Abstract
Purpose
Sleep architecture consists of rapid eye movement (REM) sleep and non-REM sleep time. Non-REM sleep time is further classified into three stages by depth (stage N1–N3). Some studies have reported that short sleep time predicts all-cause mortality. Short sleep time can have characteristics of sleep architecture which contribute to poor prognosis. Obstructive sleep apnea (OSA) is a disease which causes cessation or decline of ventilation during sleep due to upper airway stenosis and affects sleep architecture. Few studies have reported on the sleep architecture of short sleep time in patients with OSA. Therefore, we aimed to observe this phenomenon.
Methods
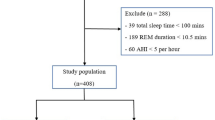
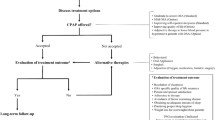
From May 2008 to September 2021, patients diagnosed with OSA at our facility were assessed for clinical history and underwent full-night polysomnography (PSG). These patients were classified into two groups: total sleep time (TST) recorded on PSG consisting of a short TST (< 7 h) group and a not short TST (≥ 7 h) group.
Results
Of 266 patients with OSA, compared to the not short TST group (n = 131), the short TST group (n = 135) had a lower REM sleep time (%) and a higher stage N1 sleep time (%). There was a significant difference in age between the two groups, so sub-analyses classified the patients by age: non-elderly patients (< 65 years) and elderly patients (≥ 65 years) to adjust for age. Both sub-analyses showed similar results to the analysis for the combined ages regarding sleep architecture.
Conclusion
Patients with OSA who had short sleep time had disordered sleep architecture with a lower REM sleep time (%) and more stage N1 sleep time.





Similar content being viewed by others
Data availability
The datasets generated and analyzed during the current study are not publicly available due to institutional limitation, yet they are available from the corresponding author on reasonable request.
Code availability
Not applicable.
References
Cappuccio FP, D’Elia L, Strazzullo P, Miller MA (2010) Sleep duration and all-cause mortality: a systematic review and meta-analysis of prospective studies. Sleep 33(5):585–592. https://doi.org/10.1093/sleep/33.5.585
Cappuccio FP, Cooper D, D’Elia L, Strazzullo P, Miller MA (2011) Sleep duration predicts cardiovascular outcomes: a systematic review and meta-analysis of prospective study. Eur Heart J 32(12):1484–1492. https://doi.org/10.1093/eurheartj/ehr007
Tamakoshi A, Ohno Y (2004) Self-reported sleep duration as a predictor of all-caused mortality: results from the JACC. Sleep 27(1):51–54
Grandner MA (2014) Addressing sleep disturbances: an opportunity to prevent cardiometabolic disease? Int Rev Psychiatry 26(2):155–176. https://doi.org/10.3109/09540261.2014.911148
Taylor DJ, Mallory LJ, Lich KL et al (2007) Comorbidity of chronic insomnia in a population-based sample. Sleep 30(2):213–218. https://doi.org/10.1093/sleep/30.2.213
Spiegel K, Tasali E, Penev P, Cauter EV (2004) Brief communication: sleep curtailment in healthy young men is associated with decreased leptin levels, elevated ghrelin levels, and increased hunger and appetite. Ann Intern Med 141(11):846–850. https://doi.org/10.7326/0003-4819-141-11-200412070-00008
Calvin AD, Carter RE, Adachi T, Macedo PG, Albuquerque FN, Walt CVD et al (2013) Effects of experimental sleep restriction on caloric intake and activity energy expenditure. Chest 144(1):79–86. https://doi.org/10.1378/chest.12-2829
Bromley LE, Booth JN 3rd, Kilkus JM, Imperial JG, Penev PD (2012) Sleep restriction decreases the physical activity of adults at risk for type 2 diabetes. Sleep 35(7):977–984. https://doi.org/10.5665/sleep.1964
McNeil J, Barberio AM, Friedenreich BDR (2019) Sleep and cancer incidence in Alberta’s Tomorrow Project cohort. Sleep 42(3):1–14. https://doi.org/10.1093/sleep/zsy252
Philips AI, Bhatti P, Neuhouser ML et al (2016) Pre-diagnostic sleep duration and sleep quality in relation to subsequent cancer survival. J Clin Sleep Med 12(4):495–503. https://doi.org/10.5664/jcsm.5674
Coutinho AE, Chapman KE (2011) The anti-inflammatory and immunosuppressive effects of glucocorticoids, recent developments and mechanistic insights. Mol Cell Endocrinol 335(1):2–13. https://doi.org/10.1016/j.mce.2010.04.005
Posadzki PP, Bajpai R, Kyaw BM, Roberts NJ, Brzezinski A, Christopoulos GI et al (2018) Melatonin and health: an umbrella review of health outcomes and biological mechanisms of action. BMC Med 16(1):18. https://doi.org/10.1186/s12916-017-1000-8
Ohayon MM, Carskadon MA, Guilleminault C, Vitiello MV (2004) Meta-analysis of quantitative sleep parameters from childfood to old age in healthy individuals: developing normative sleep values across the human lifespan. Sleep 27(7):1255–1273. https://doi.org/10.1093/sleep/27.7.1255
Senaratna CV, Perret JL, Lodge CJ, Lowe AJ, Campbell BE, Matheson MC et al (2017) Prevalence of obstructive sleep apnea in the general population: a systematic review. Sleep Med Rev 34:70–81. https://doi.org/10.1016/j.smrv.2016.07.002
Parekh A, Mullins AE, Kam K, Varga AW, Rapoport DM, Ayappa I (2019) Slow-wave activity surrounding stage N2 K-complexes and daytime function measured by psychomotor vigilance test in obstructive sleep apnea. Sleep 42(3):1–13. https://doi.org/10.1093/sleep/zsy256
Iber C, Ancoli-Israel S, Chesson AL, Quan SF (2007) The AASM manual for the scoring of sleep and associated events: rules, terminology and technician specifications. American Academy of Sleep Medicine, Westchester
Kanda Y (2013) Investigation of the freely available easy-to-use software ‘EZR’ for medical statistics. Bone Marrow Transplant 48(3):452–458. https://doi.org/10.1038/bmt.2012.244
Zhang J, Jin X, Li R, Gao Y, Li J, Wang G (2019) Influence of rapid eye movement sleep on all-cause mortality: a community-based cohort study. Aging 11(5):1580–1588. https://doi.org/10.18632/aging.101858
Collop NA, Salas RE, Delayo M, Gamaldo C (2008) Normal sleep and circadian processes. Crit Care Clin 24(3):449–460. https://doi.org/10.18632/aging.101858
Kalia M (2006) Neurobiology of sleep. Metabolism 55(10):S2-6. https://doi.org/10.1016/j.metabol.2006.07.005
Boyko Y, Ording H, Jennum P (2012) Sleep disturbances in critically ill patients in ICU: how much do we know? Acta Anaesthesiol Scand 56(8):950–958. https://doi.org/10.1111/j.1399-6576.2012.02672.x
De Andres I, Garzon M, Reioso-Suarez F (2011) Functional anatomy of non-REM sleep. Front Neurol 2:70. https://doi.org/10.3389/fneur.2011.00070
Christensen MA, Dixit S, Dewland TA, Whitman IR, Nah G, Vittinghoff E (2018) Sleep Characteristics that predict atrial fibrillation. Heart Rhythms 15(9):1289–1295. https://doi.org/10.1016/j.hrthm.2018.05.008
Landry SA, Andara C, Terrill PI, Joosten SA, Leong P, Mann DL et al (2018) Ventilatory control sensitivity in patients with obstructive sleep apnea is sleep stage dependent. Sleep 41(5):1–10. https://doi.org/10.1093/sleep/zsy040
McSharry DG, Saboisky JP, DeYound P, Jordan AS, Trinder J, Smales E et al (2014) Physiological Mechanisms of upper airway hypotonia during REM sleep. Sleep 37(3):561–569. https://doi.org/10.5665/sleep.3498
Acknowledgements
We thank Editage (www.editage.com) for English language editing.
Author information
Authors and Affiliations
Contributions
Formal analysis and investigation (Shuhei Nozawa, Kazuhisa Urushihata, and Ryosuke Machida). Additional formal analysis, interpretation, and correction (Masayuki Hanaoka). All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
This study was approved by the research ethics committee of the Shinshu University School of Medicine (Approval number: 4917). The study protocols were performed in accordance with the principles outlined in the Declaration of Helsinki of the World Medical Association.
Consent to participate
We indicate an opt-out online about it for participants.
Consent for publication
We indicate an opt-out online about it for participants.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Nozawa, S., Urushihata, K., Machida, R. et al. Sleep architecture of short sleep time in patients with obstructive sleep apnea: a retrospective single-facility study. Sleep Breath 26, 1633–1640 (2022). https://doi.org/10.1007/s11325-021-02533-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-021-02533-7