Summary
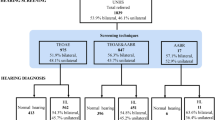
To investigate the high-risk factors for newborn hearing loss and to provide information for preventing the development of hearing loss and delaying its progression, from May 2003 to June 2006, neonates who failed to pass the universal newborn hearing screening (UNHS) were referred to Jinan Newborn Hearing Screening and Rehabilitation Center from 7 newborn hearing screening centers in seven cities of Shandong province. One-to-one pair-matched case-control method was employed for statistical analysis of the basic features of definitely identified cases. High-risk factors relating to the bilateral hearing loss were evaluated by univariate and multivariate Logistic regression analysis. Our results revealed that 721 transferred newborns who didn’t pass the hearing screening received audiological and medical evaluation and 367 were confirmed to have hearing loss. Of them, 177 neonates with hearing loss who met the matching requirements were included in the study as subjects. Univariate analysis showed that high-risk factors related to hearing loss incuded age of father, education backgrounds of parents, parity, birth weight, gestational weeks, craniofacial deformity, history of receiving treatment in neonatal intensive care unit (NICU), neonatal disease, family history of otopathy and family history of congenital hearing loss. Multivariate Logistic regression analysis revealed that 4 independent risk factors were related to bilateral hearing loss, including parity (OR=16.285, 95% CI 3.379–78.481), neonatal disease (OR=34.968, 95% CI 2.720–449.534), family history of congenital hearing loss (OR=69.488, 95% CI 4.417–1093.300) and birth weight (OR=0.241, 95% CI 0.090–0.648). It is concluded that parity, neonatal disease and family history of hearing loss are the promoting factors of bilateral hearing loss in neonates and appropriate intervention measures should be taken to deal with the risk factors.
Similar content being viewed by others
References
Joint Committee on Infant Hearing. Year 2000 Position Statement: Principles and Guideline for Early Hearing Detection and Intervention Programs. Pediatrics, 2000,106(4):798–817
Berg A L, Spitzer J B, Towers H M et al. Newborn hearing screening in the NICU: profile of failed auditory brainstem response/passed otoacoustic emission. Pediatrics, 2005,114(6):933–938
Uus K, Bamford J. Effectiveness of population-based newborn hearing screening in England: ages of interventions and profile of cases. Pediatrics, 2006,117:e887–893
Vohr B R, Widen J E, Cone-Wesson B et al. Identification of neonatal hearing impairment: char-acteristics of infants in the neonatal intensive care unit and well-baby nursery. Ear Hear, 2000,21(5):373–382
Rovet J, Walker W, Bliss B et al. Long-team hearing impairment in congenital hypothyroidism. J Pediatr, 1996,128(6):776–783
Ari-Even Roth D, Hildesheimer M, Maayan-Metzger A et al. Low prevalence of hearing impairment among very low birthweight infants as detected by universal neonatal hearing screening. Arch Dis Child Fetal Neonatal Ed, 2006,91:F257–262
Iwasaki S, Yamashita M, Maeda M et al. Audiological outcome of infants with congenital cytomegalovirus infection in a prospective Study. Audiol Neurootol, 2006,12:31–36
Qiu X Q, Zeng X Y, Qin D D et al. A case-control study on the risk factor of perinatals’ congenital malformations in seven cities of Guangxi. Chin J Epidemiol (Chinese), 2003,24(6):512–515
Chen P, Tang A Z, Su J P et al. Characteristics of hearing loss in 299 high-risk neonates. Chin J Otorhinolaryngol Head Neck Surg (Chinese), 2005,40(5):335–338
Castilla E E, Orioli I M. Prevalence rates of microtia in South America. Int J Epidemiol, 1986,15(3):364–368
Du J M, Guo W H, Han J et al. Case control study on risk factors of congenital microtia. Chin J Otorhinolaryngol Head Neck Surg (Chinese), 2006,41(2):107–111
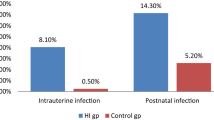
Weichbold V, Nekahm-Heis D, Welzl-Mueller K et al. Universal newborn hearing screening and postnatal hearing loss. Pediatrics, 2006,117:e631–636
Norris V W, Arnos K S, Hanks W D et al. Does universal newborn hearing screening identify all children with GJB2 (Connexin 26) deafness? Penetrance of GJB2 deafness. Ear Hear, 2006,27(6):732–741
Ravecca F, Berrettini S, Forli F et al. Cx26 gene mutations in idiopathic progressive hearing loss. J Otolaryngol, 2005,34:126–134
Pagarkar W, Bitner-Glindzicz M, Knight J. Late postnatal onset of hearing loss due to GJB2 mutations. Int J Pediatr Otorhinolaryngol, 2006,70(9):1119–1124
Author information
Authors and Affiliations
Additional information
NIE Wenying, female, born in 1968, Associate Professor
This project is supported by a grant from the National Natural Sciences Foundation (No. 30100207) and a grant from the Top Ten Scientific Research Programs of Shandong Province (No. 2004GG3202003).
Rights and permissions
About this article
Cite this article
Nie, W., Wu, H., Qi, Y. et al. A case-control study on high-risk factors for newborn hearing loss in seven cities of Shandong province. J. Huazhong Univ. Sc. Technol. 27, 217–220 (2007). https://doi.org/10.1007/s11596-007-0230-y
Received:
Issue Date:
DOI: https://doi.org/10.1007/s11596-007-0230-y