Abstract
Purpose
Consistent predictors of weight loss outcomes with very low-energy diets (VLEDs) in obstructive sleep apnea (OSA) have not been identified. This study aimed to identify variables predictive of weight loss success in obese patients with OSA undertaking an intensive weight loss programme.
Methods
We analysed biological, psychological, and behavioural variables as potential predictors of weight loss in obese patients with OSA after a 2-month VLED followed by one of two 10-month weight loss maintenance diets. Actigraphy, in-lab polysomnography, urinary catecholamines, and various psychological and behavioural variables were measured at baseline, 2, and 12 months. Spearman’s correlations analysed baseline variables with 2-month weight loss, and 2-month variables with 2–12 month-weight change.
Results
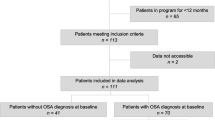
Forty-two patients completed the VLED and thirty-eight completed the maintenance diets. Actigraphy data revealed that late bedtime (rs = − 0.45, p = < 0.01) was correlated with 2-month weight loss. The change in the time that participants got out of bed (rise-time) from baseline to two months was also correlated with 2-month weight loss (rs = 0.36, p = 0.03). The Impact of Weight on Quality of Life-Lite questionnaire (IWQOL) Public Distress domain (rs = − 0.54, p = < 0.01) and total (rs = − 0.38, p = 0.02) scores were correlated with weight loss maintenance from 2 to 12 months.
Conclusions
Results from this small patient sample reveal correlations between actigraphy characteristics and weight loss in obese patients with OSA. We suggest the IWQOL may also be a useful clinical tool to identify OSA patients at risk of weight regain after initial weight loss.
Clinical trial registration
This clinical trial was prospectively registered on 18/02/2013 with the Australia and New Zealand Clinical Trials Registry (ACTRN12613000191796).
Public Registry Title
Sleep, Lifestyle, Energy, Eating, Exercise Program for the management of sleep apnea patients indicated for weight loss treatment: A randomised, controlled pilot study.
URL
https://www.anzctr.org.au/Trial/Registration/TrialReview.aspx?id=363680

Similar content being viewed by others
Data availability
Ethical approval was not granted to release participants’ raw data to third parties. We are happy to provide summaries of data collected in the trial upon request.
Code availability
No custom code was created for the analysis of this trial’s data. Statistical analysis was performed with standard medical statistics software (see ‘Methods’).
Abbreviations
- AGHE:
-
Australian Guide to Healthy Eating
- AHI:
-
Apnea-hypopnea index
- AUSNUT:
-
Australian Food, Supplement and Nutrient Database
- BMI:
-
Body mass index
- CPAP:
-
Continuous positive airway pressure
- EAC:
-
Elizabeth A. Cayanan
- IWQOL:
-
Impact of Weight on Quality of Life-Lite questionnaire
- LGHP:
-
Low Glycemic Index High-Protein
- NC:
-
North Carolina
- OSA:
-
Obstructive sleep apnea
- PA:
-
Pennsylvania
- SAS:
-
Statistical Analysis Software
- USA:
-
United States of America
- VLED:
-
Very low-energy diet
- WASO:
-
Wake after sleep onset
References
Newman AB, Foster G, Givelber R, Nieto FJ, Redline S, Young T (2005) Progression and regression of sleep-disordered breathing with changes in weight: the Sleep Heart Health Study. Arch Intern Med 165:2408–2413
Ford ES, Cooper RS (1991) Risk factors for hypertension in a national cohort study. Hypertension 18:598–606
Rimm EB, Stampfer MJ, Giovannucci E et al (1995) Body size and fat distribution as predictors of coronary heart disease among middle-aged and older US men. Am J Epidemiol 141:1117–1127
Hudgel DW, Patel SR, Ahasic AM et al (2018) The role of weight management in the treatment of adult obstructive sleep apnea. An Official American Thoracic Society Clinical Practice Guideline. Am J Respir Crit Care Med 198:e70–e87
Fernandes JF, Araujo Lda S, Kaiser SE, Sanjuliani AF, Klein MR (2015) The effects of moderate energy restriction on apnoea severity and CVD risk factors in obese patients with obstructive sleep apnoea. Br J Nutr 114:2022–2031
Smith PL, Gold AR, Meyers DA, Haponik EF, Bleecker ER (1985) Weight loss in mildly to moderately obese patients with obstructive sleep apnea. Ann Intern Med 103:850–855
Tuomilehto HP, Seppa JM, Partinen MM et al (2009) Lifestyle intervention with weight reduction: first-line treatment in mild obstructive sleep apnea. Am J Respir Crit Care Med 179:320–327
Pasman WJ, Saris WH, Westerterp-Plantenga MS (1999) Predictors of weight maintenance. Obes Res 7:43–50
Sumithran P, Purcell K, Kuyruk S, Proietto J, Prendergast LA (2018) Combining biological and psychosocial baseline variables did not improve prediction of outcome of a very-low-energy diet in a clinic referral population. Clin Obes 8:30–38
Handjieva-Darlenska T, Handjiev S, Larsen TM et al (2010) Initial weight loss on an 800-kcal diet as a predictor of weight loss success after 8 weeks: the Diogenes study. Eur J Clin Nutr 64:994–999
Linde JA, Jeffery RW, Finch EA, Ng DM, Rothman AJ (2004) Are unrealistic weight loss goals associated with outcomes for overweight women? Obes Res 12:569–576
Fabricatore AN, Wadden TA, Moore RH, Butryn ML, Heymsfield SB, Nguyen AM (2009) Predictors of attrition and weight loss success: results from a randomized controlled trial. Behav Res Ther 47:685–691
Vogels N, Diepvens K, Westerterp-Plantenga MS (2005) Predictors of long-term weight maintenance. Obes Res 13:2162–2168
Teixeira PJ, Going SB, Sardinha LB, Lohman TG (2005) A review of psychosocial pre-treatment predictors of weight control. Obes Rev 6:43–65
Zhu B, Shi C, Park CG, Zhao X, Reutrakul S (2019) Effects of sleep restriction on metabolism-related parameters in healthy adults: a comprehensive review and meta-analysis of randomized controlled trials. Sleep Med Rev 45:18–30
Ogilvie RP, Patel SR (2017) The epidemiology of sleep and obesity. Sleep Health 3:383–388
Shechter A (2017) Obstructive sleep apnea and energy balance regulation: a systematic review. Sleep Med Rev 34:59–69
Kline CE, Chasens ER, Bizhanova Z et al (2021) The association between sleep health and weight change during a 12-month behavioral weight loss intervention. Int J Obes (Lond) 45:639–649
Simpson SJ, Raubenheimer D (2005) Obesity: the protein leverage hypothesis. Obes Rev 6:133–142
Cayanan EA, Marshall NS, Hoyos CM et al (2018) Maintenance diets following rapid weight loss in obstructive sleep apnea: a pilot 1-year clinical trial. J Sleep Res 27:244–251
Moroshko I, Brennan L, O’Brien P (2011) Predictors of dropout in weight loss interventions: a systematic review of the literature. Obes Rev 12:912–934
Sasaki N, Fujiwara S, Yamashita H et al (2018) Association between obesity and self-reported sleep duration variability, sleep timing, and age in the Japanese population. Obes Res Clin Pract 12:187–194
Asarnow LD, McGlinchey E, Harvey AG (2015) Evidence for a possible link between bedtime and change in body mass index. Sleep 38:1523–1527
Baron KG, Reid KJ, Kern AS, Zee PC (2011) Role of sleep timing in caloric intake and BMI. Obesity 19:1374–1381
Teixeira PJ, Going SB, Houtkooper LB et al (2004) Pretreatment predictors of attrition and successful weight management in women. Int J Obes Relat Metab Disord 28:1124–1133
Teixeira PJ, Going SB, Houtkooper LB et al (2002) Weight loss readiness in middle-aged women: psychosocial predictors of success for behavioral weight reduction. J Behav Med 25:499–523
Shechter A, St-Onge M-P, Kuna ST et al (2014) Sleep architecture following a weight loss intervention in overweight and obese patients with obstructive sleep apnea and type 2 diabetes: relationship to apnea-hypopnea index. J Clin Sleep Med 10:1205–1211
Koolhaas CM, Kocevska D, Te Lindert BHW et al (2019) Objectively measured sleep and body mass index: a prospective bidirectional study in middle-aged and older adults. Sleep Med 57:43–50
Carlson JT, Hedner J, Elam M, Ejnell H, Sellgren J, Wallin BG (1993) Augmented resting sympathetic activity in awake patients with obstructive sleep apnea. Chest 103:1763–1768
Coy TV, Dimsdale JE, Ancoli-Israel S, Clausen J (1996) Sleep apnoea and sympathetic nervous system activity: a review. J Sleep Res 5:42–50
Marrone O, Salvaggio A, Bue AL et al (2011) Blood pressure changes after automatic and fixed CPAP in obstructive sleep apnea: relationship with nocturnal sympathetic activity. Clin Exp Hypertens 33:373–380
Carraça EV, Santos I, Mata J, Teixeira PJ (2018) Psychosocial pretreatment predictors of weight control: a systematic review update. Obes Facts 11:67–82
Ware JE Jr, Sherbourne CD (1992) The MOS 36-item short-form health survey (SF-36). I. Conceptual framework and item selection. Med Care 30:473–483
Weaver TE, Laizner AM, Evans LK et al (1997) An instrument to measure functional status outcomes for disorders of excessive sleepiness. Sleep 20:835–843
Kolotkin RL, Crosby RD (2002) Psychometric evaluation of the impact of weight on quality of life-lite questionnaire (IWQOL-lite) in a community sample. Qual Life Res 11:157–171
Johns MW (1991) A new method for measuring daytime sleepiness: the Epworth sleepiness scale. Sleep 14:540–545
Lovibond SH, Lovibond PF (1995) Manual for the depression anxiety stress scales. Psychology Foundation of Australia, Sydney
Schwarzer R, Jerusalem M (1995) Generalized self-efficacy scale. In: Weinman J, Wright S, Johnston M (eds) Measures in health psychology: a user’s portfolio. Causal and control beliefs. NFER-NELSON, Windsor, pp 35–77
Bandura A (1986) The explanatory and predictive scope of self-efficacy theory. J Soc Clin Psychol 4:359–373
Brown J, Miller W, Lawendowski L (1999) Innovations in clinical practice: a source book. Professional Resource Press/Professional Resource Exchange, Sarasota
Baer RA, Smith GT, Allen KB (2004) Assessment of mindfulness by self-report: the Kentucky inventory of mindfulness skills. Assessment 11:191–206
Funding
This trial was funded through the National Health and Medical Research Council (NHMRC) Centre for Integrated Research and Understanding of Sleep (CIRUS) Centre of Research Excellence (571421). Dr Camilla Hoyos is funded by a NHMRC-ARC Dementia Research Development Fellowship (APP1104003).
Author information
Authors and Affiliations
Contributions
Study design: TJA, NSM, CMH, CLP, BJY, RRG, EAC. Data analysis, interpretation of data, and manuscript preparation: TJA, DJB, NSM, CMH, CLP, CB, AK, AM, YS, KKHW, BJY, RRG, EAC. All authors have seen and approved the manuscript.
Corresponding author
Ethics declarations
Ethics approval
Approval was granted by the Sydney Local Health District-Ethics Review Committee (RPAH Zone), Research Development Office, Royal Prince Alfred Hospital, CAMPERDOWN NSW 2050 on 13/12/2012. Ethics approval number: HREC/12/RPAH/533.
Consent to participate
All participants freely gave written informed consent to participate.
Consent for publication
All participants gave informed consent for publication of the results of this trial, and ethics approval included permission to publish in indexed, peer-reviewed medical journals.
Institutions where the work was performed
Woolcock Institute of Medical Research, 431 Glebe Point Rd, Glebe, New South Wales, Australia, 2037.
Royal Prince Alfred Hospital Department of Respiratory and Sleep Medicine, Level 11, Main Building (Building 75), Missenden Road, Camperdown, New South Wales, Australia, 2050.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Altree, T.J., Bartlett, D.J., Marshall, N.S. et al. Predictors of weight loss in obese patients with obstructive sleep apnea. Sleep Breath 26, 753–762 (2022). https://doi.org/10.1007/s11325-021-02455-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-021-02455-4