Abstract
Background
This study investigated the impact and short-term surgical outcomes of two different main energy devices for robotic gastrectomy for gastric cancer. The outcomes of robotic gastrectomy with ultrasonic shears and those of robotic gastrectomy with conventional forceps were compared.
Methods
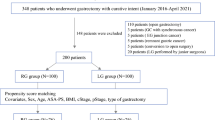
We retrospectively evaluated 171 patients who underwent robotic distal gastrectomy or total gastrectomy for gastric cancer. We classified patients into the ultrasonic shears (US) and Maryland bipolar (MB) forceps groups according to the main energy device used for robotic gastrectomy.
Results
We extracted 58 patients from the US group and 58 patients from the MB forceps groups using propensity score matching. The total console time (310 min [interquartile range (IQR), 253–369 min] and 332 min, [IQR, 294–429 min]; p = 0.022) and the console time to gastrectomy (222 min [IQR, 177–266 min] and 247 min [IQR, 208–321 min]; p = 0.004) were significantly shorter in the US group than in the MB forceps group. Less blood loss occurred in the US group than in the MB forceps group (20 mL [IQR, 10–40 mL] and 30 mL [IQR, 16–80 mL]; p = 0.014). The postoperative complication rate and postoperative hospital stay length were similar between groups. A multivariate multiple linear regression analysis demonstrated that the use of an ultrasonically activated device was one an independent factor that reduced the operative time of robotic gastrectomy.
Conclusion
Using ultrasonic shears as the main energy device may contribute to better surgical outcomes after robotic gastrectomy for gastric cancer.





Similar content being viewed by others
Abbreviations
- LG:
-
Laparoscopic gastrectomy
- RG:
-
Robotic gastrectomy
- US:
-
Ultrasonic shears
- MB:
-
Maryland bipolar
- DB:
-
Double bipolar
- PS:
-
Performance status
- DG:
-
Distal gastrectomy
- TG:
-
Total gastrectomy
References
Terashima M, Tokunaga M, Tanizawa Y, Bando E, Kawamura T, Miki Y et al. Robotic surgery for gastric cancer. Gastric Cancer. 2015;18(3):449-57. https://doi.org/10.1007/s10120-015-0501-4.
Song J, Oh SJ, Kang WH, Hyung WJ, Choi SH, Noh SH. Robot-assisted gastrectomy with lymph node dissection for gastric cancer: lessons learned from an initial 100 consecutive procedures. Ann Surg. 2009;249(6):927-32. https://doi.org/10.1097/01.sla.0000351688.64999.73.
Lu J, Zheng CH, Xu BB, Xie JW, Wang JB, Lin JX et al. Assessment of Robotic Versus Laparoscopic Distal Gastrectomy for Gastric Cancer: A Randomized Controlled Trial. Ann Surg. 2021;273(5):858-67. https://doi.org/10.1097/SLA.0000000000004466.
Kinoshita T, Sato R, Akimoto E, Tanaka Y, Okayama T, Habu T. Reduction in postoperative complications by robotic surgery: a case-control study of robotic versus conventional laparoscopic surgery for gastric cancer. Surg Endosc. 2022;36(3):1989-98. https://doi.org/10.1007/s00464-021-08483-1.
Kubo N, Sakurai K, Tamamori Y, Fukui Y, Kuroda K, Aomatsu N et al. Less Severe Intra-Abdominal Infections in Robotic Surgery for Gastric Cancer Compared with Conventional Laparoscopic Surgery: A Propensity Score-matched Analysis. Ann Surg Oncol. 2022;29(6):3922-33. https://doi.org/10.1245/s10434-022-11410-w.
Liu H, Kinoshita T, Tonouchi A, Kaito A, Tokunaga M. What are the reasons for a longer operation time in robotic gastrectomy than in laparoscopic gastrectomy for stomach cancer? Surg Endosc. 2019;33(1):192-8. https://doi.org/10.1007/s00464-018-6294-x.
Uyama I, Kanaya S, Ishida Y, Inaba K, Suda K, Satoh S. Novel integrated robotic approach for suprapancreatic D2 nodal dissection for treating gastric cancer: technique and initial experience. World J Surg. 2012;36(2):331-7. https://doi.org/10.1007/s00268-011-1352-8.
Hyung WJ, Woo Y, Noh SH. Robotic surgery for gastric cancer: a technical review. J Robot Surg. 2011;5(4):241-9. https://doi.org/10.1007/s11701-011-0263-x.
Okabe H, Obama K, Tsunoda S, Matsuo K, Tanaka E, Hisamori S et al. Feasibility of robotic radical gastrectomy using a monopolar device for gastric cancer. Surg Today. 2019;49(10):820-7. https://doi.org/10.1007/s00595-019-01802-z.
Inoue K, Nakane Y, Michiura T, Yamada M, Mukaide H, Fukui J et al. Ultrasonic scalpel for gastric cancer surgery: a prospective randomized study. J Gastrointest Surg. 2012;16(10):1840-6. https://doi.org/10.1007/s11605-012-1970-y.
Dindo D, Demartines N, Clavien PA. Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg. 2004;240(2):205-13. https://doi.org/10.1097/01.sla.0000133083.54934.ae.
Nishi M, Shimada M, Yoshikawa K, Tokunaga T, Kashihara H, Takasu C et al. Advantages of the Left-handed Ultrasonic Shears Technique for Robotic Gastrectomy. Surg Laparosc Endosc Percutan Tech. 2021;31(4):497-501. https://doi.org/10.1097/SLE.0000000000000923.
Hikage M, Tokunaga M, Makuuchi R, Tanizawa Y, Bando E, Kawamura T et al. Impact of an Ultrasonically Activated Device in Robot-Assisted Distal Gastrectomy. Innovations (Phila). 2017;12(6):453-8. https://doi.org/10.1097/IMI.0000000000000437.
Song J, Kang WH, Oh SJ, Hyung WJ, Choi SH, Noh SH. Role of robotic gastrectomy using da Vinci system compared with laparoscopic gastrectomy: initial experience of 20 consecutive cases. Surg Endosc. 2009;23(6):1204-11. https://doi.org/10.1007/s00464-009-0351-4.
Lee J, Kim YM, Woo Y, Obama K, Noh SH, Hyung WJ. Robotic distal subtotal gastrectomy with D2 lymphadenectomy for gastric cancer patients with high body mass index: comparison with conventional laparoscopic distal subtotal gastrectomy with D2 lymphadenectomy. Surg Endosc. 2015;29(11):3251-60. https://doi.org/10.1007/s00464-015-4069-1.
Shibasaki S, Suda K, Kadoya S, Ishida Y, Nakauchi M, Nakamura K et al. The safe performance of robotic gastrectomy by second-generation surgeons meeting the operating surgeon's criteria in the Japan Society for Endoscopic Surgery guidelines. Asian J Endosc Surg. 2022;15(1):70-81. https://doi.org/10.1111/ases.12967.
Kumamoto T, Ishida Y, Igeta M, Hojo Y, Nakamura T, Kurahashi Y et al. Potential advantages of robotic total gastrectomy for gastric cancer: a retrospective comparative cohort study. J Robot Surg. 2021. https://doi.org/10.1007/s11701-021-01328-y.
Japanese Gastric Cancer A. Japanese classification of gastric carcinoma: 3rd English edition. Gastric Cancer. 2011;14(2):101–12. https://doi.org/10.1007/s10120-011-0041-5.
Author information
Authors and Affiliations
Contributions
Study conception and design: KK and NK.
Methodology: KK and NK.
Acquisition of data: KK, NK, KS, YT, TH, KY, SK, YF, NA, TN, AT, KM.
Analysis and interpretation of data: KK.
Resources: KK, NK, KS, YT, TH, KY, SK, YF, NA, TN, AT, KM.
Supervision: KM.
Drafting manuscript: KK.
Drafting and revisiting manuscript: NK.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kuroda, K., Kubo, N., Sakurai, K. et al. Comparison of Short-Term Surgical Outcomes of Two Types of Robotic Gastrectomy for Gastric Cancer: Ultrasonic Shears Method Versus the Maryland Bipolar Forceps Method. J Gastrointest Surg 27, 222–232 (2023). https://doi.org/10.1007/s11605-022-05527-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-022-05527-2