Abstract
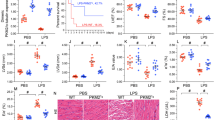
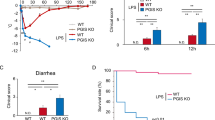
Septic shock leads to myocardial dysfunction and induces inflammation. Nod-like receptor family pyrin domain-containing 3 (NLRP3) inflammasomes are involved in inflammation, and gastrodin can inhibit the activity of inflammasomes. Our study aimed to explore the effect of gastrodin against septic shock–induced injury through inhibiting NLRP3. Before establishing septic shock mice model, the mice were injected with gastrodin of various concentrations. The cardiac function of mice was detected by a PowerLab, and the histopathological changes of mouse myocardial tissues were detected by hematoxylin-eosin staining. Apoptosis of cardiomyocytes from mice was detected by TUNEL assay, and IL-1β concentration was detected by enzyme-linked immunosorbent assay. After culture in vitro and treatment with gastrodin, lipopolysaccharide (LPS), and NLRP3 vector, the cell viability and apoptosis of cardiomyocytes were detected by cell counting kit-8 and flow cytometry respectively. Besides, the expressions of NLRP3, Caspase-1, IL-1β, Bax, and Bcl-2 in mouse myocardial tissue or cultured cardiomyocytes were detected by Western blot. Gastrodin improved survival and promoted the recovery of cardiac function in septic shock mice, as it reversed the abnormality of left ventricular function indices in septic shock mice. Besides, gastrodin decreased IL-1β concentration and apoptosis in myocardial tissues of septic shock mice and decreased apoptosis and increased cell viability in LPS-induced cardiomyocytes. In addition, gastrodin downregulated NLRP3, Caspase-1, IL-1β, and Bax expressions and upregulated Bcl-2 expression in myocardial tissues of septic shock mice and LPS-induced cardiomyocytes. NLRP3 overexpression reversed the effect of gastrodin on LPS-induced cardiomyocytes. Gastrodin promoted cardiac function recovery and protected cardiomyocytes against septic shock–induced injury by regulating NLRP3.




Similar content being viewed by others
References
Bahar T et al (2017) Inhibition of NLRP3 inflammasome contributes to protective effect of 5,14-HEDGE against lipopolysaccharide-induced septic shock. Int J Pharmacol 13:654–666
Dai JN et al (2011) Gastrodin inhibits expression of inducible NO synthase, cyclooxygenase-2 and proinflammatory cytokines in cultured LPS-stimulated microglia via MAPK pathways. PLoS One 6:e21891. https://doi.org/10.1371/journal.pone.0021891
Dargent A et al (2018) Vasopressor cumulative dose requirement and risk of early death during septic shock: an analysis from the EPISS cohort. Shock 49:625–630. https://doi.org/10.1097/shk.0000000000001022
D'Orsi B et al (2017) Control of mitochondrial physiology and cell death by the Bcl-2 family proteins Bax and Bok. Neurochem Int 109:162–170. https://doi.org/10.1016/j.neuint.2017.03.010
Du RH et al (2019) The pore-forming subunit Kir6.1 of the K-ATP channel negatively regulates the NLRP3 inflammasome to control insulin resistance by interacting with NLRP3. Exp Mol Med 51:1–13. https://doi.org/10.1038/s12276-019-0291-6
Edlich F (2018) BCL-2 proteins and apoptosis: recent insights and unknowns. Biochem Biophys Res Commun 500:26–34. https://doi.org/10.1016/j.bbrc.2017.06.190
Esposito S et al (2017) Sepsis and septic shock: new definitions, new diagnostic and therapeutic approaches. J Glob Antimicrob Resist 10:204–212. https://doi.org/10.1016/j.jgar.2017.06.013
Falk L et al (2019) Extracorporeal membrane oxygenation for septic shock. Crit Care Med 47:1097–1105. https://doi.org/10.1097/ccm.0000000000003819
Fu S et al (2018) Gastrodin pretreatment alleviates myocardial ischemia/reperfusion injury through promoting autophagic flux. Biochem Biophys Res Commun 503:2421–2428. https://doi.org/10.1016/j.bbrc.2018.06.171
Hong Y et al (2019) The neuroprotection of progesterone against Aβ-induced NLRP3-Caspase-1 inflammasome activation via enhancing autophagy in astrocytes. Int Immunopharmacol 74:105669. https://doi.org/10.1016/j.intimp.2019.05.054
Jain S (2018) Sepsis: an update on current practices in diagnosis and management. Am J Med Sci 356:277–286. https://doi.org/10.1016/j.amjms.2018.06.012
Kakihana Y et al (2016) Sepsis-induced myocardial dysfunction: pathophysiology and management. J Intensive Care 4:22. https://doi.org/10.1186/s40560-016-0148-1
Korneev KV (2019) Mouse Models of Sepsis and Septic Shock. Mol Biol (Mosk) 53:799–814. https://doi.org/10.1134/s0026898419050100
Li X et al (2018) Gastrodin protects myocardial cells against hypoxia/reoxygenation injury in neonatal rats by inhibiting cell autophagy through the activation of mTOR signals in PI3K-Akt pathway. J Pharm Pharmacol 70:259–267. https://doi.org/10.1111/jphp.12838
Lipinska-Gediga M (2016) Sepsis and septic shock-is a microcirculation a main player? Anaesthesiol Intensive Ther 48:261–265. https://doi.org/10.5603/AIT.a2016.0037
Livak KJ et al (2001) Analysis of relative gene expression data using real-time quantitative PCR and the 2(-Delta Delta C(T)) Method. Methods 25:402–408. https://doi.org/10.1006/meth.2001.1262
Maes M et al (2016) Experimental models of hepatotoxicity related to acute liver failure. Toxicol Appl Pharmacol 290:86–97. https://doi.org/10.1016/j.taap.2015.11.016
Napolitano LM (2018) Sepsis 2018: Definitions and guideline changes. Surg Infect 19:117–125. https://doi.org/10.1089/sur.2017.278
Nemzek JA et al (2008) Modeling sepsis in the laboratory: merging sound science with animal well-being. Comp Med 58:120–128
Pellegrini C et al. (2019) Phytochemicals as novel therapeutic strategies for NLRP3 inflammasome-related neurological, metabolic, and inflammatory diseases. Int J Mol Sci 20:2876. https://doi.org/10.3390/ijms20122876
Płóciennikowska A et al (2015) Co-operation of TLR4 and raft proteins in LPS-induced pro-inflammatory signaling. Cell Mol Life Sci 72:557–581. https://doi.org/10.1007/s00018-014-1762-5
Rathinam VAK et al (2019) Innate immunity to intracellular LPS. Nat Immunol 20:527–533. https://doi.org/10.1038/s41590-019-0368-3
Santos-Junior MN et al (2018) Ureaplasma diversum and its membrane-associated lipoproteins activate inflammatory genes through the NF-κB pathway via toll-like receptor 4. Front Microbiol 9:1538. https://doi.org/10.3389/fmicb.2018.01538
Seymour CW et al (2015) Septic shock: advances in diagnosis and treatment. Jama 314:708–717. https://doi.org/10.1001/jama.2015.7885
Shao A et al. (2020) Chikusetsu saponin IVa alleviated sevoflurane-induced neuroinflammation and cognitive impairment by blocking NLRP3/caspase-1 pathway. Pharmacol Rep 72:833–845. https://doi.org/10.1007/s43440-020-00078-2
Sun W et al (2019) Gastrodin ameliorates microvascular reperfusion injury-induced pyroptosis by regulating the NLRP3/caspase-1 pathway. J Physiol Biochem 75:531–547. https://doi.org/10.1007/s13105-019-00702-7
Tianyuan Y et al (2018) Gastrodin alleviates cognitive dysfunction and depressive-like behaviors by inhibiting ER stress and NLRP3 inflammasome activation in db/db mice. Int J Mol Sci 19:3977. https://doi.org/10.3390/ijms19123977
Vallabhajosyula S et al (2018) Basic and advanced echocardiographic evaluation of myocardial dysfunction in sepsis and septic shock. Anaesth Intensive Care 46:13–24. https://doi.org/10.1177/0310057x1804600104
Vasques-Nóvoa F et al (2018) MicroRNA-155 Amplifies Nitric Oxide/cGMP Signaling and Impairs Vascular Angiotensin II Reactivity in Septic Shock. Crit Care Med 46:e945–e954. https://doi.org/10.1097/ccm.0000000000003296
Wang Z et al (2019) Cardamonin from a medicinal herb protects against LPS-induced septic shock by suppressing NLRP3 inflammasome. Acta Pharm Sin B 9:734–744. https://doi.org/10.1016/j.apsb.2019.02.003
Wu P et al (2019) MicroRNA-494-3p protects rat cardiomyocytes against septic shock via PTEN. Exp Ther Med 17:1706–1716. https://doi.org/10.3892/etm.2018.7116
Yang P et al (2013) Gastrodin attenuation of the inflammatory response in H9c2 cardiomyocytes involves inhibition of NF-κB and MAPKs activation via the phosphatidylinositol 3-kinase signaling. Biochem Pharmacol 85:1124–1133. https://doi.org/10.1016/j.bcp.2013.01.020
Yu YJ et al (2018) Intermedin1-53 protects cardiac function in rats with septic shock via inhibiting oxidative stress and cardiomyocyte apoptosis. Eur Rev Med Pharmacol Sci 22:2906–2913. https://doi.org/10.26355/eurrev_201805_14993
Zeng N et al (2017) Brain-derived neurotrophic factor attenuates septic myocardial dysfunction via eNOS/NO pathway in rats. Oxidative Med Cell Longev 2017:1721434. https://doi.org/10.1155/2017/1721434
Zhang Q et al (2008) Effects of gastrodin injection on blood pressure and vasoactive substances in treatment of old patients with refractory hypertension: a randomized controlled trial. Zhong Xi Yi Jie He Xue Bao 6:695–699. https://doi.org/10.3736/jcim20080707
Zhang ZS et al (2019) Role of resveratrol in protecting vasodilatation function in septic shock rats and its mechanism. J Trauma Acute Care Surg 87:1336–1345. https://doi.org/10.1097/ta.0000000000002466
Zusso M et al (2019) Ciprofloxacin and levofloxacin attenuate microglia inflammatory response via TLR4/NF-kB pathway. J Neuroinflammation 16:148. https://doi.org/10.1186/s12974-019-1538-9
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Editor: Tetsuji Okamoto
Supplementary information
Supplementary figure 1.
A whole section of cardiac muscle (H&E staining) after LPS injection. (PNG 1747 kb)
Rights and permissions
About this article
Cite this article
Shao, F., Zhou, L., Zhang, Y. et al. Gastrodin alleviates inflammatory injury of cardiomyocytes in septic shock mice via inhibiting NLRP3 expression. In Vitro Cell.Dev.Biol.-Animal 57, 571–581 (2021). https://doi.org/10.1007/s11626-021-00593-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11626-021-00593-3