Abstract
Background
The use of laparoscopic liver resection (LLR) is widespread owing to its several advantages, especially smaller incision (Kaneko et al., Ann Gastroenterol Surg 1:33–43, 1; Ciria et al., Surg Endosc 34:349–360, 2). However, both posterior sectionectomy and donor hepatectomy are extremely difficult procedures to perform in LLR (Hasegawa et al., Ann Gastroenterol Surg 2:376–382, 3; Soubrane and Kwon, J Hepatobiliary Pancreat Sci 24:E1–E5, 4; Takahara et al., Transplantation 101:1628–1636, 5; Lee et al., Clin Transplant 33:e13683, 6; Hong et al., Surg Endosc 33:3741–3748, 7; Rhu et al., J Hepatobiliary Pancreat Sci 27:16–25, 8). Moreover, the right posterior section graft procurement is also difficult even in open laparotomy procedure (Sugawara et al., Transplantation 73:111–114, 9; Hwang et al., Liver Transpl 10:1150–1155, 10; Hori, Kirino, and Uemoto, Hepatol Res 45:1076–1082, 11; Kusakabe et al., Liver Transpl 26:299–303, 12). The pure laparoscopic donor posterior sectionectomy has not been reported yet. Therefore, we aimed to introduce a novel procedure through a video clip.
Methods
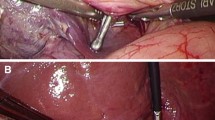
The donor was placed in the semi-left lateral decubitus position with the reverse Trendelenburg position using a bean bag device. The right liver was mobilized, and the right hepatic vein was exposed. To adopt the liver hanging maneuver, a tape was inserted between the middle and right hepatic veins along the inferior vena cava. The posterior Glissonean pedicle was encircled and controlled, and the liver parenchyma was completely transected using the liver hanging maneuver. The vessels to the posterior section were respectively isolated. The posterior branches of the hepatic duct, hepatic artery, and portal vein were cut. The right hepatic vein was divided, and the graft liver was retrieved via a suprapubic incision. This study was approved by institutional ethics board (No. MH2019-119), and informed consent was taken from the patient.
Results
The overall surgical time was 503 min, and the blood loss was 400 mL. No complications were observed, and the donor was discharged from the hospital on postoperative day 11.
Conclusion
This is the first report of pure laparoscopic donor hepatectomy of the posterior section graft. This procedure is more difficult than other laparoscopic donor hepatectomies because it involves parenchymal transection in the right intersectional plane and dissection of the posterior branches of hilar vessels.
Similar content being viewed by others
References
Kaneko H, Otsuka Y, Kubota Y, Wakabayashi G. Evolution and revolution of laparoscopic liver resection in Japan. Ann Gastroenterol Surg 2017;1: 33–43.
Ciria R, Ocana S, Gomez-Luque I, Cipriani F, Halls M, Fretland AA, Okuda Y, Aroori S, Briceno J, Aldrighetti L, Edwin B, Hilal MA. A systematic review and meta-analysis comparing the short- and long-term outcomes for laparoscopic and open liver resections for liver metastases from colorectal cancer. Surg Endosc 2020;34: 349–360.
Hasegawa Y, Nitta H, Takahara T, Katagiri H, Kanno S, Otsuka K, Sasaki A. Laparoscopic left hemihepatectomy is suitable as a first step in pure laparoscopic major hepatectomy. Ann Gastroenterol Surg 2018;2: 376–382.
Soubrane O, Kwon CH. Tips for pure laparoscopic right hepatectomy in the live donor. J Hepatobiliary Pancreat Sci 2017;24: E1-E5.
Takahara T, Wakabayashi G, Nitta H, Hasegawa Y, Katagiri H, Umemura A, Takeda D, Makabe K, Otsuka K, Koeda K, Sasaki A. The First Comparative Study of the Perioperative Outcomes Between Pure Laparoscopic Donor Hepatectomy and Laparoscopy-Assisted Donor Hepatectomy in a Single Institution. Transplantation 2017;101: 1628–1636.
Lee B, Choi Y, Han HS, Yoon YS, Cho JY, Kim S, Kim KH, Hyun IG. Comparison of pure laparoscopic and open living donor right hepatectomy after a learning curve. Clin Transplant 2019;33: e13683.
Hong SK, Suh KS, Yoon KC, Lee JM, Cho JH, Yi NJ, Lee KW. The learning curve in pure laparoscopic donor right hepatectomy: a cumulative sum analysis. Surg Endosc 2019;33: 3741–3748.
Rhu J, Choi GS, Kim JM, Joh JW, Kwon CHD. Feasibility of total laparoscopic living donor right hepatectomy compared with open surgery: comprehensive review of 100 cases of the initial stage. J Hepatobiliary Pancreat Sci 2020;27: 16–25.
Sugawara Y, Makuuchi M, Takayama T, Imamura H, Kaneko J. Right lateral sector graft in adult living-related liver transplantation. Transplantation 2002;73: 111–114.
Hwang S, Lee SG, Lee YJ, Park KM, Kim KH, Ahn CS, Sung KB, Moon DB, Ha TY, Kim KK, Kim YD. Donor selection for procurement of right posterior segment graft in living donor liver transplantation. Liver Transpl 2004;10: 1150–1155.
Hori T, Kirino I, Uemoto S. Right posterior segment graft in living donor liver transplantation. Hepatol Res 2015;45: 1076–1082.
Kusakabe J, Yagi S, Okamura Y, Iida T, Ogawa E, Ito T, Hata K, Taura K, Okajima H, Kaido T, Uemoto S. Anatomical Pitfall in Right Posterior Sector Graft Procurement in Living Donor Liver Transplantation. Liver Transpl 2020;26: 299–303.
Acknowledgments
We would like to thank the staff of the Department of Anesthesiology, Iwate Medical University, for their assistance. We would like to thank Editage (www.editage.com) for English language editing.
Author information
Authors and Affiliations
Contributions
Conception and design: all authors; data analysis and interpretation: YH; drafting: YH; revising: all authors; final approval of manuscript: all authors; agreement to be accountable for all aspects of the work: all authors.
Corresponding author
Ethics declarations
This study was approved by institutional ethics board (No. MH2019-119), and informed consent was taken from the patient.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic Supplementary Material
(MP4 155,365 kb).
Rights and permissions
About this article
Cite this article
Hasegawa, Y., Nitta, H., Takahara, T. et al. Pure Laparoscopic Donor Hepatectomy: Right Posterior Section Graft. J Gastrointest Surg 25, 2718–2719 (2021). https://doi.org/10.1007/s11605-020-04571-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-020-04571-0