Abstract
Background
In the revised Japanese and Worldwide TNM classification of distal bile duct cancer, the lymph node status is defined as N0 or N1 without reference to the tumor location or extent, according to the presence/absence of metastasis to the regional lymph nodes.
Methods
Data of 94 patients with distal bile duct cancer who had undergone pancreaticoduodenectomy were reviewed retrospectively. In formalin-fixed specimens, we measured the longitudinal lengths from the papilla to the lower and upper margins of the tumor, in order to investigate the correlation of the tumor extent with the likely sites of nodal metastasis.
Results
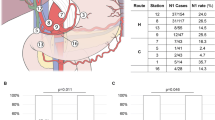
The frequencies of metastasis to the posterior pancreaticoduodenal nodes (7.1 %) and superior mesenteric artery nodes (0.0 %) were significantly lower in the cases in which the length from the papilla to the lower margin of the tumor was ≥30 mm. The frequencies of nodal metastasis to the common hepatic artery nodes (0.0 %) and hepatoduodenal ligament nodes (6.7 %) were significantly lower in the cases in which the length from the papilla to the upper margin was <40 mm.
Conclusion
The likely sites of nodal metastasis differ according to the extent of the tumor in cases of bile duct cancer.






Similar content being viewed by others
References
The Japanese Society of Hepato-Biliary-Pancreatic Surgery (JSHBPS). General Rules for Clinical and Pathological Studies on Cancer of the Biliary Tract (2013). 6 ed.
International Union Against Cancer (UICC). TNM Classification of Malignant Tumors (2009). 7 ed, Wiley-Liss, New York.
Kayahara M, Nagakawa T, Ueno K, Ohta T, Takeda T, Miyazaki I Lymphatic flow in carcinoma of the distal bile duct based on a clinicopathologic study. Cancer. 1993; 72: 2112–7.
Kurosaki I, Tsukada K, Hatakeyama K, Muto T The mode of lymphatic spread in carcinoma of the bile duct. American Journal of Surgery. 1996; 172: 239–43.
Nakao A, Harada A, Nonami T, Kaneko T, Murakami H, Inoue S, et al. Lymph node metastases in carcinoma of the head of the pancreas region. The British Journal of Surgery. 1995; 82: 399–402.
Yoshida T, Matsumoto T, Sasaki A, Morii Y, Aramaki M, Kitano S Prognostic factors after pancreatoduodenectomy with extended lymphadenectomy for distal bile duct cancer. Arch Surg. 2002; 137: 69–73.
Yoshida T, Matsumoto T, Sasaki A, Morii Y, Shibata K, Ishio T, et al. Lymphatic spread differs according to tumor location in extrahepatic bile duct cancer. Hepato-gastroenterology. 2003; 50: 17–20.
Bosman FT, Carneiro F, Hruban RH, Theise ND, eds. WHO Classification of Tumours of the Digestive System, Fourth Edition. Lyon: IARC Press; 2010.
Sobin LH, Wittekind C, eds. TNM Classification of Malignant Tumours, 6th edition. New York: Wiley-Liss; 2002.
Shaw MJ, Dorsher PJ, Vennes JA Cystic duct anatomy: an endoscopic perspective. The American Journal of Gastroenterology. 1993; 88: 2102–6.
Tsunoda M, Sasai N, Mitsumori A, Akaki A, Togami I, Jyoya I, et al. Evaluation of the Cystic Duct and Cysticohepatic Junction with MR Cholangiography: Comparison of various techniques and clinical evaluation with respiratory-trrigaered three-dimensional multislab technique. Nippon Acta Radiologica. 1998; 58: 420–5.
Nagakawa T, Konishi I, Ueno K, Ohta T, Kayahara M A clinical study on lymphatic flow in carcinoma of the pancreatic head area—peripancreatic regional lymph node grouping. Hepato-gastroenterology. 1993; 40: 457–62.
Lee HG, Lee SH, Yoo DD, Paik KY, Heo JS, Choi SH, et al. Carcinoma of the middle bile duct: is bile duct segmental resection appropriate? World Journal of Gastroenterology : WJG. 2009; 15: 5966–71.
Sakamoto Y, Shimada K, Nara S, Esaki M, Ojima H, Sano T, et al. Surgical management of infrahilar/suprapancreatic cholangiocarcinoma: an analysis of the surgical procedures, surgical margins, and survivals of 77 patients. Journal of Gastrointestinal Surgery : official journal of the Society for Surgery of the Alimentary Tract. 2010; 14: 335–43.
Akamatsu N, Sugawara Y, Osada H, Okada T, Itoyama S, Komagome M, et al. Preoperative evaluation of the longitudinal spread of extrahepatic bile duct cancer using multidetector computed tomography. Journal of Hepato-biliary-pancreatic Surgery. 2009; 16: 216–22.
Park HS, Lee JM, Choi JY, Lee MW, Kim HJ, Han JK, et al. Preoperative evaluation of bile duct cancer: MRI combined with MR cholangiopancreatography versus MDCT with direct cholangiography. AJR American Journal of Roentgenology. 2008; 190: 396–405.
Unno M, Okumoto T, Katayose Y, Rikiyama T, Sato A, Motoi F, et al. Preoperative assessment of hilar cholangiocarcinoma by multidetector row computed tomography. Journal of Hepato-biliary-pancreatic Surgery. 2007; 14: 434–40.
Acknowledgments
No special comments.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Source of Financial Support
None
Conflict of Interest
Nothing to declare
Additional information
Rights and permissions
About this article
Cite this article
Kato, Y., Takahashi, S., Gotohda, N. et al. The Likely Sites of Nodal Metastasis Differs According to the Tumor Extent in Distal Bile Duct Cancer. J Gastrointest Surg 20, 1618–1627 (2016). https://doi.org/10.1007/s11605-016-3179-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-016-3179-y