Abstract
Adolescence is a time of increased vulnerability to mental health conditions, which may necessitate hospitalization. This study sought to identify and characterize patterns of adolescent (re-)hospitalizations. The one-year (re-)hospitalization patterns of 233 adolescents were analyzed. The sequences of hospitalization and discharge was examined using cluster analyses. Results revealed five distinct (re-)hospitalization patterns or clusters: Cluster A represented brief hospitalizations with 56 cases (24.03%) averaging 7.71 days; cluster B consisted of repetitive short hospitalizations involving 97 cases (41.63%) with an average of 19.90 days; cluster C encompassed repetitive medium hospitalizations included 66 cases (28.33%) averaging 41.33 days; cluster D included long hospitalizations with 11 cases (4.72%) and an average of 99.36 days; cluster E depicted chronic hospitalizations, accounting for 3 cases (1.29%) with an average stay of 138.67 days. Despite no age-based differences across clusters, distinctions were noted in terms of sex, diagnoses, and severity of clinical and psychosocial difficulties. The study identified characteristics of both regular and atypical adolescent hospitalization users, emphasizing the distribution of hospitalization days and their associated clinical attributes. Such insights are pivotal for enhancing the organization of child and adolescent mental health services to cater to the growing care requirements of this age group.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Adolescence is an important developmental period as a precursor to a fulfilling, healthy, and balanced adult life [1]. However, many psychological and physiological changes take place during adolescence, heightening vulnerability to social challenges that can foster social insecurity and potential disorientation [2]. Indeed, the vast majority (75%) of mental health problems manifest before the age of 18, [3, 4] and approximately 40% of these young individuals continue to require care into adulthood [5, 6]. Thus, early intervention for mental health problems in adolescence represent a unique window of opportunity to alleviate future difficulties [7]. In this sense, different types of interventions, according to the clinical staging model, can be proposed depending on the status of the adolescent in distress. From this viewpoint, inpatient treatments represent one of the possible interventions, especially with the goal of treating and stabilizing acute symptomatology. [8, 9]
The goal of hospitalization is to alleviate symptoms and mitigate risks, [8, 10] ultimately promoting a functional level conducive to less intensive care or rehabilitation [11,12,13]. However, the resources for inpatient care, both in terms of public health and human capacity, are notably constrained [14]. Moreover, the hospital experience can be potentially traumatic for adolescents and can also carry the added burden or “side effect” of stigmatization [15]. However, no previous studies examined the pattern of adolescent (re-)hospitalization in the context of child and adolescent mental health service contrary to adult psychiatry or other medical conditions (for a review see [16]).
The current study
The main objective of this study is, thus, to examine the (re-)hospitalization patterns among adolescents within child and adolescent mental health service (CAMHS). Specifically, the authors aims to pinpoint distinct groups or “clusters” of adolescents with similar (re-)hospitalization patterns and examine their sociodemographic (e.g., age and sex) and clinical (e.g., diagnoses and the severity of psychosocial symptoms) characteristics.
In particular, the primary objective of this study revolves around the identification of clusters of type of inpatient (multiple) stays. The secondary objective is to examine the differences between the identified clusters in terms of sociodemographic and clinical characteristics.
By doing so, the authors hope to match resource utilization with patient profiles, ultimately refining care need. Such insight is not only academically enriching but also have clinical implications (i.e., provide the best available care for the patients who need at most) as well as for steering the clinical governance of CAMHS.
Methods
Sample
All adolescents aged 13 to 18 admitted to the psychiatric inpatient unit of the Division of Child and Adolescent Psychiatry in Lausanne at the University Hospital between 2019 and 2021 were eligible to take part in the study. Most of these patients exhibited severe behavioral or emotional challenges, often accompanied by acute suicidal ideations or behaviors, such as suicide attempts. The main objective of their hospitalization was to alleviate symptoms to a level where outpatient care, like day-care centers or ambulatory treatment, would suffice. In the unit, a multidisciplinary team, including child and adolescent psychiatrists, nurses, and pediatricians, attended to the patients.
The dataset comprised 489 inpatient stays, representing 357 distinct patients (with a single patient having up to six recorded inpatient stays). The information includes hospitalization dates, basic available sociodemographic data (age and sex), and clinical characteristics (diagnosis as well as clinical and psychosocial difficulties) from institutional medical records. The study was approved by the Ethics Committee of the Vaud Canton (#2022–01217).
Measures
The age, sex, and the International Classification of Diseases (ICD) diagnosis has been extracted. In addition, clinicians consistently employed the Health of the Nation Outcome Scales for Children and Adolescents (HoNOSCA [17,18,19]) to assess the severity of clinical and psychosocial difficulties. The HoNOSCA consists of 15 items, with each scored on a 5-point Likert scale ranging from 0 (no problem) to 4 (severe to very severe problem). In the current study, only the initial 13 items were used, as they pertained directly to patient difficulties, while the last two items did not. Notably, the reliability of these final two items has been questioned [20]. The total score represented the severity of clinical and psychosocial difficulties, with higher scores indicating pronounced difficulties. The HoNOSCA has been rated by trained clinicians with the context of clinical routine assessment. Clinicians used all the available source of information (from youths, parents, other health professional) to rate the items of the HoNOSCA.
Data analyses
The analytical methods mirrored those previously implemented in an adult psychiatry study [21]. Analyses were performed using the R software [22]. First, to address the main objective (i.e., identifying patterns of inpatient use), the authors used the TraMineR package [23] allowing the analysis of discrete event sequences, specifically hospitalization dates spanning a year. These sequences were treated as states. By using the “optimal matching algorithm,” the authors calculated the dissimilarity for each pair of sequences. This algorithm determines edit distances that reflect the least-costly means of transforming one sequence into another through insertions, deletions, or substitutions [24]. It enabled the calculation of a dissimilarity matrix for each patient. Subsequently, the authors computed a cluster analysis on this matrix employing the Ward method [25]. The criteria for identifying clusters were interpretability, the number of prototypical sequences, and the size of the clusters. The clusters were interpreted using visualization and statistical tools that enabled us to extract one or several sequences deemed statistically representative of the entire group. [26]
To address the second objective, which aimed to assess differences in sociodemographic and clinical characteristics between patterns, the authors used a Bayesian statistical approach. This approach offers a solution to the multiple comparisons dilemma [27,28,29]. Specifically, the first model, the homogenous one (A = B = C = D = E), posited that the five groups were undifferentiated. Conversely, the heterogeneous model (A ≠ B ≠ C ≠ D ≠ E) posited complete differentiation among all groups. The authors examined all intermediate possibilities to identify the most probable and fitting model. For this purpose, the authors employed the Bayes R2STATS group models calculator. [30]
Results
The authors adjusted the data to initiate each sequence with the patient's first hospitalization. Then, the patterns of (re-)hospitalizations were followed over a 1-year period. Consequently, based on the 357 distinct patients, the authors analyzed the data of 233 patients for whom a full year of follow-up data are available.
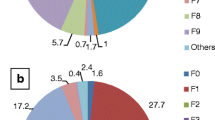
Within this group, there were a total of 6,522 hospitalization days. The average age of patients was 15.73 years (SD = 1.15), and 65.7% (n = 153) were female. The ICD diagnoses were distributed as follows: 10.4% (n = 24) had mental disorders due to the use of psychoactive substances (F1.x); 10.0% (n = 23) had schizophrenia spectrum disorders (F2.x); 32.2% (n = 74) exhibited mood (affective) disorders (F3.x); 33.5% (n = 77) presented with anxiety or obsessive–compulsive disorders (F4.x); 0.9% (n = 2) showed eating and sleeping disorders (F5.x); 2.6% (n = 6) were diagnosed with disorders of personality (F6.x); 0.9% (n = 2) had intellectual disabilities (F7.x); 1.3% (n = 3) showed disorders of psychological development (F84.9);and, finally, 8.3% (n = 19) had behavioral and emotional disorders (F9.x).
Upon segmenting the data into an increasing number of clusters, the authors identified five meaningful clusters (Fig. 1). An attempt to extract a sixth cluster did not yield further clarity or distinction in the usage patterns. Consequently, the authors settled on a five-cluster solution, detailed below.
Initially, the patients may be distinguished between the regular “moderate” users, accounting for 93.99% (n = 219) of the sample, and the atypical “heavy” users, making up 6.01% (n = 14; Fig. 1). Notably, the “moderate” users represented 78.04% of total hospitalization days, whereas the “heavy” users represented the remaining 21.96%. Approximately 20% of the number of hospitalization days are allocated to only 6% of the patients. On the opposite end of the spectrum, patients with brief hospitalizations (24%) refer to only about 6% of total hospitalization days. Within the regular “moderate” user category, three primary clusters were discerned: A. Brief hospitalization comprising 24.03% (n = 56) of users with an average duration (Mdays) of 7.71 days; B. Repetitive short hospitalizations consisting of 41.63% (n = 97) of users with Mdays = 19.90; C. Repetitive medium hospitalizations representing 28.33% (n = 66) of users with an average stay of Mdays = 41.33. Among the atypical users, the authors identified two clusters: D. Long hospitalizations: 4.72% (n = 11) with a hospitalization duration averaging Mdays = 99.36; E. Chronic hospitalizations 1.29% (n = 3) whose stays averaged Mdays = 138.67.
Each cluster represents a unique pattern. In particular, Cluster A represented brief hospitalizations, primarily singular events, Cluster B was characterized by repetitive re-hospitalizations of short duration, Cluster C referred to frequent re-hospitalization of medium-term duration, Cluster D corresponded to multiple extended hospital stays, whereas as Cluster E was indicative of chronic hospitalization of long-term duration (Fig. 2).
Bayesian statistical analyses suggested significant differences in the number of hospitalization days across these clusters (Table 1). A consistent increase in service use was observed from cluster A to cluster E.
To better understand the distinctions among the clusters, the differences between them in terms of age, sex, diagnosis and symptom severity were evaluated (Table 2). The results did not reveal any differences in terms of age. However, there were notable differences in the gender distributions: clusters A (brief hosp.), B (repetitive short hosp.), and C (repetitive medium hosp.) had a higher proportion of girls, while boys were more predominant in clusters D (long hosp.) and E (chronic hosp.). It is important to note that clusters D (long hosp.) and E (chronic hosp.) together comprised only 14 patients. Moreover, the authors observed differences in terms of diagnosis between the clusters. In particular, youths from cluster A (brief hosp.) had mainly anxiety or obsessive–compulsive disorders, whereas those in clusters B (repetitive short hosp.), C (repetitive medium hosp.), D (long hosp.), and E (chronic hosp.) demonstrated a more varied diagnostic profile. In addition, youths from clusters A (brief hosp.) and B (repetitive short hosp.) exhibited milder symptoms and fewer psychosocial difficulties, as reflected by their lower HoNOSCA scores. Conversely, youths in clusters C (repetitive medium hosp.), D (long hosp.), and E (chronic hosp.) presented with more severe symptoms and greater psychosocial difficulties.
Discussion
Similar (re-)hospitalization patterns were identified and their sociodemographic and clinical characteristics were examined. Five distinct clusters emerged from the analysis: A: Brief hospitalization; B: Repetitive short hospitalizations; C: Repetitive medium hospitalizations; D: Long hospitalizations; E: Chronic hospitalizations. Although the duration and frequency of hospitalizations varied across clusters, the age of patients did not vary significantly among the clusters. Moreover, there were noticeable differences in terms of gender, diagnoses, and the extent of symptoms severity and psychosocial challenges faced by the patients.
Patterns of (re-)hospitalization and service organization
The identified clusters in this study are largely consistent with those from previous research examining similar patterns or trajectories in adults psychiatry [21, 31, 32]. Indeed, the ratio between the number of patients and the hospitalization days (a small number of patients necessitate a large number of hospitalization is similar to what was observed in adult psychiatry, where this pattern were observed to be even more pronounced in adult psychiatry where roughly 5% of patients consume a total of 30% of the resources) [21]. Thus, the most severe and chronic cases which represent few adolescents need the most hospitalization days (or resources).
This may be understood in the light of the “stepped care” approach [33,34,35]. It tailors treatment responses to the patient's clinical stage and needs [36, 37] and may guide the organization of the hospitalization. In that sense, the efficacy of repetitive short stays is often debated, especially when considering the potential adverse effects of hospitalizations [15]. If CAMHS organizations were structured differently, there could be a bolstering of intermediate or outpatient structures (e.g., intensive community treatment, short-stay day care centers, and specialized short-term inpatient crisis units) to prevent such re-hospitalizations. Such structures aim to decrease the need for hospitalizations for adolescents while supporting continuity of care and offering them the most appropriate treatment to sustain their ongoing development. According to this approach, only patients with the most severe difficulties should be hospitalized. Thus, it emphasizes the relevant or “smarter” utilization or “smarter medicine” [38] of inpatient facilities, underscoring the importance of comprehending trends.
Sociodemographic variables related to the different patterns of (re-)hospitalization
In the analyses of the five clusters, results revealed no age-based differences, a finding consistent with a study on the adult population using analog procedure [21]. More generally, a recent systematic review of the literature [39] yielded inconsistent results. Some studies within this review [39] associated a higher risk of re-hospitalization with younger age, while others found the opposite trend. In another study with a mixed-age population (ranging from 15 to 64 y.o [40]), younger age was found to be predictive of an increased risk of the repetitive medium hospitalization phenomenon.
In the current study, females were overrepresented in the typical user clusters and underrepresented the atypical user. This is somewhat aligned with findings from a systematic review [39], where a majority of studies found an association between being female and an increased risk of re-hospitalization. As for clusters D (long hosp.) and E (chronic hosp.), the underrepresentation of females might be partially due to a significant proportion of patients in these clusters being diagnosed with schizophrenia spectrum disorders. This diagnosis is more prevalent in males than in females, with the difference being particularly marked up to the age of 25 [41,42,43]. Moreover, it should be noted that clusters D (long hosp.) and E (chronic hosp.) represent only 14 patients, which could influence these findings. In addition, this discrepancy can be partly attributed to the overrepresentation of females in the sample.
Distinct clinical profiles of hospitalized patients
To summarize, results revealed three main profiles of hospitalized patients. The first profile, represented by cluster A (brief hospitalization with an average duration of 7.71 days), comprised patients exhibiting acute symptomatology and with mild impairment in psychosocial functioning. For these individuals, a brief hospitalization, typically singular, serves to address the immediate crisis and possibly alleviate the external factors contributing to it. This is supported by the fact that re-hospitalization rarely re-occurred within a year. These individuals, who show clinical benefits from a single hospitalization, are best treated during their acute phases in short-stay hospitalization units which is consistent with the hospitalization’s goal to alleviate symptoms [8, 10] and promote functional level [11,12,13].
The second profile encompasses patients from clusters B (repetitive short hospitalizations with an average duration across hospitalizations of 19.90 days) and C (repetitive medium hospitalizations with an average of 41.33 days). These patients are marked by their propensity for re-hospitalization, which differs in frequency and length, with the repetitive medium hospitalizations group experiencing more prolonged and frequent stays. Predominantly, this group was diagnosed with mood disorders and displayed subpar psychosocial functioning. These patients together accounted for 70% of the patients and 70% of the hospitalization days. Given the high re-hospitalization rate, the authors assumed that a different management strategy needs to be developed for these patients [44]. Indeed, while traditional hospitalization proved beneficial, these patients consumed a significant portion of the available hospital days.
The third profile, represented by clusters D (long hospitalizations with an average duration of 99.36 days) and E (chronic hospitalizations with an average of 138.67 days), consisted of patients with the most severe diagnoses and the most compromised psychosocial functioning which is consistent with previous findings [45, 46]. Although this group generally benefited from traditional hospitalization, an extended duration was necessary to achieve symptom remission that aligned with outpatient treatment standards. Yet, prolonged hospital stays can introduce adverse consequences such as stigmatization and de-socialization [15]. Given these considerations, re-evaluating the efficacy and suitability of extended hospitalizations, particularly for clusters D and E, becomes paramount. While a hospital environment is undeniably beneficial during acute phases, longer-term treatment might find greater success in social-health facilities aimed at fostering reintegration into the patient's natural social setting. Adopting this approach could also free up critical resources within acute inpatient units for more urgent cases.
Limitations and future perspectives
This study has several limitations. Firstly, owing to its retrospective design based on clinical data, it offers limited insights into the clinical condition of the patients. While future studies might benefit from a prospective design, the essential attributes (due to retrospective study of data collected in routine clinical care) for clinical characterization of the clinical and socio-demographic variables, such as age, sex, and diagnoses, were the only available information in this research. Additionally, the analysis was confined to a 1-year period. A more extended study might yield additional insights, such as patterns observable over a longer timeframe. It is also worth noting that the data might have been influenced by the impact of the sanitary crisis on youth mental health. Moreover, the authors did not have access to the type of familial, social and/or community support that the youths may benefit after the hospitalization. This may impact the youths’ ability to adhere to treatment recommendations upon discharge and ultimately their ability to access the outpatient services and resources. In future research endeavors, adopting a more comprehensive approach that encompasses various treatment modalities, such as outpatient care, daycare, and assertive community treatment, could be beneficial (see for instance [47]).
Conclusion
This study identifies five distinct patterns of re-hospitalization which varies in terms of socio-demographic variables as well as of clinical characteristics. In particular, results revealed three main profiles of patients’ characteristics related to their need of (re-)hospitalization. Further studies should involve a deeper exploration of these hospitalization patterns and beyond by including other type of treatment as well as by incorporating a broader range of sociodemographic and clinical characteristics. Such research endeavors can help identify patients who may require extended stays or utilize more clinical resources, enabling tailored clinical settings to offer optimal care.
Implications for Behavioral Health
In this study, results revealed at least three profiles of hospitalized patients according to the number of re-hospitalization and their duration. In this sense, the authors observed that the most severe and chronic cases, which represent a small percentage of the total number of hospitalized adolescents, need the most days of hospitalization. This clearly shows how the needs in terms of therapeutic interventions can be extremely variable in hospitalized patients.
Accordingly, the early identification of the distinct clinical profiles may help to facilitate patient’s trajectory within the available care and, thus, may reduce their distress and optimize the best clinical and functional outcomes. This would clearly have a positive effect not only on the adolescent but also on his family context, which often experiences hospitalization as something traumatic. Moreover, at a health care system level, this would represent an opportunity to optimize the allocation of resources in accordance with the real needs and to articulate the different care options. Thus, the identification of different hospitalization profiles leads to a number of implications for the behavioral health. First, recognizing different profiles of hospitalized patients allows healthcare providers to develop personalized treatment plans. By understanding that some cases are more severe and chronic, resources can be allocated appropriately, and tailor interventions can be developed to meet the specific needs of each patient. Second, by identifying a small percentage of patients require a disproportionate amount of hospitalization days suggests that resources should be allocated strategically. This might involve ensuring sufficient staffing, specialized care, and support services for these more complex cases. Third, by requiring extended hospital stays, long-term care planning becomes crucial. This could involve coordination with community resources, rehabilitation services, and specialists to ensure continuity of care beyond the hospital settings. Four, patients with a history of re-hospitalization may require closer monitoring and follow-up care to prevent future readmissions. This might involve regular follow-ups and mental health and social support to address underlying issues contributing to repeated hospitalizations. Five, by providing education to patients and their families about the variability in therapeutic needs among hospitalized patients can help manage expectations and empower them to be proactive in their care. Understanding the potential for longer hospital stays in certain cases can also facilitate better decision-making and coping strategies.
Thus, the current results help to think the personalized need of the patients and the corresponding organization of CAMHS to address their specific difficulties.
Data Availability
The data that support the findings of this study are not publicly available due to data protection of the participants, but may be available from the corresponding author upon reasonable request.
References
Yurgelun-Todd D. Emotional and cognitive changes during adolescence. Current Opinion in Neurobiology. Apr 2007;17(2):251–7. Available at https://doi.org/10.1016/j.conb.2007.03.009. Accessed 15 November, 2023.
Silk JS, Steinberg L, Morris AS. Adolescents' emotion regulation in daily life: Links to depressive symptoms and problem behavior. Child Development. Nov-Dec 2003;74(6):1869–80. Available at https://doi.org/10.1046/j.1467-8624.2003.00643.x. Accessed 15 November, 2023.
Kim-Cohen J, Caspi A, Moffitt TE, et al. Prior juvenile diagnoses in adults with mental disorder: developmental follow-back of a prospective-longitudinal cohort. Archives of General Psychiatry. Jul 2003;60(7):709–17. Available at https://doi.org/10.1001/archpsyc.60.7.709. Accessed 15 November, 2023.
Kessler RC, Berglund P, Demler O, et al. Lifetime prevalence and age-of-onset distributions of DSM-IV disorders in the national comorbidity survey replication. Archives of General Psychiatry. Jun 2005;62(6):593–602. Available at https://doi.org/10.1001/archpsyc.62.6.593. Accessed 15 November, 2023.
Hofstra MB, van der Ende J, Verhulst FC. Child and adolescent problems predict DSM-IV disorders in adulthood: a 14-year follow-up of a Dutch epidemiological sample. Journal of the American Academy of Child & Adolescent Psychiatry. Feb 2002;41(2):182–9. Available at https://doi.org/10.1097/00004583-200202000-00012. Accessed 15 November, 2023.
Fombonne E. Epidemiology of psychiatric disorders paediatric psychiatry. EMC-Psychiatry. Aug 2005;2(3):169–194. Available at https://doi.org/10.1016/j.emcps.2005.06.001.
Fuhrmann D, Knoll LJ, Blakemore SJ. Adolescence as a sensitive period of brain development. Trends in Cognitive Science. Oct 2015;19(10):558–566. Available at https://doi.org/10.1016/j.tics.2015.07.008. Accessed 15 November, 2023.
Lamb CE. Alternatives to admission for children and adolescents: Providing intensive mental healthcare services at home and in communities: what works? Current Opinion in Psychiatry. Jul 2009;22(4):345–50. Available at https://doi.org/10.1097/YCO.0b013e32832c9082. Accessed 15 November, 2023.
Hayes C, Simmons M, Simons C, et al. Evaluating effectiveness in adolescent mental health inpatient units: A systematic review. International Journal of Mental Health Nursing. Apr 2018;27(2):498–513. Available at https://doi.org/10.1111/inm.12418. Accessed 15 November, 2023.
Mathai J, Bourne A. Patients who do well and who do less well in an inpatient adolescent unit. Australasian Psychiatry. Aug 2009;17(4):283–6. Available at https://doi.org/10.1080/10398560902842501. Accessed 15 November, 2023.
Blanz B, Schmidt MH. Preconditions and outcome of inpatient treatment in child and adolescent psychiatry. Journal of Child Psychology and Psychiatry. Sep 2000;41(6):703–12. Available at https://doi.org/10.1111/1469-7610.00658. Accessed 15 November, 2023.
Greenham SL, Bisnaire L. An outcome evaluation of an inpatient crisis stabilization and assessment program for youth. Residential Treatment for Children & Youth. 2008;25:123–143. Available at https://doi.org/10.1080/08865710802310012. Accessed 15 November, 2023.
Hanssen-Bauer K, Heyerdahl S, Hatling T, et al. Admissions to acute adolescent psychiatric units: a prospective study of clinical severity and outcome. International Journal of Mental Health Systems. Jan 6 2011;5(1):1. Available at https://doi.org/10.1186/1752-4458-5-1. Accessed 15 November, 2023.
Mason MA, Gibbs JT. Patterns of adolescent psychiatric hospitalization: Implications for social policy. American Journal of Orthopsychiatry. Jul 1992;62(3):447–57. Available at https://doi.org/10.1037/h0079361. Accessed 15 November, 2023.
Jina-Pettersen N. Fear, neglect, coercion, and dehumanization: Is inpatient psychiatric trauma contributing to a public health crisis? Journal of Patient Experience. 2022;9:23743735221079138. Available at https://doi.org/10.1177/23743735221079138. Accessed 15 November, 2023.
Mathew S, Peat G, Parry E, et al. Applying sequence analysis to uncover 'real-world' clinical pathways from routinely collected data: a systematic review. Journal of Clinical Epidemiology. Feb 2024;166:111226. Available at https://doi.org/10.1016/j.jclinepi.2023.111226. Accessed 15 March, 2024.
Gowers SG, Harrington RC, Whitton A, et al. Health of the nation outcome scales for children and adolescents (HoNOSCA). Glossary for HoNOSCA score sheet. British Journal of Psychiatry. May 1999;174:428–31. Available at https://doi.org/10.1192/bjp.174.5.428. Accessed 15 November, 2023.
Gowers SG, Harrington RC, Whitton A, et al. Brief scale for measuring the outcomes of emotional and behavioural disorders in children. Health of the nation outcome scales for children and adolescents (HoNOSCA). British Journal of Psychiatry. May 1999;174:413–6. Available at https://doi.org/10.1192/bjp.174.5.413. Accessed 15 November, 2023.
Holzer L, Tchemadjeu IK, Plancherel B, et al. Adolescent drug abuse diagnosis (ADAD) vs. health of nation outcome scale for children and adolescents (HoNOSCA) in clinical outcome measurement. Journal of Evaluation in Clinical Practice. Oct 2006;12(5):482–90. Available at https://doi.org/10.1111/j.1365-2753.2006.00654.x. Accessed 15 November, 2023.
Pirkis JE, Burgess PM, Kirk PK, et al. A review of the psychometric properties of the Health of the Nation Outcome Scales (HoNOS) family of measures. Health and Quality of Life Outcomes. Nov 28 2005;3:76. Available at https://doi.org/10.1186/1477-7525-3-76. Accessed 15 November, 2023.
Golay P, Morandi S, Conus P, et al. Identifying patterns in psychiatric hospital stays with statistical methods: towards a typology of post-deinstitutionalization hospitalization trajectories. Social Psychiatry and Psychiatric Epidemiology. Nov 2019;54(11):1411–1417. Available at https://doi.org/10.1007/s00127-019-01717-7. Accessed 15 November, 2023.
Team RC. R: A language and environment for statistical computing. R Foundation for Statistical Computing; 2018. R Foundation for Statistical Computing, Vienna, Austria. Available at https://www.R-project.org/.
Gabadinho A, Ritschard G, Mueller N, et al. Analyzing and visualizing state sequences in R with TraMineR. Journal of Statistical Software. 2011;40(4):1–37. Available at https://doi.org/10.18637/jss.v040.i04.
Gabadinho A, Ritschard G, Studer M, et al. Mining sequence data in R with the TraMineR package: a users guide for version 1.2. Available at http://traminer.unige.ch. University of Geneva; 2009.
Ward JH. Hierarchical grouping to optimize an objective function. Journal of the American Statistical Association. 1963;58:236–244. Available at https://doi.org/10.1080/01621459.1963.10500845.
Gabadinho A, Ritschard G, Studer M, et al. Extracting and rendering representative sequences. In: A. Fred, J. L. G. Dietz, K. Liu, and J. Filipe, editors, Knowledge discovery, knowledge engineering and knowledge management, Vol. 128. Springer-Verlag; 2011b. pp. 94–106.
Noël Y. Psychologie statistique avec R. EDP Sciences. 2015.
Golay P, Laloyaux J, Moga M, et al. Psychometric investigation of the French version of the Aberrant Salience Inventory (ASI): differentiating patients with psychosis, patients with other psychiatric diagnoses and non-clinical participants. Annals of General Psychiatry. 2020;19:58. Available at https://doi.org/10.1186/s12991-020-00308-0. Accessed 15 November, 2023.
Golay P, Morandi S, Silva B, et al. Feeling coerced during psychiatric hospitalization: Impact of perceived status of admission and perceived usefulness of hospitalization. International Journal of Law and Psychiatry. Nov-Dec 2019;67:101512. Available at https://doi.org/10.1016/j.ijlp.2019.101512. Accessed 15 November, 2023.
Noël Y. R2STATS Group models; http://yvonnick.noel.free.fr/r2statsweb/bayes.html/. Accessed 3 April 2023,
Han X, Jiang F, Needleman J, et al. A sequence analysis of hospitalization patterns and service utilization in patients with major psychiatric disorders in China. BMC Psychiatry. May 11 2021;21(1):245. Available at https://doi.org/10.1186/s12888-021-03251-w. Accessed 15 November, 2023.
Han XY, Jiang F, Zhou HX, et al. Hospitalization pattern, inpatient service utilization and quality of care in patients with alcohol use disorder: A sequence analysis of discharge medical records. Alcohol Alcoholism. Mar 2020;55(2):179–186. Available at https://doi.org/10.1093/alcalc/agz081. Accessed 15 March, 2024.
Berger M, Fernando S, Churchill A, et al. Scoping review of stepped care interventions for mental health and substance use service delivery to youth and young adults. Early Intervention in Psychiatry. Apr 2022;16(4):327–341. Available at https://doi.org/10.1111/eip.13180. Accessed 15 November, 2023.
Davison GC. Stepped care: Doing more with less? Journal of Consulting and Clinical Psychology. Aug 2000;68(4):580–5. Available at https://doi.org/10.1037/0022-006X.68.4.580. Accessed 15 November, 2023.
Richards DA. Stepped care: A method to deliver increased access to psychological therapies. Canadian Journal of Psychiatry. Apr 2012;57(4):210–5. Available at https://doi.org/10.1177/070674371205700403. Accessed 15 November, 2023.
McGorry PD, Mei C, Chanen A, et al. Designing and scaling up integrated youth mental health care. World Psychiatry. Feb 2022;21(1):61–76. Available at https://doi.org/10.1002/wps.20938. Accessed 15 November, 2023.
Thornicroft G, Tansella M. Components of a modern mental health service: A pragmatic balance of community and hospital care: overview of systematic evidence. British Journal of Psychiatry. Oct 2004;185:283–90. Available at https://doi.org/10.1192/bjp.185.4.283. Accessed 15 November, 2023.
Amstad H, Gaspoz JM, Zemp L. Guidelines and choosing wisely: To do’s and not to do’s. BMS. 2015;96:130–1. Available at. Accessed 15 March, 2024.
Madden A, Vajda J, Llamocca EN, et al. Factors associated with psychiatric readmission of children and adolescents in the U.S.: A systematic review of the literature. General Hospital Psychiatry. Jul-Aug 2020;65:33–42. Available at https://doi.org/10.1016/j.genhosppsych.2020.05.004. Accessed 15 November, 2023.
Lewis T, Joyce PR. The new revolving-door patients: results from a national cohort of first admissions. Acta Psychiatrica Scandinavica. Aug 1990;82(2):130–5. Available at https://doi.org/10.1111/j.1600-0447.1990.tb01369.x. Accessed 15 November, 2023.
Aleman A, Kahn RS, Selten JP. Sex differences in the risk of schizophrenia: evidence from meta-analysis. Archive of General Psychiatry. Jun 2003;60(6):565–71. Available at https://doi.org/10.1001/archpsyc.60.6.565. Accessed 15 November, 2023.
Fernando P, Sommer IEC, Hasan A. Do we need sex-oriented clinical practice guidelines for the treatment of schizophrenia? Current Opinion in Psychiatry. May 2020;33(3):192–199. Available at https://doi.org/10.1097/YCO.0000000000000597. Accessed 15 November, 2023.
Li X, Zhou W, Yi Z. A glimpse of gender differences in schizophrenia. General Psychiatry. 2022;35(4):e100823. Available at https://doi.org/10.1136/gpsych-2022-100823. Accessed 15 November, 2023.
Grenyer BFS, Lewis KL, Fanaian M, et al. Treatment of personality disorder using a whole of service stepped care approach: A cluster randomized controlled trial. PLoS One. 2018;13(11):e0206472. Available at https://doi.org/10.1371/journal.pone.0206472. Accessed 15 November, 2023.
Connell S.K., Rutman L.E., Whitlock K.B., et al. Health care reform, length of stay, and readmissions for child mental health hospitalizations. Hospital Pediatrics. 2020;Available at https://doi.org/10.1542/hpeds.2019-0197. Accessed 15 November, 2023.
Di Lorenzo R, Montardi G, Panza L, et al. Retrospective analysis of factors associated with long-stay hospitalizations in an acute psychiatric ward. Risk Manag Healthc P. 2020;13:433–442. Available at https://doi.org/10.2147/Rmhp.S238741. Accessed 15 November, 2023.
Puntis S, Pappa S, Lennox B. What happens after early intervention? Mapping early intervention in psychosis care pathways in the 12 months after discharge. Early Intervention in Psychiatry. Jan 2024;18(1):49–57. Available at https://doi.org/10.1111/eip.13433. Accessed 15 March, 2024.
Funding
Open access funding provided by University of Lausanne
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics Approval
Ethical approval was waived by the Ethics Committee of the Vaud Canton (#2022–01217) in view of the retrospective nature of the study and all the procedures being performed were part of the routine care.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Urben, S., Golay, P., Forte, A. et al. Identification of Patterns of Hospitalizations in Child and Adolescent Mental Health Service. J Behav Health Serv Res (2024). https://doi.org/10.1007/s11414-024-09887-2
Accepted:
Published:
DOI: https://doi.org/10.1007/s11414-024-09887-2