Abstract
Cerebral hypoperfusion and vascular dysfunction are closely related to common risk factors for ischemic stroke such as hypertension, dyslipidemia, diabetes, and smoking. The role of inhibitory G protein-dependent receptor (GiPCR) signaling in regulating cerebrovascular functions remains largely elusive. We examined the importance of GiPCR signaling in cerebral blood flow (CBF) and its stability after sudden interruption using various in vivo high-resolution magnetic resonance imaging techniques. To this end, we induced a functional knockout of GiPCR signaling in the brain vasculature by injection of pertussis toxin (PTX). Our results show that PTX induced global brain hypoperfusion and microvascular collapse. When PTX-pretreated animals underwent transient unilateral occlusion of one common carotid artery, CBF was disrupted in the ipsilateral hemisphere resulting in the collapse of the cortically penetrating microvessels. In addition, pronounced stroke features in the affected brain regions appeared in both MRI and histological examination. Our findings suggest an impact of cerebrovascular GiPCR signaling in the maintenance of CBF, which may be useful for novel pharmacotherapeutic approaches to prevent and treat cerebrovascular dysfunction and stroke.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Gi proteins are the principal signal transducers of a broad subset of G protein-coupled receptors (termed GiPCRs), including those for acetylcholine, adenosine, and catecholamines that control blood circulation [1,2,3,4,5]. In spite of many studies, the functions of Gi protein-dependent signaling in the brain vasculature have been largely ignored. One major reason for the undefined role of Gi proteins may be the lack of appropriate animal models, since a simultaneous genetic ablation of the major Gαi isoforms (Gαi2 and Gαi3) produces embryonic lethality in mice [6]. On the other hand, the significance of singular knockouts is limited by overlapping functions of these isoforms. Pertussis toxin (PTX) has been used to study Gi protein signaling in the cardiovascular system [7, 8], but the effects on cerebrovasculature have not yet been elucidated.
In vivo, PTX irreversibly and with high specificity blocks Gi-linked GPCR signal transduction — hereafter referred to as non-cerebral GiPCR KO — by catalyzing covalent modification of a C-terminal cysteine residue of cellular Gαi isoforms [9,10,11]. In arteries and microvessels, PTX inhibits endothelium-dependent relaxation to certain agonists such as β-adrenergic ligands, angiotensin, serotonin, or relaxins and is therefore useful for the study of vasculopathies [2, 7, 8, 12,13,14,15,16,17,18]. We have previously demonstrated that PTX, administered in a single peritoneal injection, does not cross the blood–brain barrier (BBB) and does not modify GiPCR signaling in neurons [19]. PTX administration, however, still irreversibly interrupts GiPCR signaling for up to 96 h in cells outside of the CNS, including brain vasculature. Using PTX, in this work, we evaluate the effects in cerebral blood flow caused by permanent GiPCR modification of cells outside of the brain.
MRI provides a powerful set of neuroimaging tools that allow quantification of pathological changes at the functional level in the brain [20,21,22]. In vivo MRI allows consistent acquisition of multiple tissue characteristics in a single session permitting evaluation of their longitudinal development [20, 22].
In the present study, we focused, first, on the effects of PTX administration in systemic blood flow, cerebral blood flow (CBF), and microvascular patency and, second, on GiPCR-dependent vascular responses after acute vascular occlusion. Our data reveal that injection of PTX severely reduces cerebral perfusion and impedes compensatory mechanisms regulating CBF. As a result, microcirculation collapses during vascular occlusion, contributing to ischemic brain lesions.
Materials and Methods
Animal Experiments
The study was carried out in compliance with the ARRIVE guidelines. All experiments were performed according to the EU Animals Scientific Procedures Act and the German law for the welfare of animals and were approved by the local animal ethical committees (Regierungspräsidium Tübingen, PH 10/13, PH 1/11, PH 04/19). C57BL/6 female, 8-week-old, mice were kept under specified pathogen-free conditions, controlled temperature, and humidity in 12-h day/night light cycles, receiving food and water ad libitum. Workflows of all experiments are sketched in the corresponding figures. We induced non-cerebral GiPCR KO using a single dose of PTX (150 μg/kg body weight) (Merck, Darmstadt, Germany) 48 h before intervention (sham or surgery), as previously shown [19, 23, 24]. Details are provided in the “Supplementary Information.”
Whole-Body Semi-quantitative Perfusion
In order to determine whether PTX produced whole-body systemic organ-perfusion changes, mice weighing 20–23 g were evaluated using dynamic contrast-enhanced (DCE) MRI. Vehicle (phosphate-buffered solution, PBS) or PTX was injected intraperitoneal (i.p.) into 5 mice per group. After 48 h, transversal DCE images focusing on multiple body regions including the lung, kidney, paravertebral muscle, abdominal vessels, heart, and brain were acquired. Details are provided in the “Supplementary Information.”
Longitudinal Multiparametric MRI—Animals and Treatment
For these experiments, 8-week-old mice were divided into four groups: PBS-pretreated sham-operated, PTX-pretreated sham-operated, PBS-pretreated occluded, and PTX-pretreated occluded. These groups were studied in two main experimental settings: in the first setting, mice were imaged immediately after vessel occlusion using a non-absorbable suture around one common carotid artery (CCA) or a sham surgery. In the second setting, the groups were imaged 1 week before (baseline) and 48 h after a transient occlusion (lasting 30 min) of one CCA or a sham surgery. Further experimental details are shown in the corresponding figures, Table 1, and “Supplementary Information.” PTX (150 µg/kg b.w., i.p.) or PBS were injected 48 h before surgery.
Longitudinal Multiparametric MRI—Acquisitions and Analysis
Multiparametric MRI acquisitions were performed using a ClinScan 7-T small-animal MR scanner, a rat whole-body transmitting coil, and a 4-channel mouse brain surface receiving coil (Bruker Biospin). The imaging protocol consisted of anatomical T2-weighted images (T2WI), diffusion-weighted images (DWI), perfusion-weighted images (PWI), and multi-turbo-spin-echo T2-weighted acquisitions focusing specifically on the Bregma/Interaural 3.82 ± 0.25 mm brain region as previously performed [20,21,22] and detailed in the “Supplementary Information.”
Volumes of Interest
All parametric images were coregistered to a common template using Pmod software (Bruker Biospin). Volumes of interest (VOIs) delimiting the striatal and cortical regions on both hemispheres were manually drawn at the above-described Bregma/Interaural brain regions using the T2WI as anatomical reference. The VOIs were overlaid on the PWI, ADC, and T2 maps followed by extraction of raw data. Lesion volumes were drawn on anatomical T2WI which covered the whole brain. Details are provided in the “Supplementary Information.”
Single-Vessel Multi-gradient Echo (MGE) Imaging Experiment
We performed multi-gradient echo data acquisitions for single-vessel imaging using a 14.1 T / 26 cm magnet (Magnex, Oxford, UK) with an Avance III console (Bruker Biospin) and a 12-cm-diameter gradient providing 100G / cm with 150-µs rise time (Resonance Research, Massachusetts, U.S.A). A home-made RF surface coil (8-mm outer diameter) was used for single-vessel mapping. Details are provided in the “Supplementary Information.”
Histology and Immunohistochemistry
For characterization of cerebral lesions, samples were stained with antibodies against CD31 (Abcam, Cambridge, UK), GFAP (Clone 6F2, Dako GmbH, Germany), HIF-1α (Clone ESEE 122, Abcam), and EPO (Clone H-162, Santa Cruz Biotechnology, Inc.). H&E staining was also performed. Details are provided in the “Supplementary Information.”
Statistics
Sample size and power calculations were conducted and approved by the local animal ethical committees. Animal numbers for the main experiments are shown in Table 1. We evaluated non-Gaussian distribution for all experimental datasets previous to statistical testing using the Jarque–Bera test. Whole-body perfusion data presented several datasets that were non-normality distributed; therefore, statistical evaluation was performed using a 2-sided non-parametric Wilcoxon signed-rank test. All other experiments were evaluated using either 2-way or 3-way ANOVA [25], followed by multiple comparison corrections using Tukey’s honestly significant test [26]. Details are provided in the “Supplementary Information.”
Results
Differential Effects of a Functional Non-cerebral GiPCR KO on Blood Flow to Different Organs and Body Compartments
First, we examined the rough impact of PTX-induced functional non-cerebral GiPCR KO on blood flow in different organs and compartments using whole-body dynamic contrast-enhanced (DCE) MRI. ANOVA determined a statistically significant main group difference between PTX and control animals. To detect differences between the same organs of both groups, Wilcoxon matched-pairs signed-rank test was performed, and a statistically decreased blood flow was only found in the brain of PTX animals (Fig. 1A). As with some other organs and compartments, median blood flow in the ventricle, reflecting ejection fraction in this experimental setting, was lower than in the control group, but without being statistically significant (Fig. 1B–F). Blood flow to the renal cortex after PTX treatment also suggested sustained perfusion of the kidney (Fig. 1C). The contrast agent accumulated in the renal calyceal system of PTX-treated animals, also indicating continued tubular excretion. The systemic results led us to investigate the effects of PTX in the brain using MRI techniques with better spatial resolution.
Functional non-cerebral GiPCR KO using PTX induces cerebral hypoperfusion. Whole-body perfusion was measured using dynamic contrast-enhanced imaging in PTX-pretreated and PBS-pretreated animals (n = 5 per group). A Wilcoxon matched-pairs signed-rank test found significant hypoperfusion in the brain of PTX-injected mice in comparison to PBS-treated animals (* p < 0.05). B Lung showed normal perfusion, whereas C kidney, D muscle, E abdominal vessels, and F heart yielded a hypoperfusion trend. Shown are median, 1st, and 3rd quartile of data distribution. The whiskers extend to the largest and smallest data point, respectively.
Reduction of Global CBF Following Functional Systemic Non-cerebral GiPCR KO with PTX
To confirm and extend our observation of decreased CBF, we subjected the mice to an arterial spin labeling (ASL) MRI protocol (for details, see the “Materials and Methods” section and Fig. 2A, B), which shows the distribution of blood perfusion in the brain and provides reliable quantifications of CBF [21, 27, 28]. Coronal cross-sectional perfusion-weighted imaging (PWI) confirmed whole-brain hypoperfusion in PTX-pretreated sham-operated mice (Fig. 2C; yellow arrow). We quantified the CBF for the striatal and cortical regions (Fig. 2D, E). Both ipsi- and contralateral CBF were reduced by more than half in these regions compared to untreated sham-operated controls (Fig. 2D, E). Nevertheless, all of these reduced CBF values were above a range associated with ischemic lesions [29, 30]. Thus, in agreement with the DCE measurements (see Fig. 1), our ASL data clearly reveal a systemic suppressive effect of PTX on CBF.
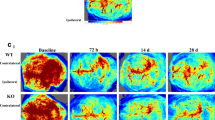
Functional PTX-induced non-cerebral GiPCR KO sensitizes for cerebral ischemia during permanent carotid artery occlusion. A Timeline of PBS/PTX injection, surgery (sham or CCA occlusion), and arterial spin-labeling MRI analysis. B Schematic overview of axial and coronal cross-sections of the mouse brain. The different brain regions of interest used for analysis are indicated. The red line shows the position of the cross-section corresponding to the coronal view. The blue line depicts the limit of ipsi (left)- and contra (right)-lateral brain hemispheres. C Perfusion-weighted images (PWI) indicate hypoperfusion of sham-operated PTX-treated mice (yellow arrow) compared to the sham PBS group. During left carotid artery ligation (occlusion), PBS-treated mice showed hypoperfusion visible in the ipsilateral hemisphere (green arrow), whereas PTX-pretreated mice exhibited global cerebral hypoperfusion, confirming the effects observed in whole-body perfusion analysis. Moreover, the perfusion of PTX-pretreated mice was interrupted in the ipsilateral hemisphere (red arrow) during occlusion, in comparison to animals receiving PBS. Shown are images of one representative mouse per group. Further examples are provided in Suppl. Fig. 1B. Corresponding quantification and statistics of CBF are shown in D for ipsi- and E for contralateral striatum and cortex (for details see Table 1). Statistical analysis was performed using 2-way ANOVA (* p < 0.05, *** p < 0.001). Shown are median, 1st, and 3rd quartile of data distribution. The whiskers extend to the largest and smallest data point, respectively.
PTX Administration Sensitizes to Ischemia
Having established that a functional non-cerebral GiPCR KO with PTX had an effect in CBF per se, we examined the consequences of acute occlusion of one common carotid artery (CCA) in cerebral hypoperfusion (see the “Materials and Methods” section and Fig. 2A, B). As evident from PWI, unilateral CCA occlusion in control animals treated with PBS resulted in a large decrease on CBF ipsilateral to the occlusion (Fig. 2C, Suppl. Fig. 1B; green arrow). This is also reflected in the calculated CBF values, which showed a clear hypoperfusion for the ipsilateral striatum and cortex (Fig. 2D). However, the hypoperfusion did not reach a level described to cause ischemia and necrosis [29, 30]. Of note, blood flow in the contralateral regions remained stable (Fig. 2E), which should allow for potential compensatory blood flow to the hypoperfused regions [31].
In contrast, PTX-pretreated mice showed global cerebral hypoperfusion that was further aggravated ipsilateral to the unilateral CCA ligation resulting in a complete breakdown of perfusion in both the striatum and cortex (Fig. 2C, D; Suppl. Fig. 1B; red arrow). These ipsilateral values were below the threshold at which ischemic injury occurs [29, 30]. On the contralateral side, an extent of reduction occurred that we had already observed in the sham-operated mice pretreated with PTX, and that may impede compensatory blood flow to the hypoperfused ipsilateral regions (Fig. 2E, Suppl. Fig. 1B).
Our findings show that a functional non-cerebral GiPCR KO with PTX suppresses cerebral perfusion, which upon challenge by unilateral CCA occlusion severely disrupts CBF distal to the ligation, i.e., in the ipsilateral hemisphere. We were therefore interested in how perfusion subsequently developed and compared PWI at baseline and 48 h after surgery, which corresponded to 96 h after PTX administration (Suppl. Fig. 2A, B). The CBF in the brain of the PBS-injected mice, sham-operated or transiently CCA-occluded, was invariant from baseline post surgically at 48 h (Suppl. Fig. 2C-F). The corresponding CBF in the non-cerebral GiPCR KO mice was reduced albeit not significantly compared to baseline. Compared with the CBF of non-cerebral GiPCR KO mice during occlusion (see Suppl. Fig. 1B and Fig. 2D, E) the CBF of mice monitored 48 h later, i.e., 96 h after PTX dosing (see Suppl. Fig. 2C-F), indicated a partial recovery. However, there was no difference in CBF in PTX-pretreated mice regardless of whether they were sham-operated or transiently CCA-occluded 48 h before (see Suppl. Fig. 2C-F). This finding was in contrast to the different results in the two PTX-pretreated groups, i.e., sham-operated or transiently CCA-occluded at the time of occlusion (see Suppl. Fig. 1B and Fig. 2D, E). This prompted us to further investigate consequences of collapsed perfusion in non-cerebral GiPCR KO mice after transient unilateral CCA occlusion (Suppl. Fig. 3A).
Functional Non-cerebral GiPCR KO Together with Transient Unilateral Carotid Artery Occlusion Leads to Cytotoxic and Vasogenic Edema
Diffusion-weighted images (DWI) provide a measurement of diffusion that can be quantified in the apparent diffusion coefficient (ADC) using MRI. ADC restrictions in the brain are the gold standard to identify ischemic stroke lesions, which have been shown to strongly correlate to final infarct lesions in tissue sections [32,33,34,35]. Diffusion restrictions have been known to start rapidly after stroke onset, peaking within one day, followed by slow value normalization [36, 37]. Consistent with these previous reports, PTX-pretreated and occluded mice already showed incipient ADC restrictions during occlusion (see Suppl. Fig. 3B-D), which were still evident in the mice imaged at 48 h post-surgery, corresponding to 96 h after PTX administration (Fig. 3B; red arrow, Fig. 3C). These ADC restrictions were clearly demarcated in DWIs of these mice (Suppl. Fig. 3B-D).
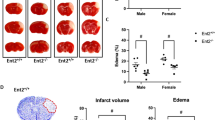
Cytotoxic and vasogenic edema in non-cerebral GiPCR KO following transient CCA occlusion. A Timeline of baseline MRI acquisition, PBS/PTX injection, surgery (sham or CCA occlusion), and post-operative MRI acquisitions. B Representative images of mouse brains showing the apparent diffusion coefficient (ADC), T2 map, and T2-weighted images (T2WI). Red arrows indicate the ischemic lesions in occluded PTX-pretreated mice consisting of reduced signal intensity of ADC images as well as hyperintensity in T2WI and T2 maps (for more details, see Tables 1, 2, and 3). Corresponding quantification and statistical analysis of ipsilateral ADC (C) and T2 (D) in the striatum. Only PTX-pretreated mice following transient CCA occlusion presented a lesioned striatum with increments in ADC, accompanied by an increased T2 relaxation time. Statistical analysis was performed using 3-way ANOVA (* p < 0.05, ** p < 0.01, *** p < 0.001). Shown are median, 1st, and 3rd quartile of data distribution. The whiskers extend to the largest and smallest data point respectively.
Moreover, T2 relaxation maps and T2WI representing vasogenic edema, demonstrated hyperintense signals only in the PTX-pretreated occluded animals at the latest timepoint (Fig. 3B, D; Suppl. Fig. 3B, E, F), consistent with previous literature [36, 37]. As the occluded animals pretreated with PTX showed vasogenic edema, we quantified edema volume in relation to their anatomical structures (Suppl. Fig. 4). In contrast, no signs of cytotoxic or vasogenic edema were detectable in both sham-operated groups and the PBS-treated occluded group 48 h after occlusion (Figs. 3C, D).
Because cytotoxic and vasogenic edema developed only in PTX-pretreated animals with transient CCA occlusion, we performed histological and immunohistochemical analyses to confirm the presence of an ischemic stroke phenotype, as we have previously done in other stroke models [20, 35]. Detection of ischemic lesions using hypoxia-inducible factor 1α (HIF-1α) and erythropoietin (EPO) immunohistochemistry has been previously shown to clearly delimit the infarct core and the peri-infarct stroke region [38, 39] (Fig. 4A-D; Suppl. Fig. 5). The immunohistochemical staining showed focal lesions in the PTX-pretreated and CCA-occluded animals demonstrating ischemia ipsilateral to the occlusion, which perfectly colocalized with hyperintense lesions seen in DWIs and T2WIs (Fig. 4). Furthermore, H&E staining and immunohistochemistry for the endothelial markers CD31 and GFAP (Suppl. Fig. 5) revealed prominent lesions with neuronal pallor, vacuolation of the neuropil and edema (H&E) in various regions of the ipsilateral hemisphere, as well as blood vessels (CD31) and reactive gliosis (GFAP). Thus, clear signs of ischemic stroke through in vivo imaging were confirmed in PTX-pretreated transiently CCA-occluded animals using immunohistochemistry and histology.
Colocalization of DWIs and T2WIs with immunohistochemical ischemia in occluded PTX-pretreated mice. A Timeline of PBS/PTX injection protocol, surgery, and MRI acquisition. B DWI (b value = 600 s/mm2) and T2WI of animals at 96 h on the coronal projection. The occluded PTX-pretreated mice show hyperintensities in the striatal, hippocampal, and cortical brain regions on DWI and T2WI (orange arrowheads). Animals of the other groups showed no visible lesions. For more details, see Table 1. C HIF-1α is stained in hippocampal stroke regions and marks the infarcted region colocalizing with the DWIs. D. Staining of the hypoxia-inducible cytokine EPO shows a focalized lesion similar to the HIF-1α-positive hypoxic region further confirming an ischemic event. Immunohistochemistry was done in n = 4 mice per group.
Functional Non-cerebral GiPCR KO with PTX Reduces Patency of Individual Cortex-Penetrating Microvessels
We investigated whether hypoperfusion was associated with collapsed microvessels. To specifically investigate the immediate response of microvessels to CCA occlusion, we used a multi-gradient echo (MGE) MRI sequence (Fig. 5A) [40,41,42]. High-resolution MGE-MRI provides a penetrating microvessel-specific measurement of the cortex that allows the estimation of microvascular collapse. Comparison of PBS-treated mice regardless of CCA occlusion revealed no difference in the number of vessels in both hemispheres (Fig. 5), indicating a normal microvascular function.
Functional non-cerebral GiPCR KO reduces patency of cortex-penetrating microvessels. A Timeline of PBS/PTX injection and surgery protocol following multi-gradient echo (MGE) MRI acquisition. These experiments were performed during occlusion or sham surgery. Results of quantification of vessel numbers in the ipsi- (B) and (C) contralateral cortex (n = 6–9). Vessel numbers of PTX-pretreated mice are reduced in both hemispheres, which is further aggravated upon occlusion in the ipsilateral cortex. Statistical analysis was performed using 2-way ANOVA (* p < 0.05, ** p < 0.01, *** p < 0.001). D Representative pictures from all four groups measured by MGE (upper panel). The black boxes mark the assessed areas, and the red dots are the identified vessels (lower panel). Shown are median, 1st, and 3rd quartile of data distribution. The whiskers extend to the largest and smallest data point, respectively.
In contrast, the PTX-induced functional non-cerebral GiPCR KO provoked a reduction of quantifiable microvessels in the cortex of both hemispheres compared to the PBS groups (Fig. 5). The effect was further aggravated in the PTX-pretreated occluded mice, where an even more prominent number of microvessels collapsed in the ipsilateral cortex (Fig. 5). In combination with our perfusion experiments, these data suggest that PTX does not only cause global cerebral hypoperfusion but also micro-cerebrovascular collapse, which has also been described to occur under low-perfusion pressure in heart vessels [7].
Discussion
Cerebrovascular functions of GiPCR-driven signaling are still largely unknown. To gain more insight, we employed the highly specific inhibitor PTX in order to specifically disrupt extraneuronal GiPCR signaling. Our results point to previously unrecognized functions of GiPCR signaling in the regulation of CBF and possibly systemic blood flow. Furthermore, extraneuronal functional PTX-induced non-cerebral GiPCR KO in combination with unilateral CCA produces brain lesions with similar imaging characteristics to human ischemic stroke.
One major drawback of the functional non-cerebral GiPCR KO with PTX is the ubiquitous nature of the KO in a multitude of systemic cellular processes. The systemic non-cerebral GiPCR KO may induce alterations in various systems, such as cardiovascular and immune system. In fact, it is used to establish the pertussis toxin-induced reversible encephalopathy dependent on monocyte chemoattractant protein-1 overexpression (PREMO) model, consisting on the injection of Mycobacterium tuberculosis and two injections of PTX [43]. We have previously shown that although PTX-sensitive Gi proteins are ubiquitously expressed, a single extraneuronal application of the toxin in vivo does not modify neuronal GiPCR and does not cross through the intact BBB [19]. Therefore, it is possible under this specific setting, to evaluate the effects of PTX in the perfusion of brain vessels and in systemic perfusion, without unwanted effects in neurons. We evaluated systemic hemodynamic effects using whole-body perfusion in order to reveal major possible alterations, and although we found only significant effects in the brain, other effects on systemic hemodynamics cannot be excluded. In fact, it has been demonstrated that PTX induces changes in blood pressure in hypertensive rats [2]. Moreover, it has been reported that in the cardiovascular system, PTX activity induces vessel size-dependent changes in vascular resistance [7], impairs endothelial Ca2+ influx [8], or lowers Ca2+ sensitivity of vasoconstriction in response to noradrenaline [2]. In line with these previous works, our findings now reveal a relevant effect in global cerebral hypoperfusion and microvascular collapse of cerebral vessels. The microvessel dysfunction could be at least partially mediated by interference with vascular Gi protein-mediated signaling affecting nitric oxide, β-adrenergic, angiotensin II type 1, serotonin-1A, or relaxin receptor function [2, 15, 18, 44]. Moreover, PTX has been shown to inhibit endothelium-dependent relaxation in hypercholesterolemic and atherosclerotic arteries [15, 16], which specifically links a disrupted G protein-mediated transduction to microvascular dysfunction. Indeed, chronic hypertension, dyslipidemias, diabetes, and increased age have been correlated to hypoperfusion and microarterial impairment [45,46,47].
Interestingly, PTX has been recently reported to be neuroprotective due to a reduction of glutamate-induced calcium influx into ischemic neurons [48]. Tang et al. injected PTX as a neuroprotectant at a dose of 40 µg/kg b.w. 30 min after applying a permanent middle cerebral artery occlusion. This occlusion triggered a BBB breakdown, allowing PTX to enter the brain [37, 49]. Consequently, Tang et al. injected PTX at a lower dose and at a time when the ischemic brain had a permeable BBB and could potentially benefit from inhibition of calcium influx. However, no perfusion deficits were observed in this study. In the current study, we administered the toxin again at 150 µg/kg b.w. 48 h before carotid artery occlusion; thus, the BBB was intact at the moment of PTX injection and not able to reach the neurons [19]. The comparison of the work from Tang et al. to our study is an excellent reminder of how timing and dosage of therapeutic interventions, especially in niche compartments, are important for outcome.
The significance of our findings in the clinical field is directly related to the involvement of G protein signaling alterations in the pathogenesis of neurodegenerative and cerebrovascular diseases. G protein signaling is involved with neurotransmitters such acetylcholine, GABA (gamma-aminobutyric acid), and glutamate. Here, for example, the acetylcholine receptor has been associated to formation of Aß peptide and neurofibrillary tangles in Alzheimer’s disease [50]. From a vascular perspective, alterations in G protein signaling involving monoamines such as adrenaline, noradrenaline, serotonin, dopamine, and histamine could be directly associated with cerebral hypoperfusion, a well-known imaging hallmark of neurodegenerative diseases [21, 51, 52]. Cerebral hypoperfusion is also a common risk factor in cerebrovascular diseases such as cerebral microbleeds and stroke [53, 54]. Therefore, GiPCR-driven signaling for the maintenance of CBF may be relevant to identify novel therapeutic targets. The PTX-triggered CBF impairment sensitized the brain to ischemic injury by disabling the mechanisms of blood flow regulation, an interesting effect that requires further mechanistic clarification focusing on the deficiency of specific G protein isoforms. The impaired hemodynamic stability and responsiveness of the cerebrovascular system caused by functional non-cerebral GiPCR KO in mice are reminiscent of observed hypoperfusion and vascular dysfunction in humans with chronic vascular disease, which is also predictive of human stroke severity [47].
Up to now, blocked GiPCR signaling had not yet been linked to the occurrence of cerebrovascular hypoperfusion and vascular collapse. It will be interesting to identify the specific GiPCRs involved in the maintenance of CBF and vascular tone. Furthermore, the effects of hypoperfusion and microvascular collapse induced by functional non-cerebral GiPCR KO may be useful for neuroscience, functional neuroimaging, and neurooncology.
References
Nagata K, Ye C, Jain M et al (2000) Gαi2 but not Gαi3 is required for muscarinic inhibition of contractility and calcium currents in adult cardiomyocytes. Circ Res 87:903–909. https://doi.org/10.1161/01.RES.87.10.903
Zemancíková A, Török J, Zicha J, Kunes J (2008) Inactivation of G(i) proteins by pertussis toxin diminishes the effectiveness of adrenergic stimuli in conduit arteries from spontaneously hypertensive rats. Physiol Res 57:299–302
Hu K, Nattel S (1995) Mechanisms of ischemic preconditioning in rat hearts. Circulation 92:2259–2265. https://doi.org/10.1161/01.CIR.92.8.2259
Rosenbaum DM, Rasmussen SGF, Kobilka BK (2009) The structure and function of G-protein-coupled receptors. Nature 459:356–363. https://doi.org/10.1038/nature08144
Drake MT, Shenoy SK, Lefkowitz RJ (2006) Trafficking of G protein-coupled receptors. Circ Res 99:570–582. https://doi.org/10.1161/01.RES.0000242563.47507.ce
Gohla A, Klement K, Piekorz RP et al (2007) An obligatory requirement for the heterotrimeric G protein Gi3 in the antiautophagic action of insulin in the liver. Proc Natl Acad Sci U S A 104:3003–3008. https://doi.org/10.1073/pnas.0611434104
Komaru T, Wang Y, Akai K et al (1994) Pertussis toxin-sensitive G protein mediates coronary microvascular control during autoregulation and ischemia in canine heart. Circ Res 75:556–566. https://doi.org/10.1161/01.RES.75.3.556
Spitzbarth-Régrigny E, Petitcolin MA, Bueb JL et al (2000) Pertussis toxin-sensitive G i -proteins and intracellular calcium sensitivity of vasoconstriction in the intact rat tail artery. Br J Pharmacol 131:1337–1344. https://doi.org/10.1038/sj.bjp.0703703
Nürnberg B (2000) Pertussis toxin as a pharmacological tool. In: Aktories K, Just I (eds) Bact. Protein Toxins. Pertussis Toxin as a Pharmacological Tool, (HEP, Vol. 145, Springer Berlin Heidelberg, Berlin, Heidelberg, pp 187–206. https://doi.org/10.1007/978-3-662-05971-5_9
Regard JB, Kataoka H, Cano DA et al (2007) Probing cell type-specific functions of Gi in vivo identifies GPCR regulators of insulin secretion. J Clin Invest 117:4034–4043. https://doi.org/10.1172/JCI32994
Wang L, Pydi SP, Zhu L et al (2020) Adipocyte Gi signaling is essential for maintaining whole-body glucose homeostasis and insulin sensitivity. Nat Commun 11:1–17. https://doi.org/10.1038/s41467-020-16756-x
Lu C, Pelech S, Zhang H et al (2008) Pertussis toxin induces angiogenesis in brain microvascular endothelial cells. J Neurosci Res 86:2624–2640. https://doi.org/10.1002/jnr.21716
Kost CK Jr, Herzer WA, Li PJ, Jackson EK (1999) Pertussis toxin-sensitive G-proteins and regulation of blood pressure in the spontaneoulsy hypertensive rat. Clin Exp Pharmacol Physiol 26:449–455. https://doi.org/10.1046/j.1440-1681.1999.03058.x
Li Y, Anand-Srivastava MB (2002) Inactivation of enhanced expression of G i proteins by pertussis toxin attenuates the development of high blood pressure in spontaneously hypertensive rats. Circ Res 91:247–254. https://doi.org/10.1161/01.RES.0000029969.39875.4B
Shimokawa H, Flavahan NA, Vanhoutte PM (1991) Loss of endothelial pertussis toxin-sensitive G protein function in atherosclerotic porcine coronary arteries. Circulation 83:652–660. https://doi.org/10.1161/01.CIR.83.2.652
Flavahan NA (1992) Atherosclerosis or lipoprotein-induced endothelial dysfunction: Potential mechanisms underlying reduction in EDRF/nitric oxide activity. Circulation 85:1927–1938. https://doi.org/10.1161/01.CIR.85.5.1927
Rao BD, Sarkar P, Chattopadhyay A (2020) Selectivity in agonist and antagonist binding to serotonin1a receptors via G-protein coupling. Biochim Biophys Acta - Biomembr 1862:183265. https://doi.org/10.1016/j.bbamem.2020.183265
Lian X, Beer-Hammer S, König GM et al (2018) RXFP1 receptor activation by relaxin-2 induces vascular relaxation in mice via a Gαi2-protein/PI3Kβ/γ/nitric oxide-coupled pathway. Front Physiol 9:1–13. https://doi.org/10.3389/fphys.2018.01234
Castaneda Vega S, Leiss V, Piekorz R et al (2020) Selective protection of murine cerebral Gi/o-proteins from inactivation by parenterally injected pertussis toxin. J Mol Med 98:97–110. https://doi.org/10.1007/s00109-019-01854-1
Castaneda Vega S, Weinl C, Calaminus C et al (2017) Characterization of a novel murine model for spontaneous hemorrhagic stroke using in vivo PET and MR multiparametric imaging. Neuroimage 155:245–256. https://doi.org/10.1016/j.neuroimage.2017.04.071
Maier FC, Wehrl HF, Schmid AM et al (2014) Longitudinal PET-MRI reveals β-amyloid deposition and rCBF dynamics and connects vascular amyloidosis to quantitative loss of perfusion. Nat Med 20:1485–1492. https://doi.org/10.1038/nm.3734
Weinl C, Castaneda Vega S, Riehle H et al (2015) Endothelial depletion of murine SRF/MRTF provokes intracerebral hemorrhagic stroke. Proc Natl Acad Sci 112:9914–9919. https://doi.org/10.1073/pnas.1509047112
Devanathan V, Hagedorn I, Köhler D et al (2015) Platelet Gαi protein Gαi2 is an essential mediator of thrombo-inflammatory organ damage in mice. Proc Natl Acad Sci 112:6491–6496. https://doi.org/10.1073/pnas.1505887112
Köhler D, Devanathan V, de Oliveira B, Franz C et al (2014) Gαi2- and Gαi3-deficient mice display opposite severity of myocardial ischemia reperfusion injury. PLoS ONE 9:e98325. https://doi.org/10.1371/journal.pone.0098325
Khan A, Rayner G (2003) Robustness to non-normality of common tests for the many-sample location problem. J Appl Math Decis Sci 7:187–206. https://doi.org/10.1207/S15327612JAMD0704_1
Nanda A, Mohapatra DBB, Mahapatra APK et al (2021) Multiple comparison test by Tukey’s honestly significant difference (HSD): do the confident level control type I error. Int J Stat Appl Math 6:59–65. https://doi.org/10.22271/maths.2021.v6.i1a.636
Bokkers RPH, Hernandez DA, Merino JG et al (2012) Whole-brain arterial spin labeling perfusion mri in patients with acute stroke. Stroke 43:1290–1294. https://doi.org/10.1161/STROKEAHA.110.589234
Zhang K, Herzog H, Mauler J et al (2014) Comparison of cerebral blood flow acquired by simultaneous [15O]water positron emission tomography and arterial spin labeling magnetic resonance imaging. J Cereb blood flow Metab 34:1373–1380. https://doi.org/10.1038/jcbfm.2014.92
Markus HS (2004) Cerebral perfusion and stroke. J Neurol Neurosurg Psychiatry 75:353–361. https://doi.org/10.1136/jnnp.2003.025825
Heiss W-D (2011) The ischemic penumbra: correlates in imaging and implications for treatment of ischemic stroke. Cerebrovasc Dis 32:307–320. https://doi.org/10.1159/000330462
Guo H, Itoh Y, Toriumi H et al (2011) Capillary remodeling and collateral growth without angiogenesis after unilateral common carotid artery occlusion in mice. Microcirculation 18:221–227. https://doi.org/10.1111/j.1549-8719.2011.00081.x
Benveniste H, Hedlund LW, Johnson GA (1992) Mechanism of detection of acute cerebral ischemia in rats by diffusion- weighted magnetic resonance microscopy. Stroke 23:746–754. https://doi.org/10.1161/01.STR.23.5.746
Shereen A, Nemkul N, Yang D et al (2011) Ex vivo diffusion tensor imaging and neuropathological correlation in a murine model of hypoxia–ischemia-induced thrombotic stroke. J Cereb Blood Flow Metab 31:1155–1169. https://doi.org/10.1038/jcbfm.2010.212
Zille M, Farr TD, Przesdzing I et al (2012) Visualizing cell death in experimental focal cerebral ischemia: promises, problems, and perspectives. J Cereb Blood Flow Metab 32:213–231. https://doi.org/10.1038/jcbfm.2011.150
Castaneda-Vega S, Katiyar P, Russo F et al (2021) Machine learning identifies stroke features between species. Theranostics 11:3017–3034. https://doi.org/10.7150/thno.51887
Loubinoux I, Volk A, Borredon J et al (1997) Spreading of vasogenic edema and cytotoxic edema assessed by quantitative diffusion and T2 magnetic resonance imaging. Stroke 28:419–427. https://doi.org/10.1161/01.STR.28.2.419
Jiang X, Andjelkovic AV, Zhu L et al (2018) Blood-brain barrier dysfunction and recovery after ischemic stroke. Prog Neurobiol 163–164:144–171. https://doi.org/10.1016/j.pneurobio.2017.10.001
Sirén A-L, Knerlich F, Poser W et al (2001) Erythropoietin and erythropoietin receptor in human ischemic/hypoxic brain. Acta Neuropathol 101:271–276. https://doi.org/10.1007/s004010000297
Wang GL, Jiang BH, Rue EA, Semenza GL (1995) Hypoxia-inducible factor 1 is a basic-helix-loop-helix-PAS heterodimer regulated by cellular O2 tension. Proc Natl Acad Sci 92:5510–5514. https://doi.org/10.1073/pnas.92.12.5510
Yu X, He Y, Wang M et al (2016) Sensory and optogenetically driven single-vessel fMRI. Nat Methods 13:337–340. https://doi.org/10.1038/nmeth.3765
He Y, Wang M, Chen X et al (2018) Ultra-slow single-vessel BOLD and CBV-based fMRI spatiotemporal dynamics and their correlation with neuronal intracellular calcium signals. Neuron 97:925-939.e5. https://doi.org/10.1016/j.neuron.2018.01.025
He Y, Wang M, Yu X (2020) High spatiotemporal vessel-specific hemodynamic mapping with multi-echo single-vessel fMRI. J Cereb Blood Flow Metab 40:2098–2114. https://doi.org/10.1177/0271678X19886240
Huang D, Tani M, Wang J et al (2002) Pertussis toxin-induced reversible encephalopathy dependent on monocyte chemoattractant protein-1 overexpression in mice. J Neurosci 22:10633–10642. https://doi.org/10.1523/JNEUROSCI.22-24-10633.2002
Hare JM, Kim B, Flavahan NA et al (1998) Pertussis toxin-sensitive G proteins influence nitric oxide synthase III activity and protein levels in rat heart. J Clin Invest 101:1424–1431. https://doi.org/10.1172/JCI1012
Yonas H, Smith HA, Durham SR et al (1993) Increased stroke risk predicted by compromised cerebral blood flow reactivity. J Neurosurg 79:483–489. https://doi.org/10.3171/jns.1993.79.4.0483
Isozaki M, Arai Y, Kudo T et al (2010) Clinical implication and prognosis of normal baseline cerebral blood flow with impaired vascular reserve in patients with major cerebral artery occlusive disease. Ann Nucl Med 24:371–377. https://doi.org/10.1007/s12149-010-0367-9
Gupta A, Chazen JL, Hartman M et al (2012) Cerebrovascular reserve and stroke risk in patients with carotid stenosis or occlusion. Stroke 43:2884–2891. https://doi.org/10.1161/STROKEAHA.112.663716
Tang Z, Li S, Han P et al (2015) Pertussis toxin reduces calcium influx to protect ischemic stroke in a middle cerebral artery occlusion model. J Neurochem 135:998–1006. https://doi.org/10.1111/jnc.13359
Abdullahi W, Tripathi D, Ronaldson PT (2018) Blood-brain barrier dysfunction in ischemic stroke: targeting tight junctions and transporters for vascular protection. Am J Physiol Physiol 315:C343–C356. https://doi.org/10.1152/ajpcell.00095.2018
Barrantes FJ, Borroni V, Vallés S (2010) Neuronal nicotinic acetylcholine receptor-cholesterol crosstalk in Alzheimer’s disease. FEBS Lett 584:1856–1863. https://doi.org/10.1016/j.febslet.2009.11.036
Fernández-Seara MA, Mengual E, Vidorreta M et al (2012) Cortical hypoperfusion in Parkinson’s disease assessed using arterial spin labeled perfusion MRI. Neuroimage 59:2743–2750. https://doi.org/10.1016/j.neuroimage.2011.10.033
Austin BP, Nair VA, Meier TB et al (2011) Effects of hypoperfusion in Alzheimer’s disease. Adv Alzheimer’s Dis 2:253–263. https://doi.org/10.3233/978-1-60750-793-2-253
Sweet JG, Chan S, Cipolla MJ (2015) Effect of hypertension and carotid occlusion on brain parenchymal arteriole structure and reactivity. J Appl Physiol 119:817–823. https://doi.org/10.1152/japplphysiol.00467.2015
Tian G, Ji Z, Lin Z et al (2020) Cerebral autoregulation is heterogeneous in different stroke mechanism of ischemic stroke caused by intracranial atherosclerotic stenosis. Brain Behav 11:1–13. https://doi.org/10.1002/brb3.1907
Acknowledgements
Special thanks to Dr. Lisa Wang for her expertise and advice on the statistical analyses performed for this manuscript. The authors thank Daniel Bukala, Maren Harant, Henri De Maissin, Sandra Schwegmann, and Dennis Thiele for their assistance in this research. We are indebted to Prof. Klaus Schulze-Osthoff for valuable comments and discussions.
Funding
Open Access funding enabled and organized by Projekt DEAL. Funding for this research project was provided by the DFG (to B.N.: GRK 1089, SFB 612, NU 53/12–2; NU 53/13–1; to X.Y.: YU 215/3–1, to M.G. GRK 1365, GO 766/12–3, GO 766/15–2, GO 766/18–2), BMBF (to X.Y.: 01GQ1702), NIH Brain Initiative (to X.Y.: 1RF1NS113278-01), the Werner-Siemens foundation (to B.P.), and Karl Kuhn foundation (to B.N.).
Author information
Authors and Affiliations
Contributions
S.C.V., S.B.-H., B.J.P., B.N. designed research; S.C.V., S.B.-H., H.N., M.V., H.Z., Y.H., U.F., U.K., I.G.M., X.Y. performed research; S.C.V., A.M.S., J.-M.H. contributed reagents/analytic tools; S.C.V., M.V., A.M.S., V.L., I.G.M., L.Q.-M., X.Y., B.J.P., B.N. analyzed data; and S.C.V., S.B.-H., V.L., M.G., X.Y., B.J.P., B.N. wrote the paper. All authors read and edited the paper.
Corresponding authors
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Castaneda-Vega, S., Beer-Hammer, S., Leiss, V. et al. Cerebrovascular Gi Proteins Protect Against Brain Hypoperfusion and Collateral Failure in Cerebral Ischemia. Mol Imaging Biol 25, 363–374 (2023). https://doi.org/10.1007/s11307-022-01764-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11307-022-01764-8