Abstract
Study objectives
Frailty is frequently reported following sleep disorders; however, the extent to which sleep disorders influence frailty remains unclear. In the current study, we performed a meta-analysis to evaluate the quantitative effects of different sleep disorders on frailty in the elderly.
Methods
We conducted a systematic search of several databases, including PubMed, Web of Science, Embase, and Scopus, to retrieve articles published from May 2009 to June 2021. The data outcomes are expressed as the odds ratio (OR) and 95% confidence interval (CI).
Results
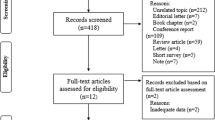
Eighteen studies were included, with 39669 participants. Older adults with sleep disorders were found to have a higher risk of frailty (pooled OR = 1.49, 95%CI = 1.35–1.64, p < 0.01). Specifically, daytime sleepiness (pooled OR = 1.69, 95%CI = 1.09–2.61, p < 0.01), short sleep duration (pooled OR = 1.36, 95%CI = 1.20–1.54, p = 0.45), long sleep duration (pooled OR = 1.99, 95%CI = 1.39–2.85, p = 0.02), sleep latency extension (pooled OR = 1.38, 95%CI = 1.19–1.60, p = 0.72), and sleep disordered breathing (pooled OR = 1.30, 95%CI = 1.11–1.53, p = 0.37) were correlated with frailty.
Conclusions
The risk of frailty differs between older adults with sleep disorders and controls, suggesting that the relationships between different sleep disorders and frailty vary. These results highlight the need to monitor sleep disorders of the elderly and conduct intervention to prevent or delay the frailty process.





Similar content being viewed by others
References
Ohayon MM (2002) Epidemiology of insomnia: what we know and what we still need to learn. Sleep Med Rev 6(2):97–111. https://doi.org/10.1053/smrv.2002.0186
Hirshkowitz M (2004) Normal human sleep: an overview. Med Clin N Am 88(3):551–65, vii. https://doi.org/10.1016/j.mcna.2004.01.001
Gorelick PB, Scuteri A, Black SE et al (2011) Vascular contributions to cognitive impairment and dementia: a statement for healthcare professionals from the american heart association/american stroke association. Stroke 42(9):2672–2713. https://doi.org/10.1161/STR.0b013e3182299496
Walston J, Hadley EC, Ferrucci L et al (2006) Research agenda for frailty in older adults: toward a better understanding of physiology and etiology: summary from the American Geriatrics Society/National Institute on Aging Research Conference on Frailty in Older Adults. J Am Geriatr Soc 54(6):991–1001. https://doi.org/10.1111/j.1532-5415.2006.00745.x
Fried LP, Tangen CM, Walston J et al (2001) Frailty in older adults: evidence for a phenotype. J Gerontol A Biol Sci Med Sci 56(3):M146–M156. https://doi.org/10.1093/gerona/56.3.m146
Collard RM, Boter H, Schoevers RA, Oude Voshaar RC (2012) Prevalence of frailty in community-dwelling older persons: a systematic review. J Am Geriatr Soc 60(8):1487–1492. https://doi.org/10.1111/j.1532-5415.2012.04054.x
Cesari M, Calvani R, Marzetti E (2017) Frailty in older persons. Clin Geriatr Med 33(3):293–303. https://doi.org/10.1016/j.cger.2017.02.002
Gill TM, Gahbauer EA, Han L, Allore HG (2010) Trajectories of disability in the last year of life. N Engl J Med 362(13):1173–1180. https://doi.org/10.1056/NEJMoa0909087
Del Brutto OH, Mera RM, Sedler MJ et al (2016) The effect of age in the association between frailty and poor sleep quality: A population-based study in community-dwellers (The Atahualpa Project). J Am Med Dir Assoc 17(3):269–271. https://doi.org/10.1016/j.jamda.2015.12.009
Vaz Fragoso CA, Gahbauer EA, Van Ness PH, Gill TM (2009) Sleep-wake disturbances and frailty in community-living older persons. J Am Geriatr Soc 57(11):2094–2100. https://doi.org/10.1111/j.1532-5415.2009.02522.x
Ensrud KE, Blackwell TL, Redline S et al (2009) Sleep disturbances and frailty status in older community-dwelling men. J Am Geriatr Soc 57(11):2085–2093. https://doi.org/10.1111/j.1532-5415.2009.02490.x
Stang A (2010) Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol 25(9):603–605. https://doi.org/10.1007/s10654-010-9491-z
Endeshaw YW, Unruh ML, Kutner M, Newman AB, Bliwise DL (2009) Sleep-disordered breathing and frailty in the cardiovascular health study cohort. Am J Epidemiol 170(2):193–202. https://doi.org/10.1093/aje/kwp108
Ensrud KE, Blackwell TL, Ancoli-Israel S et al (2012) Sleep disturbances and risk of frailty and mortality in older men. Sleep Med 13(10):1217–1225. https://doi.org/10.1016/j.sleep.2012.04.010
Moreno-Tamayo K, Manrique-Espinoza B, Rosas-Carrasco O, Perez-Moreno A, Salinas-Rodriguez A (2017) Sleep complaints are associated with frailty in Mexican older adults in a rural setting. Geriatr Gerontol Int 17(12):2573–2578. https://doi.org/10.1111/ggi.13111
Nakakubo S, Makizako H, Doi T et al (2018) Long and short sleep duration and physical frailty in community-dwelling older adults. J Nutr Health Aging 22(9):1066–1071. https://doi.org/10.1007/s12603-018-1116-3
Kang I, Kim S, Kim BS, Yoo J, Kim M, Won CW (2019) Sleep latency in men and sleep duration in women can be frailty markers in community-dwelling older adults: The Korean Frailty and Aging Cohort Study (KFACS). J Nutr Health Aging 23(1):63–67. https://doi.org/10.1007/s12603-018-1109-2
Baniak LM, Yang K, Choi J, Chasens ER (2020) Long sleep duration is associated with increased frailty risk in older community-dwelling adults. J Aging Health 32(1):42–51. https://doi.org/10.1177/0898264318803470
Sun XH, Ma T, Yao S et al (2020) Associations of sleep quality and sleep duration with frailty and pre-frailty in an elderly population Rugao longevity and ageing study. BMC Geriatr 20(1):9. https://doi.org/10.1186/s12877-019-1407-5
Akın S, Özer FF, Zararsız GE et al (2020) The impact of sleep duration on frailty in community-dwelling Turkish older adults. Sleep Biol Rhythms 18(3):243–248. https://doi.org/10.1007/s41105-020-00264-y
Fu P, Zhou C, Meng Q (2020) Associations of sleep quality and frailty among the older adults with chronic disease in China: The mediation effect of psychological distress. Int J Environ Res Public Health 17(14):5240. https://doi.org/10.3390/ijerph17145240
Çavuşoğlu Ç, Deniz O, Tuna Doğrul R et al (2021) Frailty is associated with poor sleep quality in the oldest old. Turk J Med Sci 51(2):540–546. https://doi.org/10.3906/sag-2001-168
Balomenos V, Ntanasi E, Anastasiou CA et al (2021) Association between sleep disturbances and frailty: evidence from a population-based study. J Am Med Dir Assoc 22(3):551-558 e1. https://doi.org/10.1016/j.jamda.2020.08.012
Shih AC, Chen LH, Tsai CC, Chen JY (2020) Correlation between Sleep quality and frailty status among middle-aged and older Taiwanese people: A community-based, cross-sectional study. Int J Environ Res Public Health 17(24):9457. https://doi.org/10.3390/ijerph17249457
Liu M, Hou T, Nkimbeng M et al (2021) Associations between symptoms of pain, insomnia and depression, and frailty in older adults: A cross-sectional analysis of a cohort study. Int J Nurs Stud 117:103873. https://doi.org/10.1016/j.ijnurstu.2021.103873
Guida JL, Alfini AJ, Gallicchio L, Spira AP, Caporaso NE, Green PA (2021) Association of objectively measured sleep with frailty and 5-year mortality in community-dwelling older adults. Sleep 44(7):zsab003. https://doi.org/10.1093/sleep/zsab003
Liu X, Wang C, Qiao X, Si H, Jin Y (2021) Sleep quality, depression and frailty among Chinese community-dwelling older adults. Geriatr Nurs 42(3):714–720. https://doi.org/10.1016/j.gerinurse.2021.02.020
Pourmotabbed A, Boozari B, Babaei A et al (2020) Sleep and frailty risk: a systematic review and meta-analysis. Sleep breathing = Schlaf Atmung 24(3):1187–1197. https://doi.org/10.1007/s11325-020-02061-w
Wai JL, Yu DS (2020) The relationship between sleep-wake disturbances and frailty among older adults: A systematic review. J Adv Nurs 76(1):96–108
Langmann GA, Perera S, Ferchak MA, Nace DA, Resnick NM, Greenspan SL (2017) Inflammatory markers and frailty in long-term care residents. J Am Geriatr Soc 65(8):1777–1783. https://doi.org/10.1111/jgs.14876
Leng SX, Tian X, Matteini A et al (2011) IL-6-independent association of elevated serum neopterin levels with prevalent frailty in community-dwelling older adults. Age Ageing 40(4):475–481. https://doi.org/10.1093/ageing/afr047
Mekli K, Nazroo JY, Marshall AD, Kumari M, Pendleton N (2016) Proinflammatory genotype is associated with the frailty phenotype in the English Longitudinal Study of Ageing. Aging Clin Exp Res 28(3):413–421. https://doi.org/10.1007/s40520-015-0419-z
Ritter PS, Kretschmer K, Pfennig A, Soltmann B (2013) Disturbed sleep in bipolar disorder is related to an elevation of IL-6 in peripheral monocytes. Med Hypotheses 81(6):1031–1033. https://doi.org/10.1016/j.mehy.2013.09.025
Taylor-Gjevre RM, Gjevre JA, Nair BV, Skomro RP, Lim HJ (2011) Improved sleep efficiency after anti-tumor necrosis factor α therapy in rheumatoid arthritis patients. Ther Adv Musculoskelet Dis 3(5):227–233. https://doi.org/10.1177/1759720X11416862
Woods NF, LaCroix AZ, Gray SL et al (2005) Frailty: emergence and consequences in women aged 65 and older in the women’s health initiative observational study. J Am Geriatr Soc 53(8):1321–1330. https://doi.org/10.1111/j.1532-5415.2005.53405.x
Hayes AL, Xu F, Babineau D, Patel SR (2011) Sleep duration and circulating adipokine levels. Sleep 34(2):147–152. https://doi.org/10.1093/sleep/34.2.147
Zeng F, Wang X, Hu W, Wang L (2017) Association of adiponectin level and obstructive sleep apnea prevalence in obese subjects. Medicine 96(32):e7784. https://doi.org/10.1097/MD.0000000000007784
Lana A, Valdés-Bécares A, Buño A, Rodríguez-Artalejo F, Lopez-Garcia E (2017) Serum leptin concentration is associated with incident frailty in older adults. Aging Dis 8(2):240–249. https://doi.org/10.14336/AD.2016.0819
Nagasawa M, Takami Y, Akasaka H et al (2018) High plasma adiponectin levels are associated with frailty in a general old-old population: The Septuagenarians, Octogenarians, Nonagenarians Investigation with Centenarians study. Geriatr Gerontol Int 18(6):839–846. https://doi.org/10.1111/ggi.13258
Tsai JS, Wu CH, Chen SC et al (2013) Plasma adiponectin levels correlate positively with an increasing number of components of frailty in male elders. PLoS ONE 8(2):e56250. https://doi.org/10.1371/journal.pone.0056250
Perez-Saez MJ, Redondo-Pachon D, Arias-Cabrales CE et al (2022) Outcomes of frail patients while waiting for kidney transplantation: differences between physical frailty phenotype and FRAIL scale. J Clin Med 11(3):672. https://doi.org/10.3390/jcm11030672
Acknowledgements
We thank LetPub (www.letpub.com) for its linguistic assistance during the preparation of this manuscript.
Funding
This study was funded by the National Key Research and Development Program of China (grant number 2020YFC2005300) and the Clinical Research Fund of Wu Jieping Medical Foundation (grant number 320.6750.2021–18-1).
Author information
Authors and Affiliations
Contributions
Sun, E, Li designed the study; Xie, Jiang collected and checked the data; Sun, Jiang processed and analyzed the data; Sun, Li wrote the paper.
Corresponding authors
Ethics declarations
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
Informed consent was not necessary for this meta-analysis.
Disclosure statement
The authors affirm that this is an original unpublished manuscript, and this manuscript is not under consideration for publication elsewhere. All authors have read and approved the manuscript.
conflict of interest
All authors have read and approved the manuscript. The authors have indicated no financial conflicts of interest in conducting this study and preparing the manuscript.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Sun, R., Xie, Y., Jiang, W. et al. Effects of different sleep disorders on frailty in the elderly: a systematic review and meta-analysis of observational studies. Sleep Breath 27, 91–101 (2023). https://doi.org/10.1007/s11325-022-02610-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-022-02610-5