Abstract
Hochuekkito (HET) is a Kampo prescription, used for the clinical treatment of skin diseases such as atopic dermatitis (AD), in Japan. Oral administration of HET exerts anti-allergic effects in an experimental dermatitis mice model and in patients with atopic dermatitis; however, the mechanism underlying the anti-allergic effects of HET is still unclear. Therefore, we investigated the immunopharmacological properties of the anti-allergic actions of HET using a 2,4,6-trinitrochlorobenzene (TNCB)-induced murine contact hypersensitivity (CHS) model and adoptive cell transfer experiments. Oral administration of HET (1.4 g/kg) exhibited anti-allergic effects in a TNCB-induced CHS model via activation of Tregs; this activation was observed even without antigen sensitization in donor mice. Activation was dependent on the duration of HET administration and required at least 4 days of dosing. In addition, the anti-allergic effects of HET through the activation of Tregs were not antigen specific. Flow cytometry results indicated that the proportion of CD4+CD25+Foxp3+ cells in the splenic lymphocytes increased after oral administration of HET. Therefore, oral administration of HET induced both inducible regulatory T cells (iTregs) and thymus-derived naturally occurring regulatory T cells (nTregs). Ginseng radix and Bupleuri radix were involved in the anti-allergic actions of HET through the induction and/or activation of Tregs; Bupleuri radix participated in the activation of nTregs. In conclusion, our findings suggest that HET exerts the anti-allergic effects through the induction and/or activation of Tregs. These findings elucidate the usefulness of HET as an immunomodulator.
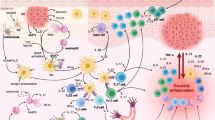
Graphical abstract











Similar content being viewed by others
Data availability
All data generated or analyzed during this study are included in this published article and its supplementary material files.
References
Miyano K, Tsunemi Y (2021) Current treatments for atopic dermatitis in Japan. J Dermatol 48:140–151
Saeki H, Huya Y, Furuta AH, Ichiyama S, Katsunuma T, Katoh N, Tanaka A, Tsunemi Y, Nakahara T, Nagao M, Narita M, Hide M, Fujisawa T, Futamura M, Masuda K, Matsubara T, Murota H, Yamamoto-Hanada K (2022) English version of clinical practice guidelines for the management of atopic dermatitis 2021. J Dermatol 49:e315–e375
Bieber T (2008) Atopic dermatitis N Eng J Med 358:1483–1494
Kabashima K (2013) New concept of the pathogenesis of atopic dermatitis: interplay among the barrier, allergy, and pruritus as a trinity. J Dermatol Sci 70:3–11
Kamata M, Tada Y (2021) A literature review of real-world effectiveness and safety of dupilumab for atopic dermatitis. JID Innovations 1:100042. https://doi.org/10.1016/j.xjidi.2021.100042
Nakajima S, Tie D, Nomura T, Kabashima K (2021) Novel pathogenesis of atopic dermatitis from the view of cytokines in mice and humans. Cytokine 148:1555664. https://doi.org/10.1016/j.cyto.2021.155664
Tominaga M, Takamori K (2022) Peripheral itch sensitization in atopic dermatitis. Allergol Int 71:265–277
Saeki H, Imamura T, Yokota D, Tsubouchi H (2022) Difamilast ointment in Japanese adult and pediatric patients with atopic dermatitis: a phase III, long-term, open-label study. Dermatol Ther 12:1589–1601
Vu YH, Hashimoto-Hachiya A, Takemura M, Yumine A, Mitamura Y, Nakahara T, Furue M, Tsuji G (2020) IL-24 negatively regulates keratinocyte differentiation induced by tapinarof, an aryl hydrocarbon receptor modulator: implication in the treatment of atopic dermatitis. Int J Mol Sci 21:9412. https://doi.org/10.3390/ijms21249412
Nakahara T, Takemoto S, Houzawa H, Nakayama M (2022) Desire for alternative treatment options in patients with atopic dermatitis in Japan: results of a web-based cross-sectional study (AD-JOIN study). Dermatol Ther 12:1383–1396
Shimizu T (2013) Efficacy of kampo medicine in treating atopic dermatitis: an overview. Evid Based Complement Altern Med. https://doi.org/10.1155/2013/260235
Nose M, Sakushima J, Harada D, Ogihara Y (1999) Comparison of immunopharmacological actions of 8 kinds of Kampo-hozais clinically used in atopic dermatitis on delayed-type hypersensitivity in mice. Biol Pharm Bull 22:48–54
Tsuge A, Yonekura S, Watanabe S, Kurosaki Y, Hisaka S, Nose M (2022) Juzentaihoto exerts anti-allergic effects by inhibiting effector T-cell activation and inducing and/or activating regulatory T cells in a murine model of contact hypersensitivity. Int Arch Allergy Immunol 183:1–13
Tsuge A, Watanabe A, Kodama Y, Hisaka S, Nose M (2022) Orengedokuto exerts anti-allergic effects via inhibition of effector T cell activation in a murine model of contact hypersensitivity. J Nat Med 76:144–151
The Ministry of Health, Labour and Welfare of Japan (2021) The Japanese pharmacopeia 18th ed., Crude drugs and related drugs. The Ministry og Health, Labour and Welfare of Japan, Tokyo. https://www.mhlw.go.jp/content/11120000/000904450.pdf
Nair AB, Jacob S (2016) A simple practice guide for dose conversion between animals and human. J Basic Clin Pharm 7:27–31
Nakada T, Watanabe K, Matsumoto T, Santa K, Triizuka K, Hanawa T (2002) Effect of orally administered Hochu-ekki-to, a Japanese herbal medicine, on contact hypersensitivity caused by repeated application of antigen. Int Immunopharmacol 2:910–911
Gao XK, Fuseda K, Shibata T, Tanaka H, Inagaki N, Nagai H (2005) Kampo medicines for mite antigen-induced allergic dermatitis in NC/Nga mice. eCAM 2:191–199
Yamashita H, Makino T, Inagaki N, Nose M, Mizukami H (2013) Assessment of relief from pruritus due to Kampo medicines by using murine models of atopic dermatitis. J Trad Med 30:114–123
Wang XQ, Takahashi T, Zhu SJ, Moriya J, Saegusa S, Yamakawa J, Kusaka K, Itoh T, Kanda T (2004) Effect of hochu-ekki-to (TJ-41), a Japanese herbal medicine, on daily activity in a murine model of chronic fatigue syndrome. eCAM 1:203–206
Jeong JS, Ryu BH, Kim JS, Park JW, Choi WC, Yoon SW (2010) Bojungikki-Tang for cancer-related fatigue: a pilot randomized clinical trial. Integr Cancer Ther 9:331–338
He Q, Sawada M, Yamasaki A, Akazawa S, Furuta H, Uenishi H, Meng X, Nakahashi T, Ishigaki Y, Moriya J (2020) Neuroinflammation, oxidative stress, and the treatment with Kampo medicine. Biol Pharm Bull 43:110–115
Kobayashi H, Mizuno N, Kutsuna H, Teramae H, Ueoku S, Onoyama J, Yamanaka K, Fujita N, Ishii M (2003) Hochu-ekki-to suppresses development of dermatitis and elevation of serum IgE level in NC/Nga mice. Drug Exp Clin Res 29:81–84
Kobayashi H, Takahashi K, Mizuno N, Kutsuna H, Ishii M (2004) An alternative approach to atopic dermatitis. Part I—Case-series presentation. eCAM 1:49–62
Kobayashi H, Takahashi K, Mizuno N, Kutsuna H, Ishii M (2004) An alternative approach to atopic dermatitis: Part II—Summary of cases and discussion. eCAM 1:145–155
Kobayashi H, Ishii M, Takeuchi S, Tanaka Y, Shintani T, Yamatodani A, Kusunoki T, Furue M (2010) Efficacy and safety of a traditional herbal medicine, Hochu-ekki-to in the long-term management of kikyo (delicate constitution) patients with atopic dermatitis: a 6 month, multicenter, double-blind, randomized, placebo-controlled study. eCAM 7:367–373
Jeong MK, Kim TE, Kim A, Jung J, Son MJ (2019) The herbal drug, Bu-Zhong-Yi-Qi-Tang, for the treatment of atopic dermatitis. Medicine 98:1–4
Gao X, Yanaka H, Inagaki N, Teramachi H, Tsuchiya T, Nagai H (2006) Immunopharmacological studies on the effects of Juzentaihoto and Hochuekkito on experimental autoimmune encephalomyelitis in rats. J Trad Med 23:196–202
Kiyomi A, Matsuda A, Nara M, Yamazaki K, Imai S, Sugiura M (2021) Immunological differences in human peripheral blood mononuclear cells treated with traditional Japanese herbal medicines Hochuekkito, Juzentaihoto, and Ninjin’yoeito from different pharmaceutical companies. eCAM. Doi: https://doi.org/10.1155/2021/7605057
Jiang S, Lechier RI (2006) CD4+CD25+ regulatory T-cell therapy for allergy, autoimmune disease and transplant rejection. Inflamm Allrgy Drug Targets 5:239–242
Miyara M, Wing K, Sakaguchi S (2009) Therapeutic approaches to allergy and autoimmunity based on FoxP3+ regulatory T-cell activation and expansion. J Allergy Clin Immunol 123:749–755
Lee JH, Cho SH (2011) Korean red ginseng extract ameliorates skin lesions in NC/Nga mice: an atopic dermatitis model. J Ethnopharmacol 133:810–817
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
11418_2023_1683_MOESM1_ESM.pdf
Supplementary file1 Fig. S1 3D-HPLC profile of hochuekkito (HET). Fig. S2 Gating strategy for analysis of CD4+CD25+FoxP3+, CD4+CD25+GITR+, and GITR+CD25+Foxp3+ cells in splenic lymphocytes administered by HET. (1) Whole cells were fractionated by side scatter (SSCs) and forward scatter (FSCc) to lymphocytes. (2, 3) Debris and doublets were discriminated. (4) Single cells were then fractionated by Fixable viability stain 575 V into living cells. (5) Living cells were fractionated by CD4. (6) CD4+ populations were then fractionated by Foxp3 and CD25 to analyze the population of CD25+ and Foxp3+ cells. (7) CD4+ populations were then fractionated by GITR and CD25 to analyze the population of GITR+ and CD25+ cells. (8) Alternatively, living cells were fractionated by CD4 and GITR to analyze the population of CD4+ and GITR+ cells. (9) CD4+ and GITR+ cells were fractionated by CD25 and Foxp3 to analyze the population of CD4+CD25+GITR+Foxp3+ cells. Fig. S3 Characterization of regulatory T cells induced and/or activated by oral administration of hots water extracts of Ginseng radix (a) and Bupleuri radix (b) using magnetic-activated cell sorting. Each column represents the mean ± SEM of 3 to 5 mice. *** p < 0.001, * p < 0.05 vs. the control group using ANOVA with Bonferroni correction for multiple comparisons. †† p < 0.01 vs. the control group using ANOVA with Bonferroni correction for the selected two group. See the Materials and Methods section for details. Fig. S4 Effect of different administration periods of hot water extract of Bupleuri radix on the induction and/or activation of regulatory T cells (Tregs) in TNCB-induced CHS response without sensitization with 5% TNCB in donor mice. (a) Experimental protocol. (b) Ear swelling 24 h after the topical application of 1% TNCB on the ear. N, normal group; Vehicle, vehicle-negative control group; CTRL, control group; BR, hot water extract of Bupleuri radix group. Each column represents the mean ± SEM of 3 to 5 mice. ***p < 0.001vs. the control group using ANOVA with Bonferroni correction for multiple comparisons. † p < 0.05 vs. the control group using ANOVA with Bonferroni correction for the selected two group. See the Materials and Methods section for details (PDF 572 KB)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Tsuge, A., Chiba, S., Yagura, Y. et al. Hochuekkito exerts the anti-allergic effects via activating regulatory T cells in a murine model of contact hypersensitivity. J Nat Med 77, 352–362 (2023). https://doi.org/10.1007/s11418-023-01683-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11418-023-01683-0