Abstract
The receptor for epidermal growth factor (EGFR, ErbB1, HER1) supports the growth and maintenance of a broad range of human tumor types, and EGFR-targeting drugs are approved for the treatment of several advanced stage cancers, including non-small cell lung cancer (NSCLC), pancreatic cancer, squamous cell cancer of the head and neck (SCCHN), and colorectal cancer. Recent years have witnessed significant advances in our understanding of dysregulated signal transduction in cancer cells resulting from changes in the expression and/or mutational status of key signaling molecules that modulate sensitivity to drugs targeting EGFR. Based on this knowledge, we have an exciting opportunity to maximize the benefit provided to cancer patients by EGFR inhibitors. In this review article, we describe molecular determinants of sensitivity or resistance to EGFR-targeted agents, with specific emphasis on EGFR tyrosine kinase inhibitors (TKIs). The impact of these findings on our ability to evaluate candidate predictive biomarkers and to design robust mechanism-based combination strategies is also discussed.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The receptor for epidermal growth factor (EGFR, ErbB1, HER1) is overexpressed in a broad range of human cancers, including non-small cell lung cancer (NSCLC), pancreatic cancer, squamous cell cancer of the head and neck (SCCHN), as well as colorectal, breast, hepatocellular and ovarian carcinomas [1–6]. EGFR signaling contributes to the growth and survival of tumor cells through its ability to activate multiple signal transduction networks including the mitogen-activated protein kinase (MAPK) and AKT pathways. In preclinical models, inhibition of EGFR signaling either by antibodies that neutralize ligand-mediated activation or small molecule kinase inhibitors results in decreased tumor cell proliferation and/or viability in vitro and inhibition of tumor growth in vivo. Anti-EGFR monoclonal antibodies (e.g., cetuximab, panitumumab) have been approved for the treatment of advanced SCCHN and colorectal cancer [7–9] and EGFR tyrosine kinase inhibitors (TKI) (e.g., erlotinib, gefitinib) have been approved for the treatment of advanced NSCLC and pancreatic cancer [10–14]. The approval of these drugs has been based on demonstration of modest efficacy in large clinical studies that enrolled broad patient populations and it is clear that relatively small proportions of patients received dramatic benefit whereas the majority of patients received little to no benefit. These observations highlight the need for biomarkers that will identify those patients most likely to maximally benefit from EGFR-targeted drugs as monotherapies or in combination with other anticancer agents. This review article will focus on recent advances in our understanding of tumor cell signaling that mediates sensitivity or resistance to EGFR TKIs and how this knowledge has led to the identification of potential biomarkers that might be used to identify patients most likely to benefit from treatment with EGFR TKIs.
EGFR signaling and ErbB3
An understanding of the signal transduction pathways that mediate sensitivity to EGFR TKIs provides a basis for the identification of predictive, mechanism-based biomarkers and for the design of rational combination strategies. EGFR activation occurs through ligand binding to receptor monomers, which promotes dimer formation and enhanced catalytic activity. Ligands for EGFR include EGF and transforming growth factor α (TGFα) EGFR can form EGFR-EGFR homodimers as well as heterodimers with other members of the ErbB receptor family (ErbB2/HER2, ErbB3/HER3, ErbB4/HER4) [15–17]. Within this family, EGFR and ErbB4 have functional ligand binding and catalytic domains. There are no known ligands for ErbB2 and its kinase activity is primarily transactivated by dimerization with other ErbB family members [18]. In contrast, ErbB3 lacks a functional kinase domain, but does have a competent ligand-binding domain [19, 20], which binds ligands of the neuregulin family. Although ErbB3 lacks enzymatic activity, it contains several tyrosine residues within the YXXM motif, which can by phosphorylated by heterodimer partners and by crosstalk with other receptors. When phosphorylated, these YXXM sites serve as docking sites for SH2-containing intracellular signaling proteins including the p85 regulatory subunit of phosphatidyl inositide-3 kinase (PI3K) [21–24]. Thus, ErbB3 is capable of transducing intracellular signals despite its inherent lack of kinase activity.
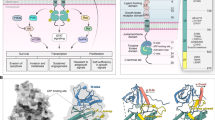
Different ErbB family dimers show distinct signaling patterns. For example, EGFR-ErbB2 and EGFR-ErbB3 heterodimers are generally more effective than EGFR homodimers at transducing growth and survival signals [25]. Recent studies have shown that EGFR homodimers may contribute primarily to activation of the MAPK pathway, whereas EGFR-ErbB3 heterodimers preferentially contribute to activation of the PI3K-AKT pathway (Fig. 1). Small-interfering RNAs (siRNA) directed toward ErbB3 decrease AKT signaling, but not MAPK signaling [26]. Interestingly, ErbB3 expression and thus AKT activation is associated with sensitivity to EGFR TKIs, suggesting that ErbB3 and/or phospho-AKT could serve as positive predictive biomarkers for EGFR TKIs.
EGFR mutations
Mutations within EGFR (exon 19 deletions, exon 20 insertions or point mutations that result in the L858R substitution) give rise to enhanced catalytic activity, which confers greater “addiction” of tumor cells to the EGFR signaling pathway [27–30]. Tumor cells that harbor such mutations are more sensitive to EGFR TKIs [31–33]. This increased sensitivity to TKIs may be mediated by multiple mechanisms, including “onco-addiction” to the EGFR pathway and/or structural changes in EGFR that result in higher binding affinities for TKIs. Indeed, the binding affinity of EGFR TKIs is increased by greater than 10-fold by the L858R substitution in EGFR [34]. Additionally, the affinity for ATP, which competes for TKI binding, is reduced by the L858 substitution, yielding an approximately 500-fold increase in the Kd (TKI) to Km (ATP) ratio.
Recently, secondary mutations in EGFR that result in a T790M substitution have been shown to contribute to acquired resistance to EGFR TKIs [35–39]. When NSCLC cell lines expressing highly sensitive EGFR variants, described above, were subjected to long term exposure to gefitinib in vitro, the resulting resistance to gefitinib was accompanied by the acquisition of secondary mutations in EGFR that encode the T790M substitution [35]. This observation has been validated in the clinic; patients whose tumors harbor activating mutations of EGFR initially respond well to EGFR TKIs, but their cancers eventually progress. The development of resistance to EGFR TKIs in approximately 50% of these patients is associated with the acquisition secondary mutations that result in the T790M substitution in EGFR [35, 36, 40, 41]. Residue 790 of EGFR lies within the hinge region of the catalytic domain and is the “gatekeeper” residue for EGFR. Interestingly, “gatekeeper” mutations are commonly associated with resistance to TKIs, such as the T315I mutation in BCR-ABL that can confer resistance to imatinib in chronic myelogenous leukemia (CML) patients [42, 43]. Initial studies suggested that EGFR TKIs may exhibit weaker binding to the EGFR double mutants compared to either wild-type (WT) EGFR or the single mutants (L858R or exon 19/20 mutations). However, recent reports have shown a three- to four-fold increase in TKI binding affinity for the T790M-L858R double mutant compared to WT EGFR. Despite this observation, the affinity of TKIs for the single L858R mutant-EGFR was still approximately four-fold greater [34]. Rather than being mediated by reduced binding affinity, the reduced potency of EGFR TKIs for T790M double mutants is driven by an associated increase in the Km for ATP, which competes with the EGFR TKI for binding in the catalytic domain.
In human tumors, T790M EGFR has been detected only in cis with either of the two primary activating mutations [35]. Although initial reports showed that the T790M substitution, in an otherwise WT EGFR background, conferred decreased sensitivity to reversible EGFR TKIs such as gefitinib and erlotinib by 100-fold, the T790M substitution has not been detected in the absence of either of the two primary activating mutations either in established tumor cell lines or in patient samples. Recently, characterization of the relative catalytic gain conferred by various mutations, either alone or in combination has shed light onto these observations [44]. Unlike the primary mutations that confer a strong gain in catalytic activity compared to WT EGFR, the T790M substitution results in only a modest gain in catalytic activity compared to WT EGFR and is relatively silent in the context of cellular signaling [44]. However, in combination with either of the two primary activating mutations, T790M confers a synergistic gain in catalytic activity. The development of acquired resistance by the T790M substitution may be modeled in two ways. In one model, the T790M substitution is absent in the initial tumor cell population and arises de novo in one or more clonal populations upon treatment with an EGFR TKI. In the second model, the T790M substitution pre-exists in cis with a primary activating mutation in a small population and is subjected to positive selection pressure in the presence of an EGFR TKI. Recent data suggest that the latter scenario may be more likely because mutations encoding T790M have been detected in cis with a primary activating mutation in tumors from patients who had not been treated with an EGFR TKI. The observation that this mutation confers a gain in catalytic activity provides a rationale for its co-existence in tumors with activating mutations in EGFR but not in those tumors with WT EGFR [45]. Given that the T790M substitution alone does not confer substantially higher catalytic activity compared to WT EGFR, it is unlikely that it would have a selective advantage in a primary tumor. Collectively, these data suggest a role for the T790M mutation for tumors that harbor primary activating mutations in EGFR, but suggest that this mode of resistance is unlikely among tumors of WT EGFR status. Therefore, it is critically important that we continue to study other mechanisms of resistance to EGFR TKIs so that we can provide tailored treatment regimens to appropriately defined patient subpopulations.
K-RAS mutations
Activating mutations in the gene encoding K-RAS in human tumors have been implicated in reduced sensitivity to EGFR inhibitors. The mechanistic rationale for this hypothesis is based upon long-standing dogma: since K-RAS mainly functions downstream of EGFR, then EGFR inhibitors should have little impact on signaling through the RAS-RAF-MEK-MAPK pathway [46]. In colorectal cancer patients, K-RAS mutations are predictive for poor response to the EGFR neutralizing antibodies, cetuximab or panitumumab [47, 48]. Currently, there are no definitive clinical data that extend this finding to EGFR TKIs. In preclinical models K-RAS status is not strongly associated with either sensitivity or insensitivity to EGFR TKIs, but it will be important to carefully study emerging clinical data [26, 49, 50].There are interesting differences between the pharmacological mechanisms of anti-EGFR MAbs and EGFR TKIs. In some preclinical models, EGFR TKIs such as erlotinib inhibited both the MAPK and AKT pathways, whereas the EGFR neutralizing antibody, C225, affected only MAPK signaling [51]. This distinction was associated with differential regulation of EGFR homodimers and EGFR-ErbB3 heterodimers; while both erlotinib and C225 similarly inhibited EGFR phosphorylation, only erlotinib inhibited EGFR trans-phosphorylation of ErbB3. This is consistent with the observation that C225 was unable to block PI3K-AKT signaling. These data indicate that anti-EGFR MAbs, which affect signaling preferentially through the MAPK pathway, might be more sensitive to activating K-RAS mutations compared to EGFR TKIs, which provide an additional activity by inhibiting signaling through the AKT survival pathway. While limited clinical data do suggest that mutant K-RAS may behave as a modifier of erlotinib efficacy in NSCLC patients, it does not appear to be a key determinant of efficacy to the same extent as it is for anti-EGFR MAbs in colorectal cancer [52]. Furthermore, erlotinib has proven efficacy in combination with gemcitabine for treatment of patients with advanced pancreatic cancer, a tumor type that has a very high prevalence (80–95%) of activating K-RAS mutations [53]. The utility of K-RAS mutations as predictive biomarkers for EGFR TKIs is additionally obscured by their mutual exclusivity with EGFR activating mutations, their association with smoking, and by being a general indicator of poor prognosis [54–57]. Clearly, further studies are necessary to fully elucidate the role of K-RAS mutations in affecting EGFR TKI sensitivity.
Epithelial mesenchymal transition
Recent studies have shown that biomarkers associated with epithelial mesenchymal transition (EMT) can be used to predict sensitivity to EGFR TKIs [49, 50, 58–60]. Carcinomas originate as epithelial cells and express characteristic epithelial markers such as E-cadherin, which function in homotypic cell-cell adhesion [61]. While these cells can rapidly proliferate upon oncogenic transformation, their epithelial phenotype hinders their ability to migrate from the primary tumor site or to survive in an anchorage independent manner. Intrinsic and extrinsic signals can trigger tumor cells to undergo an epithelial-mesenchymal transition, whereby tumor cells lose the expression of epithelial proteins such as E-cadherin and gain mesenchymal markers including vimentin. Tumor cells that have undergone EMT exhibit a number of phenotypic hallmarks including decreased cell-cell adherence, increased motility, increased invasiveness and anchorage independent survival.
Proteomic and gene expression profiling experiments revealed differential expression of epithelial and mesenchymal proteins in erlotinib-sensitive and erlotinib–insensitive tumor cell lines [49, 50]. Those tumor cells most sensitive to growth inhibition by erlotinib in vitro and in vivo expressed epithelial protein markers such as E-cadherin and β-catenin. In contrast, tumor cells that had undergone EMT were less sensitive to erlotinib and accordingly downregulated the expression of epithelial markers while increasing the expression of mesenchymal markers, including vimentin and fibronectin. Erlotinib–sensitive tumor cell lines exhibited the cobblestone appearance typical of epithelial cells, while erlotinib–insensitive tumor cell lines exhibited a spindle-like morphology that is typical of mesenchymal cells. These preclinical observations have been substantiated with some preliminary analyses from at least one clinical trial [50]. A retrospective analysis of samples taken from the TRIBUTE study, which evaluated the efficacy of carboplatin/paclitaxel compared to carboplatin/paclitaxel plus erlotinib in front line NSCLC, was conducted to investigate the possible correlation of EMT status with erlotinib sensitivity. While the addition of erlotinib to chemotherapy did not provide a statistically significant benefit in terms of progression-free survival (PFS) across the broad group of unselected patients, a retrospective analysis showed that there was a significant relationship between longer time to progression (hazard ratio = 0.37) and E-cadherin expression in patient tumors for the erlotinib plus chemotherapy arm compared to the chemotherapy-alone arm.
Further preclinical studies have shown that EMT may play a role in predicting sensitivity to EGFR inhibitors across a number of tumor types including pancreatic, colorectal, breast, bladder and hepatocellular cancers as well as SCCHN [59, 60]. For example, in pancreatic cancer cell lines, erlotinib inhibited EGFR phosphorylation in both erlotinib–insensitive (mesenchymal) and erlotinib–sensitive (epithelial) tumor cells, however, erlotinib only inhibited AKT and MAPK signaling in epithelial cell lines (erlotinib sensitive).
Recent studies into the mechanism by which erlotinib sensitivity is restricted to epithelial tumor cells have shown that ErbB3 expression, which mediates EGFR directed AKT signaling, also appears to be restricted to epithelial tumor cells, and expression of ErbB3 is decreased when tumor cells undergo EMT. Snail, a transcription factor that functions to promote EMT, represses transcription of CDH1 (the gene encoding E-cadherin) and ErbB3 [62]. In experimental models where EMT can be induced in vitro by treating tumor cells with TGFβ, increased expression of mesenchymal proteins including snail, zeb1, and vimentin is associated with decreased expression of both E-cadherin and ErbB3 [63]. Thus, when tumor cells undergo EMT they lose an important conduit for transducing EGFR-driven signals to the AKT pathway.
EMT can also contribute to EGFR TKI resistance by shifting the tumor cells’ predominant reliance on EGFR to other networks, such as those activated by fibroblast growth factor receptor (FGFR), platelet derived growth factor receptor (PDGFR) or α5β1 integrin [63]. One hypothesis posits that epithelial tumor cells may rely on one suite of RTKs, including EGFR, for growth and survival in the epithelial state and also to enable EMT, but once the transition to the mesenchymal phenotype occurs, the tumor cells rely on a different array of signaling inputs to drive growth, survival, and virulence. There may be significant flexibility built into this system such that tumor cells are able to thrive in different metastatic microenvironments that offer distinct sets of “drivers.” Indeed, Minn et al. have shown distinct gene expression profiles from different metastatic sites in breast cancers [64].
Redundant RTKs
EGFR and other RTKs including the IGF-1R, MET, ErbB2/HER2, FGFR, and PDGFR can function redundantly or cooperatively to activate downstream signal transduction networks including the MAPK and AKT pathways. Activation of these other pathways can provide alternative proliferation and/or survival signals to bypass EGFR blockade. Tumor cells may intrinsically use independent RTKs de novo, where receptor crosstalk does not initially occur, but where inhibition of each independent pathway is required for maximal efficacy. Treatment with an EGFR inhibitor might also actively promote the activation of other RTKs, thereby initiating receptor crosstalk. By broadening our knowledge of specific RTKs that can contribute to insensitivity or acquired resistance to EGFR inhibitors, we will be better prepared to design rational combination regimens to maximize patient benefit. Below, we will summarize preclinical data supporting a role of IGF-1R and MET in contributing to intrinsic insensitivity or acquired resistance to EGFR inhibitors.
Although IGF-1R expression has not been associated with intrinsic resistance to the EGFR inhibitor gefitinib in patients with advanced non-small cell lung cancer [65], the phosphorylation state of IGF-1R (p-IGF-1R) was increased upon treatment with gefitinib. Resistance to EGFR inhibitors via p-IGF-1R has been reported for a number of tumor models including glioblastoma [66], breast and prostate [67], lung [68, 69], hepatocellular [70]), SCCHN [69], and colorectal [71]. Several mechanisms for IGF-1R-mediated acquired resistance to erlotinib have been described. One mechanism involves the formation of activated EGFR/IGF-1R complexes on the cell surface upon EGFR blockade. This has been shown in NSCLC cell lines both in vitro and in vivo upon erlotinib treatment, and this increase in EGFR/IGF-1R complexes is thought to enable the coordinated transmission of growth and survival signals to the AKT and MAPK pathways, such that targeted inhibition of both EGFR and IGF-1R is required for maximal efficacy (Fig. 2) [68]. Guix et al. reported that the interaction between IGF-1R and IRS-1, and thus active signaling to AKT, was induced upon treatment with erlotinib [69]). Increased formation of EGFR/IGF-1R complexes is thought to lead to further increases in the expression of EGFR and of the anti-apoptotic protein survivin in an mTOR-mediated manner. Blocking the IGF-1R pathway is sufficient to suppress survivin protein expression and to restore pro-apoptotic activities of erlotinib in NSCLC cells both in vitro and in vivo [68]. Furthermore, knockdown of survivin expression by siRNA resulted in increased sensitivity to erlotinib for NSCLC tumor cells, underscoring the critical role of survivin as a mechanism for IGF-1R mediated acquired resistance to erlotinib.
Crosstalk between EGFR and IGF-1R has been reported in pancreatic, colorectal and NSCLC cell lines [71]. Blockade of IGF-1R or EGFR by pharmacological approaches (e.g., the low molecular weight IGF-1R inhibitor PQIP, erlotinib) or by molecular approaches (e.g., siRNA) resulted in compensatory activation of the reciprocal receptor. Only the combined blockade of EGFR and IGF-1R resulted in sustained inhibition of the AKT pathway. Phenotypically, combined blockade of these receptors caused a synergistic inhibition of cell growth and survival in vitro and resulted in greater decreases in xenograft tumor growth compared to inhibition of either target alone. In fact, in a number of pancreatic, NSCLC and colon xenograft models in which either erlotinib or PQIP caused reduction of tumor growth rates or stasis, the combination of erlotinib plus PQIP caused bona fide and durable tumor regressions. Inhibition of the MAPK pathway by erlotinib resulted in increased IGF-1R-IRS-1 signaling through AKT, opening up an opportunity for PQIP to shut down this important escape mechanism.
Some IGF binding proteins (IGFBPs) can attenuate IGF-1r activation by acting as “chelators” of its ligands, IGF-1 and IGF-2. Therefore, an additional mechanism that may contribute to IGF-1R-mediated EGFR TKI resistance involves decreased expression of IGF-binding proteins, particularly IGFBP3 and IGFBP4 [69]). In a gefitinib-resistant variant of the A431 epidermoid carcinoma cell line, derived by long term gefitinib exposure, gefitinib retained the ability to inhibit phosphorylation of EGFR, ErbB3, and MAPK. However, gefitinib lost the ability to inhibit AKT phosphorylation, and this was associated with increased phospho-IGF-1R. The gefitinib resistant A431 variant exhibited increased complex formation between IRS-1 and PI3K, suggesting that resistance may be mediated by enhanced activity of IGF-1R/IRS-1/PI3K signaling. Gene expression profiling revealed that mRNAs encoding IGFBP3 and IGFBP4 were downregulated in the resistant clones. Addition of exogenous IGFBP3 to gefitinib–resistant A431 cultures restored sensitivity to gefitinib, further implicating IGF-1R signaling as the resistance mechanism. Finally, A431 xenografts treated with the combination of EGFR and IGF-1R inhibitors, gefitinib and a neutralizing antibody to IGF-1R, did not develop resistance to single agent gefitinib. Collectively, these data highlight the importance of IGF-1R activation as a mechanism to escape EGFR inhibition and suggest that the combined blockade of EGFR and IGF-1R might provide substantial benefit for many cancer patients.
Earlier, we summarized data showing that EGFR-ErbB3 heterodimers are potent activators of the AKT pathway in a subset of NSCLC cell lines and that ErbB3 in the context of EGFR expression may be a good predictor of sensitivity to EGFR TKIs [72]. In addition to EGFR, other RTKs such as MET also signal through ErbB3 to activate the AKT pathway, providing a resistance mechanism to EGFR inhibitors (Fig. 3) [73]. MET is receptor for hepatocyte growth factor (HGF), which is known to activate multiple signal transduction pathways including the AKT pathway [74–76]. Genomic amplification of MET results in increased expression of the MET protein, increased phosphorylation of ErbB3 and activation of PI3K/AKT in an EGFR- and ErB2-independent manner [73]. Furthermore, MET amplification has been detected in lung tumors with EGFR mutations that confer resistance to gefitinib or erlotinib [41, 73]. In one study, MET amplification occurred during the generation of gefitinib–resistant NSCLC by prolonged treatment with gefitinib. Increased phosphorylation of MET, ErbB3, EGFR and AKT accompanied MET amplification and the acquisition of gefitinib–resistance. While neither gefitinib nor the MET inhibitor, PHA-665752, were effective as single agents in this model, the combination of the two agents inhibited both ErbB3 and AKT phosphorylation and decreased tumor cell proliferation and survival and promoted apoptosis. Furthermore, downregulation of MET expression by MET-specific shRNAs restored gefitinib sensitivity. Coversely, ectopic overexpression of MET in the parental cells conferred gefitinb resistance. MET amplification as a resistance mechanism to EGFR inhibitors has also been observed in the clinic. In a group of 18 NSCLC patients whose cancers initially responded to EGFR TKI treatment, disease progression was associated with MET amplification for 22% of the patients (4 out of 18). Together, these observations support the concept that concomitant inhibition of both EGFR and MET might be required to maximize efficacy against cancers predisposed to employ MET amplification as a means of circumventing EGFR blockade. Identifying patients whose tumors might be predisposed to this mode of EGFR TKI resistance is a key challenge to translational researchers.
Figure 3.
Conclusions
Since their approval, EGFR TKIs have provided tremendous benefit to large numbers of cancer patients. However, we continue to face important challenges such as identifying patients a prior who are most likely to benefit from these drugs, and delaying or preventing drug-resistance. Preclinical studies have provided a platform for identifying predictive biomarkers and for broadening our understanding of mechanisms of resistance to EGFR-targeted drugs (Fig. 4). Specific activating mutations in EGFR are associated with enhanced sensitivity to EGFR TKIs. While patients with tumors harboring these activated mutant forms of EGFR initially respond well to EGFR TKIs, long term treatment can result in resistance, mediated in part by the acquisition of a secondary point mutation, T790M, within EGFR. However, preclinical data suggest that the T790M mode of resistance is unlikely to predominate for tumors of WT EGFR status.
Inhibition of both MAPK and AKT signaling is an important determinant of erlotinib sensitivity in NSCLC and pancreatic cancer models. Activating K-RAS mutations are believed by some to confer resistance to EGFR inhibitors activating the MAPK pathway downstream of EGFR. Indeed, patients with colorectal cancers harboring K-RAS mutations appear to respond poorly to anti-EGFR MAbs [47, 77]. Currently, data for the predictive value of K-RAS mutations as measure of response to EGFR TKIs is less clear. However, observations for select tumor cells where EGFR antibodies affect signaling primarily through the MAPK pathway, while EGFR TKIs can affect signaling through both the MAPK and the AKT pathway, may indicate that TKIs could be less affected by K-RAS mutations.
ErbB3 has emerged as a primary conduit for EGFR-directed AKT signaling and determinant of erlotinib sensitivity in preclinical models. ErbB3 is expressed primarily by epithelial-like cancer cells but not those that have undergone EMT. Thus, there is an emerging mechanistic link between ErbB3 and EMT with respect to understanding sensitivity and resistance to EGFR inhibitors. Furthermore, the observation that ErbB3-AKT signaling is blocked by EGFR TKIs but not by anti-EGFR MAbs further substantiates the notion that all EGFR inhibitors are not identical in terms of their spectra of activity against human cancers. Distinct sets of predictive biomarkers should be pursued for anti-EGFR MAbs and EGFR TKIs.
Complementary signaling and RTK reciprocity is an emerging concept in the context of EGFR TKIs. It is clear that EGFR and IGF-1R functionally interact in terms of ERK and AKT signaling and that combined blockade of EGFR and IGF-1R may be an effective strategy to treat a wide range of cancer and to prevent or delay the acquisition of resistance to EGFR inhibitors [68–70]. MET can also compensate for EGFR-resistance inhibition to maintain ErbB3-PI3K-AKT signaling. The combination of EGFR inhibitors and MET inhibitors promote sustained tumor growth inhibition in preclinical models. Collectively, these observations suggest that combinations of molecularly targeted drugs in molecularly-specified patient populations will be required for maximal efficacy.
References
Roskoski R Jr (2004) The ErbB/HER receptor protein–tyrosine kinases and cancer. Biochem Biophys Res Commun 319(1):1–11
Levitzki A (2003) EGF receptor as a therapeutic target. Lung Cancer 41(Suppl 1):S9–S14
Giannelli G, Napoli N, Antonaci S (2007) Tyrosine kinase inhibitors: a potential approach to the treatment of hepatocellular carcinoma. Curr Pharm Des 13(32):3301–3304
Lafky JM, Wilken JA, Baron AT, Maihle NJ (2008) Clinical implications of the ErbB/epidermal growth factor (EGF) receptor family and its ligands in ovarian cancer. Biochim Biophys Acta 1785(2):232–265
Mendelsohn J, Baselga J (2003) Status of epidermal growth factor receptor antagonists in the biology and treatment of cancer. J Clin Oncol 21(14):2787–2799
Normanno N, De Luca A, Bianco C et al (2006) Epidermal growth factor receptor (EGFR) signaling in cancer. Gene 366(1):2–16
Lee JJ, Chu E (2007) First-line use of anti-epidermal growth factor receptor monoclonal antibodies in metastatic colorectal cancer. Clin Colorectal Cancer 6(Suppl 2):S42–S46
Mano M, Humblet Y (2008) Drug Insight: panitumumab, a human EGFR-targeted monoclonal antibody with promising clinical activity in colorectal cancer. Nature Clin Practice Oncol 5:415–425
Siena S, Peeters M, Van Cutsem E et al (2007) Association of progression-free survival with patient-reported outcomes and survival: results from a randomised phase 3 trial of panitumumab. Br J Cancer 97(11):1469–1474
Johnson JR, Cohen M, Sridhara R et al (2005) Approval summary for erlotinib for treatment of patients with locally advanced or metastatic non-small cell lung cancer after failure of at least one prior chemotherapy regimen. Clin Cancer Res 11(18):6414–6421
Kim TE, Murren JR (2002) Erlotinib OSI/Roche/Genentech. Curr Opin Investig Drugs 3(9):1385–1395
Moore M (2005) Erlotinib plus gemcitabine compared to gemcitabine alone in patients with advanced pancreatic cancer. A phase III trial of the National Cancer Institute of Canada Clinical Trials Group [NCIC-CTG]. J Clin Oncol, 2005 ASCO Annual Meeting Proceedings 23(16S), Part I of II:1
Moyer JD, Barbacci EG, Iwata KK et al (1997) Induction of apoptosis and cell cycle arrest by CP-358,774, an inhibitor of epidermal growth factor receptor tyrosine kinase. Cancer Res 57(21):4838–4848
Shepherd FA, Rodrigues Pereira J, Ciuleanu T et al (2005) Erlotinib in previously treated non-small-cell lung cancer. N Engl J Med 353(2):123–132
Lemmon MA, Bu Z, Ladbury JE et al (1997) Two EGF molecules contribute additively to stabilization of the EGFR dimer. Embo J 16(2):281–294
Yarden Y (2001) The EGFR family and its ligands in human cancer. Signalling mechanisms and therapeutic opportunities. Eur J Cancer 37(Suppl 4):S3–S8
Yarden Y, Sliwkowski MX (2001) Untangling the ErbB signalling network. Nat Rev Mol Cell Biol 2(2):127–137
Penuel E, Schaefer G, Akita RW, Sliwkowski MX (2001) Structural requirements for ErbB2 transactivation. Semin Oncol 28(6 Suppl 18):36–42
Carraway KL 3rd, Sliwkowski MX, Akita R et al (1994) The erbB3 gene product is a receptor for heregulin. J Biol Chem 269(19):14303–14306
Guy PM, Platko JV, Cantley LC, Cerione RA, Carraway KL 3rd (1994) Insect cell-expressed p180erbB3 possesses an impaired tyrosine kinase activity. Proc Natl Acad Sci U S A 91(17):8132–8136
Soltoff SP, Carraway KL 3rd, Prigent SA, Gullick WG, Cantley LC (1994) ErbB3 is involved in activation of phosphatidylinositol 3-kinase by epidermal growth factor. Mol Cell Biol 14(6):3550–3558
Kim HH, Vijapurkar U, Hellyer NJ, Bravo D, Koland JG (1998) Signal transduction by epidermal growth factor and heregulin via the kinase-deficient ErbB3 protein. Biochem J 334(Pt 1):189–195
Kraus MH, Issing W, Miki T, Popescu NC, Aaronson SA (1989) Isolation and characterization of ERBB3, a third member of the ERBB/epidermal growth factor receptor family: evidence for overexpression in a subset of human mammary tumors. Proc Natl Acad Sci U S A 86(23):9193–9197
Plowman GD, Whitney GS, Neubauer MG et al (1990) Molecular cloning and expression of an additional epidermal growth factor receptor-related gene. Proc Natl Acad Sci U S A 87(13):4905–4909
Pinkas-Kramarski R, Soussan L, Waterman H et al (1996) Diversification of Neu differentiation factor and epidermal growth factor signaling by combinatorial receptor interactions. Embo J 15(10):2452–2467
Buck E, Eyzaguirre A, Haley JD, Gibson NW, Cagnoni P, Iwata KK (2006) Inactivation of Akt by the epidermal growth factor receptor inhibitor erlotinib is mediated by HER-3 in pancreatic and colorectal tumor cell lines and contributes to erlotinib sensitivity. Mol Cancer Ther 5(8):2051–2059
Kumar A, Petri ET, Halmos B, Boggon TJ (2008) Structure and clinical relevance of the epidermal growth factor receptor in human cancer. J Clin Oncol 26(10):1742–1751
Riese DJ 2nd, Gallo RM, Settleman J (2007) Mutational activation of ErbB family receptor tyrosine kinases: insights into mechanisms of signal transduction and tumorigenesis. Bioessays 29(6):558–565
Shigematsu H, Gazdar AF (2006) Somatic mutations of epidermal growth factor receptor signaling pathway in lung cancers. Int J Cancer 118(2):257–262
Sasaki H, Endo K, Takada M et al (2007) EGFR exon 20 insertion mutation in Japanese lung cancer. Lung Cancer 58(3):324–328
Lynch TJ, Bell DW, Sordella R et al (2004) Activating mutations in the epidermal growth factor receptor underlying responsiveness of non-small cell lung cancer to gefitinib. N Engl J Med 350(21):2129–2139
Sordella R, Bell DW, Haber DA, Settleman J (2004) Gefitinib-sensitizing EGFR mutations in lung cancer activate anti-apoptotic pathways. Science 305(5687):1163–1167
Sequist LV, Lynch TJ (2008) EGFR tyrosine kinase inhibitors in lung cancer: an evolving story. Ann Rev Med 59:429–442
Yun CH, Mengwasser KE, Toms AV et al (2008) The T790M mutation in EGFR kinase causes drug resistance by increasing the affinity for ATP. Proc Natl Acad Sci U S A 105(6):2070–2075
Engelman JA, Mukohara T, Zejnullahu K et al (2006) Allelic dilution obscures detection of a biologically significant resistance mutation in EGFR-amplified lung cancer. J Clin Invest 116(10):2695–2706
Pao W, Miller VA, Politi KA et al (2005) Acquired resistance of lung adenocarcinomas to gefitinib or erlotinib is associated with a second mutation in the EGFR kinase domain. PLoS Med 2(3):e73
Inukai M, Toyooka S, Ito S et al (2006) Presence of epidermal growth factor receptor gene T790M mutation as a minor clone in non-small cell lung cancer. Cancer Res 66(16):7854–7858
Blencke S, Ullrich A, Daub H (2003) Mutation of threonine 766 in the epidermal growth factor receptor reveals a hotspot for resistance formation against selective tyrosine kinase inhibitors. J Biol Chem 278(17):15435–15440
Ogino A, Kitao H, Hirano S et al (2007) Emergence of epidermal growth factor receptor T790M mutation during chronic exposure to gefitinib in a non small cell lung cancer cell line. Cancer Res 67(16):7807–7814
Balak MN, Gong Y, Riely GJ et al (2006) Novel D761Y and common secondary T790M mutations in epidermal growth factor receptor-mutant lung adenocarcinomas with acquired resistance to kinase inhibitors. Clin Cancer Res 12(21):6494–6501
Bean J, Brennan C, Shih JY et al (2007) MET amplification occurs with or without T790M mutations in EGFR mutant lung tumors with acquired resistance to gefitinib or erlotinib. Proc Natl Acad Sci U S A 104(52):20932–20937
Burgess MR, Skaggs BJ, Shah NP, Lee FY, Sawyers CL (2005) Comparative analysis of two clinically active BCR-ABL kinase inhibitors reveals the role of conformation-specific binding in resistance. Proc Natl Acad Sci U S A 102(9):3395–3400
Gorre ME, Mohammed M, Ellwood K et al (2001) Clinical resistance to STI-571 cancer therapy caused by BCR-ABL gene mutation or amplification. Science 293(5531):876–880
Godin-Heymann N, Bryant I, Rivera MN et al (2007) Oncogenic activity of epidermal growth factor receptor kinase mutant alleles is enhanced by the T790M drug resistance mutation. Cancer Res 67(15):7319–7326
Mulloy R, Ferrand A, Kim Y et al (2007) Epidermal growth factor receptor mutants from human lung cancers exhibit enhanced catalytic activity and increased sensitivity to gefitinib. Cancer Res 67(5):2325–2330
Bos JL (1989) ras oncogenes in human cancer: a review. Cancer Res 49(17):4682–4689
Amado RG, Wolf M, Peeters M et al (2008) Wild-type KRAS is required for panitumumab efficacy in patients with metastatic colorectal cancer. J Clin Oncol 26(10):1626–1634
Eng C (2008) K-Ras and sensitivity to EGFR inhibitors in metastatic colorectal cancer. Clin Adv Hematol Oncol 6(3):174–175
Thomson S, Buck E, Petti F et al (2005) Epithelial to mesenchymal transition is a determinant of sensitivity of non-small-cell lung carcinoma cell lines and xenografts to epidermal growth factor receptor inhibition. Cancer Res 65(20):9455–9462
Yauch RL, Januario T, Eberhard DA et al (2005) Epithelial versus mesenchymal phenotype determines in vitro sensitivity and predicts clinical activity of erlotinib in lung cancer patients. Clin Cancer Res 11(24 Pt 1):8686–8698
Buck E, Eyzaguirre A, Thomson S et al 2007) Differential effects for small molecule versus antibody inhibitors of EGFR: Erlotinib, but not the neutralizing antibody C225, achieves inhibition of the EGFR-HER3-Akt signaling cascade. EORTC Annual Meeting Proceedings 2007;#A128
Tsao M, Zhu C, Sakurada A et al (2006) An analysis of the prognostic and predictive importance of K-ras mutation status in the National Cancer Institute of Canada Clinical Trials Group BR.21 study of erlotinib versus placebo in the treatment of non-small cell lung cancer. J Clin Oncol 24(18S):7005
Zhu CQ, da Cunha Santos G, Ding K et al (2008) Role of KRAS and EGFR as biomarkers of response to erlotinib in National Cancer Institute of Canada Clinical Trials Group Study BR.21. J Clin Oncol 26:4268–4275
Huncharek M, Muscat J, Geschwind JF (1999) K-ras oncogene mutation as a prognostic marker in non-small cell lung cancer: a combined analysis of 881 cases. Carcinogenesis 20(8):1507–1510
Broermann P, Junker K, Brandt BH et al (2002) Trimodality treatment in Stage III nonsmall cell lung carcinoma: prrognostic impact of K-ras mutations after neoadjuvant therapy. Cancer 94(7):2055–2062
Le Calvez F, Mukeria A, Hunt JD et al (2005) TP53 and KRAS mutation load and types in lung cancers in relation to tobacco smoke: distinct patterns in never, former, and current smokers. Cancer Res 65(12):5076–5083
Ahrendt SA, Decker PA, Alawi EA et al (2001) Cigarette smoking is strongly associated with mutation of the K-ras gene in patients with primary adenocarcinoma of the lung. Cancer 92(6):1525–1530
Barr S, Thomson S, Buck E et al (2008) Bypassing cellular EGF receptor dependence through epithelial-to-mesenchymal-like transitions. Clin Exp Metastasis 25(6):685–693
Buck E, Eyzaguirre A, Barr S et al (2007) Loss of homotypic cell adhesion by epithelial-mesenchymal transition or mutation limits sensitivity to epidermal growth factor receptor inhibition. Mol Cancer Ther 6(2):532–541
Fuchs BC, Fujii T, Dorfman JD et al (2008) Epithelial-to-mesenchymal transition and integrin-linked kinase mediate sensitivity to epidermal growth factor receptor inhibition in human hepatoma cells. Cancer Res 68(7):2391–2399
Thiery JP (2003) Epithelial-mesenchymal transitions in development and pathologies. Curr Opin Cell Biol 15(6):740–746
De Craene B, Gilbert B, Stove C, Bruyneel E, van Roy F, Berx G (2005) The transcription factor snail induces tumor cell invasion through modulation of the epithelial cell differentiation program. Cancer Res 65(14):6237–6244
Thomson S, Petti F, Sujka-Kwok I, Epstein D, Haley JD (2008) Kinase switching in mesenchymal-like non-small cell lung cancer lines contributes to EGFR inhibitor resistance through pathway redundancy. Clin Exper Metastasis doi:10.1007/s10585-008-9200-4
Minn AJ, Gupta GP, Siegel PM et al (2005) Genes that mediate breast cancer metastasis to lung. Nature 436(7050):518–524
Cappuzzo F, Toschi L, Tallini G et al (2006) Insulin-like growth factor receptor 1 (IGFR-1) is significantly associated with longer survival in non-small cell lung cancer patients treated with gefitinib. Ann Oncol 17(7):1120–1127
Chakravarti A, Loeffler JS, Dyson NJ (2002) Insulin-like growth factor receptor I mediates resistance to anti-epidermal growth factor receptor therapy in primary human glioblastoma cells through continued activation of phosphoinositide 3-kinase signaling. Cancer Res 62(1):200–207
Jones HE, Goddard L, Gee JM et al (2004) Insulin-like growth factor-I receptor signalling and acquired resistance to gefitinib (ZD1839; Iressa) in human breast and prostate cancer cells. Endocr Relat Cancer 11(4):793–814
Morgillo F, Woo JK, Kim ES, Hong WK, Lee HY (2006) Heterodimerization of insulin-like growth factor receptor/epidermal growth factor receptor and induction of survivin expression counteract the antitumor action of erlotinib. Cancer Res 66(20):10100–10111
Guix M, Faber AC, Wang SE et al (2008) Acquired resistance to EGFR tyrosine kinase inhibitors in cancer cells is mediated by loss of IGF-binding proteins. J Clin Invest 118(7):2609–2619
Desbois-Mouthon C, Cacheux W, Blivet-Van Eggelpoel MJ et al (2006) Impact of IGF-1R/EGFR cross-talks on hepatoma cell sensitivity to gefitinib. Int J Cancer 119(11):2557–2566
Buck E, Eyzaguirre A, Rosenfeld-Franklin M et al (2008) Feedback mechanisms promote cooperativity for small molecule inhibitors of epidermal and insulin-like growth factor receptors. Cancer Research: in press
Engelman JA, Janne PA, Mermel C et al (2005) ErbB-3 mediates phosphoinositide 3-kinase activity in gefitinib-sensitive non-small cell lung cancer cell lines. Proc Natl Acad Sci U S A 102(10):3788–3793
Engelman JA, Zejnullahu K, Mitsudomi T et al (2007) MET amplification leads to gefitinib resistance in lung cancer by activating ERBB3 signaling. Science 316(5827):1039–1043
Benvenuti S, Comoglio PM (2007) The MET receptor tyrosine kinase in invasion and metastasis. J Cell Phys 213(2):316–325
Mazzone M, Comoglio PM (2006) The Met pathway: master switch and drug target in cancer progression. Faseb J 20(10):1611–1621
Sattler M, Salgia R (2007) c-Met and hepatocyte growth factor: potential as novel targets in cancer therapy. Curr Oncol Rep 9(2):102–108
Van Cutsem E, Lang I, D’haens G et al (2008) KRAS status and efficacy in the first-line treatment of patients with metastatic colorectal cancer (mCRC) treated with FOLFIRI with or without cetuximab: The CRYSTAL experience. J Clin Oncol 26(15S):Abstract #2.
Conflict of interest statement
The authors are currently employees at OSI Pharmaceuticals, Inc.
Open Access
This article is distributed under the terms of the Creative Commons Attribution Noncommercial License which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This is an open access article distributed under the terms of the Creative Commons Attribution Noncommercial License (https://creativecommons.org/licenses/by-nc/2.0), which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
About this article
Cite this article
Eyzaguirre, A., Buck, E., Iwata, K.K. et al. Mechanisms of resistance to EGFR tyrosine kinase inhibitors: implications for patient selection and drug combination strategies. Targ Oncol 3, 235–243 (2008). https://doi.org/10.1007/s11523-008-0093-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11523-008-0093-6