Abstract
Despite the global impact of substance misuse, there are inadequate levels of specialist service provision and continued difficulties with treatment engagement. Within policy and research, there is substantial consideration of the importance of these factors. However, there is little empirical evidence of the views of non-treatment-seeking substance users, who make up the majority of the substance using population. The aim of this study was to understand how these individuals make sense of their behaviour and their reasons for not accessing treatment. A constructivist grounded theory approach was used to interview eight individuals who were currently using substances and not seeking help to stop. The analysis highlighted the importance of attachment to an identity associated with substance use, and relational variables such as connectedness to others, for treatment decisions for individuals who use substances. Understanding these influences, through trauma- and attachment-informed service provision, may reduce barriers to help-seeking and improve treatment uptake.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Context
Problematic substance misuse is a global concern, which is prevalent in both wealthy and underprivileged countries. The World Drug Report (2019) released by the United Nations Office on Drugs and Crime (UNODC) indicated that globally, 35 million people are experiencing a drug use disorder that requires treatment. Furthermore, the report also highlighted that prevention and treatment of substance misuse continued to fall short, with only 1 in 7 people who required treatment receiving this each year. Locally in Scotland, in 2018, there was a 27% increase in drug-related deaths in comparison to the previous year. At 1187, this was Scotland’s highest number of drug-related deaths ever recorded which had more than doubled over a 10-year period (National Records of Scotland, 2019). In addition to local strategies addressing access to services and treatment retention, a need was identified for research which incorporates the preferences, priorities, and values of those with lived experience who are most at risk.
Theories of Substance Misuse
An early theory in relation to substance misuse was the “self-medication” hypothesis (Khantzian, 1997). The hypothesis suggests that individuals are vulnerable to substance misuse if they have difficulties in tolerating, regulating, and recognising their emotions. Later versions identified three further areas of vulnerability to substance misuse: (i) inability to sustain a coherent sense of self, (ii) inability to create and maintain containing, supportive relationships, and (iii) an inability to regulate behaviour, impacting on daily functioning (Khantzian, 2012). However, there has been criticism of the hypothesis’ capacity to capture the complex biopsychosocial drivers of substance misuse (Lembecke, 2012). The hypothesis also postulates that specific substances would be used to ameliorate particular affective states (e.g. alcohol for emotional suppression and cocaine for restlessness; Suh et al., 2008). However, empirical research exploring the association between affect and substance use has been inconclusive (Schindler, 2019; Tronnier, 2015).
Regulation theory builds upon the self-medication hypothesis by integrating attachment theory as a way to provide further detail in relation to the self-regulatory aspects of substance misuse (Tronnier, 2015). Positive and responsive early attachment relationships are seen as pivotal in shaping an individual’s ability to regulate arousal. Therefore, in the absence of this, an individual will be more likely to develop an insecure attachment style where they have difficulty independently managing their emotional arousal and may instead rely on external means such as substance use. Due to this, treatment interventions tend to focus on building skills in self-regulation whilst fostering attachment security within the therapeutic relationship (Waters et al., 2014). The regulatory nature of substance use in managing distress is well recognised within the clinical field. Services also acknowledge that a large majority of individuals who access support have experienced trauma. Individuals who have experienced early relational trauma may develop an insecure attachment style in an attempt to cope when caregivers have responded inconsistently or abusively to their needs. It is essential for all staff working within health and care services to be appropriately trained in relation to recognising and responding to trauma at all levels (NHS Education for Scotland, 2018).
Help-Seeking and Barriers to Recovery
Despite the global impact of substance misuse, there are inadequate levels of specialist service provision and continued difficulties with treatment engagement and retention (Boniface & Strang, 2019). Due to this, a substantial amount of research has been dedicated to exploring the factors that influence treatment engagement and drop out within substance misuse services (Heyes et al., 2016; Tsogia et al., 2001). It has been suggested that factors such as fear of experiencing emotions (which have been supressed through substance use), difficulties breaking ties with substance using communities, and institutional expectations and stigma can act as barriers to treatment (Notley et al., 2013). Many believe the construction of a non-addict identity is fundamental for the recovery process, and a key element to this process is for the individual to have a coherent biographical narrative (Giddens, 1991). Studies exploring identity and addiction have suggested that treatment engagement is often preceded by a conflict between an addict identity and one opposed to substance use, for example, being a parent or an employee (McIntosh & McKeganey, 2000; McKeganey, 2001; Shinebourne & Smith, 2009).
In contrast, very little is known about the experiences of those who encounter substantial difficulties related to their substance misuse but choose not to access treatment. The consequence of this is a large proportion of individuals with problematic substance use do not have their perspectives adequately represented in research. It is unclear whether this non-treatment-seeking population would be motivated to engage in substance misuse research. However, recent research has indicated that individuals who initially approach services but do not access treatment have still expressed enthusiasm for being involved in research (Boniface & Strang, 2019). By building a better understanding of this population, services will identify barriers to treatment and highlight potential service gaps or improvements, promoting increased treatment engagement and retention. In line with this, the primary research aim is to create an explanatory theory of how non-treatment-seeking individuals, who use substances, make sense of their behaviour, and decision not to seek treatment. In addition, the second research aim is to explore the willingness of people currently experiencing problematic substance use to be involved in research.
Method
Grounded Theory
Qualitative methods were used to produce rich data and an in-depth understanding of the research area (Corbin & Strauss, 2015). The current study adopts the constructivist grounded theory (CGT) approach which was developed by Charmaz (2014). Grounded theory involves an inductive process which allows for the development of theory as opposed to testing hypotheses (Lauridsen & Higginbottom, 2014). This process involves data collection one interview at a time and then concurrent analysis and theory development (Alemu et al., 2017). The findings from CGT research are considered to be co-constructed by the researcher and their participants as opposed to a purely objective reality which was proposed by earlier forms of grounded theory (Howard-Payne, 2016). Due to this, it is important for the researcher to consider the interaction between their own characteristics, the data they are collecting, and the influence on their interpretation. This was achieved by the researcher keeping a reflective log and through regular supervision with the research supervisor.
Participants and Recruitment
Organisations were identified where individuals who use substances may access support not directly related to addressing their substance use, including third sector, NHS, and local authority services (e.g. harm reduction, homeless services, blood-borne virus network). Staff identified individuals who met inclusion criteria and approached them to take part in the study. Inclusion criteria specified that individuals had to consider themselves to be someone who uses substances and not actively trying to stop. Individuals were excluded if they were unable to provide informed consent for study participation and/or had insufficient capability of the English language. Capacity of participants was assessed by the lead researcher prior to requesting formal written consent from each participant. Capacity to give informed consent was assessed in line with principles from Scottish government guidance (adults with incapacity: guide to assessing capacity, 2008).
Procedure
Support workers provided potential participants with both verbal and written information in relation to the study, and they were given at least 24 h to decide if they would like to take part. Interviews were conducted by the main author who liaised with support workers to identify suitable times to promote participant attendance. Participants completed a written consent form and were asked some background and demographic information (e.g. age, type of substance use, and age of first substance use). Interviews were recorded using an encrypted digital voice recorder and transcribed verbatim. A semi-structured interview schedule was developed to generate the data for the study. The initial questions were designed to act as general prompts to describe events and processes related to the individual’s substance use. These were open and general such as can you tell me a bit about your current drug use? Can you tell me about the first time you tried drugs? Or tell me about how you started using drugs in the first place? What was happening around this time? These questions allowed space for the individual to tell their story so that their current treatment decisions could be understood within this broader narrative. After every 1–2 interviews, data is analysed through open coding, and initial tentative interpretations are made, as illustrated in Table 1. These were recorded in memos and used to adapt the interview schedule prior to the next interview so that emerging categories could be explored.
Ethical Considerations
The study was approved by the NHS West Midlands–Coventry and Warwickshire Research Ethics Committee, the local NHS Research and Development Office, and the University of Edinburgh. Data was securely managed in line with the European General Data Protection Regulation (EU) 2016/679 (GDPR) and NHS code of confidentiality. Data was pseudonymised by replacing participant names with a number, and any other identifying information such as names of people or places were also removed. Participation in the study was voluntary, and participants were explicitly informed of their right to withdraw, at any time, prior to consenting to take part. Participants were also informed of the main researcher’s dual role as a trainee clinical psychologist aligned to the Addiction Psychology Service.
Data Analysis
Transcribed interviews were analysed in line with guidelines set out by Charmaz (2014). Dedoose software (version 8.3.17) was used to support the analysis and to provide an audit trail. Line-by-line coding was completed initially to identify potential paths for analysis. Focused coding was then conducted by reading and re-reading transcripts and comparing and combining initial codes to identify the theoretical direction of the analysis. Emerging themes were also explored and expanded upon during supervision with the second author. Memos were used throughout data collection and analysis to aid construction of the theoretical categories by identifying further lines of enquiry, assumptions, and comparison and connections of codes.
Sample
Purposive sampling was used to include participants who were knowledgeable and experienced in relation to substance use to provide rich data (Palinkas et al., 2015). In total, eight participants were interviewed across five different services. This included one NHS and four third sector services. Participants were all males and Scottish and aged between 25 and 52 years (M = 42.6, SD = 9.2). The length of time they had engaged with the support organisation ranged from 18 days to 6 years (M = 1.7, SD = 2 years). Six participants reported their main substance use as heroin, one reported cannabis use only, and one reported prescription medication abuse only. The age they first began using substances ranged from 13 to 32 years (M = 20.4, SD = 6.9). Interviews were conducted between December 2018 and February 2020. The length of interviews ranged from 22 to 97 min.
Barriers to Recruitment
There were a number of recruitment and data collection difficulties related to population characteristics and service pressures. Timing of the interviews had to be co-ordinated with individuals in line with their substance use. At times, this left a very short window where individuals were willing to engage and where their substance use was at a level so as not to have overly impacted on their cognitive functioning. The researcher ascertained the appropriateness of engaging a participant in the interview process by discussing the participant information leaflet and asking individuals to reflect on and repeat back information provided. This was particularly relevant for participants who reported heroin use as previous research indicates an association between opiate use and deficits in working memory, planning, impulse control, and decision-making (Loeber et al., 2012). Two interviews were cut short, one due to the individual finding it difficult to concentrate for more than a very short period which only became evident after the interview had begun. Another was halted due to a disturbance within the service. In addition, three recruited individuals moved on from the service before the interviews could take place. At the service level, there were management restructures in at least two of the recruitment organisations that delayed recruitment processes. Unfortunately, time limitations prevented recruitment from being extended.
Results
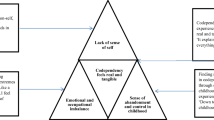
The aim of the study was to create an explanatory theory of how non-treatment-seeking individuals, who use substances, make sense of their behaviour. The model “drug identity–sense of self” is depicted in Fig. 1 and is composed of four linked theoretical categories. In summary, the model outlined indicates that participant’s attachment to their drug identify–sense of self appears to be the main explanatory variable in preventing treatment-seeking behaviour. Categories and subcategories are described in detail below using pseudononymised excerpts from interviews.
Drugs as a Self-Regulator
All participants described their substance use as essential to their day to day functioning and their primary “self-regulation strategy” (subthemes: block out thoughts and emotions, predictability and safety, managing physical pain and coping with relational trauma).
Block Out Thoughts and Emotions
All participants described an aspect of their continued substance use as a strategy to “block out” or manage difficult thoughts or emotions.
Give us a burn of that heroin you know what I mean.... They are burning their problems away you know what I mean all the pressure that is on their head. P8
So, I had that in my head and I came up the road, my anxiety was to the hilt. I would have taken anything. To take that feeling away. If the devil came to me and said I’ll take that away from you if you give me your soul I would have done it. I would have done it. P5
I think it was Just because I had been using for a long time by then and like I say I had just pulled the shutters down basically. And I was letting nothing in or out. P7
Predictability and Safety
One participant described their substance use as so intrinsically linked with their view of the self that it appeared to be impossible to imagine life without it.
Me..... I don’t know....... I don’t know what life would be like without drugs actually. P8
One participant also described their substance use as providing a sense of stability.
It’s always been.. always been there since… it’s been just me.... so it’s been me and drugs and we’ve become so close that basically drugs are my best friend. P7
Two participants also described their substance use as providing a sense of safety and protection without which they would feel exposed and restricted.
Basically, my main reason, as I say, I was on my own. So it made me feel safer. I didn’t feel so vulnerable then. It was like a shield around me sort of thing, nothing bothered me, then you know like all my emotions, nothing came into it then. P7
If I got up and tried to go out the door without a drug in me, there is no way it could happen. I would be absolutely ill. P6
Managing Physical Pain
Two participants described their initial pathway into substance misuse as a means to manage physical pain. They both identified that although this was their original motivation, they quickly recognised the additional benefit as an emotion regulation strategy.
As I say, I started taking heroin as a pain killer..the doctor had said to take half of one of my dad’s pain killers at the time......and they sort of stopped working... P1
Coping with Relational Trauma
In addition, seven out of the eight participants described their substance use as a means to cope with experiences of relational trauma with five identifying this as the point their substance use escalated or became problematic.
So I was in and out of foster carers. We used to get beaten up aff of them. My maw was a drug addict herself. So I think that’s why it spiralled out of control. My mum died 10 year ago with an overdose. P3
I was getting into a lot of trouble, not going to school. I was in a children’s home, I was coming up to my girlfriend, I just not long became a dad at 15 and I was sleeping rough. I had nowhere to live basically. I couldn’t live at home because of my stepdad….. My drug use at that time…. It was… it was recreational basically at that time, after that, that’s when it had become an everyday thing after that. P7
Being Part of a Drug Community
Participants depicted life in a “drug community” (subthemes: normalisation within a subculture, accessibility and morality) where drugs are easily accessible and normalised if you adhere to street rules and values. All participants described growing up in environments where illicit substances were readily available, and a number witnessed family substance use. Most normalised the substance use of others around them and saw this as an experience which made them feel part of a group or as understandable given the environment they lived in.
I was down the woods and I’d seen the young team basically. The troopers. So, they were all doing it and I was like I want to do that, basically. To follow the crowd. P2
Normalisation (Within a Subculture)
Two participants described an early sense of inevitability in relation to their current circumstances due to the context of the environments they grew up in.
The way that I was.... and I think I knew back then that.... that I wasn’t..... Not that I was going to end up like this.... You know disabled.... I think I knew back then that this was the way my life is going to be...... I am going to be a user. P7
I was just a.... wild child at the time you know what I mean.... I just didn’t care for nobody you know what I mean..... I was born and bred in X .....in X when you were born and bred you really had to learn to fight before you could walk you know what I mean so...... It was just the way of life you know what I mean. P8
Three participants described growing up around substances and witnessing family use. Of those, two said this led to parents being lenient in relation to their own use with the remaining participant describing an early aversion to substances due to witnessing his mum’s difficulties.
Aye, well she used to take speed all the time. She was drinking an all, all the time. That’s why I was going.. and basically f**k it, I don’t care. I’ll dae what I dae you know what I mean. If I see my maw doing it, I’m like, well she’s no caring what we’re doing, you know what I mean. P3
Accessibility
Half of the participants also identified the easy accessibility of substances as contributing to their initial and continued use.
Everybody I know..... personally..... Or just to say alright to or whatever.... Is an addict of some sort. So, it’s so easy and there’s so much of it that its.................. There’s no... There doesn’t seem to be a way of getting away from it....... Yeah, there doesn’t seem to be a way of getting away from it. P7
When you do rehab they let you out and then put you in a hostel...... What’s in a hostel as soon as you go in it?..... Drugs.... They are putting your right back into the vipers den....... You know what I mean and you’re going to get mad with it again. P8
Morality
Throughout the interviews, all participants spoke of a moral code in relation to their substance use. For some, this related only to the types of substances they would not use, but for most, this related to how they would fund their drug use. Half reported paying for substances by selling to others, some received money from family, and a number reported begging, stealing, or shoplifting to fund their use. All participants described a strong sense that it was wrong to “steal handbags” to fund their substance use. This appeared to reflect a rule that it is unacceptable to steal for small amounts from the vulnerable; however, with larger scale crime, there was almost a sense of notoriety and status. One participant noted the conflicting nature of this statement.
Well if you’ve not got four concrete walls around you then most junkies go out an…this is what gives most junkies a bad name….about 5-10% will rob grannies you know what I mean….I find it quite contradictory, in fact….if I rob you of £6 I’m a beast but if I rob you of £6000 then it’s a turn…. P1
Connection Vs Disconnection
Descriptions alluded to a “connection Vs disconnection” category (subthemes: disconnection, self-stigma, and connection) where participants felt distanced and judged by others and disconnected as a way to protect themselves.
Disconnection
Throughout the narratives, each participant described periods of disconnection from others. At times, this involved disconnecting themselves due to lack of trust or to avoid a sense of shame. This involved separation from valued relationships with children and other family members. On other occasions, families had disconnected from the participant due to their substance use, and there were disconnections through death or relationship breakdowns leading to an escalation in substance use.
I don’t know what I was trying to escape from but I think it was either.. if I had stayed I think I would either have killed myself, not deliberately but I would have died or I would have ended up in prison for a lot of.. a lot of years. So, my mum decided.. me and my mum decided that maybe it would be better if I moved away………Yes. When I was high I had no thoughts of it then. You know sort of thing. I was on my own basically. It was just me. You know. Looking after me, taking care of me. I went from recreational use maybe once or twice a week to every day. P7
I’ve got kids of my own..... I’ve got a 30, 33 year old daughter....em and....i’ve not seen her.... since she was seven... which was my choice..... Because she didn’t have to see..... Really I thought she didn’t have to see my................ The way that I was.... P7
Social networks began to narrow so that remaining connections tended to be with other substance users. This appeared to lead to a sense of disconnection from wider society and a feeling of being misunderstood and judged by the system around them.
This government isn’t interested in people like us. See if I was to get stabbed in the street..... I have been stabbed hundreds of times.. and see when I got took to the hospital the doctors don’t want to deal with you.... So I am lying there for ages pissing of blood..... You know what I mean because I’m a drug user....... P8
Self-Stigma
This sense of being judged by others appeared to lead to a focus on internal attributions in relation to control of their substance use and the development of self-stigmatising beliefs.
No, it’s just totally me. There’s no point turning around and saying I blame him or I blame him. At the end of the day it’s your fault you're the one that’s doing it. So, there’s no point in blaming Tom, Dick or Harry. You know what I mean. It’s your own fault. P6
Aye, there was like, we used to always call them junkies. See when we were younger and that. There was hunners of them about X and we would see them and we would slag them and all of that. But now, I canny say nothing, you know what I mean, I’m one of them myself….P3
Connection
One participant appeared to briefly contemplate what would motivate him to address his substance use which appeared to be related to re-establishing connections with his children.
........ The only reason I would stop taking drugs would be if I got to see my wean again........ One of my weans is down in London, she is a model you know what I mean....... My other wee lassie is coming up for 16..... So I am hoping to see her. I got told I wasn’t allowed to see her because of my previous convictions. I have 147 previous convictions for drugs, violence and firearms. So they put us down as a violent person. P8
One participant had recently secured a permanent tenancy after over 10 years of rough sleeping. He described examples of different support organisations attempting to engage with him over the years without success. The following passage illustrates how the power of feeling a genuine connection with workers led to him getting a home.
Interviewer: What do you think was helpful about the people you had around you?
Interviewee: They just cared. Blatantly in my opinion they cared and they showed it. With the other ones down there it was just a job to them. They just passed the day. That was a big difference. P6
Incoherent Sense of Self
Findings also indicated an “incoherent sense of self–stuck in the here and now” with incoherent narratives and inconsistencies when describing their sense of control over their substance use. Participants would also flit between pro-substance use standpoints and self-stigmatising statements. Linked with this, there was little future planning, a sense of inevitability in their continued substance use, and hopelessness for the future. Throughout the course of the interviews, narratives were often incoherent, jumping from one topic to another. At times, this appeared to be triggered by discussing a particularly emotive subject.
It depends how they get them. If you get them mugging old grannies and all that.... then I’ve no time for them at all. Don’t get me wrong I’ve no time for most of them. As I prefer to kind of................. See when I was at a funeral the other day... I mean that’s boys I hadn’t seen for about 20 years, some of them I could kind of recognise but they were coming up to me and going how have you been and that you know they were like you don’t remember me do you? But it was good that way you know a lot of them were happy that I was backup this end. You know. They were saying will have to come up and keep an eye on you. Haha. Apart from the occasion it was a good day. P6
During interviews, childhood trauma was often minimised with comments such as “it wasn’t that bad” or “that’s just the way it was”. When discussing childhood memories, participants were often over general, with idealised descriptions of caregivers. The participant below appeared hesitant to recall difficult episodes before acknowledging that his substance use may have been a coping strategy to deal with his experiences of trauma.
I just enjoyed. I enjoyed the high from it. em.... Maybe there was something..... That I was trying to distract myself from. Em, but it’s not something that comes to mind. There was no set thing I was trying to.... I did grow up in a ..... My step-dad was an alcoholic and em I grew up in a...in a... household where there was violence. I saw my stepdad beat my mum up and things like that... I got involved in trying to help my mum and things like that...... So I think possibly that could be where I was trying to hide from..... P7
There were also regular contradictions in relation to perceived sense of control over their substance use. Many individuals would shift from describing their substance use as a lifestyle choice that they make a conscious decision to continue to describing a sense of powerlessness and vice versa.
So I would. I’ve not got a lot of control. Over it. I don’t feel
(Later in the interview)
And if I really in my heart wanted to stop, doing what I was doing, I would stop but I enjoy it. That’s the truth I enjoy it. I enjoy that peace. P5
There also appeared to be an unwillingness or inability to forward plan or set future directed goals. Most descriptions of the future involved a sense of hopelessness or that it was too late for change.
Tomorrow was yesterday. Tomorrow is never going to come it’s always been yesterday and that’s just the way it is. And that’s the way... You know.... That’s the way it is going to stay.... P7
See the thing is, I don’t want to die but........... If I don’t wake up tomorrow morning, I don’t really.... I’m not really that a**ed to be honest........ P7
The way I see it I’ve already done all the damage to my body. You know what I mean. I think that if I was to stop I probably wouldn’t wake up you know what I mean. So I just keep on taking it for the sake of it you know what I mean. P8
One participant directly addressed the fact that he feels driven to find a coherent sense of himself within the world and the associated distress when this feels unobtainable.
I keep back from my family, I isolate. I want to be me but I don’t know who me is. P5
Discussion
The aim of the current study was to understand how individuals who use substances make sense of their behaviour and their reasons for not accessing treatment. All themes were accompanied by an incoherent sense of self and an identity enmeshed with substance use. The findings further suggest that identity and relational variables influence treatment decisions. Study participants rely on their substance use to regulate many aspects of the self. They also describe life within a community where substances are easily accessible and normalised within the moral structure of “street rules”. Relational trauma was common and often precipitated problematic substance use, leading to social disconnection. Disconnection was also described as a coping strategy to avoid distress associated with self-stigma and shame. In contrast, a sense of connection was described as leading to more positive outcomes and motivation for change. The focus on sense of self, self-regulation, relational trauma, and interpersonal connectedness to explain treatment decisions suggests that understanding barriers to help-seeking through an attachment framework may be useful.
The finding that substances were used as a regulatory strategy was perhaps expected given the vast amount of literature on regulation theory (Schore & Schore, 2008). These results also fit with previous research which explored the views of individuals who accessed treatment for their substance use, including qualitative research where service users described the “emotional levelling” effect of heroin and fear of experiencing emotions initially acting as a barrier to help-seeking (Notley et al., 2013). The common experience of disconnection is also supported by previous qualitative research where a sense of belonging (Blank et al., 2016) and relationship disconnection (Kreis et al., 2016) were identified as central to understanding substance misuse and help-seeking. It may be that the participants within the current study experienced a sense of belonging from being part of a drug community and a sense of connection from following the moral code of the streets, which acted as a barrier to addressing their substance use. Whilst there is considerable overlap with findings from studies that recruited help-seeking substance-users, it is unique to identify these characteristics in a population of non-help-seeking substance users.
The current findings may be indicative of attachment styles within this population that act as barriers to both acknowledging needs and help-seeking (Shaffer et al., 2006; Vogel & Wei, 2005). Experiences of relational trauma were common within the sample which corresponds with reported prevalence rates within substance misuse services (Charney et al., 2007; Driessen et al., 2008; Reynolds et al., 2005). Early childhood trauma is well understood as influencing self-identity and attachment development and has been related to an increased vulnerability for adult substance misuse (Stone et al., 2012). Reviews have indicated that an insecure attachment style is more common within a substance misuse population (Fairbairn et al., 2018; Iglesias et al., 2014; Schindler et al., 2005; Schindler & Bröning, 2015). Individuals with an insecure attachment style are more likely to under-report symptoms of psychological distress (Dozier & Lee, 1995) and are less likely to engage with treatment (Caspers et al., 2006). Although this research did not directly assess the attachment styles of the participants, it seems likely that the themes and the narrative style within the sample could be understood from an attachment perspective. Efforts towards disconnection and the observed disorganisation of the narratives may act as deactivating strategies with respect to potentially painful memories, (Daniel, 2009; Main, 1991), but these self-regulatory strategies prevent the development of a more coherent sense of self that feels sufficiently secure to request help from others when required. Understandably, engagement with treatment is challenging as often the first requirement is to surrender their usual coping strategy at a time when they are asked to show vulnerability by accepting support from others (Schindler, 2019). An attachment-based approach to treatment could be helpful by acknowledging that addressing substance misuse is likely to be more successful when a secure attachment is established, but the process of establishing such connection requires a thoughtful person-centred approach sensitive to the individual’s attachment needs. There is tentative support from previous research which indicated an increase in attachment security after receiving treatment for substance misuse (Gidhagen et al., 2018).
Strengths and Limitations
The study provides an important contribution to the literature on this under researched population. It also provides further support that non-treatment-seeking substance users are motivated to take part in research. As with all constructivist grounded theory research, the methodological process and final theory are influenced by the researcher’s own perceptions (Charmaz, 2014). Where possible, procedures were employed to ensure transparency and reflection including memo writing, reflexivity statement, and involvement of second author during analysis and interpretation. There was some variation in terms of substances used within the sample and settings from which they were recruited. The sample was entirely male, and there is some evidence for gender differences within substance misuse populations (Chatham et al., 1999; Holloway & Bennett, 2007; Light et al., 2013). The population may also differ from those who refused or became too unstable to take part or those with different patterns of substance misuse (e.g. alcohol only). Despite this, it is important to stress the homogeneity of the sample and that the themes described within the model were consistent across participant responses.
Implications for Future Research
Findings indicate the importance of identity and relational variables in engaging individuals in substance misuse treatment. It is worth noting that all participants were engaged with some form of support agency; therefore, an understanding of the type of help that they are willing to access out with substance misuse services is essential. Longitudinal exploration of the model, where non-treatment seekers are followed up on a regular basis, could help establish whether there are any changes in identity or relational variables when an individual seeks help. Some of the participants within the study were engaged with their support service for a number of years. Therefore, regular contact may be possible despite the complex nature of the population. The paucity of research in relation to non-treatment-seeking, at risk populations, remains evident despite national drivers to increase access to services. The current study provides further evidence that these individuals are willing to engage with research and so future projects should continue to build the evidence base with this under researched population (Fisher, 2011). Where possible, research should also be conducted collaboratively with individuals, involving them meaningfully in each level of the research process.
Implications for Clinical Practice
This research suggests that opportunities may have been overlooked to tailor treatment for those who are not accessing current substance misuse services. The model identifies a number of important factors to consider including understanding interactions within the context of attachment, the need to foster a coherent sense of self-identity and non-substance related connections, and the importance of building capacity for self-regulation. This provides further evidence for the need for staff training in relation to attachment and trauma that encourages reflection on their own attachment style to respond in a way that avoids further harm and supports recovery (Moses, 2000; Schuengel et al., 2010). In addition, appropriate structures should be in place for staff supervision and team meetings and consultation to address challenges and reduce staff burnout (Edwards et al., 2006; Schulz et al., 1995).
It is acknowledged that there are a high number of individuals who make initial contact with substance misuse services but do not commence or continue treatment (Boniface & Strang, 2019). There is a small body of research which has explored recovery from substance misuse without formal help or treatment which could inform interventions targeted at this group. Sobell and Sobell (2000) suggested that in these circumstances we should “take the treatment to the people” and that alternative interventions should be made available. This could include reaching into services where individuals are already engaged and addictions services providing input to 3rd sector organisations to skill up the keyworkers rather than having to refer elsewhere. In addition to this, individuals who make initial contact and then disengage could be provided with material that promotes self-change within an attachment-based framework. With the current findings in mind, materials could include self-regulation strategies and community resources for building connections. This could be accompanied by a therapeutic letter aimed at instilling hope and reducing self-stigma. In turn, this could promote self-change with no further need for formal services or alternatively encourage earlier service engagement.
In conclusion, the factors influencing non-treatment-seeking individual’s substance use are complex. Traumatic relational experiences are likely to lead to under-developed regulation strategies. Easy access and normalisation of substance use mean this is quickly adopted to address the attachment needs that have not been met. Continued use leads to a sense of disconnection from others, and any sense of identity or belonging is increasingly attached to a drug community. Service engagement would involve letting go of coping strategies and aspects of belonging. Disjointed narratives and inconsistencies in perceived control suggest an incoherent sense of self which impacts on the ability to forward plan and generate hope for the future. These factors may act as barriers to treatment, and it is important for services to address these issues to increase engagement and outcomes for the most vulnerable.
References
Alemu, G., Stevens, B., Ross, P., & Chandler, J. (2017). The use of a constructivist grounded theory method to explore the role of socially-constructed metadata (Web 2.0) approaches. Qualitative and Quantitative Methods in Libraries, 4(3), 517–540.
Blank, A., Finlay, L., & Prior, S. (2016). The lived experience of people with mental health and substance misuse problems: Dimensions of belonging. British Journal of Occupational Therapy, 79(7), 434–441.
Boniface, S., & Strang, J. (2019). Untreated help seekers in addiction services: An opportunity to reach under-served groups in research. Lancet Psychiatry, 7, 116.
Caspers, K. M., Yucuis, R., Troutman, B., & Spinks, R. (2006). Attachment as an organizer of behavior: Implications for substance abuse problems and willingness to seek treatment. Substance Abuse Treatment, Prevention, and Policy, 1(1), 32.
Charmaz, K. (2014). Constructing grounded theory. Sage.
Charney, D. A., Palacios-Boix, J., & Gill, K. J. (2007). Sexual abuse and the outcome of addiction treatment. American Journal on Addictions, 16(2), 93–100.
Chatham, L. R., Hiller, M. L., Rowan-Szal, G. A., Joe, G. W., & Simpson, D. D. (1999). Gender differences at admission and follow-up in a sample of methadone maintenance clients. Substance Use & Misuse, 34(8), 1137–1165.
Corbin, J., & Strauss, A. (2015). Basics of qualitative research: Techniques and procedures for developing grounded theory (4th ed.). Sage.
Daniel, S. I. (2009). The developmental roots of narrative expression in therapy: Contributions from attachment theory and research. Psychotherapy: Theory, Research, Practice, Training, 46(3), 301.
Dozier, M., & Lee, S. W. (1995). Discrepancies between self-and other-report of psychiatric symptomatology: Effects of dismissing attachment strategies. Development and Psychopathology, 7(1), 217–226.
Driessen, M., Schulte, S., Luedecke, C., Schaefer, I., Sutmann, F., Ohlmeier, M., & Broese, T. (2008). Trauma and PTSD in patients with alcohol, drug, or dual dependence: A multi-center study. Alcoholism: Clinical and Experimental Research, 32(3), 481–488.
Edwards, D., Burnard, P., Hannigan, B., Cooper, L., Adams, J., Juggessur, T., & Coyle, D. (2006). Clinical supervision and burnout: The influence of clinical supervision for community mental health nurses. Journal of Clinical Nursing, 15(8), 1007–1015.
Fairbairn, C. E., Briley, D. A., Kang, D., Fraley, R. C., Hankin, B. L., & Ariss, T. (2018). A meta-analysis of longitudinal associations between substance use and interpersonal attachment security. Psychological Bulletin, 144(5), 532.
Fisher, C. B. (2011). Addiction research ethics and the Belmont principles: Do drug users have a different moral voice? Substance Use & Misuse, 46(6), 728–741.
Giddens, A. (1991). Modernity and self-identity: Self and society in the late modern age. Stanford University Press.
Gidhagen, Y., Holmqvist, R., & Philips, B. (2018). Attachment style among outpatients with substance use disorders in psychological treatment. Psychology and Psychotherapy: Theory, Research and Practice, 91(4), 490–508.
Heyes, C. M., Baillie, A. J., Schofield, T., Gribble, R., & Haber, P. S. (2016). The reluctance of liver transplant participants with alcoholic liver disease to participate in treatment for their alcohol use disorder: An issue of treatment matching? Alcoholism Treatment Quarterly, 34(2), 233–251.
Holloway, K., & Bennett, T. (2007). Gender differences in drug misuse and related problem behaviors among arrestees in the UK. Substance Use & Misuse, 42(6), 899–921.
Howard-Payne, L. (2016). Glaser or Strauss? Considerations for selecting a grounded theory study. South African Journal of Psychology, 46(1), 50–62.
Iglesias, E. B., del Río, E. F., Calafat, A., & Hermida, J. R. F. (2014). Attachment and substance use in adolescence: A review of conceptual and methodological aspects. Adicciones, 26(1), 77–86.
Khantzian, E. J. (1997). The self-medication hypothesis of substance use disorders: A reconsideration and recent applications. Harvard Review of Psychiatry, 4(5), 231–244.
Khantzian, E. J. (2012). Reflections on treating addictive disorders: A psychodynamic perspective. The American Journal on Addictions, 21(3), 274–279.
Kreis, M. K., Gillings, K., Svanberg, J., & Schwannauer, M. (2016). Relational pathways to substance misuse and drug-related offending in women: The role of trauma, insecure attachment, and shame. International Journal of Forensic Mental Health, 15(1), 35–47.
Lauridsen, E. I., & Higginbottom, G. (2014). The roots and development of constructivist grounded theory. Nurse Researcher, 21(5), 8.
Lembke, A. (2012). Time to abandon the self-medication hypothesis in patients with psychiatric disorders. The American Journal of Drug and Alcohol Abuse, 38(6), 524–529.
Light, M., Grant, E., & Hopkins, K. (2013). Gender differences in substance misuse and mental health amongst prisoners. Results from the Surveying Prisoner Crime Reduction (SPCR) Longitudinal Cohort Study of Prisoners.
Loeber, S., Nakovics, H., Kniest, A., Kiefer, F., Mann, K., & Croissant, B. (2012). Factors affecting cognitive function of opiate-dependent patients. Drug and Alcohol Dependence, 120(1–3), 81–87.
Main, M. (1991). Metacognitive knowledge, metacognitive monitoring, and singular (coherent) vs. multiple (incoherent) models of attachment. Attachment across the Life Cycle, 127, 159.
McIntosh, J., & McKeganey, N. (2000). Addicts’ narratives of recovery from drug use: Constructing a non-addict identity. Social Science & Medicine, 50(10), 1501–1510.
McKeganey, J. M. N. (2001). Identity and recovery from dependent drug use: The addict’s perspective. Drugs: Education, Prevention and Policy, 8(1), 47–59.
Moses, T. (2000). Attachment theory and residential treatment: A study of staff-client relationships. American Journal of Orthopsychiatry, 70(4), 474–490.
Narrow, W. E., Regier, D. A., Rae, D. S., Manderscheid, R. W., & Locke, B. Z. (1993). Use of services by persons with mental and addictive disorders: Findings from the National Institute of Mental Health Epidemiologic Catchment Area Program. Archives of General Psychiatry, 50(2), 95–107.
National Records of Scotland (2019) Drug-related deaths in Scotland in 2018.
National Health Service (NHS) Education for Scotland. (2018). The delivery of psychological interventions in substance misuse services in Scotland: A guide for commissioners, managers, trainers and practitioners.
Notley, C., Blyth, A., Maskrey, V., Craig, J., & Holland, R. (2013). The experience of long-term opiate maintenance treatment and reported barriers to recovery: A qualitative systematic review. European Addiction Research, 19(6), 287–298.
Palinkas, L. A., Horwitz, S. M., Green, C. A., Wisdom, J. P., Duan, N., & Hoagwood, K. (2015). Purposeful sampling for qualitative data collection and analysis in mixed method implementation research. Administration and Policy in Mental Health and Mental Health Services Research, 42(5), 533–544.
Reynolds, M., Mezey, G., Chapman, M., Wheeler, M., Drummond, C., & Baldacchino, A. (2005). Co-morbid post-traumatic stress disorder in a substance misusing clinical population. Drug and Alcohol Dependence, 77(3), 251–258.
Shaffer, P. A., Vogel, D. L., & Wei, M. (2006). The mediating roles of anticipated risks, anticipated benefits, and attitudes on the decision to seek professional help: An attachment perspective. Journal of Counselling Psychology, 53(4), 442.
Schindler, A. (2019). Attachment and substance use disorders—Theoretical models, empirical evidence, and implications for treatment. Frontiers in Psychiatry. https://doi.org/10.3389/fpsyt.2019.00727
Schindler, A., & Bröning, S. (2015). A review on attachment and adolescent substance abuse: Empirical evidence and implications for prevention and treatment. Substance Abuse, 36(3), 304–313.
Schindler, A., Thomasius, R., Sack, P. M., Gemeinhardt, B., Kustner, U., & Eckert, J. (2005). Attachment and substance use disorders: A review of the literature and a study in drug dependent adolescents. Attachment & Human Development, 7(3), 207–228.
Schuengel, C., Kef, S., Damen, S., & Worm, M. (2010). ‘People who need people’: Attachment and professional caregiving. Journal of Intellectual Disability Research, 54, 38–47.
Schulz, R., Greenley, J. R., & Brown, R. (1995). Organization, management, and client effects on staff burnout. Journal of Health and Social Behavior, 36, 333–345.
Scottish Government. (2008). Adults with incapacity: Guide to assessing capacity. Guidance for healthcare and social work professionals.
Shinebourne, P., & Smith, J. A. (2009). Alcohol and the self: An interpretative phenomenological analysis of the experience of addiction and its impact on the sense of self and identity. Addiction Research & Theory, 17(2), 152–167.
Schore, J. R., & Schore, A. N. (2008). Modern attachment theory: The central role of affect regulation in development and treatment. Clinical Social Work Journal, 36(1), 9–20.
Sobell, L. C., Ellingstad, T. P., & Sobell, M. B. (2000). Natural recovery from alcohol and drug problems: Methodological review of the research with suggestions for future directions. Addiction, 95(5), 749–764.
Stone, A. L., Becker, L. G., Huber, A. M., & Catalano, R. F. (2012). Review of risk and protective factors of substance use and problem use in emerging adulthood. Addictive Behaviors, 37(7), 747–775.
Suh, J. J., Ruffins, S., Robins, C. E., Albanese, M. J., & Khantzian, E. J. (2008). Self-medication hypothesis: Connecting affective experience and drug choice. Psychoanalytic Psychology, 25(3), 518.
Tronnier, C. D. (2015). Harnessing attachment in addiction treatment: Regulation theory and the self-medication hypothesis. Journal of Social Work Practice in the Addictions, 15(3), 233–251.
Tsogia, A. C., & Jim Orford, D. (2001). Entering treatment for substance misuse: A review of the literature. Journal of Mental Health, 10(5), 481–499.
United Nations Office on Drugs and Crime. (UNODC, 2019). World Drug Report.
Vogel, D. L., & Wei, M. (2005). Adult attachment and help-seeking intent: The mediating roles of psychological distress and perceived social support. Journal of Counselling Psychology, 52(3), 347.
Waters, K., Holttum, S., & Perrin, I. (2014). Narrative and attachment in the process of recovery from substance misuse. Psychology and Psychotherapy: Theory, Research and Practice, 87(2), 222–236.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by SL. The first draft of the manuscript was written by SL and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethical Approval
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2000 (5). Informed consent was obtained from all participants for being included in the study. The study was approved by the NHS West Midlands–Coventry and Warwickshire Research Ethics Committee, the local NHS Research and Development office and the University of Edinburgh.
Informed Consent
All participants signed informed consent regarding publishing their anonymised data.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Lawson, S., Griffiths, H. A Grounded Theory Study: How Non-Treatment-Seeking Substance Users Make Sense of Their Behaviour “I Want To Be Me but I Don’t Know Who Me Is”. Int J Ment Health Addiction 21, 273–291 (2023). https://doi.org/10.1007/s11469-021-00592-1
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11469-021-00592-1