Abstract
Background
Obesity is a common risk factor for polycystic ovary syndrome (PCOS) and obstructive sleep apnoea (OSA). Both PCOS and OSA are associated with increased risk of type 2 diabetes and cardiovascular disease. Hence, it is important to determine the burden of OSA in women with PCOS.
Methods
We searched electronic databases (MEDLINE, Embase, CINAHL, PsycINFO, Scopus, Web of Science, OpenGrey, CENTRAL), conference abstracts, and reference lists of relevant articles, up to January 2019. No restriction for language or publication status. Studies that examined the presence of OSA in women with PCOS using polysomnography and/or level III devices were eligible for inclusion.
Results
Seventeen studies involving 648 participants were included. Our meta-analysis showed that 35.0% (95% CI 22.2–48.9%) of women with PCOS had OSA. This prevalence was not affected by variation in PCOS definition between studies. Approximately one-tenth of the variation in OSA prevalence was related to differences in study population (higher in adults than adolescents and mixed populations), and around one-tenth was related to sample size (higher in smaller studies). OSA prevalence was markedly higher in obese versus lean women with PCOS, and in women with PCOS compared to controls (odds ratio = 3.83, 95% CI 1.43–10.24, eight studies, 957 participants (349 PCOS and 608 controls)). However, most of the studies were at high risk of selection bias, did not account for important confounders, included predominantly women with class II obesity, and were conducted in one country (USA).
Conclusions
Future studies need to examine the true prevalence of OSA in a more representative sample of women with PCOS. Nevertheless, our results suggest that the prevalence of OSA in women with PCOS and obesity is high and clinicians should have a high index of suspicion of OSA in these women.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Polycystic ovary syndrome (PCOS) is the most frequent endocrine disorder in women of reproductive age, affecting around one in ten women [1,2,3,4,5,6]. The Rotterdam criteria [7] are widely used to diagnose PCOS, requiring the presence of two of the following features: (i) hyperandrogenism (clinical or biochemical), (ii) oligomenorrhoea/anovulation, and (iii) polycystic ovaries on ultrasound, and the exclusion of conditions with similar presentation [8]. PCOS carries a significant burden on the overall health of affected women as it is associated with multiple comorbidities, including obesity [9], subfertility [10], cardiovascular disease (CVD) risk [11], type 2 diabetes mellitus (T2DM) [12], depression, and impaired quality of life (QoL) [13,14,15]. Hyperandrogenism and obesity that are commonly seen in women with PCOS are believed to predispose these women to obstructive sleep apnoea (OSA) [16, 17].
OSA is a common disorder with data from a recent systematic review showing that the prevalence of OSA in women in the general population ranges from 6 to 19% [18]. OSA is characterised by recurrent episodes of partial or complete upper airway obstruction during sleep [19]. These episodes are associated with oxygen desaturations, sleep fragmentation, change in intra-thoracic pressure, sympathetic overactivity, and increase in heart rate and blood pressure [19, 20]. The risk of OSA increases with older age, obesity, male gender, smoking, alcohol intake, sedative use, menopause, and in certain ethnicities [19]. Similar to PCOS, OSA is a health burden in affected individuals and it is associated with increased risk of hypertension [21], CVD [22,23,24], mortality [25, 26], insulin resistance (IR) and T2DM [27], road traffic accidents [28], depression and impaired QoL [29,30,31], as well as subfertility [32].
In a recent systematic review and meta-analysis, OSA was associated with worse metabolic profile in women with PCOS [33]. However, despite its high prevalence and clinical implications, OSA often remains undiagnosed particularly in women [19, 34]. A few studies have suggested a high prevalence of OSA in women with PCOS [16, 35]. This is also supported by the Endocrine Society clinical practice guideline [36] which states in its evidence analysis that ‘women with PCOS develop OSA at rates that equal or exceed those in men’. However, the reported prevalence of OSA in women with PCOS has been very wide, ranging from 0 to 70% [17, 37], which raises concerns about the methodologies used in these studies. Similarly, a recent meta-analysis has attempted to answer this question [38]; however, the review contained significant methodological weaknesses that question its validity (‘OSA prevalence in PCOS’ in discussion). To date, there is no comprehensive, well-conducted, systematic review that examined the prevalence of OSA in women with PCOS. Assessing the prevalence of OSA in women with PCOS will allow the implementation of appropriate screening strategies and further development of clinical studies to examine the impact of OSA in women with PCOS. This is particularly important as OSA is a treatable condition, and it is associated with significant comorbidities [39].
Objectives
To assess the prevalence of OSA in women with PCOS based on the existing literature.
Methods
The protocol for this review was prospectively registered with PROSPERO: CRD42016041464 (http://www.crd.york.ac.uk/PROSPERO/) and is reported following the meta-analysis of Observational Studies in Epidemiology (MOOSE) guidelines [40].
Selection criteria
Human studies, interventional or observational, that examined the presence of OSA in women with PCOS were included. We included studies that used polysomnography or level III devices to diagnose OSA, regardless of the cut-offs used. Conference abstracts and published studies were included.
All women with PCOS were included regardless of age (adults (premenopausal and postmenopausal) and adolescents (postmenarchal)), ethnicity, or PCOS diagnostic criteria.
Exclusion criteria are the following: conditions with presentation similar to PCOS including congenital adrenal hyperplasia, Cushing’s syndrome, prolactinomas, thyroid disease, and androgen-secreting tumours.
Primary outcome
Prevalence of OSA in women with PCOS.
Secondary outcomes
Prevalence of OSA in subpopulations of women with PCOS (obese, non-obese, adolescents, and adults).
Search strategy
The initial literature search was performed on 11 April 2016 and updated on 7 February 2017, and on 11 January 2019. The search was not restricted by language or publication status. We searched Embase (Ovid), MEDLINE (Ebsco), PsycINFO (ProQuest), Scopus, CINAHL (Ebsco), OpenGrey, Web of Science, Cochrane Central Register of Controlled Trials (CENTRAL), and abstracts from major conferences. The reference lists of relevant papers and review articles were manually searched. The search strategy is provided in Appendix 1 (online data supplement).
Selection of studies
Two authors (HK and IK) independently screened titles and abstracts. All potentially relevant articles were reviewed in full. Any disagreements between the two authors were resolved by consensus and, if necessary, discussion with a third author (OU).
Data extraction and management
Two authors (HK and IK) independently extracted data. In case of multiple publications, we included the main study report/paper and, where necessary, additional details extracted from secondary papers. Study investigators were contacted to resolve any data queries, as required. For duplicate publications, we contacted study investigators to clarify the original publication, and if no response was received, we chose the study with the largest number of participants. We extracted the following details from each study: study design, participants’ characteristics, and prevalence estimates.
Risk of bias
Two authors (HK and IK) independently assessed the risk of bias. Any disagreements between the two authors were resolved by consensus and discussion with a third author (OU), if necessary. We used the Risk of Bias Assessment Tool for Non-Randomised Studies (RoBANS) [41] to assess the risk of bias for included study. We assessed the following domains: selection bias (sample population), selection bias (confounding variables), performance bias (measurement of exposure), performance bias (analytical methods to control for bias), and other bias. The methodological components of the studies were assessed and classified as high risk, low risk, or unclear.
Unit of analysis
Number of women with OSA in a population of women with PCOS.
Data synthesis
We pooled the prevalence estimates using the DerSimonian–Laird random effects model [42]. We assessed the between study variations in prevalence estimates using the Higgins I2 statistic, and, as recommended, a value of greater than 50% was considered for moderate heterogeneity [43, 44]. We conducted series of meta-regression and subgroup analyses to explore the effect of study-level covariates on the prevalence estimates. The following study-level factors were considered: type of publication (conference abstract or journal article), year of publication (earlier studies: 2001 to 2009 or recent studies: 2010 to 2015), country, population (adults, adolescent, or mixed population), body mass index (non-obese versus obese), sample size, and PCOS definition (National Institutes of Health (NIH) definition [45], Rotterdam criteria [7], or not reported). The possibility of reporting bias was assessed using an Egger’s test and funnel plot [46]. Leave-one-study-out sensitivity analysis was also performed to assess the stability of the meta-analysis result [47]. Stata 14 was used for all analyses (StataCorp, College Station, TX).
Results
Search results and study characteristics
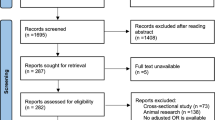
The search results are shown in a PRISMA flow diagram (Fig. 1). Main characteristics of the 17 included and 15 excluded studies are summarised in Table 1 and Table S1 (in the online data supplement), respectively. All of the included studies used polysomnography to diagnose OSA and were reported in English. Five studies did not specify the cut-offs used to diagnose OSA; three studies used an apnoea/hypopnoea index (AHI) > 5 events per hour, and nine studies used variable diagnostic criteria (Table 1).
Risk of bias of included studies
The risk of bias assessment summary for each study is presented in Fig. 2. The selection bias due to inadequate selection of participants was high in five studies and unclear in the remaining 12 studies. The selection bias caused by the inadequate confirmation and consideration of confounding variables was high in most of the studies (15 out of 17 studies) and low only in one study. The performance bias due to inadequate measurement of exposure was low in 12 studies, high in two studies, and unclear in the remaining three studies. The detection bias due to inadequate blinding of outcome assessments was low in most studies (16 out of 17 studies) and high only in one study. The attrition bias due to inadequate handling of incomplete outcome data was low in all 17 studies. The reporting bias due to selective reporting was low in most studies (16 out of 17 studies) and high in one study.
Overall prevalence of OSA in women with PCOS
The prevalence of OSA in women with PCOS and 95% CIs from individual studies with a pooled estimate are shown in Fig. 3. The pooled prevalence of OSA for all studies yielded an estimate of 35.0% (95% CI 22.2 to 48.9%) of women with PCOS. The I2 statistic was 92%, indicating statistically significant heterogeneity among the studies. The contour-enhanced funnel plot of examination of publication bias is shown in Fig. S1 in the online data supplement. We found no evidence of publication bias as indicated by the relatively symmetrical funnel plot of studies’ precision against prevalence estimates (in logarithmic scale). This was confirmed when formally tested using the Egger method (p value for small study bias = 0.063). The results of leave-one-study-out sensitivity analyses showed that no study had undue influence on the pooled OSA prevalence; see Fig. S2 in the online data supplement.
Prevalence of OSA by different subgroups
The results of subgroup analyses are shown in Fig. 4. There is no evidence of statistically significant difference in the pooled prevalence of OSA by type of publication, publication year, or sample size. Studies published in the USA tended to report higher prevalence of OSA than studies from other countries (43.7% versus 22.8%); however, this difference did not reach a statistically significant level (p = 0.725). Compared to studies that used the NIH PCOS definition, studies that used the Rotterdam criteria and those not reporting how PCOS was diagnosed tended to have higher OSA prevalence, albeit not statistically significant. Two studies stratified the prevalence estimates by body mass index, i.e. non-obese versus obese women (Fig. 5). For both studies, the prevalence of OSA was 0% in the non-obese population. In the Gateva and colleagues study [51], two of the six obese women had OSA (33%), while in the Kenigsberg and colleagues study [52], nine out of 22 obese women had OSA (41%). When these two studies were pooled, the prevalence of OSA was 38% higher in women with obesity and PCOS compared to non-obese women with PCOS (prevalence difference = + 37.9%, 95% CI 15.0 to 60.9%).
Obstructive sleep apnoea (OSA) prevalence difference in women with PCOS and obesity versus women with PCOS without obesity. In the study by Gateva et al., the cut-offs used to define obesity in women with PCOS were not reported. Kenigsberg et al. included females with PCOS between the ages of 13–21 years and defined obesity as a BMI z-score > 95th percentile, while participants with BMI z-score < 85th percentile were considered lean
Factors modifying the prevalence of OSA as identified by meta-regression analysis
Factors associated with prevalence estimates and proportion of explained variability in prevalence estimates as identified by meta-regression analyses are shown in Table S2 in the online data supplement. In a series of meta-regression analyses, none of the study-level factors were significantly associated with the prevalence estimates. However, approximately one-tenth of the between study variation in the prevalence estimates was explained by the variations in the study sample size (higher in smaller studies), and around one-tenth was related to differences in the study population (higher in adults compared to adolescents and mixed populations).
Discussion
Our analysis of the existing data suggests that OSA prevalence in women with PCOS is high. This is mainly driven by studies that were conducted in the USA, included women with PCOS and class II obesity, and had a relatively high level of selection bias. Accordingly, it is difficult to draw firm conclusions about the true prevalence of OSA in women with PCOS based on the available data. As expected, the prevalence of OSA in women with PCOS appears to increase with age and obesity.
OSA prevalence in PCOS
Based on our meta-analysis, OSA is present in almost one-third of women with PCOS. In the recent meta-analysis by Helvaci et al., the prevalence of OSA was lower at 0.22 (95% CI 0.08–0.40) in women with PCOS [38]. The lower OSA prevalence reported could be explained by differences in study methodology. In the study by Helvaci et al., the literature search was limited to two electronic databases, was restricted to studies published in English language, and did not include ‘grey literature’ (for example, conference abstracts). In addition, in their meta-analysis, Helvaci et al. included duplicate publications [50, 61,62,63], and one study with 0% prevalence of OSA as only women without OSA were recruited [64].
The prevalence of OSA in women in the general population has been reported at 6–19% [18]. Seven studies have compared OSA prevalence in women with PCOS to matched controls, and the majority [16, 35, 54, 56, 57] have shown OSA to be more prevalent in women with PCOS (Table 2). Women with PCOS were four times more likely to have developed OSA than controls (odds ratio = 3.83, 95% CI 1.43–10.24, eight studies, 957 participants) (Fig. 6). However, important confounding factors that are known to affect the risk of OSA have not been adequately considered in these studies, including obesity [16], abdominal adiposity [16, 35, 54, 56], and ethnicity [16, 54]. Moreover, while controls were recruited from the general population [16, 35, 56], women with PCOS were recruited from specialised clinics [35, 37, 56]. In addition, PCOS was not formally ruled out in controls [16]. Subsequently, it is not clear if women with PCOS in the community are at higher risk of OSA compared to age- and adiposity-matched controls. Well-conducted large observational studies in the general population are needed to answer this question.
Factors affecting OSA prevalence in PCOS
We found a trend for OSA to be more common in adult women with PCOS compared to adolescents, and in women with PCOS and obesity compared to women with PCOS without obesity. This is not surprising as the risk of OSA in the general population increases with increasing age and obesity [19, 65]. Therefore, it is likely that PCOS precedes the development of OSA, particularly as features of PCOS have been identified in prepubertal girls [66, 67]. However, it is also possible that OSA may precede the development of PCOS in some women [68]; for example, a third of the adolescent girls with PCOS in the study by Nandalike et al. [54] had a previous history of tonsillectomy, and tonsillitis and/or tonsillar enlargement are the most common cause of OSA in children [69].
The limited data available suggest that OSA prevalence is low in women with PCOS who are lean/non-obese. This is based on three studies that reported data on a total of 40 participants with these characteristics [37, 51, 52]. However, the sample size is too small to draw firm conclusions.
Androgens are believed to play a role in the pathogenesis of OSA and may contribute to the higher prevalence of OSA in men compared to women [19]. However, despite the higher levels of testosterone and/or free testosterone in the PCOS group compared to controls in three studies [37, 50, 53], there was no difference in OSA prevalence (Table 2). Furthermore, while some studies showed the severity of OSA in women with PCOS to correlate with hyperandrogenism [35]; others did not show a similar relationship [56]. In addition, while women with PCOS diagnosed based on the NIH definition are expected to show higher degree of hyperandrogenism compared to those diagnosed using the Rotterdam criteria, we did not find a significant difference in OSA prevalence based on the PCOS diagnostic criteria/definition used. Subsequently, based on the existing data, the role of hyperandrogenism in influencing OSA risk in women with PCOS is probably small, which might be due to the relatively lower levels of androgens in women with PCOS compared to men.
Large cohort studies with long duration of follow-up are needed to clarify the natural history and relationship between PCOS, OSA, and obesity.
PCOS and OSA... chicken-and-egg?
While obesity is a shared feature between PCOS and OSA that may contribute to the high prevalence of OSA in women with PCOS reported in some studies, other factors may also play an important role in how these two conditions interact [68].
PCOS may contribute to the pathogenesis of OSA through its association with hyperandrogenism and low progesterone levels and may lead to increased upper airway collapsibility, and/or changes in the sensitivity and responsiveness of the ventilatory chemoreceptors [70].
On the other hand, OSA may contribute to the pathogenesis of PCOS through promoting the following: (i) IR [71]; (ii) oxidative stress [72], which may exacerbate IR [73] and contribute to infertility through disruption of the meiotic spindle formation in the oocyte [74]; and (iii) increased sympathetic activity that may lead to IR, altered ovarian function, and the development polycystic ovarian morphology [75, 76].
Subsequently, it is plausible that the relationship between PCOS and OSA is bidirectional [33, 68] (Fig. S3 in the online data supplement). Understanding this relationship is important, as many of the mechanisms through which OSA might impact on PCOS (e.g. IR, inflammation [77], oxidative stress, and sympathetic activation) are amenable to treatment with continuous positive airway pressure (CPAP) [78, 79]. In addition, due to the increased risk of road traffic accidents in patients with OSA, it is important to identify these patients as CPAP lowers this risk [80]. Well-conduced longitudinal large cohort studies and randomised controlled trials are needed to assess the exact relationship between these two common conditions.
Study limitations
We found high heterogeneity in the reported studies. However, this is not unexpected in observational studies. We conducted meta-regression analyses to explore between study-level factors that could explain the observed between study heterogeneity and found that the study population (i.e. adolescents, adults, mixed), and study sample size each explained around one-tenth of the noted heterogeneity. In addition, to prevent wrong or misleading conclusions, meta-analysis rather than narrative synthesis has been recommended even in the presence of high between study variations in the prevalence estimates. Examining the effects of the different cut-offs used to diagnose OSA on its prevalence was not possible as, while some studies reported AHI, others reported RDI or AI when diagnosing OSA, and five studies did not report how OSA was diagnosed. The majority of studies that examined OSA prevalence in PCOS was found to be at high risk of selection bias and did not account for important confounding factors. Subsequently, the prevalence of OSA in women with PCOS reported in this systematic review should be viewed with some caution.
We would like to note a few deviations from our original protocol: we included studies that used level III devices, in addition to polysomnography, as they are validated and approved methods to diagnose OSA [81]. However, all the studies we identified have used polysomnography to diagnose OSA. We accepted the study authors’ own definitions of OSA and PCOS, regardless of the diagnostic criteria used. In five conference abstracts and two journal articles, the authors did not report the criteria used to diagnose OSA and/or PCOS (Table 1). However, we do not believe that these deviations affected our results since we did not find a significant difference in OSA prevalence between conference abstracts and journal articles, neither did we find a difference in OSA prevalence based on the PCOS diagnostic criteria used. In addition, the AHI threshold to diagnose OSA differs between children and adults.
Study strengths
We conducted and reported this systematic review and meta-analysis following internationally recognised recommendations. We have searched a large number of databases/sources to identify relevant articles, and our search was not restricted by study design, language, or publication type or year.
Conclusions
Obstructive sleep apnoea appears to affect a third of women with polycystic ovary syndrome, but this is mainly driven by studies that recruited women with class II obesity and had significant limitations. Whether, and to what extent, women with PCOS are at increased risk of OSA, compared to women without PCOS, remains unclear. Well-conducted, large, cohort studies in the general population with extended follow-up are required to assess the true prevalence of OSA in women with PCOS and to examine the natural history and relationship between PCOS, OSA, and obesity.
References
Fauser BC, Tarlatzis BC, Rebar RW, Legro RS, Balen AH, Lobo R, Carmina E, Chang J, Yildiz BO, Laven JS, Boivin J, Petraglia F, Wijeyeratne CN, Norman RJ, Dunaif A, Franks S, Wild RA, Dumesic D, Barnhart K (2012) Consensus on women’s health aspects of polycystic ovary syndrome (PCOS): the Amsterdam ESHRE/ASRM-Sponsored 3rd PCOS Consensus Workshop Group. Fertil Steril 97(1):28–38 e25. https://doi.org/10.1016/j.fertnstert.2011.09.024
Kyrou I, Weickert MO, Randeva HS (2015) Diagnosis and management of polycystic ovary syndrome (PCOS). In: Ajjan R, Orme SM (eds) Endocrinology and diabetes. Springer, London, pp 99–113
Azziz R, Woods KS, Reyna R, Key TJ, Knochenhauer ES, Yildiz BO (2004) The prevalence and features of the polycystic ovary syndrome in an unselected population. J Clin Endocrinol Metab 89(6):2745–2749. https://doi.org/10.1210/jc.2003-032046
Knochenhauer ES, Key TJ, Kahsar-Miller M, Waggoner W, Boots LR, Azziz R (1998) Prevalence of the polycystic ovary syndrome in unselected black and white women of the southeastern United States: a prospective study. J Clin Endocrinol Metab 83(9):3078–3082
Diamanti-Kandarakis E, Kouli CR, Bergiele AT, Filandra FA, Tsianateli TC, Spina GG, Zapanti ED, Bartzis MI (1999) A survey of the polycystic ovary syndrome in the Greek island of Lesbos: hormonal and metabolic profile. J Clin Endocrinol Metab 84(11):4006–4011
Asuncion M, Calvo RM, San Millan JL, Sancho J, Avila S, Escobar-Morreale HF (2000) A prospective study of the prevalence of the polycystic ovary syndrome in unselected Caucasian women from Spain. J Clin Endocrinol Metab 85(7):2434–2438
Rotterdam EA-SPCWG (2004) Revised 2003 consensus on diagnostic criteria and long-term health risks related to polycystic ovary syndrome. Fertil Steril 81(1):19–25
Kyritsi EM, Dimitriadis GK, Kyrou I, Kaltsas G, Randeva HS (2016) PCOS remains a diagnosis of exclusion: a concise review of key endocrinopathies to exclude. Clin Endocrinol 86:1–6. https://doi.org/10.1111/cen.13245
Glueck CJ, Dharashivkar S, Wang P, Zhu B, Gartside PS, Tracy T, Sieve L (2005) Obesity and extreme obesity, manifest by ages 20-24 years, continuing through 32-41 years in women, should alert physicians to the diagnostic likelihood of polycystic ovary syndrome as a reversible underlying endocrinopathy. Eur J Obstet Gynecol Reprod Biol 122(2):206–212. https://doi.org/10.1016/j.ejogrb.2005.03.010
West S, Vahasarja M, Bloigu A, Pouta A, Franks S, Hartikainen AL, Jarvelin MR, Corbett S, Vaarasmaki M, Morin-Papunen L (2014) The impact of self-reported oligo-amenorrhea and hirsutism on fertility and lifetime reproductive success: results from the Northern Finland Birth Cohort 1966. Hum Reprod 29(3):628–633. https://doi.org/10.1093/humrep/det437
Randeva HS, Tan BK, Weickert MO, Lois K, Nestler JE, Sattar N, Lehnert H (2012) Cardiometabolic aspects of the polycystic ovary syndrome. Endocr Rev 33(5):812–841. https://doi.org/10.1210/er.2012-1003
Moran LJ, Misso ML, Wild RA, Norman RJ (2010) Impaired glucose tolerance, type 2 diabetes and metabolic syndrome in polycystic ovary syndrome: a systematic review and meta-analysis. Hum Reprod Update 16(4):347–363. https://doi.org/10.1093/humupd/dmq001
Barnard L, Ferriday D, Guenther N, Strauss B, Balen AH, Dye L (2007) Quality of life and psychological well being in polycystic ovary syndrome. Hum Reprod 22(8):2279–2286. https://doi.org/10.1093/humrep/dem108
Hahn S, Janssen OE, Tan S, Pleger K, Mann K, Schedlowski M, Kimmig R, Benson S, Balamitsa E, Elsenbruch S (2005) Clinical and psychological correlates of quality-of-life in polycystic ovary syndrome. Eur J Endocrinol 153(6):853–860. https://doi.org/10.1530/eje.1.02024
Cinar N, Kizilarslanoglu MC, Harmanci A, Aksoy DY, Bozdag G, Demir B, Yildiz BO (2011) Depression, anxiety and cardiometabolic risk in polycystic ovary syndrome. Hum Reprod 26(12):3339–3345. https://doi.org/10.1093/humrep/der338
Vgontzas AN, Legro RS, Bixler EO, Grayev A, Kales A, Chrousos GP (2001) Polycystic ovary syndrome is associated with obstructive sleep apnea and daytime sleepiness: role of insulin resistance. J Clin Endocrinol Metab 86(2):517–520. https://doi.org/10.1210/jcem.86.2.7185
Gopal M, Duntley S, Uhles M, Attarian H (2002) The role of obesity in the increased prevalence of obstructive sleep apnea syndrome in patients with polycystic ovarian syndrome. Sleep Med 3(5):401–404
Senaratna CV, Perret JL, Lodge CJ, Lowe AJ, Campbell BE, Matheson MC, Hamilton GS, Dharmage SC (2017) Prevalence of obstructive sleep apnea in the general population: a systematic review. Sleep Med Rev 34:70–81. https://doi.org/10.1016/j.smrv.2016.07.002
Lee W, Nagubadi S, Kryger MH, Mokhlesi B (2008) Epidemiology of obstructive sleep apnea: a population-based perspective. Expert Rev Respir Med 2(3):349–364. https://doi.org/10.1586/17476348.2.3.349
Tahrani AA, Ali A (2014) Oxidative stress, inflammation and endothelial dysfunction: the link between obstructive sleep apnoea and vascular disease in type 2 diabetes. In: Obrosova I, Stevens MJ, Yorek MA (eds) Studies in diabetes, pp 149–170
Peppard PE, Young T, Palta M, Skatrud J (2000) Prospective study of the association between sleep-disordered breathing and hypertension. N Engl J Med 342(19):1378–1384. https://doi.org/10.1056/NEJM200005113421901
Arzt M, Young T, Finn L, Skatrud JB, Bradley TD (2005) Association of sleep-disordered breathing and the occurrence of stroke. Am J Respir Crit Care Med 172(11):1447–1451. https://doi.org/10.1164/rccm.200505-702OC
Peker Y, Hedner J, Norum J, Kraiczi H, Carlson J (2002) Increased incidence of cardiovascular disease in middle-aged men with obstructive sleep apnea: a 7-year follow-up. Am J Respir Crit Care Med 166(2):159–165. https://doi.org/10.1164/rccm.2105124
Marin JM, Carrizo SJ, Vicente E, Agusti AG (2005) Long-term cardiovascular outcomes in men with obstructive sleep apnoea-hypopnoea with or without treatment with continuous positive airway pressure: an observational study. Lancet 365(9464):1046–1053. https://doi.org/10.1016/S0140-6736(05)71141-7
Young T, Finn L, Peppard PE, Szklo-Coxe M, Austin D, Nieto FJ, Stubbs R, Hla KM (2008) Sleep disordered breathing and mortality: eighteen-year follow-up of the Wisconsin sleep cohort. Sleep 31(8):1071–1078
Punjabi NM, Caffo BS, Goodwin JL, Gottlieb DJ, Newman AB, O’Connor GT, Rapoport DM, Redline S, Resnick HE, Robbins JA, Shahar E, Unruh ML, Samet JM (2009) Sleep-disordered breathing and mortality: a prospective cohort study. PLoS Med 6(8):e1000132. https://doi.org/10.1371/journal.pmed.1000132
Wang X, Ouyang Y, Wang Z, Zhao G, Liu L, Bi Y (2013) Obstructive sleep apnea and risk of cardiovascular disease and all-cause mortality: a meta-analysis of prospective cohort studies. Int J Cardiol 169(3):207–214. https://doi.org/10.1016/j.ijcard.2013.08.088
Tregear S, Reston J, Schoelles K, Phillips B (2009) Obstructive sleep apnea and risk of motor vehicle crash: systematic review and meta-analysis. J Clin Sleep Med 5(6):573–581
Finn L, Young T, Palta M, Fryback DG (1998) Sleep-disordered breathing and self-reported general health status in the Wisconsin Sleep Cohort Study. Sleep 21(7):701–706
Akashiba T, Kawahara S, Akahoshi T, Omori C, Saito O, Majima T, Horie T (2002) Relationship between quality of life and mood or depression in patients with severe obstructive sleep apnea syndrome. Chest 122(3):861–865
Engleman HM, Douglas NJ (2004) Sleep. 4: sleepiness, cognitive function, and quality of life in obstructive sleep apnoea/hypopnoea syndrome. Thorax 59(7):618–622
Kloss JD, Perlis ML, Zamzow JA, Culnan EJ, Gracia CR (2015) Sleep, sleep disturbance, and fertility in women. Sleep Med Rev 22:78–87. https://doi.org/10.1016/j.smrv.2014.10.005
Kahal H, Kyrou I, Uthman O, Brown A, Johnson S, Wall P, Metcalfe A, Tahrani AA, Randeva HS (2018) The association between obstructive sleep apnoea and metabolic abnormalities in women with polycystic ovary syndrome: a systematic review and meta-analysis. Sleep 41. https://doi.org/10.1093/sleep/zsy085
McNicholas WT (2008) Diagnosis of obstructive sleep apnea in adults. Proc Am Thorac Soc 5(2):154–160. https://doi.org/10.1513/pats.200708-118MG
Fogel RB, Malhotra A, Pillar G, Pittman SD, Dunaif A, White DP (2001) Increased prevalence of obstructive sleep apnea syndrome in obese women with polycystic ovary syndrome. J Clin Endocrinol Metab 86(3):1175–1180. https://doi.org/10.1210/jcem.86.3.7316
Legro RS, Arslanian SA, Ehrmann DA, Hoeger KM, Murad MH, Pasquali R, Welt CK, Endocrine S (2013) Diagnosis and treatment of polycystic ovary syndrome: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab 98(12):4565–4592. https://doi.org/10.1210/jc.2013-2350
Yang HP, Kang JH, Su HY, Tzeng CR, Liu WM, Huang SY (2009) Apnea-hypopnea index in nonobese women with polycystic ovary syndrome. Int J Gynaecol Obstet 105(3):226–229. https://doi.org/10.1016/j.ijgo.2009.02.004
Helvaci N, Karabulut E, Demir AU, Yildiz BO (2017) Polycystic ovary syndrome and the risk of obstructive sleep apnea: a meta-analysis and review of the literature. Endocr Connect 6(7):437–445. https://doi.org/10.1530/EC-17-0129
Greenstone M, Hack M (2014) Obstructive sleep apnoea. BMJ 348:g3745. https://doi.org/10.1136/bmj.g3745
Stroup DF, Berlin JA, Morton SC, Olkin I, Williamson GD, Rennie D, Moher D, Becker BJ, Sipe TA, Thacker SB (2000) Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis Of Observational Studies in Epidemiology (MOOSE) group. JAMA 283(15):2008–2012
Kim SY, Park JE, Lee YJ, Seo HJ, Sheen SS, Hahn S, Jang BH, Son HJ (2013) Testing a tool for assessing the risk of bias for nonrandomized studies showed moderate reliability and promising validity. J Clin Epidemiol 66(4):408–414. https://doi.org/10.1016/j.jclinepi.2012.09.016
DerSimonian R, Laird N (1986) Meta-analysis in clinical trials. Control Clin Trials 7(3):177–188
Higgins JP, Thompson SG (2002) Quantifying heterogeneity in a meta-analysis. Stat Med 21(11):1539–1558. https://doi.org/10.1002/sim.1186
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327(7414):557–560. https://doi.org/10.1136/bmj.327.7414.557
Dunaif A, Givens JR, Haseltine FP (1992) Polycystic ovary syndrome. Blackwell, Oxford
Egger M, Davey Smith G, Schneider M, Minder C (1997) Bias in meta-analysis detected by a simple, graphical test. BMJ 315(7109):629–634
Normand SL (1999) Meta-analysis: formulating, evaluating, combining, and reporting. Stat Med 18(3):321–359
AbdelWahab NH, Mahmoud MI, Abdelnaby MA, Morsi TS, Abdelfatah MF (2013) Sleep-related breathing disorders in Egyptian females with polycystic ovary syndrome. Paper presented at the American Thoracic Society International Conference, ATS, Philadelphia
Chatterjee B, Suri J, Suri JC, Mittal P, Adhikari T (2014) Impact of sleep-disordered breathing on metabolic dysfunctions in patients with polycystic ovary syndrome. Sleep Med 15(12):1547–1553. https://doi.org/10.1016/j.sleep.2014.06.023
de Sousa G, Schluter B, Buschatz D, Menke T, Trowitzsch E, Andler W, Reinehr T (2012) The impact of insulin resistance and hyperandrogenemia on polysomnographic variables in obese adolescents with polycystic ovarian syndrome. Sleep Breath 16(1):169–175. https://doi.org/10.1007/s11325-010-0469-6
Gateva A, Kamenov Z, Mondeshki T, Bilyukov R, Georgiev O (2013) Obstructive sleep apnea in Bulgarian patients with polycystic ovarian syndrome. Paper presented at the 15th European Congress of Endocrinology, Copenhagen, Denmark
Kenigsberg L, Agarwal A, Arens R, Heptulla R (2015) Is insulin resistance and obstructive sleep apnea present in obese and lean adolescents with PCOS? Paper presented at the Endocrine Society’s 97th Annual Meeting and Expo, San Diego
Morselli LL, Temple KA, Mokhlesi B, Tasali E, Chapotot F, Van Cauter E, Ehrmann DA (2013) Effects of polycystic ovary syndrome (PCOS) on REM and non-REM sleep in African-American (AA) women. Paper presented at the 95th Annual Meeting and Expo of the Endocrine Society, ENDO, San Francisco, CA United States
Nandalike K, Agarwal C, Strauss T, Coupey SM, Isasi CR, Sin S, Arens R (2012) Sleep and cardiometabolic function in obese adolescent girls with polycystic ovary syndrome. Sleep Med 13(10):1307–1312. https://doi.org/10.1016/j.sleep.2012.07.002
Saha S, Sinha S, Sharma SK, Soneja M, Nischal N, Pandey RM (2018) Sleep disorders in polycystic ovary syndrome (PCOS) and their metabolic correlates. American Journal of Respiratory and Critical Care Medicine Conference: American Thoracic Society International Conference, ATS 197 (MeetingAbstracts)
Tasali E, Van Cauter E, Hoffman L, Ehrmann DA (2008) Impact of obstructive sleep apnea on insulin resistance and glucose tolerance in women with polycystic ovary syndrome. J Clin Endocrinol Metab 93(10):3878–3884. https://doi.org/10.1210/jc.2008-0925
Temple KA, Tasali E, Mokhlesi B, Whitmore H, Watson S, Van Cauter E, Ehrmann DA (2013) Abnormal glucose tolerance in women with polycystic ovary syndrome (PCOS): role of sex steroids and obstructive sleep apnea. Paper presented at the 73rd Scientific Sessions of the American Diabetes Association, Chicago, IL United States
Tock L, Carneiro G, Togeiro SM, Hachul H, Pereira AZ, Tufik S, Zanella MT (2014) Obstructive sleep apnea predisposes to nonalcoholic fatty liver disease in patients with polycystic ovary syndrome. Endocr Pract 20(3):244–251. https://doi.org/10.4158/EP12366.OR
Wootton DM, Luo H, Yazdani A, Sin S, McDonough J, Isasi CR, Wagshul ME, Arens R (2017) Increased cfd pharyngeal airway flow resistance in adolescent girls with polycystic ovarian syndrome and obstructive sleep apnea syndrome. American Journal of Respiratory and Critical Care Medicine Conference: American Thoracic Society International Conference, ATS 195 (no pagination). https://doi.org/10.1164/ajrccm-conference.2017.D30
Zea-Hernandez J, Sin S, Graw-Panzer K, Arens R (2014) Sleep disordered breathing in adolescent girls with polycystic ovary syndrome. Paper presented at the American Thoracic Society International Conference, ATS
de Sousa G, Schluter B, Buschatz D, Menke T, Trowitzsch E, Andler W, Reinehr T (2010) A comparison of polysomnographic variables between obese adolescents with polycystic ovarian syndrome and healthy, normal-weight and obese adolescents. Sleep Breath 14(1):33–38. https://doi.org/10.1007/s11325-009-0276-0
de Sousa G, Schluter B, Menke T, Trowitzsch E, Andler W, Reinehr T (2012) Longitudinal analyses of polysomnographic variables, serum androgens, and parameters of glucose metabolism in obese adolescents with polycystic ovarian syndrome. Sleep Breath 16(4):1139–1146. https://doi.org/10.1007/s11325-011-0620-z
de Sousa G, Schluter B, Menke T, Trowitzsch E, Andler W, Reinehr T (2011) A comparison of polysomnographic variables between adolescents with polycystic ovarian syndrome with and without the metabolic syndrome. Metab Syndr Relat Disord 9(3):191–196. https://doi.org/10.1089/met.2010.0081
Vgontzas AN, Trakada G, Bixler EO, Lin HM, Pejovic S, Zoumakis E, Chrousos GP, Legro RS (2006) Plasma interleukin 6 levels are elevated in polycystic ovary syndrome independently of obesity or sleep apnea. Metabolism 55(8):1076–1082. https://doi.org/10.1016/j.metabol.2006.04.002
Tahrani AA (2015) Diabetes and sleep apnea. In: DeFronzo RA, Ferrannini E, Alberti G (eds) International textbook of diabetes mellitus, 4th edn, pp 316–336
Sir-Petermann T, Codner E, Maliqueo M, Echiburu B, Hitschfeld C, Crisosto N, Perez-Bravo F, Recabarren SE, Cassorla F (2006) Increased anti-Mullerian hormone serum concentrations in prepubertal daughters of women with polycystic ovary syndrome. J Clin Endocrinol Metab 91(8):3105–3109. https://doi.org/10.1210/jc.2005-2693
Crisosto N, Codner E, Maliqueo M, Echiburu B, Sanchez F, Cassorla F, Sir-Petermann T (2007) Anti-Mullerian hormone levels in peripubertal daughters of women with polycystic ovary syndrome. J Clin Endocrinol Metab 92(7):2739–2743. https://doi.org/10.1210/jc.2007-0267
Kahal H, Kyrou I, Tahrani AA, Randeva HS (2017) Obstructive sleep apnoea and polycystic ovary syndrome: a comprehensive review of clinical interactions and underlying pathophysiology. Clin Endocrinol 87:313–319. https://doi.org/10.1111/cen.13392
Kang KT, Chou CH, Weng WC, Lee PL, Hsu WC (2013) Associations between adenotonsillar hypertrophy, age, and obesity in children with obstructive sleep apnea. PLoS One 8(10):e78666. https://doi.org/10.1371/journal.pone.0078666
Kapsimalis F, Kryger MH (2002) Gender and obstructive sleep apnea syndrome, part 2: mechanisms. Sleep 25(5):499–506
Tahrani AA, Ali A, Stevens MJ (2013) Obstructive sleep apnoea and diabetes: an update. Curr Opin Pulm Med 19(6):631–638. https://doi.org/10.1097/MCP.0b013e3283659da5
Tahrani AA, Ali A, Raymond NT, Begum S, Dubb K, Mughal S, Jose B, Piya MK, Barnett AH, Stevens MJ (2012) Obstructive sleep apnea and diabetic neuropathy: a novel association in patients with type 2 diabetes. Am J Respir Crit Care Med 186(5):434–441. https://doi.org/10.1164/rccm.201112-2135OC
Zuo T, Zhu M, Xu W (2016) Roles of oxidative stress in8589318 polycystic ovary syndrome and cancers. Oxidative Med Cell Longev 2016. https://doi.org/10.1155/2016/8589318
Chattopadhayay R, Ganesh A, Samanta J, Jana SK, Chakravarty BN, Chaudhury K (2010) Effect of follicular fluid oxidative stress on meiotic spindle formation in infertile women with polycystic ovarian syndrome. Gynecol Obstet Investig 69(3):197–202. https://doi.org/10.1159/000270900
Lansdown A, Rees DA (2012) The sympathetic nervous system in polycystic ovary syndrome: a novel therapeutic target? Clin Endocrinol 77(6):791–801. https://doi.org/10.1111/cen.12003
Dissen GA, Garcia-Rudaz C, Paredes A, Mayer C, Mayerhofer A, Ojeda SR (2009) Excessive ovarian production of nerve growth factor facilitates development of cystic ovarian morphology in mice and is a feature of polycystic ovarian syndrome in humans. Endocrinology 150(6):2906–2914. https://doi.org/10.1210/en.2008-1575
Altaf QA, Ali A, Piya MK, Raymond NT, Tahrani AA (2016) The relationship between obstructive sleep apnea and intra-epidermal nerve fiber density, PARP activation and foot ulceration in patients with type 2 diabetes. J Diabetes Complicat 30(7):1315–1320. https://doi.org/10.1016/j.jdiacomp.2016.05.025
Iftikhar IH, Khan MF, Das A, Magalang UJ (2013) Meta-analysis: continuous positive airway pressure improves insulin resistance in patients with sleep apnea without diabetes. Ann Am Thorac Soc 10(2):115–120. https://doi.org/10.1513/AnnalsATS.201209-081OC
Hedner J, Darpo B, Ejnell H, Carlson J, Caidahl K (1995) Reduction in sympathetic activity after long-term CPAP treatment in sleep apnoea: cardiovascular implications. Eur Respir J 8(2):222–229
Karimi M, Hedner J, Habel H, Nerman O, Grote L (2015) Sleep apnea-related risk of motor vehicle accidents is reduced by continuous positive airway pressure: Swedish Traffic Accident Registry data. Sleep 38(3):341–349. https://doi.org/10.5665/sleep.4486
Kapur VK, Auckley DH, Chowdhuri S, Kuhlmann DC, Mehra R, Ramar K, Harrod CG (2017) Clinical practice guideline for diagnostic testing for adult obstructive sleep apnea: an American Academy of Sleep Medicine clinical practice guideline. J Clin Sleep Med 13(3):479–504. https://doi.org/10.5664/jcsm.6506
Acknowledgements
Dr. Abd Tahrani is a Clinician Scientist supported by the National Institute for Health Research (NIHR). Dr. Olalekan Uthman is supported by the National Institute of Health Research using Official Development Assistance (ODA) funding. NIHR Clinical Lectureship supported Dr. Hassan Kahal.
Author information
Authors and Affiliations
Contributions
HK, IK, OAU, AM, PDHW, AAT, and HSR contributed to study design. AB and SJ designed search strategies and performed literature search. HK and IK selected studies, extracted data, and assessed risk of bias. OAU performed data analyses. HK, IK, OAU, AM, DGP, AAT, and HSR contributed to data interpretation. HK wrote the first draft of report. All authors critically reviewed the paper and approved the final version of the manuscript. AAT and HSR are joint senior authors and contributed equally to the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare that there is no conflict of interest.
Disclaimer
The views expressed in this publication are those of the authors and not necessarily those of the NHS, the National Institute for Health Research, or the Department of Health.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 672 kb)
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Kahal, H., Kyrou, I., Uthman, O.A. et al. The prevalence of obstructive sleep apnoea in women with polycystic ovary syndrome: a systematic review and meta-analysis. Sleep Breath 24, 339–350 (2020). https://doi.org/10.1007/s11325-019-01835-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-019-01835-1