Abstract
Background
Inflammation plays a role in the pathogenesis and consequences of sleep-disordered breathing (SDB). The nasal mucosa and paranasal sinuses produce high levels of nitric oxide (NO). In asthma, exhaled NO is a marker of airway inflammation. There is only limited information whether nasal NO (nNO) accompanies also chronic upper airway obstruction, specifically, SDB. The objective of this study was to investigate nNO levels in children with SDB in comparison to healthy non-snoring children.
Methods
Nasal NO was measured in children who underwent overnight polysomnographic studies due to habitual snoring and suspected SDB and in healthy non-snoring controls.
Results
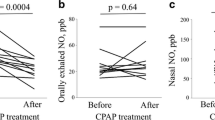
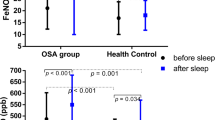
One hundred and eleven children participated in the study: 28 with obstructive sleep apnea (OSA), 60 with primary snoring (PS), and 23 controls. Nasal NO levels were significantly higher in children with OSA and PS compared to controls (867.4 ± 371.5, 902.0 ± 330.9, 644.1 ± 166.5 ppb, respectively, p = 0.047). No difference was observed between children with OSA and PS. No correlations were found between nNO levels and any of the PSG variables, nor with age, BMI percentile or tonsils size.
Conclusions
Compared to healthy controls, nNO is increased in children with SDB, but it is not correlated with disease severity. This is probably due to the local mechanical processes and snoring.


Similar content being viewed by others
Abbreviations
- ADD:
-
Attention deficit disorder
- AHI:
-
Apnea/hypopnea index
- AT:
-
Adenotonsillectomy
- BMI:
-
Body mass index
- ENO:
-
Exhaled nitric oxide
- nNO:
-
Nasal nitric oxide
- NO:
-
Nitric oxide
- OSA:
-
Obstructive sleep apnea
- PPB:
-
Parts per billion
- PS:
-
Primary snoring
- PSG:
-
Polysomnography
- SDB:
-
Sleep-disordered breathing
- SpO2:
-
Blood oxygen saturation
- TST:
-
Total sleep time
References
Tal A (2014) Obstructive sleep apnea syndrome: pathophysiology and clinical characteristics. In: Sheldon SH, Ferber R, Kryger MH, Gozal D (eds) Principles and practice of pediatric sleep medicine, 2nd edn. Elseveir, London, pp 215–220
Kim J, Hakim F, Kheirandish-Gozal L, Gozal D (2011) Inflammatory pathways in children with insufficient or disordered sleep. Respir Physiol Neurobiol 178:465–474
Gozal D, Kheirandish L (2006) Oxidant stress and inflammation in the snoring child: confluent pathways to upper airway pathogenesis and end-organ morbidity. Sleep Med Rev 10:83–96
Goldbart AD, Tal A (2008) Inflammation and sleep disordered breathing in children: a state-of-the-art review. Pediatr Pulmonol 43:1151–1160
Hatipoğlu U, Rubinstein I (2003) Inflammation and obstructive sleep apnea syndrome pathogenesis: a working hypothesis. Respiration 70:665–671
Kent BD, Ryan S, McNicholas WT (2011) Obstructive sleep apnea and inflammation: relationship to cardiovascular co-morbidity. Respir Physiol Neurobiol 178:475–481
Rubinstein I (1995) Nasal inflammation in patients with obstructive sleep apnea. Laryngoscope 105:175–177
Salerno FG, Carpagnano E, Guido P, Bonsignore MR, Roberti A, Aliani M, Vignola AM, Spanevello A (2004) Airway inflammation in patients affected by obstructive sleep apnea syndrome. Respir Med 98:25–28
Carpagnano GE (2011) Exhaled breath analysis and sleep. J Clin Sleep Med 7:S34–S37
Sekosan M, Zakkar M, Wenig BL, Olopade CO, Rubinstein I (1996) Inflammation in the uvula mucosa of patients with obstructive sleep apnea. Laryngoscope 106:1018–1020
Boyd JH, Petrof BJ, Hamid Q, Fraser R, Kimoff RJ (2004) Upper airway muscle inflammation and denervation changes in obstructive sleep apnea. Am J Respir Crit Care Med 170:541–546
Philippe C, Boussadia Y, Prulière-Escabasse V, Papon JF, Clérici C, Isabey D, Coste A, Escudier E, d’Ortho MP (2015) Airway cell involvement in intermittent hypoxia-induced airway inflammation. Sleep Breath 19:297–306
Goldbart AD, Goldman JL, Li RC, Brittian KR, Tauman R, Gozal D (2004) Differential expression of cysteinyl leukotriene receptors 1 and 2 in tonsils of children with obstructive sleep apnea syndrome or recurrent infection. Chest 126:13–18
Li AM, Hung E, Tsang T, Yin J, So HK, Wong E, Fok TF, Ng PC (2007) Induced sputum inflammatory measures correlate with disease severity in children with obstructive sleep apnoea. Thorax 62:75–79
Goldbart AD, Krishna J, Li RC, Serpero LD, Gozal D (2006) Inflammatory mediators in exhaled breath condensate of children with obstructive sleep apnea syndrome. Chest 130:143–148
Benedek P, Lazar Z, Bikov A, Kunos L, Katona G, Horvath I (2013) Exhaled biomarker pattern is altered in children with obstructive sleep apnoea syndrome. Int J Pediatr Otorhinolaryngol 77:1244–1247
Malakasioti E, Alexopoulos C, Befani K, Tanou V, Varlami D, Ziogas D, Liakos P, Gourgoulianis K, Kaditis AG (2012) Oxidative stress and inflammatory markers in the exhaled breath condensate of children with OSA. Sleep Breath 16:703–718
Kaditis AG, Ioannou MG, Chaidas K, Alexopoulos EI, Apostolidou M, Apostolidis T, Koukoulis G, Gourgoulianis K (2008) Cysteinyl leukotriene receptors are expressed by tonsillar T cells of children with obstructive sleep apnea. Chest 134:324–331
Dayyat E, Serpero LD, Kheirandish-Gozal L, Goldman JL, Snow A, Bhattacharjee R, Gozal D (2009) Leukotriene pathways and in vitro adenotonsillar cell proliferation in children with obstructive sleep apnea. Chest 135:1142–1149
Goldbart AD, Goldman JL, Veling MC, Gozal D (2005) Leukotriene modifier therapy for mild sleep-disordered breathing in children. Am J Respir Crit Care Med 172:364–370
Goldbart AD, Greenberg-Dotan S, Tal A (2012) Montelukast for children with obstructive sleep apnea: a double-blind, placebo-controlled study. Pediatrics 130:e575–e580
Almendros I, Acerbi I, Puig F, Montserrat JM, Navajas D, Farré R (2007) Upper-airway inflammation triggered by vibration in a rat model of snoring. Sleep 30:225–227
Barnes PJ, Dweik RA, Gelb AF, Gibson PG, George SC, Grasemann H, Pavord ID, Ratjen F, Silkoff PE, Taylor DR, Zamel N (2010) Exhaled nitric oxide in pulmonary diseases: a comprehensive review. Chest 138:682–692
Lundberg JO, Rinder J, Weitzberg E, Lundberg JM, Alving K (1994) Nasally exhaled nitric oxide in humans originates mainly in the paranasal sinuses. Acta Physiol Scand 152:431–432
Corbelli R, Hammer J (2007) Measurement of nasal nitric oxide. Paed Resp Rev 8:269–672
Struben VM, Wieringa MH, Feenstra L, de Jongste JC (2006) Nasal nitric oxide and nasal allergy. Allergy 61:665–670
Arnal JF, Didier A, Rami J, M’Rini C, Charlet JP, Serrano E, Besombes JP (1997) Nasal nitric oxide is increased in allergic rhinitis. Clin Exp Allergy 27:358–362
Baraldi E, Azzolin NM, Carra S, Dario C, Marchesini L, Zacchello F (1998) Effect of topical steroids on nasal nitric oxide production in children with perennial allergic rhinitis: a pilot study. Respir Med 92:558–561
Palm JP, Alving K, Lundberg JO (2003) Characterization of airway nitric oxide in allergic rhinitis: the effect of intranasal administration of l-NAME. Allergy 58:885–892
Maniscalco M, Sofia M, Carratu L, Higenbottam T (2001) Effect of nitric oxide inhibition on nasal airway resistance after nasal allergen challenge in allergic rhinitis. Eur J Clin Invest 31:462–466
Petrosyan M, Perraki E, Simoes D, Koutsourelakis I, Vagiakis E, Roussos C, Gratziou C (2008) Exhaled breath markers in patients with obstructive sleep apnoea. Sleep Breath 12:207–215
Brodsky L, Adler E, Stanievich JF (1989) Naso- and oropharyngeal dimensions in children with obstructive sleep apnea. Int J Pediatr Otorhinolaryngol 17:1–11
Section on Pediatric Pulmonology, Subcommittee on Obstructive Sleep Apnea Syndrome. American Academy of Pediatrics (2002) Clinical practice guideline: diagnosis and management of childhood obstructive sleep apnea syndrome. Pediatrics 109:704–712
Marcus CL, Omlin KJ, Basinki DJ, Bailey SL, Rachal AB, Von Pechmann WS, Keens TG, Ward SL (1994) Normal polysomnographic values for children and adolescents. Am J Respir Crit Care Med 149:715–721
Uliel S, Tauman R, Greenfeld M, Sivan Y (2004) Normal polysomnographic respiratory values in children and adolescents. Chest 125:872–878
American Thoracic Society; European Respiratory Society (2005) ATS/ERS recommendations for standardized procedures for the online and offline measurement of exhaled lower respiratory nitric oxide and nasal nitric oxide. Am J Respir Crit Care Med 171:912–930
Carpagnano GE, Spanevello A, Sabato R, Depalo A, Turchiarelli V, Foschino Barbaro MP (2008) Exhaled pH, exhaled nitric oxide, and induced sputum cellularity in obese patients with obstructive sleep apnea syndrome. Transl Res 151:45–50
Culla B, Guida G, Brussino L, Tribolo A, Cicolin A, Sciascia S, Badiu I, Mietta S, Bucca C (2010) Increased oral nitric oxide in obstructive sleep apnoea. Respir Med 104:316–320
Puig F, Rico F, Almendros I, Montserrat JM, Navajas D, Farre R (2005) Vibration enhances interleukin-8 release in a cell model of snoring induced airway inflammation. Sleep 28:1312–1316
Marcus CL, Brooks LJ, Draper KA, Gozal D, Halbower AC, Jones J, Schechter MS, Ward SD, Sheldon SH, Shiffman RN, Lehmann C, Spruyt K, American Academy of Pediatrics (2012) Diagnosis and management of childhood obstructive sleep apnea syndrome. Pediatrics 130:e714–e755
Acknowledgments
We are grateful to Bat-el Yakir, Ety Kadosh, and Ety Zefania for their help and support.
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gut, G., Tauman, R., Greenfeld, M. et al. Nasal nitric oxide in sleep-disordered breathing in children. Sleep Breath 20, 303–308 (2016). https://doi.org/10.1007/s11325-015-1189-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-015-1189-8