Abstract
Objective
The objective of this paper is to evaluate the perioperative outcomes of major hepatectomy for intrahepatic cholangiocarcinoma (ICC) in patients with cirrhosis.
Methods
We retrospectively evaluated the preoperative, intraoperative, and postoperative findings in 42 consecutive patients with cirrhosis and in 102 patients with normal livers who underwent major hepatectomy for ICC.
Results
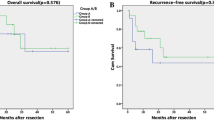
Preoperative liver function was worse in patients with cirrhosis compared to patients without cirrhosis. Cirrhotic patients had significantly higher intraoperative blood loss, longer operation time, and longer hospital stay than non-cirrhotic patients. However, the two groups had similar overall morbidity and hospital mortality rates and similar rates of liver failure or other complications. Their R0 resection rates, resection margin widths and disease-free survival rates were also similar.
Conclusions
Major hepatectomy for ICC can be performed in selected cirrhotic patients with acceptable morbidity and mortality rates, as compared to patients without cirrhosis.


Similar content being viewed by others
References
Khan SA, Taylor-Robinson SD, Toledano MB, Beck A, Elliott P, Thomas HC. Changing international trends in mortality rates for liver, biliary and pancreatic tumours. J Hepatol 2002; 37: 806–13.
Patel T. Worldwide trends in mortality from biliary tract malignancies. BMC Cancer 2002; 2:10.
Shaib Y, El-Serag HB. The epidemiology of cholangiocarcinoma. Semin Liver Dis 2004; 24:115–25.
Parkin DM, Bray F, Ferlay J, Pisani P. Global cancer statistics 2002. CA Cancer J Clin 2002; 55:74–108.
Hou J, Liu Z, Gu F. Epidemiology and prevention of hepatitis B virus infection. Int J Med Sci 2005; 2:50–7.
Pausawasdi A, Watanapa P. Hepatolithiasis: epidemiology and classification. Hepatogastroenterology 1997; 44:314–6.
Chen CC, Yen CH, Wu WY, Hu SW, Chen SC, Bell WR, Lee MC. Epidemiology of hepatitis B virus infection among young adults in Taiwan, China after public vaccination program. Chin Med J (Engl) 2007; 120:1155–8.
Sorensen HT, Friis S, Olsen JH, Thulstrup AM, Mellemkjaer L, Linet M, Trichopoulos D, Vilstrup H, Olsen J. Risk of liver and other types of cancer in patients with cirrhosis: a nationwide cohort study in Denmark. Hepatology 1998; 28:921–5.
Shin HR, Lee CU, Park HJ, Seol SY, Chung JM, Choi HC, Ahn YO, Shigemastu T. Hepatitis B and C virus, Clonorchis sinensis for the risk of liver cancer: a case–control study in Pusan, Korea. Int J Epidemiol 1996; 25:933–40.
Kubo S, Kinoshita H, Hirohashi K, Hamba H. Hepatolithiasis associated with cholangiocarcinoma. World J Surg 1995; 19:637–41.
Okuda K, Nakanuma Y, Miyazaki M. Cholangiocarcinoma: recent progress. Part 1: epidemiology and etiology. J Gastroenterol Hepatol 2002; 17:1049–55.
Li YY, Li H, Lv P, Liu G, Li XR, Tian BN, Chen DJ. Prognostic value of cirrhosis for intrahepatic cholangiocarcinoma after surgical treatment. J Gastrointest Surg. 2011; 15:608–13.
Lang H, Sotiropoulos GC, Frühauf NR, Dömland M, Paul A, Kind EM, Malagó M, Broelsch CE. Extended hepatectomy for intrahepatic cholangiocellular carcinoma (ICC): when is it worthwhile? Single center experience with 27 resections in 50 patients over a 5-year period. Ann Surg 2005; 241:134–43.
Nakagohri T, Kinoshita T, Konishi M, Takahashi S, Gotohda N. Surgical outcome and prognostic factors in intrahepatic cholangiocarcinoma. World J Surg 2008; 32:2675–80.
Shimada K, Sano T, Sakamoto Y, Esaki M, Kosuge T, Ojima H. Clinical impact of the surgical margin status in hepatectomy for solitary mass-forming type intrahepatic cholangiocarcinoma without lymph node metastases. J Surg Oncol 2007; 96:160–5.
Strasberg SM, Belghiti J, Clavien PA, Gadzijev E, Garden JO, Lau WY, Makuuchi M, Strong RW. Terminology Committee of the International Hepato-Pancreato-Biliary Association. The Brisbane 2000 terminology of liver anatomy and resections. HPB 2000; 2:333–9.
Pugh RN, Murray-Lyon IM, Dawson JL, Pietroni MC, Williams R. Transection of the oesophagus for bleeding oesophageal varices. Br J Surg 1973; 60:646–9.
Fan ST, Lai EC, Lo CM, Ng IO, Wong J. Hospital mortality of major hepatectomy for hepatocellular carcinoma associated with cirrhosis. Arch Surg 1995; 130:198–203.
Wiesner R, Edwards E, Freeman R, Harper A, Kim R, Kamath P, Kremers W, Lake J, Howard T, Merion RM, Wolfe RA, Krom R; United Network for Organ Sharing Liver Disease Severity Score Committee. Model for end-stage liver disease (MELD) and allocation of donor livers. Gastroenterology 2003; 124:91–6.
Mayo SC, Shore AD, Nathan H, Edil BH, Hirose K, Anders RA, Wolfgang CL, Schulick RD, Choti MA, Pawlik TM. Refining the definition of perioperative mortality following hepatectomy using death within 90 days as the standard criterion. HPB (Oxford) 2011; 13:473–82.
Thelen A, Benckert C, Tautenhahn HM, Hau HM, Bartels M, Linnemann J, Bertolini J, Moche M, Wittekind C, Jonas S. Liver resection for hepatocellular carcinoma in patients without cirrhosis. Br J Surg 2013; 100:130–7.
Liver Cancer Study Group of Japan. The general rules for the clinical and pathological study of primary liver cancer. Jpn J Surg 1989; 19:98–129.
Meyer CG, Penn I, James L. Liver transplantation for cholangiocarcinoma: results in 207 patients. Transplantation 2000; 69:1633–7.
Teh SH, Christein J, Donohue J, Que F, Kendrick M, Farnell M, Cha S, Kamath P, Kim R, Nagorney DM. Hepatic resection of hepatocellular carcinoma in patients with cirrhosis: Model of End-Stage Liver Disease (MELD) score predicts perioperative mortality. J Gastrointest Surg 2005; 9:1207–15.
Capussotti L, Muratore A, Massucco P, Ferrero A, Polastri R, Bouzari H. Major liver resections for hepatocellular carcinoma on cirrhosis: early and long-term outcomes. Liver Transpl 2004; 10:S64-8.
Schneider PD. Preoperative assessment of liver function. Surg Clin North Am. 2004: 84:355–73.
Clavien PA, Petrowsky H, DeOliveira ML, Graf R. Strategies for safer liver surgery and partial liver transplantation. N Engl J Med 2007; 356:1545–59.
Redaelli CA, Dufour JF, Wagner M, Schilling M, Husler J, Krahenbuhl L, Buchler MW, Reichen J. Preoperative galactose elimination capacity predicts complications and survival after hepatic resection. Ann Surg 2002; 235:77–85.
McCormack L, Petrowsky H, Clavien PA. Surgical therapy of hepatocellular carcinoma. Eur J Gastroenterol Hepatol 2005; 17:497–503.
Poon RT, Fan ST, Lo CM, Liu CL, Lam CM, Yuen WK, Yeung C, Wong J. Extended hepatic resection for hepatocellular carcinoma in patients with cirrhosis: is it justified? Ann Surg 2002; 236:602–11.
Northup PG, Wanamaker RC, Lee VD, Adams RB, Berg CL. Model for end-stage liver disease (MELD) predicts nontransplant surgical mortality in patients with cirrhosis. Ann Surg 2005; 242:244–51.
Befeler AS, Palmer DE, Hoffman M, Longo W, Solomon H, Di Bisceglie AM. The safety of intra-abdominal surgery in patients with cirrhosis: model for end-stage liver disease is superior to Child-Turcotte-Pugh classification in predicting outcome. Arch Surg 2005; 140:650–54.
Cucchetti A, Ercolani G, Vivarelli M, Cescon M, Ravaioli M, La Barba G, Zanello M, Grazi GL, Pinna AD. Impact of model for end-stage liver disease (MELD) score on prognosis after hepatectomy for hepatocellular carcinoma on cirrhosis. Liver Transpl 2006; 12:966–71.
Delis SG, Bakoyiannis A, Biliatis I, Athanassiou K, Tassopoulos N, Dervenis C. Model for end-stage liver disease (MELD) score, as a prognostic factor for post-operative morbidity and mortality in cirrhotic patients, undergoing hepatectomy for hepatocellular carcinoma. HPB (Oxford) 2009; 11:351–7.
Poon RT, Fan ST. Hepatectomy for hepatocellular carcinoma: patient selection and postoperative outcome. Liver Transpl.2004; 10:S39-45.
Poon RT, Fan ST, Lo CM, Liu CL, Lam CM, Yuen WK, Yeung C, Wong J. Improving perioperative outcome expands the role of hepatectomy in management of benign and malignant hepatobiliary diseases: analysis of 1222 consecutive patients from a prospective database. Ann Surg 2004; 240:698–708.
Nagano Y, Matsuo K, Kunisaki C, Ike H, Imada T, Tanaka K, Togo S, Shimada H. Practical usefulness of ultrasonic surgical aspirator with argon beam coagulation for hepatic parenchymal transection. World J Surg 2005; 29:899–902.
Scatton O, Massault PP, Dousset B, Houssin D, Bernard D, Terris B, Soubrane O. Major liver resection without clamping: a prospective reappraisal in the era of modern surgical tools. J Am Coll Surg 2004; 199:702–08.
Conflict of Interest
There is no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Li, H., Wu, Js., Wang, Xt. et al. Major Hepatectomy Is a Safe Modality for the Treatment of Intrahepatic Cholangiocarcinoma in Selected Patients Complicated with Cirrhosis. J Gastrointest Surg 18, 194–199 (2014). https://doi.org/10.1007/s11605-013-2363-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-013-2363-6