Abstract
Depending on their size, all glenoid defects lead to a certain amount of loss of glenohumeral stability and therefore may represent a risk factor for the recurrence of instability after soft tissue stabilization procedures. The degree of loss of stability depends not only on the extent of the defect but also on differences in individual constitutional shape, which need to be analyzed in a three-dimensional context. Additionally, patient-specific factors such as age and activity level have a significant influence on the clinical effect of glenoid bone loss. Therefore, when treating a patient with glenoid bone loss, a bony glenoid reconstruction surgery in the form of a free bone graft transfer or Latarjet should be considered based on the extent of the defect, native glenoid shape, age, and activity level. Furthermore, in the presence of a relevant Hill–Sachs defect, the addition of a remplissage to a Bankart procedure should be considered or the use of a bony glenoid augmentation procedure instead.
Zusammenfassung
Abhängig von ihrer Größe führen alle Glenoiddefekte zu einem mehr oder weniger relevanten Verlust von glenohumeraler Stabilität und müssen deshalb als ein Risikofaktor für Rezidivinstabilität nach Weichteilstabilisierungsoperationen der Schulter angesehen werden. Das Ausmaß des Stabilitätsverlusts hängt jedoch nicht nur von der Defektgröße ab, sondern auch von der individuellen Glenoidmorphologie, welche in einem dreidimensionalen Kontext betrachtet werden muss. Zusätzlich haben patientenspezifische Faktoren wie Alter und Aktivitätsniveau einen großen Einfluss auf die klinische Auswirkung von Glenoiddefekten. Deshalb sollte bei Patienten mit Glenoiddefekt nicht nur die Defektgröße, sondern auch die individuelle Glenoidmorphologie, das Patientenalter und Aktivitätsniveau in die Entscheidung für oder gegen eine knöcherne Glenoidrekonstruktionstechnik in Form einer Spanplastik oder einer Latarjet-Operation mit einbezogen werden. Zusätzlich sollte im Fall einer relevanten Hill-Sachs-Läsion die Durchführung einer Remplissage als Zusatz zur Bankart-Operation erwogen werden oder stattdessen die Durchführung einer knöchernen Glenoidaugmentationsoperation.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Shoulder instability is a common pathology that mostly affects young patients [40]. The causes can be either of structural nature (structural shoulder instability) or functional nature (functional shoulder instability; [26]). A key step for successfully treating shoulder instability is the identification of the cause of instability and its subsequent elimination with a specific surgical procedure (structural instability) or physiotherapeutic intervention (functional instability). The purpose of this review is to provide an overview of the European perspective of how to treat structural bony defects in patients with anterior shoulder instability.
Glenoid bone loss
Glenoid bone loss in patients with anterior shoulder instability is a major risk factor for recurrence of instability after soft tissue stabilization surgery [9, 36]. It has been widely accepted that in the case of significant glenoid bone loss, a bony glenoid reconstruction surgery should be performed instead of simply soft tissue stabilization [10]. Since Burkhart and De Beer first highlighted the importance of general glenoid bone loss in the year 2000 [9], several clinical and biomechanical studies have tried to establish the critical threshold that makes a glenoid defect significant.
The earliest biomechanical studies found that the critical glenoid bone loss starts at approximately 20–30% [21, 37, 38]. The main problem was the lack of agreement in terms of measurement technique for bone loss. Among others, the two most common measurements, defect diameter and defect area, were viewed as one and the same in clinical as well as scientific practice. However, these two measurement techniques render widely differing results and have a nonlinear relationship ([6, 31]; Fig. 1). Therefore, several study results reporting on glenoid bone loss have to be reinterpreted. If, for example, the results of the aforementioned earliest biomechanical studies are translated to the Pico method (3D en-face defect area measurement in relation to a best-fit circle; [5]), the critical glenoid bone loss would start at 14–25%.
Two-dimensional en-face measurement technique for a defect diameter and b defect area in relation to a best-fit circle of the glenoid. c The relationship between both measurements is nonlinear as outlined in the graph. d The pizza slice analogy helps to understand this nonlinear relationship. If a pizza is cut into stripes of equal diameter, the outer stripes will have less area than the central stripes
Furthermore, on closer inspection, the biomechanical data show a progressive but not abrupt decrease of stability with increasing glenoid bone loss, meaning that in reality the critical threshold value will also be variable depending on patient-specific factors such as age and activity level. Accordingly, Bankart surgeries in a cohort of non-athletic patients with large glenoid defects (20–29% diameter or 14–24% area) showed excellent clinical results with a low recurrence rate [22], while Bankart surgeries in a highly active cohort of patients rendered unsatisfactory results already starting with small glenoid defects of 13.5% diameter, which translates to 8% area [35].
Furthermore, in a recent rigid-body computer simulation, it was shown that current (mono- or two-dimensional) measurement techniques oversimplify the issue as they do not account for the concave shape of the glenoid that is responsible for bone-mediated stability by means of the so-called concavity compression effect. In fact, when considering the concave shape of the glenoid, it shows that the relationship between the glenoid defect size and the resulting biomechanical effect is non-linear and that smaller defects have a far greater impact than previously acknowledged [25]. Additionally, a case–control study found large interindividual glenoid shape differences in terms of concavity depth. Patients with unilateral shoulder instability showed significantly flatter glenoids on the unaffected side than did healthy controls. This means that several patients with instability have constitutional biomechanically relevant glenoid shape deficiencies that are not accounted for with current measurement techniques (Fig. 2; [27]).
a Axial computed tomography scans of two right shoulders showing individual constitutional glenoid concavity shape differences. b The theoretical half-pipe example shows that the first meter of defect (red line) leads to more loss of concavity than the second meter (orange line). By analogy, the first millimeter of glenoid defect counts the most in terms of stability. (With kind permission of SAGE Journals [25])
Increasing glenoid bone loss leads to a gradual decrease of stability
In summary, it can be stated that all glenoid defects lead to a loss of glenohumeral stability. The degree of loss of stability depends on individual constitutional shape differences and the defect extent that needs to be analyzed in a three-dimensional context. The fact that software allowing for these kinds of complex analyses in daily clinical practice are currently not available along with the fact that patient-specific factors such as age and activity level have a significant influence on the clinical effect of glenoid bone loss called into question our natural tendency of trying to set a general threshold value for critical glenoid bone loss in anterior shoulder instability.
Hill–Sachs defect
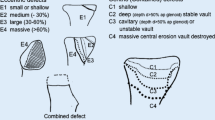
Similar to glenoid defects, Hill–Sachs defects of the humeral head are also a risk factor for instability. However, the mechanism of instability is different. While glenoid defects diminish the stability ratio of the joint by reducing the concavity (“the ball jumps out of the socket more easily”), Hill–Sachs defects can engage with the glenoid rim during end-range of motion. As explained in the glenoid track concept [15], glenoid defects can increase the risk of engagement, as the glenoid track becomes narrower (“the narrow glenoid falls into the Hill–Sachs defect more easily”) thus creating a synergistic negative effect. Biomechanical studies showed that in the presence of a combined Hill–Sachs and glenoid defect (bipolar bone loss; Fig. 3) smaller defects that individually would be considered noncritical become critical defects [2, 18]. Accordingly, the appreciation of bipolar bone loss is a stronger predictor for recurrence of instability after Bankart repair than glenoid bone loss alone [34]. However, the identification of a threshold for critical Hill–Sachs lesions seems to be even more difficult than it is for glenoid defects when considering that the engagement largely depends on rotational capacity, which varies considerably between individuals depending on laxity.
Treatment approaches
Based on the aforementioned considerations, bony stabilization surgeries (e.g., Latarjet or free bone graft transfers) have gained ground against soft tissue stabilization techniques (e.g., Bankart Repair). While a large majority of instability cases are still treated with Bankart surgeries, some authors advocate for the general replacement of Bankart surgeries with the Latarjet due to an admittedly higher stabilization success rate, especially in the long-term follow-up [41]. However, there is also concern regarding this approach, as it leads to overtreatment of patients with a non-anatomical procedure that carries a rather high risk for complications. Obviously, this rate of complications varies from surgeon to surgeon. While we reported low rates of complications in a prospective randomized trial [29], up to 30% of complication rate have been reported in systematic reviews [11]. Hardware problems are among the most frequently mentioned complications. This might be explained by the fact that if bony stabilization techniques are used in the case of no or little bone loss, the graft undergoes extensive resorption processes according to Wolff’s law [17] which might lead to secondary hardware protrusion into the subscapularis or even into the joint. This graft resorption has been reported for the Latarjet procedure [14] as well as for the free bone graft transfers [24, 28]. Due to these considerations, an undifferentiated switch from soft tissue to bony stabilization procedures seems to be overtreatment that comes at a price. On the other hand, it cannot be ignored that the soft tissue stabilization procedures show quite high redislocation rates at long-term follow-up [30]. A patient-specific approach factoring in not only bony defects but also other risk factors such as, for example, age and activity level seems feasible [3, 16]. When deciding which bony glenoid reconstruction surgery to choose between Latarjet and free bone graft transfers (e.g., iliac crest bone grafts), there is evidence that both lead to similar outcomes and mostly differ regarding their types of complications [29].
Free bone graft transfers and coracoid transfers lead to similar clinical outcomes
Examples of recent attempts to decrease complication rates for both methods include altered fixation types in the form of endobuttons [8] or the use of allografts for the free bone graft transfers [33]; however, both modifications still need further evaluation [7, 19].
Regarding the Hill–Sachs defect, there is growing evidence that its treatment in the form of a remplissage can improve outcomes in terms of stability [4, 20, 23]. However, this procedure conveys the risk for affecting rotational range of motion [1, 32]. As an alternative treatment, the Latarjet procedure has been proposed for patients with subcritical glenoid but critical Hill–Sachs defects as it leads to comparable stability levels. However, the restriction in range of motion is similar and the complication risk seems to be higher [12, 13]. Despite this elevated risk for complications, significant advantages have been observed in revision cases and contact athletes [39].
Practical conclusion
-
Even moderate glenoid defects are a relevant risk factor of recurrence of instability after soft tissue stabilization procedures.
-
Therefore, a bony glenoid reconstruction surgery in the form of a free bone graft transfer or Latarjet should be considered based on the extent of the defect and the patient’s age and activity level.
-
The effect of Hill–Sachs lesions should not be disregarded. If a relevant Hill–Sachs defect is present, the addition of a remplissage to a Bankart procedure should be considered or the use of a bony glenoid augmentation procedure instead.
References
Alkaduhimi H, Verweij LPE, Willigenburg NW, van Deurzen DFP, van den Bekerom MPJ (2019) Remplissage with Bankart repair in anterior shoulder instability: a systematic review of the clinical and cadaveric literature. Arthroscopy 35(4):1257–1266
Arciero RA, Parrino A, Bernhardson AS et al (2015) The effect of a combined Glenoid and Hill-Sachs defect on Glenohumeral stability: a biomechanical cadaveric study using 3‑dimensional modeling of 142 patients. Am J Sports Med 43(6):1422–9
Balg F, Boileau P (2007) The instability severity index score. A simple pre-operative score to select patients for arthroscopic or open shoulder stabilisation. J Bone Joint Surg Br 89(11):1470–1477
Bastard C, Herisson O, Gaillard J, Nourissat G (2019) Impact of remplissage on global shoulder outcome: a long-term comparative study. Arthroscopy 35(5):1362–1367
Baudi P, Righi P, Bolognesi D et al (2005) How to identify and calculate glenoid bone deficit. Chir Organi Mov 90(2):145–152
Bhatia S, Saigal A, Frank RM et al (2015) Glenoid diameter is an inaccurate method for percent glenoid bone loss quantification: analysis and techniques for improved accuracy. Arthroscopy 31(4):608–614e1
Boehm E, Minkus M, Moroder P, Scheibel M (2020) Massive graft resorption after iliac crest allograft reconstruction for glenoid bone loss in recurrent anterior shoulder instability. Arch Orthop Trauma Surg 140(7):895–903
Boileau P, Saliken D, Gendre P et al (2019) Arthroscopic Latarjet: suture-button fixation is a safe and reliable alternative to screw fixation. Arthroscopy 35(4):1050–1061
Burkhart SS, De Beer JF (2000) Traumatic glenohumeral bone defects and their relationship to failure of arthroscopic Bankart repairs: significance of the inverted-pear glenoid and the humeral engaging Hill-Sachs lesion. Arthroscopy 16(7):677–694
Bushnell BD, Creighton RA, Herring MM (2008) Bony instability of the shoulder. Arthroscopy 24(9):1061–1073
Butt U, Charalambous CP (2012) Complications associated with open coracoid transfer procedures for shoulder instability. J Shoulder Elbow Surg 21(8):1110–1119
Cho NS, Yoo JH, Rhee YG (2016) Management of an engaging Hill-Sachs lesion: arthroscopic remplissage with Bankart repair versus Latarjet procedure. Knee Surg Sports Traumatol Arthrosc 24(12):3793–3800
Degen RM, Giles JW, Johnson JA, Athwal GS (2014) Remplissage versus latarjet for engaging Hill-Sachs defects without substantial glenoid bone loss: a biomechanical comparison. Clin Orthop Relat Res 472(8):2363–2371
Di Giacomo G, de Gasperis N, Costantini A et al (2014) Does the presence of glenoid bone loss influence coracoid bone graft osteolysis after the Latarjet procedure? A computed tomography scan study in 2 groups of patients with and without glenoid bone loss. J Shoulder Elbow Surg 23(4):514–518
Di Giacomo G, Itoi E, Burkhart SS (2014) Evolving concept of bipolar bone loss and the Hill-Sachs lesion: from “engaging/non-engaging” lesion to “on-track/off-track” lesion. Arthroscopy 30(1):90–98
Di Giacomo G, Peebles LA, Pugliese M et al (2020) Glenoid track instability management score: radiographic modification of the instability severity index score. Arthroscopy 36(1):56–67
Frost HM (1987) Bone “mass” and the “mechanostat”: a proposal. Anat Rec 219(1):1–9
LJt G, Walia P, Patel RM et al (2016) Stability of the Glenohumeral joint with combined humeral head and Glenoid defects: a cadaveric study. Am J Sports Med 44(4):933–940
Hardy A, Sabatier V, Schoch B et al (2019) Latarjet with cortical button fixation is associated with an increase of the risk of recurrent dislocation compared to screw fixation. Knee Surg Sports Traumatol Arthrosc 28(7):2354–2360
Hughes JL, Bastrom T, Pennock AT, Edmonds EW (2018) Arthroscopic Bankart repairs with and without remplissage in recurrent adolescent anterior shoulder instability with Hill-Sachs deformity. Orthop J Sports Med 6(12):2325967118813981
Itoi E, Lee SB, Berglund LJ, Berge LL, An KN (2000) The effect of a glenoid defect on anteroinferior stability of the shoulder after Bankart repair: a cadaveric study. J Bone Joint Surg Am 82(1):35–46
Kim SJ, Kim SH, Park BK, Chun YM (2014) Arthroscopic stabilization for recurrent shoulder instability with moderate glenoid bone defect in patients with moderate to low functional demand. Arthroscopy 30(8):921–927
Liu JN, Gowd AK, Garcia GH et al (2018) Recurrence rate of instability after remplissage for treatment of traumatic anterior shoulder instability: a systematic review in treatment of subcritical Glenoid Bone loss. Arthroscopy 34(10):2894–2907.e2 (e2892)
Moroder P, Blocher M, Auffarth A et al (2014) Clinical and computed tomography-radiologic outcome after bony glenoid augmentation in recurrent anterior shoulder instability without significant glenoid bone loss. J Shoulder Elbow Surg 23(3):420–426
Moroder P, Damm P, Wierer G et al (2019) Challenging the current concept of critical glenoid Bone loss in shoulder instability: does the size measurement really tell it all? Am J Sports Med 47(3):688–694
Moroder P, Danzinger V, Maziak N et al (2020) Characteristics of functional shoulder instability. J Shoulder Elbow Surg 29(1):68–78
Moroder P, Ernstbrunner L, Pomwenger W et al (2015) Anterior shoulder instability is associated with an underlying deficiency of the bony Glenoid concavity. Arthroscopy 31(7):1223–1231
Moroder P, Hirzinger C, Lederer S et al (2012) Restoration of anterior glenoid bone defects in posttraumatic recurrent anterior shoulder instability using the J‑bone graft shows anatomic graft remodeling. Am J Sports Med 40(7):1544–1550
Moroder P, Schulz E, Wierer G et al (2019) Neer Award 2019: latarjet procedure vs. iliac crest bone graft transfer for treatment of anterior shoulder instability with glenoid bone loss: a prospective randomized trial. J Shoulder Elbow Surg 28(7):1298–1307
Murphy AI, Hurley ET, Hurley DJ, Pauzenberger L, Mullett H (2019) Long-term outcomes of the arthroscopic Bankart repair: a systematic review of studies at 10-year follow-up. J Shoulder Elbow Surg 28(11):2084–2089
Nofsinger C, Browning B, Burkhart SS, Pedowitz RA (2011) Objective preoperative measurement of anterior glenoid bone loss: a pilot study of a computer-based method using unilateral 3‑dimensional computed tomography. Arthroscopy 27(3):322–329
Pandey V, Gangadharaiah L, Madi S et al (2020) A retrospective cohort analysis of arthroscopic Bankart repair with or without remplissage in patients with off-track Hill-Sachs lesion evaluated for functional outcomes, recurrent instability, and range of motion. J Shoulder Elbow Surg 29(2):273–281
Provencher MT, Frank RM, Golijanin P et al (2017) Distal tibia allograft Glenoid reconstruction in recurrent anterior shoulder instability: clinical and radiographic outcomes. Arthroscopy 33(5):891–897
Shaha JS, Cook JB, Rowles DJ et al (2016) Clinical validation of the glenoid track concept in anterior Glenohumeral instability. J Bone Joint Surg Am 98(22):1918–1923
Shaha JS, Cook JB, Song DJ et al (2015) Redefining “critical” bone loss in shoulder instability: functional outcomes worsen with “Subcritical” bone loss. Am J Sports Med 43(7):1719–1725
Tauber M, Resch H, Forstner R, Raffl M, Schauer J (2004) Reasons for failure after surgical repair of anterior shoulder instability. J Shoulder Elbow Surg 13(3):279–285
Yamamoto N, Itoi E, Abe H et al (2009) Effect of an anterior glenoid defect on anterior shoulder stability: a cadaveric study. Am J Sports Med 37(5):949–954
Yamamoto N, Muraki T, Sperling JW et al (2010) Stabilizing mechanism in bone-grafting of a large glenoid defect. J Bone Joint Surg Am 92(11):2059–2066
Yang JS, Mehran N, Mazzocca AD et al (2018) Remplissage versus modified Latarjet for off-track Hill-Sachs lesions with subcritical glenoid bone loss. Am J Sports Med 46(8):1885–1891
Zacchilli MA, Owens BD (2010) Epidemiology of shoulder dislocations presenting to emergency departments in the United States. J Bone Joint Surg Am 92(3):542–549
Zimmermann SM, Scheyerer MJ, Farshad M et al (2016) Long-term restoration of anterior shoulder stability: a retrospective analysis of arthroscopic Bankart repair versus open Latarjet procedure. J Bone Joint Surg Am 98(23):1954–1961
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
P. Moroder declares that he has no competing interests.
For this article no studies with human participants or animals were performed by the author. All studies performed were in accordance with the ethical standards indicated in each case.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Moroder, P. State-of-the art treatment of bony defects in anterior shoulder instability—the European perspective. Obere Extremität 16, 22–26 (2021). https://doi.org/10.1007/s11678-020-00618-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11678-020-00618-5