure is recommended for concomitant injuries to the SLAP complex or LHBT when feasible. SLAP repair was demonstrated to provide convincing postoperative improvement of clinical scoring [65] and a return to sports [33] with an acceptable failure rate [65] in patients < 35 years, the typical age of the patients presenting with anteroinferior instability with multidirectional hyperlaxity. In selected cases, where surgery is indicated in patients with anteroinferior instability and hyperlaxity > 35 years with preexisting degenerative lesions of the biceps anchor, a biceps tenodesis may be considered due to the superior clinical results, a return to activity [18] and lower revision rates [15] in this age group. A combined approach addressing injury to the LHB with biceps tenodesis while attempting to preserve the biomechanical advantages of an intact SLAP complex with a SLAP repair is not advised, as this results in significantly worse clinical outcome compared to isolated procedures [12].
While certain studies recommend rotator interval closure as an adjunct procedure when addressing clinical instability with arthroscopic Bankart repair and posteroinferior plication [13], there is no consensus on the indication of this procedure [14, 66]. Due to lack of consensus on the definition of the procedure, reports in the literature remain inhomogenous [14]. While biomechanically the closure of the rotator interval reduces overall glenohumeral translation—most markedly in the inferior direction [61, 83]—reports on the subsequent effect on glenohumeral stability remain ambiguous [26, 43, 48]. Moreover, rotator interval closure results in a significant loss of range of motion [14, 48]. While the literature suggests critically evaluating rotator interval closure in cases of multidirectional instability or shoulder instability with extensive inferior laxity [14, 66], there is insufficient evidence to recommend this procedure as a standard treatment for anteroinferior instability with multidirectional hyperlaxity.
In daily practice, the authors perform arthroscopic anteroinferior capsulolabroplasty and posteroinferior plication (Fig. 3) for anterior shoulder instability with multidirectional laxity. Preoperatively, anteroinferior instability and multidirectional hyperlaxity are confirmed by clinical examination under general anesthesia and the patient is placed in lateral decubitus position. After establishing a standard posterior viewing portal and the subsequent diagnostic visualization of the joint (Fig. 4a), an anterosuperior viewing and an anteroinferior working portal is created. Subsequently, the capsulolabral complex is carefully mobilized (Fig. 4b–d) and a bleeding bed is induced along the glenoid rim to enhance healing capacity (Fig. 4e). For posteroinferior capsular plication, a deep posterolateral portal (approximately 2 cm laterally and 6 cm caudally to the posterolateral acromion) is established (Fig. 5).
a Proposed technique for arthroscopic stabilization with anteroinferior capsulolabroplasty consisting of a minimum of three anterior suture anchors and posteroinferior plication with an additional suture anchor at the 7 o’clock position, with an optional suture anchor at 8 o’clock in case of persistent hyperlaxity. b Anchors should be inserted at an angle of 135° to the glenoid surface to avoid chondral damage or anchor dislocation
Intraoperative arthroscopic images of a right shoulder in the lateral decubitus position. a Hypoplastic posterior labrum; b mobilisation of the anterior labrum; c creation of a bleeding bed; d placement of a posteroinferior anchor (7:00); e–f posteroinferior plication; g placement of an anteroinferior anchor (5:30); h placement of an anterior anchor (4:00); i completed anteroinferior stabilization
Intraoperative image of cannula setting with a standard posterior viewing portal, an anterosuperior viewing and an anteroinferior working portal equipped with Twist-In™ cannulas (Arthex, Naples, FL, USA) and a deep posterolateral portal equipped with a Gemini cannula (Arthex, Naples, FL, USA), before the establishment of the 5:30 portal
The first suture anchor (FiberTak®-Soft 1.6 mm all-suture anchor; Arthex, Naples, FL, USA) is introduced posteroinferiorly at the 7 o’clock position (right shoulder) at the chrondrolabral junction, and the anchor’s suture is passed through the capsular tissue 10–15 mm posteroinferiorly of the labrum to shift the PIGHL complex superomedially and reduce the capsular volume of the posteroinferior axillary pouch and posterior joint space. The knot is tightened while correct position and tension of the capsulolabral complex are ensured with a grasper superiorly of the knot.
Using the anteroinferior working portal at the 5:30 position [28], the first anteroinferior suture anchor is placed in the 5:30 position (right shoulder) at the chrondrolabral junction (Fig. 4j). The AIGHL complex as well as the anteroinferior axillary pouch are purchased equivalently to the posteroinferior capsulolabroplasty. In the same way, two further anchors are introduced at the 4:30 and 3:00 o’clock positions and a capsulolabral “bumper” is created at the anteroinferior circumference of the glenoid (Fig. 4j–l).
After tying the knots, anterior, posterior and inferior translation are carefully tested. If reduction of posterior translation is found to still be insufficient, a second posteroinferior anchor can be inserted at the 8 o’clock position in the same manner as the 7 o’clock anchor.
Postoperative management
The postoperative management regime is equivalent to an anteroinferior Bankart repair. A sling orthosis is required to maintain immobilization and preservation of the repair and should be worn during the night and walking for 6 weeks postoperatively. For the first 3 weeks following surgery, range of motion in abduction is gradually increased from 45° to 90°, while external rotation is limited to 0°. After 6 weeks, a regime with actively assisted range of motion exercises is initiated. Strengthening exercises are initiated 3 months after surgery and no contact sports should be started before 6 months postoperatively.
Pearls and pitfalls
-
For the posteroinferior portal, a cannula with a deployable wing feature should be employed to prevent dislocation of the cannula and enable enlargement of the posteroinferior working space by applying traction to the cannula.
-
When establishing the 5:30 portal, a blunt preparation technique should be employed to spare neurovascular structures. A switching stick can be advanced to the humeral shaft and directed cranially to penetrate the capsule directly superior to the AIGHL complex and subsequently used for the placement of a cannula.
-
When performing anteroinferior capsulolabroplasty via an anteroinferior portal only (not employing a deep anteroinferior [5:30] portal), the use of all-suture anchors provides the benefit of using curved guides to achieve optimal positioning of the anteroinferior (5:30) anchor.
-
Knots should be tied in the capsular tissue away from the chondrolabral junction to avoid chondral damage to the glenoid or humeral head during glenohumeral motion.
-
Anchors should be inserted at an angle of 135° to the glenoid surface to avoid chondral damage or anchor dislocation.
-
During capsular plication, an inferior-to-superior stitching direction should be selected to sufficiently reduce inferior capsular redundancy.
Clinical take home message
-
Patients with multidirectional hyperlaxity represent a subgroup at risk of failure in arthroscopic Bankart repair for anteroinferior shoulder instability.
-
With regard to classification and terminology, a clear differentiation to multidirectional instability and isolated anteroinferior instability must be ensured.
-
The key factor for diagnosis is the physical examination of the affected shoulder with positive tests for unidirectional anteroinferior instability and concomitant signs of shoulder hyperlaxity.
-
Anteroinferior capsulolabroplasty and posteroinferior plication to reduce capsular redundancy restore stability while preserving physiological glenohumeral biomechanics.
-
A minimum of four suture anchors in a simple stitch configuration should be used at the 3–7 o’clock position (right shoulder) to generate a sufficient bumper and to reduce capsular volume effectively.
References
Aboalata M, Plath JE, Seppel G et al (2017) Results of arthroscopic bankart repair for anterior-inferior shoulder instability at 13-year follow-up. Am J Sports Med 45:782–787
Ahmad CS, Freehill MQ, Blaine TA et al (2003) Anteromedial capsular redundancy and labral deficiency in shoulder instability. Am J Sports Med 31:247–252
Ahmad CS, Wang VM, Sugalski MT et al (2005) Biomechanics of shoulder capsulorrhaphy procedures. J Shoulder Elbow Surg 14:12s–18s
Alexander S, Southgate DF, Bull AM et al (2013) The role of negative intraarticular pressure and the long head of biceps tendon on passive stability of the glenohumeral joint. J Shoulder Elbow Surg 22:94–101
Balg F, Boileau P (2007) The instability severity index score. A simple pre-operative score to select patients for arthroscopic or open shoulder stabilisation. J Bone Joint Surg Br 89:1470–1477
Bents EJ, Brady PC, Adams CR et al (2017) Patient-reported outcomes of knotted and knotless glenohumeral labral repairs are equivalent. Am J Orthop (Belle Mead NJ) 46:279–283
Bigliani LU, Kurzweil PR, Schwartzbach CC et al (1994) Inferior capsular shift procedure for anterior-inferior shoulder instability in athletes. Am J Sports Med 22:578–584
Bigliani LU, Weinstein DM, Glasgow MT et al (1995) Glenohumeral arthroplasty for arthritis after instability surgery. J Shoulder Elbow Surg 4:87–94
Bishop JY, Jones GL, Rerko MA et al (2013) 3‑D CT is the most reliable imaging modality when quantifying glenoid bone loss. Clin Orthop Relat Res 471:1251–1256
Boileau P, Villalba M, Héry JY et al (2006) Risk factors for recurrence of shoulder instability after arthroscopic Bankart repair. J Bone Joint Surg Am 88:1755–1763
Burkhead WZ Jr., Rockwood CA Jr. (1992) Treatment of instability of the shoulder with an exercise program. J Bone Joint Surg Am 74:890–896
Chalmers PN, Monson B, Frank RM et al (2016) Combined SLAP repair and biceps tenodesis for superior labral anterior-posterior tears. Knee Surg Sports Traumatol Arthrosc 24:3870–3876
Chiang ER, Wang JP, Wang ST et al (2010) Arthroscopic posteroinferior capsular plication and rotator interval closure after Bankart repair in patients with traumatic anterior glenohumeral instability—a minimum follow-up of 5 years. Injury 41:1075–1078
Coughlin RP, Bullock GS, Shanmugaraj A et al (2018) Outcomes after arthroscopic rotator interval closure for shoulder instability: a systematic review. Arthroscopy 34:3098–3108.e1
de Sa D, Arakgi ME, Lian J et al (2019) Labral repair versus biceps tenodesis for primary surgical management of type II superior labrum anterior to posterior tears: a systematic review. Arthroscopy 35:1927–1938
de Sa D, Sheean AJ, Morales-Restrepo A et al (2019) Patient positioning in arthroscopic management of posterior-inferior shoulder instability: a systematic review comparing beach chair and lateral decubitus approaches. Arthroscopy 35:214–224.e3
Dekker TJ, Aman ZS, Peebles LA et al (2020) Quantitative and qualitative analyses of the glenohumeral ligaments: an anatomic study. Am J Sports Med 48:1837–1845
Denard PJ, Lädermann A, Parsley BK et al (2014) Arthroscopic biceps tenodesis compared with repair of isolated type II SLAP lesions in patients older than 35 years. Orthopedics 37:e292–297
Dewing CB, Mccormick F, Bell SJ et al (2008) An analysis of capsular area in patients with anterior, posterior, and multidirectional shoulder instability. Am J Sports Med 36:515–522
DVSE (2012) Untersuchungstechniken des Schultergelenks. Obere Extremität 7:1–67
Eberbach H, Jaeger M, Bode L et al (2020) Arthroscopic Bankart repair with an individualized capsular shift restores physiological capsular volume in patients with anterior shoulder instability. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-020-05952-3
Frank RM, Saccomanno MF, Mcdonald LS et al (2014) Outcomes of arthroscopic anterior shoulder instability in the beach chair versus lateral decubitus position: a systematic review and meta-regression analysis. Arthroscopy 30:1349–1365
Gerber C, Nyffeler RW (2002) Classification of glenohumeral joint instability. Clin Orthop Relat Res 400:65–76. https://doi.org/10.1097/00003086-200207000-00009
Giphart JE, Elser F, Dewing CB et al (2012) The long head of the biceps tendon has minimal effect on in vivo glenohumeral kinematics: a biplane fluoroscopy study. Am J Sports Med 40:202–212
Green A, Norris TR (2001) Shoulder arthroplasty for advanced glenohumeral arthritis after anterior instability repair. J Shoulder Elbow Surg 10:539–545
Harryman DT 2nd, Sidles JA, Harris SL et al (1992) The role of the rotator interval capsule in passive motion and stability of the shoulder. J Bone Joint Surg Am 74:53–66
Hovelius L, Olofsson A, Sandström B et al (2008) Nonoperative treatment of primary anterior shoulder dislocation in patients forty years of age and younger. a prospective twenty-five-year follow-up. J Bone Joint Surg Am 90:945–952
Imhoff AB, Ansah P, Tischer T et al (2010) Arthroscopic repair of anterior-inferior glenohumeral instability using a portal at the 5:30-o’clock position: analysis of the effects of age, fixation method, and concomitant shoulder injury on surgical outcomes. Am J Sports Med 38:1795–1803
Itoi E, Kuechle DK, Newman SR et al (1993) Stabilising function of the biceps in stable and unstable shoulders. J Bone Joint Surg Br 75:546–550
Javed S, Gheorghiu D, Torrance E et al (2019) The incidence of traumatic posterior and combined labral tears in patients undergoing arthroscopic shoulder stabilization. Am J Sports Med 47:2686–2690
Johansson K (2016) Multidirectional instability of the glenohumeral joint: an unstable classification resulting in uncertain evidence-based practice. Br J Sports Med 50:1105–1106
Johnson SM, Robinson CM (2010) Shoulder instability in patients with joint hyperlaxity. J Bone Joint Surg Am 92:1545–1557
Kaisidis A, Pantos P, Heger H et al (2011) Arthroscopic fixation of isolated type II SLAP lesions using a two-portal technique. Acta Orthop Belg 77:160–166
Kraeutler MJ, McCarty EC, Belk JW et al (2018) Descriptive epidemiology of the MOON shoulder instability cohort. Am J Sports Med 46:1064–1069
Krøner K, Lind T, Jensen J (1989) The epidemiology of shoulder dislocations. Arch Orthop Trauma Surg 108:288–290
Lacheta L, Brady A, Rosenberg SI et al (2020) Biomechanical evaluation of knotless and knotted all-suture anchor repair constructs in 4 Bankart repair configurations. Arthroscopy 36:1523–1532
Lee SJ, Kim JH, Gwak HC et al (2020) Influence of glenoid labral bumper height and capsular volume on clinical outcomes after arthroscopic Bankart repair as assessed with serial CT Arthrogram: Can anterior-inferior volume fraction be a prognostic factor? Am J Sports Med 48:1846–1856
Leedle BP, Miller MD (2005) Pullout strength of knotless suture anchors. Arthroscopy 21:81–85
Lewis A, Kitamura T, Bayley JIL (2004) (ii) The classification of shoulder instability: new light through old windows! Curr Orthop 18:97–108
Longo UG, Loppini M, Rizzello G et al (2014) Management of primary acute anterior shoulder dislocation: systematic review and quantitative synthesis of the literature. Arthroscopy 30:506–522
Longo UG, Rizzello G, Loppini M et al (2015) Multidirectional instability of the shoulder: a systematic review. Arthroscopy 31:2431–2443
Lubowitz J, Bartolozzi A, Rubinstein D et al (1996) How much does inferior capsular shift reduce shoulder volume? Clin Orthop Relat Res 328:86–90. https://doi.org/10.1097/00003086-199607000-00015
Maman E, Dolkart O, Kazum E et al (2017) Rotator interval closure has no additional effect on shoulder stability compared to Bankart repair alone. Arch Orthop Trauma Surg 137:673–677
Martetschläger F, Kraus TM, Hardy P et al (2013) Arthroscopic management of anterior shoulder instability with glenoid bone defects. Knee Surg Sports Traumatol Arthrosc 21:2867–2876
Martetschläger F, Michalski MP, Jansson KS et al (2014) Biomechanical evaluation of knotless anterior and posterior Bankart repairs. Knee Surg Sports Traumatol Arthrosc 22:2228–2236
Martetschläger F, Tauber M, Habermeyer P (2017) Diagnostics and treatment concepts for anteroinferior shoulder instability : current trends. Orthopade 46:877–892
Mayer SW, Kraszewski AP, Skelton A et al (2018) What are the effects of capsular plication on translational laxity of the glenohumeral joint: a study in cadaveric shoulders. Clin Orthop Relat Res 476:1526–1536
Mologne TS, Zhao K, Hongo M et al (2008) The addition of rotator interval closure after arthroscopic repair of either anterior or posterior shoulder instability: effect on glenohumeral translation and range of motion. Am J Sports Med 36:1123–1131
Moroder P, Danzinger V, Maziak N et al (2020) Characteristics of functional shoulder instability. J Shoulder Elbow Surg 29:68–78
Neer CS 2nd, Foster CR (1980) Inferior capsular shift for involuntary inferior and multidirectional instability of the shoulder. A preliminary report. J Bone Joint Surg Am 62:897–908
Ng DZ, Kumar VP (2014) Arthroscopic Bankart repair using knot-tying versus knotless suture anchors: is there a difference? Arthroscopy 30:422–427
Nho SJ, Frank RM, Van Thiel GS et al (2010) A biomechanical analysis of shoulder stabilization: posteroinferior glenohumeral capsular plication. Am J Sports Med 38:1413–1419
O’driscoll SW, Evans DC (1991) Contralateral shoulder instability following anterior repair. An epidemiological investigation. J Bone Joint Surg Br 73:941–946
Olds M, Ellis R, Donaldson K et al (2015) Risk factors which predispose first-time traumatic anterior shoulder dislocations to recurrent instability in adults: a systematic review and meta-analysis. Br J Sports Med 49:913–922
Owens BD, Duffey ML, Nelson BJ et al (2007) The incidence and characteristics of shoulder instability at the United States military academy. Am J Sports Med 35:1168–1173
Pagnani MJ, Deng XH, Warren RF et al (1996) Role of the long head of the biceps brachii in glenohumeral stability: a biomechanical study in cadavera. J Shoulder Elbow Surg 5:255–262
Pagnani MJ, Speer KP, Altchek DW et al (1995) Arthroscopic fixation of superior labral lesions using a biodegradable implant: a preliminary report. Arthroscopy 11:194–198
Panossian VR, Mihata T, Tibone JE et al (2005) Biomechanical analysis of isolated type II SLAP lesions and repair. J Shoulder Elbow Surg 14:529–534
Peltier KE, Mcgarry MH, Tibone JE et al (2012) Effects of combined anterior and posterior plication of the glenohumeral ligament complex for the repair of anterior glenohumeral instability: a biomechanical study. J Shoulder Elbow Surg 21:902–909
Piasecki DP, Verma NN, Romeo AA et al (2009) Glenoid bone deficiency in recurrent anterior shoulder instability: diagnosis and management. J Am Acad Orthop Surg 17:482–493
Plausinis D, Bravman JT, Heywood C et al (2006) Arthroscopic rotator interval closure: effect of sutures on glenohumeral motion and anterior-posterior translation. Am J Sports Med 34:1656–1661
Pogorzelski J, Fritz EM, Horan MP et al (2018) Failure following arthroscopic Bankart repair for traumatic anteroinferior instability of the shoulder: is a glenoid labral articular disruption (GLAD) lesion a risk factor for recurrent instability? J Shoulder Elbow Surg 27:e235–e242
Ponce BA, Rosenzweig SD, Thompson KJ et al (2011) Sequential volume reduction with capsular plications: relationship between cumulative size of plications and volumetric reduction for multidirectional instability of the shoulder. Am J Sports Med 39:526–531
Provencher MT, Leclere LE, King S et al (2011) Posterior instability of the shoulder: diagnosis and management. Am J Sports Med 39:874–886
Provencher MT, Mccormick F, Dewing C et al (2013) A prospective analysis of 179 type 2 superior labrum anterior and posterior repairs: outcomes and factors associated with success and failure. Am J Sports Med 41:880–886
Provencher MT, Peebles LA (2018) Editorial commentary: rotator interval closure of the shoulder continues to be a challenge in consensus on treatment. Arthroscopy 34:3109–3111
Provencher MT, Verma N, Obopilwe E et al (2008) A biomechanical analysis of capsular plication versus anchor repair of the shoulder: can the labrum be used as a suture anchor? Arthroscopy 24:210–216
Rodosky MW, Harner CD, Fu FH (1994) The role of the long head of the biceps muscle and superior glenoid labrum in anterior stability of the shoulder. Am J Sports Med 22:121–130
Scheibel M, Kuke A, Nikulka C et al (2009) How long should acute anterior dislocations of the shoulder be immobilized in external rotation? Am J Sports Med 37:1309–1316
Schneider DJ, Tibone JE, Mcgarry MH et al (2005) Biomechanical evaluation after five and ten millimeter anterior glenohumeral capsulorrhaphy using a novel shoulder model of increased laxity. J Shoulder Elbow Surg 14:318–323
Shaha JS, Cook JB, Song DJ et al (2015) Redefining “critical” bone loss in shoulder instability: functional outcomes worsen with “subcritical” bone loss. Am J Sports Med 43:1719–1725
Shin JJ, Mascarenhas R, Patel AV et al (2015) Clinical outcomes following revision anterior shoulder arthroscopic capsulolabral stabilization. Arch Orthop Trauma Surg 135:1553–1559
Simonet WT, Cofield RH (1984) Prognosis in anterior shoulder dislocation. Am J Sports Med 12:19–24
Strauss EJ, Salata MJ, Sershon RA et al (2014) Role of the superior labrum after biceps tenodesis in glenohumeral stability. J Shoulder Elbow Surg 23:485–491
Su F, Kowalczuk M, Ikpe S et al (2018) Risk factors for failure of arthroscopic revision anterior shoulder stabilization. J Bone Joint Surg Am 100:1319–1325
Thomas SC, Matsen FA 3rd (1989) An approach to the repair of avulsion of the glenohumeral ligaments in the management of traumatic anterior glenohumeral instability. J Bone Joint Surg Am 71:506–513
Voos JE, Livermore RW, Feeley BT et al (2010) Prospective evaluation of arthroscopic bankart repairs for anterior instability. Am J Sports Med 38:302–307
Wang VM, Sugalski MT, Levine WN et al (2005) Comparison of glenohumeral mechanics following a capsular shift and anterior tightening. J Bone Joint Surg Am 87:1312–1322
Warby SA, Pizzari T, Ford JJ et al (2016) Exercise-based management versus surgery for multidirectional instability of the glenohumeral joint: a systematic review. Br J Sports Med 50:1115–1123
Watson L, Balster S, Lenssen R et al (2018) The effects of a conservative rehabilitation program for multidirectional instability of the shoulder. J Shoulder Elbow Surg 27:104–111
Werner BC, Chen X, Camp CL et al (2017) Medial posterior capsular plication reduces anterior shoulder instability similar to remplissage without restricting motion in the setting of an engaging Hill-Sachs defect. Am J Sports Med 45:1982–1989
Wiater JM, Vibert BT (2007) Glenohumeral joint volume reduction with progressive release and shifting of the inferior shoulder capsule. J Shoulder Elbow Surg 16:810–814
Wolf RS, Zheng N, Iero J et al (2004) The effects of thermal capsulorrhaphy and rotator interval closure on multidirectional laxity in the glenohumeral joint: a cadaveric biomechanical study. Arthroscopy 20:1044–1049
Wu IT, Desai VS, Mangold DR et al (2020) Comparable clinical outcomes using knotless and knot-tying anchors for arthroscopic capsulolabral repair in recurrent anterior glenohumeral instability at mean 5‑year follow-up. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-020-06057-7
Yamamoto N, Itoi E, Abe H et al (2007) Contact between the glenoid and the humeral head in abduction, external rotation, and horizontal extension: a new concept of glenoid track. J Shoulder Elbow Surg 16:649–656
Zacchilli MA, Owens BD (2010) Epidemiology of shoulder dislocations presenting to emergency departments in the United States. J Bone Joint Surg Am 92:542–549
Funding
Open Access funding enabled and organized by Projekt DEAL.
Author information
Authors and Affiliations
Contributions
All authors contributed in a significant way to writing and editing the manuscript. MCR, ABI, SS, BS and JP conceived of the idea for the manuscript and made substantial contributions to its conception, design and writing. MCR and JP were engaged in writing the manuscript. SS, BS and ABI provided figures and made edits to the manuscript. All authors read and approved the final manuscript. All authors provided critical feedback and helped shape the analysis and the manuscript. All authors read and approved the final manuscript
Corresponding author
Ethics declarations
Conflict of interest
A.B. Imhoff receives royalties from Arthrex. M.-C. Rupp, S. Siebenlist, B. Scheiderer, and J. Pogorzelski declare that they have no competing interests.
For this article no studies with human participants or animals were performed by any of the authors. All studies performed were in accordance with the ethical standards indicated in each case.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Rupp, MC., Siebenlist, S., Scheiderer, B. et al. Indication and technique for arthroscopic stabilization of anterior shoulder instability with multidirectional laxity. Obere Extremität 16, 41–50 (2021). https://doi.org/10.1007/s11678-021-00623-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11678-021-00623-2