Abstract
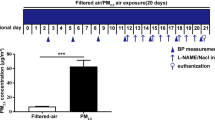
A growing body of epidemiological evidence has supported the association between maternal exposure to airborne fine particulate matter (PM2.5) during pregnancy and adverse pregnancy outcomes. However, the specific biological mechanisms implicated in the causes of adverse pregnancy outcomes are not well defined. In this study, a pregnant rat model of exposure to different doses of cooking oil fumes (COFs)-derived PM2.5 by tail intravenous injection in different pregnant stages was established. The results indicated that exposure to COFs-derived PM2.5 was associated with adverse pregnancy outcomes, changed the structure of umbilical cord blood vessels, decreased the diameter and lumen area, and increased wall thickness. What’s more, a significant increase of maximum contraction tension was observed in the early pregnancy high-dose exposure group and pregnant low-dose exposure group compared to the control group. Based on the maximum contraction tension, acetylcholine (ACh) did not induce vasodilation but caused a dose-dependent constriction, and there were significant differences in the two groups compared to the control group. Exposure to COFs-derived PM2.5 impaired the vasomotor function of umbilical veins by affecting the expression of NO and ET-1. This is the first study that evaluated the association of risk of adverse pregnancy outcomes and pregnant rats exposed to COFs-derived PM2.5 and primarily explored the potential mechanisms of umbilical cord blood vessels injury on a rat model. More detailed vitro and vivo studies are needed to further explore the mechanism in the future.








Similar content being viewed by others
References
Anderson HD, Rahmutula D, Gardner DG (2004) Tumor necrosis factor-alpha inhibits endothelial nitric-oxide synthase gene promoter activity in bovine aortic endothelial cells. J Biol Chem 279(2):963–969
Cao XN, Yan C, Liu DY et al (2015) Fine particulate matter leads to reproductive impairment in male rats by overexpressing phosphatidylinositol 3-kinase (PI3K)/protein kinase B (Akt) signaling pathway. Toxicol Lett 237(3):181–190
Che Z, Liu Y, Chen Y et al (2014) The apoptotic pathways effect of fine particulate from cooking oil fumes in primary fetal alveolar type II epithelial cells. Mutat Res Genet Toxicol Environ Mutagen 761:35–43
Chen N, Lv J, Bo L et al (2015) Muscarinic-mediated vasoconstriction in human, rat and sheep umbilical cords and related vasoconstriction mechanisms. BJOG 122(12):1630–1639
Dadvand P, Parker J, Bell ML et al (2013) Maternal exposure to particulate air pollution and term birth weight: a multi-country evaluation of effect and heterogeneity. Environ Health Perspect 121(3):267–373
Davel AP, Lemos M, Pastro LM et al (2012) Endothelial dysfunction in the pulmonary artery induced by concentrated fine particulate matter exposure is associated with local but not systemic inflammation. Toxicology 295(1-3):39–46
Di NE, Ghezzi F, Raio L, Franchi M, D’Addario V (2001) Umbilical cord morphology and pregnancy outcome. Eur J Obstet Gynecol Reprod Biol 96(2):150–157
Fleischer NL, Merialdi M, van Donkelaar A et al (2014) Outdoor air pollution, preterm birth, and low birth weight: analysis of the world health organization global survey on maternal and perinatal health. Environ Health Perspect 122(4):425–430
Gaillard R, Steegers EA, Tiemeier H, Hofman A, Jaddoe VW (2013) Placental vascular dysfunction, fetal and childhood growth, and cardiovascular development: the generation R study. Circulation 128(20):2202–2210
Gamez-Mendez AM, Vargas-Robles H, Rios A, Escalante B (2015) Oxidative Stress-Dependent Coronary Endothelial Dysfunction in Obese Mice. PLoS ONE 10(9), e0138609
Guo L, Zhu N, Guo Z et al (2012) Particulate matter (PM10) exposure induces endothelial dysfunction and inflammation in rat brain. J Hazard Mater 213–214:28–37
Han J, Chen ZW, He GW (2013) Acetylcholine- and sodium hydrosulfide-induced endothelium-dependent relaxation and hyperpolarization in cerebral vessels of global cerebral ischemia-reperfusion rat. J Pharmacol Sci 121(4):318–326
Heo J, Schauer JJ, Yi O, Paek D, Kim H, Yi SM (2014) Fine particle air pollution and mortality: importance of specific sources and chemical species. Epidemiology 25(3):379–388
Hipolito UV, Callera GE, Simplicio JA, De Martinis BS, Touyz RM, Tirapelli CR (2015) Vitamin C prevents the endothelial dysfunction induced by acute ethanol intake. Life Sci 141:99–107
Husain K, Hernandez W, Ansari RA, Ferder L (2015) Inflammation, oxidative stress and renin angiotensin system in atherosclerosis. World J Biol Chem 6(3):209–217
Hyder A, Lee HJ, Ebisu K, Koutrakis P, Belanger K, Bell ML (2014) PM2.5 exposure and birth outcomes: use of satellite- and monitor-based data. Epidemiology 25(1):58–67
Kellow ZS, Feldstein VA (2011) Ultrasound of the placenta and umbilical cord: a review. Ultrasound Q 27(3):187–197
Knothe G, Steidley KR (2009) A comparison of used cooking oils: a very heterogeneous feedstock for biodiesel. Bioresour Technol 100(23):5796–5801
Knuckles TL, Lund AK, Lucas SN, Campen MJ (2008) Diesel exhaust exposure enhances venoconstriction via uncoupling of eNOS. Toxicol Appl Pharmacol 230(3):346–351
Koech A, Ndungu B, Gichangi P (2008) Structural changes in umbilical vessels in pregnancy induced hypertension. Placenta 29(2):210–214
Kovo M, Schreiber L, Bar J (2013) Placental vascular pathology as a mechanism of disease in pregnancy complications. Thromb Res 131(Suppl 1):S18–S21
Liu Y, Chen YY, Cao JY et al (2015) Oxidative stress, apoptosis, and cell cycle arrest are induced in primary fetal alveolar type II epithelial cells exposed to fine particulate matter from cooking oil fumes. Environ Sci Pollut Res Int 22(13):9728–9741
Nkwabong E, Kamgnia NN, Sando Z, Mbu RE, Mbede J (2015) Risk factors and placental histopathological findings of term born low birth weight neonates. Placenta 36(2):138–141
Nurkiewicz TR, Porter DW, Hubbs AF et al (2009) Pulmonary nanoparticle exposure disrupts systemic microvascular nitric oxide signaling. Toxicol Sci 110(1):191–203
Olsen Y, Karottki DG, Jensen DM et al (2014) Vascular and lung function related to ultrafine and fine particles exposure assessed by personal and indoor monitoring: a cross-sectional study. Environ Health 13:112
Ostro B, Lipsett M, Reynolds P et al (2010) Long-term exposure to constituents of fine particulate air pollution and mortality: results from the California Teachers Study. Environ Health Perspect 118(3):363–369
Pereira T, Armada-da SPA, Amorim I et al (2014) Effects of Human Mesenchymal Stem Cells Isolated from Wharton’s Jelly of the Umbilical Cord and Conditioned Media on Skeletal Muscle Regeneration Using a Myectomy Model. Stem Cells Int 2014:376918
Peyter AC, Delhaes F, Baud D et al (2014) Intrauterine growth restriction is associated with structural alterations in human umbilical cord and decreased nitric oxide-induced relaxation of umbilical vein. Placenta 35(11):891–899
Pujol LVA, Hita FJ, Gobbi MD, Verdi MG, Rodriguez MC, Rothlin RP (2006) Pharmacological characterization of muscarinic receptor subtypes mediating vasoconstriction of human umbilical vein. Br J Pharmacol 147(5):516–523
Raio L, Ghezzi F, Di NE, Duwe DG, Cromi A, Schneider H (2003) Umbilical cord morphologic characteristics and umbilical artery Doppler parameters in intrauterine growth-restricted fetuses. J Ultrasound Med 22(12):1341–1347
Rankin JH, Goodman A, Phernetton T (1975) Local regulation of the uterine blood flow by the umbilical circulation. Proc Soc Exp Biol Med 150(3):690–694
Ritz B, Wilhelm M (2008) Ambient air pollution and adverse birth outcomes: methodologic issues in an emerging field. Basic Clin Pharmacol Toxicol 102(2):182–190
Selevan SG, Kimmel CA, Mendola P (2000) Identifying critical windows of exposure for children’s health. Environ Health Perspect 108(Suppl 3):451–455
Shah AM, MacCarthy PA (2000) Paracrine and autocrine effects of nitric oxide on myocardial function. Pharmacol Ther 86(1):49–86
Shan M, Yang X, Ezzati M et al (2014) A feasibility study of the association of exposure to biomass smoke with vascular function, inflammation, and cellular aging. Environ Res 135:165–172
Stieb DM, Chen L, Beckerman BS et al (2016) Associations of Pregnancy Outcomes and PM2.5 in a National Canadian Study. Environ Health Perspect 124(2):243–249
Sussan TE, Ingole V, Kim JH et al (2014) Source of biomass cooking fuel determines pulmonary response to household air pollution. Am J Respir Cell Mol Biol 50(3):538–548
Tailor A, Granger DN (2000) Role of adhesion molecules in vascular regulation and damage. Curr Hypertens Rep 2(1):78–83
Veras MM, Guimaraes-Silva RM, Caldini EG, Saldiva PH, Dolhnikoff M, Mayhew TM (2012) The effects of particulate ambient air pollution on the murine umbilical cord and its vessels: a quantitative morphological and immunohistochemical study. Reprod Toxicol 34(4):598–606
Yamashita K, Yoshioka Y, Higashisaka K et al. (2011) Silica and titanium dioxide nanoparticles cause pregnancy complications in mice. Nat Nanotechnol. 6(5): 321–8
Yoshimatsu J, Goto K, Nasu K, Narahara H, Miyakawa I (2006) Intrauterine growth restriction and the proliferation of smooth muscle cells in umbilical vessels. Aust N Z J Obstet Gynaecol 46(3):212–216
Zhu X, Liu Y, Chen Y, Yao C, Che Z, Cao J (2015) Maternal exposure to fine particulate matter (PM2.5) and pregnancy outcomes: a meta-analysis. Environ Sci Pollut Res Int 22(5):3383–3396
Acknowledgments
This work was supported by the Science Research Fund of Anhui Province (090413265X). We are grateful to thank all of the participants in this study and the reviewers and editors for their work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there is no conflict of interests.
Additional information
Responsible editor: Philippe Garrigues
Rights and permissions
About this article
Cite this article
Zhu, X., Hou, L., Zhang, J. et al. The structural and functional effects of fine particulate matter from cooking oil fumes on rat umbilical cord blood vessels. Environ Sci Pollut Res 23, 16567–16578 (2016). https://doi.org/10.1007/s11356-016-6821-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11356-016-6821-z