Abstract
Purpose
Obstructive sleep apnea (OSA) is very common occurrence among morbidly obese patients. Our main objectives were to validate the No-Apnea, a 2-item screening tool, in morbidly obese patients and compare its performance with three other instruments: STOP-Bang questionnaire, NoSAS score, and Epworth Sleepiness Scale (ESS).
Methods
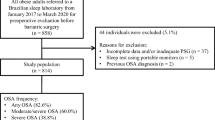
A cross-sectional analysis of morbidly obese patients (body mass index [BMI] ≥ 35.0 kg/m2) grouped into two independent samples: bariatric surgery patients (BS) and non-bariatric surgery patients (NBS). All patients underwent overnight polysomnography. Discriminatory ability was assessed by area under the curve (AUC). OSA severity was defined by apnea/hypopnea index cut-off points: ≥ 5.0/h (OSA≥5), ≥ 15.0/h (OSA≥15), and ≥ 30.0/h (OSA≥30).
Results
A total of 1017 subjects (40.4% in BS cohort and 59.6% in NBS cohort) were evaluated. In the BS cohort, No-Apnea had similar discrimination to STOP-Bang and NoSAS for predicting OSA≥5 (p = 0.979 and p = 0.358, respectively), OSA≥15 (p = 0.158 and p = 0.399, respectively), and OSA≥30 (p = 0.388 and p = 0.903, respectively). In the NBS cohort, No-Apnea had similar discrimination to STOP-Bang and NoSAS for predicting OSA≥5 (p = 0.528 and p = 0.428, respectively), OSA≥15 (p = 0.825 and p = 0.108, respectively), and OSA≥30 (p = 0.458 and p = 0.186, respectively). Moreover, No-Apnea performed significantly better than ESS in both BS and NBS cohorts (p < 0.001).
Conclusions
No-Apnea is a useful and practical tool for screening of OSA in morbidly obese patients, with non-inferior performance to STOP-Bang questionnaire and NoSAS score.



Similar content being viewed by others
References
Peppard PE, Young T, Barnet JH, Palta M, Hagen EW, Hla KM (2013) Increased prevalence of sleep-disordered breathing in adults. Am J Epidemiol 177:1006–1014
Heinzer R, Vat S, Marques-Vidal P, Martin-Soler H, Andries D, Tobback N, Mooser V, Preisig M, Malhotra A, Waeber G, Vollenweider P, Tafti M, Haba-Rubio J (2015) Prevalence of sleep-disordered breathing in the general population: the HypnoLaus study. Lancet Respir Med 3:310–318
Kapur VK, Auckley DH, Chowdhuri S, Kuhlmann DC, Mehra R, Ramar K, Harrod CG (2017) Clinical practice guideline for diagnostic testing for adult obstructive sleep apnea: an American Academy of Sleep Medicine clinical practice guideline. J Clin Sleep Med 13:479–504
Mortimore I, Marshall I, Wraith PK, Sellar RJ, Douglas NJ (1998) Neck and total body fat deposition in nonobese and obese patients with sleep apnea compared with that in control subjects. Am J Respir Crit Care Med 157:280–283
Kositanurit W, Muntham D, Udomsawaengsup S, Chirakalwasan N (2018) Prevalence and associated factors of obstructive sleep apnea in morbidly obese patients undergoing bariatric surgery. Sleep Breath 22:251–256
Duarte RL, Magalhães-da-Silveira FJ (2015) Factors predictive of obstructive sleep apnea in patients undergoing pre-operative evaluation for bariatric surgery and referred to a sleep laboratory for polysomnography. J Bras Pneumol 41:440–448
Rasmussen JJ, Fuller WD, Ali MR (2012) Sleep apnea syndrome is significantly underdiagnosed in bariatric surgical patients. Surg Obes Relat Dis 8:569–573
Ravesloot MJ, van Maanen JP, Hilgevoord AA, van Wagensveld BA, de Vries N (2012) Obstructive sleep apnea is underrecognized and underdiagnosed in patients undergoing bariatric surgery. Eur Arch Otorhinolaryngol 269:1865–1871
O’Keeffe T, Patterson EJ (2004) Evidence supporting routine polysonography before bariatric surgery. Obes Surg 14:23–26
Nepomnayshy D, Hesham W, Erikson B, MacDonald J, Iorio R, Brams D (2013) Sleep apnea: is routine preoperative screening necessary? Obes Surg 23:287–291
Kong WT, Chopra S, Kopf M, Morales C, Khan S, Zuccala K, Choi L, Chronakos J (2016) Perioperative risks of untreated obstructive sleep apnea in the bariatric surgery patient: a retrospective study. Obes Surg 26:2886–2890
Carron M, Zarantonello F, Tellaroli P, Ori C (2016) Perioperative noninvasive ventilation in obese patients: a qualitative review and meta-analysis. Surg Obes Relat Dis 12:681–692
Muraja-Murro A, Kulkas A, Hiltunen M, Kupari S, Hukkanen T, Tiihonen P, Mervaala E, Töyräs J (2013) The severity of individual obstruction events is related to increased mortality rate in severe obstructive sleep apnea. J Sleep Res 22:663–669
Oliveira MG, Treptow EC, Fukuda C, Nery LE, Valadares RM, Tufik S, Bittencourt L, Togeiro SM (2015) Diagnostic accuracy of home-based monitoring system in morbidly obese patients with high risk for sleep apnea. Obes Surg 25:845–851
Duarte RLM, Rabahi MF, Magalhães-da-Silveira FJ, Oliveira-e-Sá TS, Mello FCQ, Gozal D (2018) Simplifying the screening of obstructive sleep apnea with a 2-item model, No-Apnea: a cross-sectional study. J Clin Sleep Med 14:1097–1107
Chung F, Yegneswaran B, Liao P, Chung SA, Vairavanathan S, Islam S, Khajehdehi A, Shapiro CM (2008) STOP questionnaire: a tool to screen patients for obstructive sleep apnea. Anesthesiology 108:812–821
Marti-Soler H, Hirotsu C, Marques-Vidal P, Vollenweider P, Waeber G, Preisig M, Tafti M, Tufik SB, Bittencourt L, Tufik S, Haba-Rubio J, Heinzer R (2016) The NoSAS score for screening of sleep-disordered breathing: a derivation and validation study. Lancet Respir Med 4:742–748
Reed K, Pengo MF, Steier J (2016) Screening for sleep-disordered breathing in a bariatric population. J Thorac Dis 8:268–275
Horvath CM, Jossen J, Kröll D, Nett PC, Baty F, Brill AK, Ott SR (2018) Prevalence and prediction of obstructive sleep apnea prior to bariatric surgery-gender-specific performance of four sleep questionnaires. Obes Surg 28:2720–2726
Johns MW (1991) A new method for measuring daytime sleepiness: the Epworth sleepiness scale. Sleep 14:540–545
Chung F, Yang Y, Liao P (2013) Predictive performance of the STOP-Bang score for identifying obstructive sleep apnea in obese patients. Obes Surg 23:2050–2057
Berry RB, Budhiraja R, Gottlieb DJ, Gozal D, Iber C, Kapur VK, Marcus CL, Mehra R, Parthasarathy S, Quan SF, Redline S, Strohl KP, Davidson Ward SL, Tangredi MM, American Academy of Sleep Medicine (2012) Rules for scoring respiratory events in sleep: update of the 2007 AASM manual for the scoring of sleep and associated events. J Clin Sleep Med 8:597–619
Hanley JA, McNeil BJ (1983) A method of comparing the areas under receiver operating characteristic curves derived from the same cases. Radiology 148:839–843
Duarte RLM, Fonseca LBM, Magalhães-da-Silveira FJ, Silveira EAD, Rabahi MF (2017) Validation of the STOP-Bang questionnaire as a means of screening for obstructive sleep apnea in adults in Brazil. J Bras Pneumol 43:456–463
Nagappa M, Liao P, Wong J, Auckley D, Ramachandran SK, Memtsoudis S, Mokhlesi B, Chung F (2015) Validation of the STOP-Bang questionnaire as a screening tool for obstructive sleep apnea among different populations: a systematic review and meta-analysis. PLoS One 10:e0143697
Glazer SA, Erickson AL, Crosby RD, Kieda J, Zawisza A, Deitel M (2018) The evaluation of screening questionnaires for obstructive sleep apnea to identify high-risk obese patients undergoing bariatric surgery. Obes Surg 28:3544–3552
Tan A, Hong Y, Tan LWL, van Dam RM, Cheung YY, Lee CH (2017) Validation of NoSAS score for screening of sleep-disordered breathing in a multiethnic Asian population. Sleep Breath 21:1033–1038
Hong C, Chen R, Qing S, Kuang A, Yang H, Su X, Zhao D, Wu K, Zhang N (2018) Validation of the NoSAS score for the screening of sleep-disordered breathing: a hospital-based retrospective study in China. J Clin Sleep Med 14:191–197
Vana KD, Silva GE, Goldberg R (2013) Predictive abilities of the STOP-bang and Epworth sleepiness scale in identifying sleep clinic patients at high risk for obstructive sleep apnea. Res Nurs Health 36:84–94
Panchasara B, Poots AJ, Davies G (2017) Are the Epworth sleepiness scale and Stop-Bang model effective at predicting the severity of obstructive sleep apnoea (OSA); in particular OSA requiring treatment? Eur Arch Otorhinolaryngol 274:4233–4239
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The authors declare that the protocol of the research work was approved by the Ethics Commission of the Universidade Federal do Rio de Janeiro (UFRJ) according to the Helsinki Declaration, and all the patients provided written informed consent.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Duarte, R.L.M., Mello, F.C.Q., Magalhães-da-Silveira, F.J. et al. Comparative performance of screening instruments for obstructive sleep apnea in morbidly obese patients referred to a sleep laboratory: a prospective cross-sectional study. Sleep Breath 23, 1123–1132 (2019). https://doi.org/10.1007/s11325-019-01791-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-019-01791-w