Abstract
Objective
Although the effect of decitabine on myelodysplastic syndrome (MDS) has been demonstrated, merely a proportion of patients respond to therapy, and no well-recognized predictors have been identified. This study was conducted to investigate the effectiveness of decitabine in real-world clinical practice, and determine the predictive factors of response and overall survival (OS) in MDS patients.
Methods
Clinical and pathological data were collected from 94 patients and analyzed. These patients were reclassified according to the 2016 World Health Organization classification criteria, and restratified by International Prognostic Scoring System prognostic scores. The response evaluation was performed according to the 2006 modified International Working Group response criteria.
Results
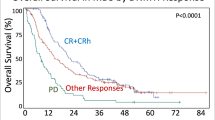
In this study, 62% of patients responded to decitabine. Among these patients, 15 patients (16%) obtained complete remission (CR), 15 patients (16%) obtained marrow CR with hematologic improvement (HI), 20 patients (21%) obtained marrow CR without HI, and 8 patients (9%) only obtained HI, and no patient botained partial remission. The OS of the responders was significantly longer than that of non-responders (67 months vs. 7 months, P<0.001). The OS in patients with and without platelet doubling was significantly different in both the low/intermediate and high/very high risk groups (P=0.0398 and P=0.0330). The multivariate analysis revealed that platelet doubling after the first decitabine cycle is an independent predictor of response and OS in MDS patients (P=0.002 and P=0.008).
Conclusion
Decitabine is effective for treating MDS patients in real-world clinical practice. Furthermore, platelet doubling after the first decitabine cycle can be used as a predictor of response and survival in MDS patients.
Similar content being viewed by others
References
Gil-Perez A, Montalban-Bravo G. Management of myelodysplastic syndromes after failure of response to hypomethylating agents. Ther Adv Hematol, 2019,10: 2040620719847059
Kantarjian H, Issa JPJ, Rosenfeld CS, et al. Decitabine improves patient outcomes in myelodysplastic syndromes—Results of a Phase III randomized study. Cancer, 2006,106(8):1794–1803
Fenaux P, Mufti GJ, Hellstrom-Lindberg E, et al. Efficacy of azacitidine compared with that of conventional care regimens in the treatment of higher-risk myelodysplastic syndromes: a randomised, open-label, phase III study. Lancet Oncol, 2009,10(3):223–232
Scott LJ. Azacitidine: A Review in Myelodysplastic Syndromes and Acute Myeloid Leukaemia. Drugs, 2016,76(8):889–900
Jabbour E, Short NJ, Montalban-Bravo G, et al. Randomized phase 2 study of low-dose decitabine vs low-dose azacitidine in lower-risk MDS and MDS/MPN. Blood, 2017,130(13):1514–1522
Nazha A, Sekeres MA, Bejar R, et al. Genomic Biomarkers to Predict Resistance to Hypomethylating Agents in Patients With Myelodysplastic Syndromes Using Artificial Intelligence. JCO Precis Oncol, 2019,3: 1–11
Jung KS, Kim YJ, Kim YK, et al. Clinical Outcomes of Decitabine Treatment for Patients With Lower-Risk Myelodysplastic Syndrome on the Basis of the International Prognostic Scoring System. Clin Lymphoma Myeloma Leuk, 2019,19(10):656–664
Wang H, Li Y, Lv N, et al. Predictors of clinical responses to hypomethylating agents in acute myeloid leukemia or myelodysplastic syndromes. Ann Hematol, 2018, 97(11):2025–2038
Bejar R, Lord A, Stevenson K, et al. TET2 mutations predict response to hypomethylating agents in myelodysplastic syndrome patients. Blood, 2014, 124(17):2705–2712
Solly F, Koering C, Mohamed AM, et al. An miRNA-DNMT1 Axis Is Involved in Azacitidine Resistance and Predicts Survival in Higher-Risk Myelodysplastic Syndrome and Low Blast Count Acute Myeloid Leukemia. Clin Cancer Res, 2017,23(12):3025–3034
van der Helm LH, Alhan C, Wijermans PW, et al. Platelet doubling after the first azacitidine cycle is a promising predictor for response in myelodysplastic syndromes (MDS), chronic myelomonocytic leukaemia (CMML) and acute myeloid leukaemia (AML) patients in the Dutch azacitidine compassionate named patient programme. Br J Haematol, 2011,155(5):599–606
Jung HA, Maeng CH, Kim M, et al. Platelet response during the second cycle of decitabine treatment predicts response and survival for myelodysplastic syndrome patients. Oncotarget, 2015,6(18):16653–16662
Tang Y, Zhang X, Han S, et al. Prognostic Significance of Platelet Recovery in Myelodysplastic Syndromes With Severe Thrombocytopenia. Clin Appl Thromb Hemost, 2018,24(9_suppl):217S–222S
Arber DA, Orazi A, Hasserjian R, et al. The 2016 revision to the World Health Organization classification of myeloid neoplasms and acute leukemia. Blood, 2016,127(20):2391–2405
Greenberg PL, Tuechler H, Schanz J, et al. Revised international prognostic scoring system for myelodysplastic syndromes. Blood, 2012,120(12):2454–2465
Cheson BD, Greenberg PL, Bennett JM, et al. Clinical application and proposal for modification of the International Working Group (IWG) response criteria in myelodysplasia. Blood, 2006,108(2):419–425
Jeong SH, Kim YJ, Lee JH, et al. A prospective, multicenter, observational study of long-term decitabine treatment in patients with myelodysplastic syndrome. Oncotarget, 2015,6(42):44985–44994
Salim O, Toptas T, Avsar E, et al. Azacitidine versus decitabine in patients with refractory anemia with excess blast-Results of multicenter study. Leuk Res, 2016,45: 82–89
Lee JH, Jang JH, Park J, et al. A prospective multicenter observational study of decitabine treatment in Korean patients with myelodysplastic syndrome. Haematologica, 2011,96(10):1441–1447
Ye L, Ren Y, Zhou X, et al. Decitabine improves overall survival inmyelodysplastic syndromes-RAEB patients aged ≥60 years and has lower toxicities: Comparison with low-dose chemotherapy. Blood Cells Mol Dis, 2019,77:88–94
Kantarjian HM, O’Brien S, Huang X, et al. Survival advantage with decitabine versus intensive chemotherapy in patients with higher risk myelodysplastic syndrome: comparison with historical experience. Cancer, 2007, 109(6):1133–1137
Wang M, Han HH, Guo R, et al. Clinical Efficacy of Low-dose Decitabine Combined with CAG Regimen in Patients with Myelodysplastic Syndrome-refractory Anemia with Excess Blasts(MDS-RAEB). Zhongguo Shi Yan Xue Ye Xue Za Zhi (Chinese), 2017,25(5):1482–1486
Zhang JL, Cao YP, Li JG. Efficacy and Safety of Decitabine Combined with CAG (Cytarabine, Aclarubicin, G-CSF) for Patients with Intermediate or High Risk Myelodysplastic Syndrome and Acute Myeloid Leukemia: a Meta-Analysis. Zhongguo Shi Yan Xue Ye Xue Za Zhi (Chinese), 2019,27(2):494–503
Itzykson R, Thepot S, Quesnel B, et al. Prognostic factors for response and overall survival in 282 patients with higher-risk myelodysplastic syndromes treated with azacitidine. Blood, 2011,117(2):403–411
Traina F, Visconte V, Elson P, et al. Impact of molecular mutations on treatment response to DNMT inhibitors in myelodysplasia and related neoplasms. Leukemia, 2014,28(1):78–87
DiNardo CD, Patel KP, Garcia-Manero G, et al. Lack of association of IDH1, IDH2 and DNMT3A mutations with outcome in older patients with acute myeloid leukemia treated with hypomethylating agents. Leuk Lymphoma, 2014,55(8):1925–1929
Welch JS, Petti AA, Miller CA, et al. TP53 and Decitabine in Acute Myeloid Leukemia and Myelodysplastic Syndromes. N Engl J Med, 2016,375(21):2023–2036
Bally C, Ades L, Renneville A, et al. Prognostic value of TP53 gene mutations in myelodysplastic syndromes and acute myeloid leukemia treated with azacitidine. Leuk Res, 2014,38(7):751–755
Wang J, Yi Z, Wang S, et al. The effect of decitabine on megakaryocyte maturation and platelet release. Thromb Haemost, 2011,106(2):337–343
Ding K, Fu R, Liu H, et al. Effects of decitabine on megakaryocyte maturation in patients with myelodysplastic syndromes. Oncol Lett, 2016,11(4): 2347–2352
Zhang W, Liu C, Wu D, et al. Decitabine improves platelet recovery by down-regulating IL-8 level in MDS/AML patients with thrombocytopenia. Blood Cells Mol Dis, 2019,76:66–71
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The authors declare that they have no conflict of interest.
Additional information
This work was supported by the National Natural Science Foundation of China (No. 81770168 and No. 81570110).
Rights and permissions
About this article
Cite this article
Lu, Pf., Deng, Ln., Meng, Fk. et al. Platelet Doubling After First Decitabine Cycle Predicts Response and Survival of Myelodysplastic Syndrome Patients. CURR MED SCI 42, 77–84 (2022). https://doi.org/10.1007/s11596-022-2533-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11596-022-2533-4