Abstract
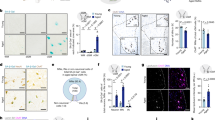
Age-related muscle weakness and loss of muscle mass (sarcopenia) is a universal problem in the elderly. Our previous studies indicate that alpha motor neurons (α-MNs) play a critical role in this process. The goal of the current study is to uncover changes in the aging spinal cord that contribute to loss of innervation and the downstream degenerative processes that occur in skeletal muscle. The number of α-MNs is decreased in the spinal cord of wildtype mice during aging, beginning in middle age and reaching a 41% loss by 27 months of age. There is evidence for age-related loss of myelin and mild inflammation, including astrocyte and microglia activation and an increase in levels of sICAM-1. We identified changes in metabolites consistent with compromised neuronal viability, such as reduced levels of N-acetyl-aspartate. Cleaved caspase-3 is more abundant in spinal cord from old mice, suggesting that apoptosis contributes to neuronal loss. RNA-seq analysis revealed changes in the expression of a number of genes in spinal cord from old mice, in particular genes encoding extracellular matrix components (ECM) and a 172-fold increase in MMP-12 expression. Furthermore, blood-spinal cord barrier (BSCB) permeability is increased in old mice, which may contribute to alterations in spinal cord homeostasis and exacerbate neuronal distress. Together, these data show for the first time that the spinal cord undergoes significant changes during aging, including progressive α-MNs loss that is associated with low-grade inflammation, apoptosis, changes in ECM, myelination, and vascular permeability.










Similar content being viewed by others

References
Akiyama H, Barger S, Barnum S, Bradt B, Bauer J, Cole GM, et al. Inflammation and Alzheimer’s disease. Neurobiol Aging. 2000;21:383–421.
Bell-Temin H, Culver-Cochran AE, Chaput D, Carlson CM, Kuehl M, Burkhardt BR, et al. Novel molecular insights into classical and alternative activation states of microglia as revealed by stable isotope labeling by amino acids in cell culture (SILAC)-based proteomics. Mol Cell Proteomics, Dec. 2015;14(12):3173–84.
Best JG, Stagg CJ, Dennis A. Other significant metabolites: Myo-Inositol, GABA, glutamine, and lactate. In: Stagg CJ, Rothman D, editors. Magnetic resonance spectroscopy. Tools for neuroscience research and emerging clinical applications. Academic Press; 2014. p.122–138.
Brooks JCW, Roberts N, Kemp GJ, Gosney MA, Spark V, Lye M, Whitehouse GH. Age-related decrease in NAA concentration and NAA/creatine ratio revealed by single voxel ‘H-MRS and compartmentation analysis in fifty subjects. 1999. https://cds.ismrm.org/ismrm-1999/PDF5/1399.pdf.
Chelluboina B, Klopfenstein JD, Pinson DM, Wang DZ, Vemuganti R, Veeravalli KK. Matrix metalloproteinase-12 induces blood-brain barrier damage after focal cerebral ischemia. Stroke. 2015a;46(12):3523–31.
Chelluboina B, Warhekar A, Dillard M, Klopfenstein JD, Pinson DM, Wang DZ, et al. Post-transcriptional inactivation of matrix metalloproteinase-12 after focal cerebral ischemia attenuates brain damage. Sci Rep. 2015b;5:9504.
Chelluboina B, Nalamolu KR, Klopfenstein JD, Pinson DM, Wang DZ, Vemuganti R, et al. MMP-12, a promising therapeutic target for neurological diseases. Mol Neurobiol. 2018;55(2):1405–9.
Conradi S, Ronnevi LO. Selective vulnerability of alpha motor neurons in ALS: relation to autoantibodies toward acetylcholinesterase (AChE) in ALS patients. Brain Res Bull. 1993;30(3–4):369–71.
Cserép C, et al. Microglia monitor and protect neuronal function through specialized somatic purinergic junctions. Science. 2020;367(6477):528–37.
Czirr E, Wyss-Coray T. The immunology of neurodegeneration. J Clin Invest. 2012;122(4):1156–63.
Dandachi N, Kelly NJ, Wood JP, Burton CL, Radder JE, Leme AS, et al. Macrophage elastase induces TRAIL-mediated tumor cell death through its carboxy-terminal domain. Am J Respir Crit Care Med. 2017;196(3):353–63.
Das UN. Ageing: is there a role for arachidonic acid and other bioactive lipids? A review. J Adv Res. 2018;11:67–79.
Dennis EA, Norris PC. Eicosanoid storm in infection and inflammation. Nat Rev Immunol. 2015;15(8):511–23.
Drake JC, Peelor FF, Biela LM, Watkins MK, Miller RA, Hamilton KL, et al. Assessment of mitochondrial biogenesis and mTORC1 signaling during chronic rapamycin feeding in male and female mice. J Gerontol A Biol Sci Med Sci. 2013;68:1493–501.
Drake JC, Bruns DR, Peelor FF, Biela LM, Miller RA, Miller BF, et al. Long-lived Snell dwarf mice display increased proteostatic mechanisms that are not dependent on decreased mTORC1 activity. Aging Cell. 2015;14:474–82.
Duan W, Zhang R, Guo Y, Jiang Y, Huang Y, Jiang H, et al. Nrf2 activity is lost in the spinal cord and its astrocytes of aged mice. In Vitro Cell Dev Biol Anim. 2009;45(7):388–97.
Duan W, Zhang YP, Hou Z, Huang C, Zhu H, Zhang CQ, et al. Novel insights into NeuN: from neuronal marker to splicing regulator. Mol Neurobiol. 2016;53(3):1637–47.
Erschbamer M, Oberg J, Westman E, Sitnikov R, Olson L, Spenger C. 1H-MRS in spinal cord injury: acute and chronic metabolite alterations in rat brain and lumbar spinal cord. Eur J Neurosci. 2011;33(4):678–88.
Falk DJ, Todd AG, Lee S, Soustek MS, ElMallah MK, Fuller DD, et al. Peripheral nerve and neuromuscular junction pathology in Pompe disease. Hum Mol Genet. 2015;24(3):625–36.
Franceschi C, Bonafè M, Valensin S, Olivieri F, De Luca M, Ottaviani E, et al. Inflamm-aging. An evolutionary perspective on immunosenescence. Ann N Y Acad Sci. 2000;908:244–54.
Freitas-Rodríguez S, Folgueras AR, López-Otín C. The role of matrix metalloproteinases in aging: tissue remodeling and beyond. Biochim Biophys Acta Mol Cell Res. 2017;1864(11 Pt A):2015–25.
Galbavy W, Lu Y, Kaczocha M, Puopolo M, Liu L, Rebecchi MJ. Transcriptomic evidence of a parainflammatory state in the middle aged lumbar spinal cord. Immunity & Aging. 2017;14:9.
Gillon A, Nielsen K, Steel C, Cornwall J, Sheard P. Exercise attenuates age-associated changes in motoneuron number, nucleocytoplasmic transport proteins and neuromuscular health. Geroscience., 177. 2018;40(2):–192.
Gorska-Ciebiada M, Saryusz-Wolska M, Borkowska A, Ciebiada M, Loba J. Serum soluble adhesion molecules and markers of systemic inflammation in elderly diabetic patients with mild cognitive impairment and depressive symptoms. Biomed Res Int. 2015;2015:826180.
Grimal S, Puech S, Wagener R, Ventéo S, Carroll P, Fichard-Carroll A. Collagen XXVIII is a distinctive component of the peripheral nervous system nodes of ranvier and surrounds nonmyelinating glial cells. Glia. 2010;58(16):1977–87.
Hodes R. Selective destruction of large motoneurons by poliomyelitis virus; conduction velocity of motor nerve fibers of chronic poliomyelitis patients. J Neurophysiol. 1949;12(4):257–66.
Hodes R, Peacock SM Jr, Bodian D. Selective destruction of large motoneurons by poliomyelitis virus; size of motoneurons in the spinal cord of rhesus monkeys. J Neuropathol Exp Neurol. 1949;8(4):400–10.
Ivannikov M, Van Remmen H. Sod1 gene ablation in adult mice leads to physiological changes at the neuromuscular junction similar to changes that occur in old wild-type mice. Free Radic Biol Med. 2015;84:254–62.
Jang YC, Van Remmen H. Age-associated alterations of the neuromuscular junction. Exp Gerontol. 2011;46(2–3):193–8.
Jang YC, Liu Y, Hayworth CR, Bhattacharya A, Lustgarten MS, Muller FL, et al. Dietary restriction attenuates age-associated muscle atrophy by lowering oxidative stress in mice even in complete absence of CuZnSOD. Aging cell. 2012;11(5):770–82.
Jessen F, Block W, Träber F, Keller E, Flacke S, Lamerichs R, et al. Decrease of N-acetylaspartate in the MTL correlates with cognitive decline of AD patients. Neurology. 2001;57(5):930–2.
Kamiya K, Furuya T, Hashimoto M, Mannoji C, Inada T, Ota M, Maki S, Ijima Y, Saito J, Kitamura M, Ohtori S, Orita S, Inage K, Yamazaki M, Koda M. Exploration of spinal cord aging–related proteins using a proteomics approach. J Exp Neurosci. 2017;11:1179069517713019.
Kawamura Y, Okazaki H, O'Brien PC, Dyck PJ. Lumbar motoneurons of man. I: numbers and diameter histograms of alpha and gamma axons and ventral roots. J Neuropathol & Exp Neurol. 1977a;36:853–60.
Kawamura Y, O'Brien PC, Okazaki H, Dyck PJ. Lumbar motoneurons of man. II: numbers and diameter distributions of large- and intermediate-diameter cytons in motoneuron columns of spinal cord of man. J Neuropathol & Exp Neurol. 1977b;36:860–70.
Lee KY, Kang JY, Yun JI, Chung JY, Hwang IK, Won MH, et al. Age-related change of Iba-1 immunoreactivity in the adult and aged gerbil spinal cord. Anat Cell Biol. 2017;50(2):135–42.
Li S, Clements R, Sulak M, Gregory R, Freeman E, McDonough J. Decreased NAA in gray matter is correlated with decreased availability of acetate in white matter in postmortem multiple sclerosis cortex. Neurochem Res. 2013;38(11):2385–96.
Lintl P, Braak H. Loss of intracortical myelinated fibers: a distinctive age-related alteration in the human striate area. Acta Neuropathol. 1983;61:178–82.
Liu RH, Bertolotto C, Engelhardt JK, Chase MH. Age-related changes in soma size of neurons in the spinal cord motor column of the cat. Neurosci Lett. 1996;211(3):163–6.
Liu Y, Zhang M, Hao W, Mihaljevic I, Liu X, Xie K, et al. Matrix metalloproteinase-12 contributes to neuroinflammation in the aged brain. Neurobiol Aging. 2013;34(4):1231–9.
Machado-Salas J, Scheibel ME, Scheibel AB. Neuronal changes in the aging mouse: spinal cord and lower brain stem. Exp Neurol. 1977;54:504–12.
Maxwell N, Castro RW, Sutherland NM, Vaughan KL, Szarowicz MD, de Cabo R, et al. α-Motor neurons are spared from aging while their synaptic inputs degenerate in monkeys and mice. Aging Cell. 2018;17:2.
McCawley LJ, Matrisian LM. Matrix metalloproteinases: they’re not just for matrix anymore! Curr Opin Cell Biol. 2001;13(5):534–40.
Merdad A, Karim S, Schulten HJ, Dallol A, Buhmeida A, Al-Thubaity F, et al. Expression of matrix metalloproteinases (MMPs) in primary human breast cancer: MMP-9 as a potential biomarker for cancer invasion and metastasis. Anticancer Res. 2014;34(3):1355–66.
Miller BF, Hamilton KL. A perspective on the determination of mitochondrial biogenesis. Am J Physiol Endocrinol Metab. 2012;302(5):496–9.
Miller BF, Baehr LM, Musci RV, Reid JJ, Peelor FF 3rd, Hamilton KL, et al. Muscle-specific changes in protein synthesis with aging and reloading after disuse atrophy. J Cachexia Sarcopenia Muscle. 2019;10(6):1195–209.
Muller FL, Song W, Jang YC, Liu Y, Sabia M, Richardson A, et al. Denervation-induced skeletal muscle atrophy is associated with increased mitochondrial ROS production. Am J Physiol Regul Integr comp Physiol. 2007;293(3):R1159–68.
Musiał K, Zwolińska D. Matrix metalloproteinases and soluble Fas/FasL system as novel regulators of apoptosis in children and young adults on chronic dialysis. Apoptosis. 2011;16(7):653–9.
Nacka-Aleksić SM, Simić L, Bufan B, Kotur-Stevuljević J, Stojić-Vukanić Z, Dimitrijević M, et al. Sex as a determinant of age-related changes in spinal cord inflammation-oxidation state. Biogerontology. 2017;18:821–39. https://doi.org/10.1007/s10522-017-9726-4.
Nishio T, Miyadera R, Sakai R, Abe K, Kanazawa H, Fukui K, et al. Increased F2-Isoprostane levels in the rat brain and plasma caused by oxidative stress and aging, and inhibitory effect of vitamin E. J Clin Biochem Nutr. 2006;38:161–6.
Noble LJ, Donovan F, Igarashi T, Goussev S, Werb Z. Matrix metalloproteinases limit functional recovery after spinal cord injury by modulation of early vascular events. J Neurosci. 2002;22(17):7526–35.
Palumbo S, Bosetti F. Alterations of brain eicosanoid synthetic pathway in multiple sclerosis and in animal models of demyelination: role of cyclooxygenase-2. Prostaglandins Leukot Essent Fatty Acids. 2013;89(5):273–8.
Parkinson GM, Dayas CV, Smith DW. Perturbed cholesterol homeostasis in aging spinal cord. Neurobiol Aging. 2016;45:123–35.
Reid JJ, Linden MA, Peelor FF, Miller RA, Hamilton KL, Miller BF. Brain protein synthesis rates in the UM-HET3 mouse following treatment with rapamycin or rapamycin with metformin. J Gerontol A Biol Sci Med Sci. 2019. https://doi.org/10.1093/gerona/glz069.
Roberts BM, Morrow JD. Measurement of F(2)-isoprostanes as an index of oxidative stress in vivo. Free Radic Biol Med. 2000;28:505–13.
Shay G, Lynch CC, Fingleton B. Moving targets: emerging roles for MMPs in cancer progression and metastasis. Matrix Biol. 2015;44-46:200–6.
Sherin JE, Bartzokis G. Human brain myelination trajectories across the life span: implications for CNS function and dysfunction. In: Masoro EJ, Austa SN, editors. Handbook of the biology of aging. San Diego: Academic Press; 2011. p. 333–46.
Singh AK, Wang AM, Sanders W. Magnetic resonance spectroscopy of the brain. Suppl to Applied Radiology. 2002. https://pdfs.semanticscholar.org/d4e3/fd85837a11d83cf4bc2827f6ceb6c5896c18.pdf.
Sparkman NL, Johnson RW. Neuroinflammation associated with aging sensitizes the brain to the effects of infection or stress. Neuroimmunomodulation. 2008;15(4–6):323–30.
Stekovic S, et al. Alternate day fasting improves physiological and molecular markers of aging in healthy, non-obese humans. Cell Metab. 2019;30(3):462–76.
Tassoni D, Kaur G, Weisinger RS, Sinclair AJ. The role of eicosanoids in the brain. Asia Pac J Clin Nutr. 2008;17(Suppl 1):220–8.
Toedebusch CM, Garcia VB, Snyder JC, Jones MR, Schulz DJ, Johnson GC, et al. Lumbar spinal cord microglia exhibited increased activation in aging dogs compared with young adult dogs. Geroscience. 2019;11. https://doi.org/10.1007/s11357-019-00133-8.
Tomlinson BE, Irving D. The numbers of limb motor neurons in the human lumbosacral cord throughout life. J Neurol Sci. 1977;34:213–9.
Walsh ME, Sloane LB, Fischer KE, Austad SN, Richardson A, Van Remmen H. Use of nerve conduction velocity to assess peripheral nerve health in aging mice. J Gerontol A Biol Sci Med Sci. 2015;70(11):1312–9.
Xie F, Zhang JC, Fu H, Chen J. Age-related decline of myelin proteins is highly correlated with activation of astrocytes and microglia in the rat CNS. International Journal of Molecular Medicine, November. 2013;32(5):1021–8.
Yin F, Sancheti H, Patil I, Cadenas E. Energy metabolism and inflammation in brain aging and Alzheimer's disease. Free Radic Biol Med. 2016;100:108–22.
Yong VW. Metalloproteinases: mediators of pathology and regeneration in the CNS. Nat Rev Neurosci. 2005;6(12):931–44.
Yonutas HM, Pandya JD, Sullivan PG. Changes in mitochondrial bioenergetics in the brain versus spinal cord become more apparent with age. J Bioenerg Biomembr. 2015;47(1–2):149–54.
Zhou M, Goto N, Zhang C, Tang W. Aging process of the human lumbar spinal cord: a morphometric analysis. Neuropathology. 1996;16(2):106–11.
Funding
The study was supported by a grant from the National Institute on Aging (P01AG051442) awarded to HVR, and National Institutes of Health S10 grant 1S10OD023508 awarded to RT. KMP was supported by the Drs. Patricia H. and J. Donald Capra Fund Oklahoma Medical Research Foundation Predoctoral Scholarship. Dr. Van Remmen is the recipient of a Senior Research Career Scientist award (#1 IK6BX005234) from the Department of Veterans Afffairs.
Author information
Authors and Affiliations
Contributions
KMP designed research, conducted experiments, analyzed the results, and wrote the paper; SB contributed western blot and EM data; KS contributed to cytokine assay and the RNA-seq experiment; KSt contributed to the RNA-seq experiment; PP performed and analyzed isoprostanes assay; DS performed MRI; MZ and RG analyzed MRI data; SK, JL, RP, and BFM performed and analyzed data from the protein turnover assay; RT contributed to MRI experiment design, supervision, and interpretation; HVR supervised experiments and edited the paper.
Corresponding author
Ethics declarations
All experiments were approved by the Institutional Animal Care and Use Committee at the Oklahoma Medical Research Foundation (OMRF)
Conflict of interest
The authors declare that they have no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Fig. S1
Age-related α-motor neuron loss. Nuclear Fast Red staining of lumbar spinal cord sections. There is approximately a 39% decrease in α-MN number in old mice (females, 27 mo, n = 4, median and IQR = 7.542 and 2.455) comparing to young (6–7 mo, n = 4, median and IQR = 12.38 and 2.56; Mann-Whitney test, p = 0.0286); (PNG 40 kb)
Fig. S2
Blood vessel density does not decrease with age. A – A representative image of a cross section of lumbar spinal cord of a young (3 mo) and old (29 mo) mice stained for CD31 to visualize blood vessels (tiling of four 10x images, z-stack of 5, maximum intensity projection); B – quantification of blood vessel density a percentage of total SC area. There is no significant difference between young (n = 4, mean ± SD = 4.66 ± 1.79) and old mice (n = 7, mean ± SD = 5.42 ± 1.82; two-tailed unpaired t-test, t = 0.6720, p = 0.5185). (PNG 1017 kb)
Fig. S3
BSCB permeability to Gd-DTPA. MRI assessment of BSCB permeability; percentage change in the signal intensity pre- and post-Gd-DTPA injection in young (3–4 mo) and old (26–27 mo) mice measured in cervical (A), thoracic (B), and lumbar (C) spinal cord. (PNG 128 kb)
Supplementary Table 1
IPA analysis results on RNA-seq data from young and old spinal cord. Canonical pathways; Molecules; Diseases – main categories; Detailed diseases of functions; Predicted upstream regulators. (XLSX 81 kb)
About this article
Cite this article
Piekarz, K.M., Bhaskaran, S., Sataranatarajan, K. et al. Molecular changes associated with spinal cord aging. GeroScience 42, 765–784 (2020). https://doi.org/10.1007/s11357-020-00172-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11357-020-00172-6