Abstract
Purpose
The determination of an optimal pivot point (\({ OPP}\)) is important for instrument manipulation in minimally invasive surgery. Such knowledge is of particular importance for robotic-assisted surgery where robots need to rotate precisely around a specific point in space in order to minimize trauma to the body wall while maintaining position control. Remote center of motion (RCM) mechanisms are commonly used, where the RCM point is manually and visually aligned. If not positioned appropriately, this misalignment might lead to intolerably high forces on the body wall with increased risk of postoperative complications or instrument damage. An automated method to align the RCM with the \({ OPP}\) was developed and tested.
Method
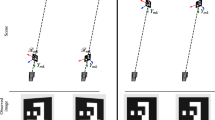
Computer vision and a lightweight calibration procedure are used to estimate the optimal pivot point. One or two pre-calibrated cameras viewing the surgical scene are employed. The surgeon is asked to make short pivoting movements, applying as little torque as possible, with an instrument of choice passing through the insertion point while camera images are being recorded. The physical properties of an instrument rotating around a pivot point are exploited in a random sample consensus scheme to robustly estimate the ideal position of the RCM in the image planes. Triangulation is used to estimate the RCM position in 3D. Experiments were performed on a specially designed mockup to test the method.
Results
The position of the pivot point is estimated with an average error less than 1.85 mm using two webcams placed from approximately 30 cm to 1 m away from the scene. The entire procedure was completed in a few seconds.
Conclusion
An automated method to estimate the ideal position of the RCM was shown to be reliable. The method can be implemented within a visual servoing approach to automatically place the RCM point, or the results can be displayed on a screen to provide guidance to the surgeon. Further work includes the development of an image-guided alignment method and validation with in vivo experiments.






Similar content being viewed by others
Notes
Open Source Computer Vision Library, http://opencv.org.
References
Berghöfer A, Pischon T, Reinhold T, Apovian CM, Sharma AM, Willich SN (2008) Obesity prevalence from a european perspective: a systematic review. BMC Public Health 8(1):200
Bouguet J (2014) MATLAB calibration toolbox. http://www.vision.caltech.edu/bouguetj/calib_doc/ (consulted March 1)
Doignon C, Graebling P, de Mathelin M (2005) Real-time segmentation of surgical instruments inside the abdominal cavity using a joint hue saturation color feature. Real-Time Imaging 11(5):429–442
Fischler MA, Bolles RC (1981) Random sample consensus: a paradigm for model fitting with applications to image analysis and automated cartography. Commun ACM 24(6):381–395
Givens ML, Ayotte K, Manifold C (2004) Needle thoracostomy: implications of computed tomography chest wall thickness. Acad Emerg Med 11(2):211–213
Hartley R, Zisserman A (2003) Multiple view geometry in computer vision. Cambridge university press, Cambridge
Helgstrand F, Rosenberg J, Bisgaard T (2011) Trocar site hernia after laparoscopic surgery: a qualitative systematic review. Hernia 15(2):113–121
Herman B, Dehez B, Duy KT, Raucent B, Dombre E, Krut S (2009) Design and preliminary in vivo validation of a robotic laparoscope holder for minimally invasive surgery. Int J Med Robot Comput Assist Surg 5(3):319–326
Intuitive Surgical: da Vinci prostatectomy procedure guide. PN 871403 Rev. A 4/06
Krupa A, Gangloff J, Doignon C, de Mathelin MF, Morel G, Leroy J, Soler L, Marescaux J (2003) Autonomous 3-d positioning of surgical instruments in robotized laparoscopic surgery using visual servoing. IEEE Trans Robot Autom 19(5):842–853
Kwaan MR, Sirany AM, Rothenberger DA, Madoff RD (2013) Abdominal wall thickness: is it associated with superficial and deep incisional surgical site infection after colorectal surgery? Surg Infect (Larchmt) 14(4):363–368
Ma Y, Soatto S, Kosecká J, Sastry S (2004) An invitation to 3-d vision: from images to geometric models, interdisciplinary applied mathematics, vol 26. Springer, Berlin
Mayer H, Nagy I, Knoll A (2004) Kinematics and modelling of a system for robotic surgery. In: Lenarčič J, Galletti C (eds) On Advances in robot kinematics. Springer, Berlin, pp 181–190
Milad MP, Terkildsen MF (2002) The spinal needle test effectively measures abdominal wall thickness before cannula placement at laparoscopy. J Am Assoc Gynecol Laparosc 9(4):514–518
Oddsdottir M, Birgisson G (2004) Aesop: a voice-controlled camera holder. In: Ballantyne GH, Marescaux J, Giulianotti PC (eds) Primer of robotic and telerobotic surgery. Chap 5, pp 35–41
Ogden CL, Carroll MD (2010) Prevalence of overweight, obesity, and extreme obesity among adults: United States, trends 1960–1962 through 2007–2008. National Center for Health Statistics 6:1–6
Ortmaier T, Hirzinger G (2000) Cartesian control issues for minimally invasive robot surgery. In: Intelligent robots and systems, 2000. (IROS 2000). Proceedings 2000 IEEE/RSJ International Conference on vol 1, pp 565–571. IEEE
Ostrowitz MB, Eschete D, Zemon H, DeNoto G (2009) Robotic-assisted single-incision right colectomy: early experience. Int J Med Robot Comput Assist Surg 5(4):465–470
Schurr M, Arezzo A, Neisius B, Rininsland H, Hilzinger HU, Dorn J, Roth K, Buess G (1999) Trocar and instrument positioning system TISKA. Surg Endosc 13(5):528–531
Song C, Alijani A, Frank T, Hanna G, Cuschieri A (2006) Mechanical properties of the human abdominal wall measured in vivo during insufflation for laparoscopic surgery. Surg Endosc Other Interv Tech 20(6):987–990
Tang HW, Van Brussel H, Peirs J, Janssens T (2010) Remote centre of motion positioner WO Patent 2,010,130,817
Taylor RH, Funda J, Eldridge B, Gomory S, Gruben K, LaRose D, Talamini M, Kavoussi L, Anderson J (1995) A telerobotic assistant for laparoscopic surgery. Eng Med Biol Mag IEEE 14 (3):279–288
Tonouchi H, Ohmori Y, Kobayashi M, Kusunoki M (2004) Trocar site hernia. Arch Surg 139(11):1248–1256
Voros S, Haber GP, Menudet JF, Long JA, Cinquin P (2010) Viky robotic scope holder: initial clinical experience and preliminary results using instrument tracking. IEEE/ASME Trans Mechatron 15(6):879–886
Voros S, Long JA, Cinquin P (2007) Automatic detection of instruments in laparoscopic images: A first step towards high-level command of robotic endoscopic holders. Int J Robot Res 26(11–12):1173–1190
Wilson J, Tsao TC, Hubschman J, Schwartz S (2010) Evaluating remote centers of motion for minimally invasive surgical robots by computer vision. In: Advanced Intelligent Mechatronics (AIM), 2010 IEEE/ASME International Conference on, pp 1413–1418 doi:10.1109/AIM.2010.5695924
Wolf R, Duchateau J, Cinquin P, Voros S (2011) 3d tracking of laparoscopic instruments using statistical and geometric modeling. In: Fichtinger G, Martel A, Peters T (eds) Medical Image Computing and Computer-Assisted Intervention-MICCAI 2011. Springer, Berlin, pp 203–210
Zhang Z (2000) A flexible new technique for camera calibration. IEEE Trans Pattern Anal Mach Intell 22(11):1330–1334
Conflict of interest
Benoît Rosa, Emmanuel Vander Poorten, Caspar Gruijthuijsen, Ben Van Cleynenbreugel, Dominiek Reynaerts and Jos Vander Sloten declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rosa, B., Gruijthuijsen, C., Van Cleynenbreugel, B. et al. Estimation of optimal pivot point for remote center of motion alignment in surgery. Int J CARS 10, 205–215 (2015). https://doi.org/10.1007/s11548-014-1071-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11548-014-1071-3